The Artistry of Direct Resin Veneers
A challenging treatment option that achieves beautiful, long-lasting results
Jeff Lineberry, DDS, FAGD, FICOI, AAACD
In today's society, the quest for a beautiful smile is a top priority for many adults. With technology and material advancements occurring all the time, there are many options available to achieve the desired results for patients, many of which can do so in a very conservative manner. In addition to the many improvements to indirect restorative materials, there have been many improvements to the formulations of direct resin materials that can help optimize the efficiency and predictability of restorative treatment. When a patient presents seeking to restore and enhance his or her smile, responsible clinicians actively pursue doing so in a way that will achieve the best possible result in the most conservative manner possible.
To achieve significant changes in a patient's smile, a frequently used treatment modality is the placement of indirect porcelain restorations. In years past, more aggressive preparations were used due to the materials, which helped achieve an excellent result but lead to unnecessary loss of tooth structure. As time went on, the advent of enamel bonding changed dentistry forever and became the stepping-stone for the current world of adhesive dentistry. With the arrival of enamel bonding and the availability of feldspathic porcelain veneers, dentistry could recreate smiles with minimal tooth preparations and achieve excellent results; however, the process was still technically challenging and time-consuming for both the dentist and laboratory technician. With today's technology, indirect porcelain restorations can be fabricated by a skilled ceramist in a dental laboratory setting or by clinicians using in-office milling units and digital scans. And with today's newer, stronger ceramics, such as lithium disilicates, clinicians can do little to no preparation of the dentition and still achieve an excellent esthetic result.
Another alternative is the use of direct resin materials. For many restorative dentists, direct resin bonding (ie, direct resin veneers) can be one of the most daunting tasks because it requires a significant amount of time, skill, passion, and artistry to achieve beautiful, long-lasting results. Beyond affording the restorative dentist with the opportunity to express his or her artistic abilities, direct resin bonding allows for greater control over the color, shape, and contours of the final restoration. It also empowers the dentist to make future repairs when needed and to avoid removing tooth structure in areas of undercuts that if restored indirectly, would have to be reshaped to allow for proper seating.1
Following this principle and using proper layering and finishing techniques, the restorative dentist can create long-lasting direct restorations with exceptional esthetics. To help achieve these results, this article will discuss tooth preparation, material choice, and bonding procedures as well as techniques for layering, tinting, and finishing.
Preparation
The amount of tooth preparation needed, whether it is for a direct or indirect restoration, should be informed by the specific needs of each individual case. It depends on many factors that need to be assessed prior to restoration. Even with all of the advancements in materials, dentists still have to keep many things in mind when deciding how much preparation of the dentition is required to achieve an ideal result, including the existing color, condition, and position of the teeth. All of these variables can require a more aggressive preparation of the dentition in order to obtain the ideal result, especially if the tooth/teeth are in a less than ideal position in the arch form or if the existing color is several shades darker than that of the desired final restoration. Otherwise, it is difficult to disguise the dark underlying tooth structure with a natural looking, opalescent restoration, regardless of the material used. The darker the current tooth shade and the whiter the final shade desired, the more preparation is needed to mask the underlying tooth and achieve an ideal result. And if the tooth is protruding into the dental arch form, the patient must either commit to orthodontics to move the tooth into an ideal position or agree to the removal of more tooth structure in order to achieve a restoration with ideal form and function.
Material Selection
When treatment planning a direct resin restoration, some basic questions need to be answered before preparation of the teeth. Will the restoration be located in the posterior segment or in the esthetic zone, which is readily visible to the patient and other people? In addition, will the restoration be replacing part of or all of the facial surface of the tooth/teeth? The dentist needs to have some understanding of the properties of the materials selected regarding handling, strength, opacity, and overall polishability.2,3 Poor material selection may lead to a less than ideal result, such as a restoration that lacks the strength to maintain long-term function or one that becomes dull over time as opposed to maintaining its luster.
When it comes to choosing a resin in today's marketplace, there is a wide array of brands to choose from that offer a variety of formulations. The different categories of composite resins include the following4:
Microfills. These resins, which have been around for over 30 years, contain approximately 35% to 50% silicon dioxide filler particles ranging from 0.02 to 0.04 µm. Due to their small filler size, they can be highly polished to mimic a luster similar to enamel. Unfortunately, what many gain in appearance, they lose in overall strength, making them most suitable for use in anterior restorations or in Class V cervical restorations.
Hybrids. Hybrid composite resins offer both strength and reasonable polishability and have been frequently used in posterior restorations. A heterogeneous aggregate of filler particles in sizes ranging from 0.04 to 5.00 µm comprises approximately 70% to 80% of the weight of these materials. Although many kits offer a variety of shades, including incisal and various opacities, some hybrids are less able to retain their gloss over time when compared with newer formulations of composite resins.
Nanofills and nanohybrids. These materials represent the newest category of resins to be added to the composite armamentarium. They consist of nanomers (ie, 5- to 75-nm particles) and "nanocluster" agglomerates (ie, 0.6 to 1.4 µm in size) as fillers. The advantage of these resins is that they possess strength similar to that of microhybrids, but offer the ability to be polished and appear to retain their gloss for a longer period of time when compared with older composite formulations.5
Case Study
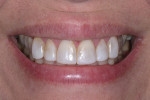
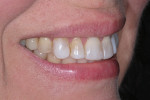
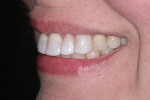
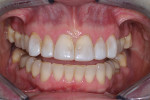
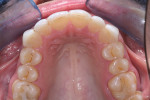
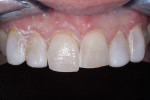
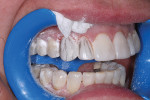
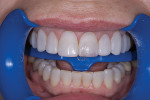
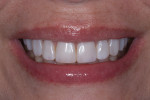
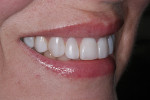
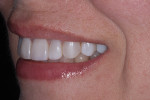
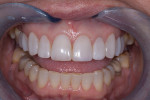
A 43-year-old patient presented with the chief complaint of wanting to improve her smile (Figure 1 through Figure 5). She wanted it to be "whiter and brighter" because her teeth were "darkening" and noted that old bonding was failing. In addition, she was concerned about how her "smile had collapsed in" on the sides, emphasizing that her smile was "not as full as it used to be." The results of her periodontal and temporomandibular joint exams were within normal limits. After discussing all treatment options at length, the patient consented to treatment with direct resin veneers.
Treatment
The maxillary area involving teeth Nos. 4 through 13 was anesthetized because the patient had hypersensitivity due to an exposed root surface. Beginning with the central incisors only, the previous bonding was removed using a high-speed handpiece with a 12-fluted carbide bur (No. 7408, Brasseler USA) (Figure 6). Based on the patient's request to have lighter-colored final restorations; the slightly proclined overall position of her teeth; and the poor esthetics of the previously placed "no preparation" restorations, it was decided that some tooth removal was needed on the facial and incisal aspects to achieve the desired final result. A 0.3 mm depth cutting bur (LVS2, Brasseler USA) was used to create consistent facial reduction planes, and then a medium-grit diamond bur was used to reduce the incisal aspect of the preparations by approximately 1.0 mm and to finish and blend the remaining portion of the preparation of tooth No. 9. The teeth were isolated using cotton rolls and retractors. After placing mylar strips in the interproximal areas to confine acid etching to the maxillary centrals, they were etched with 35% phosphoric acid for 15 seconds, rinsed, and lightly dried. Next, a bonding agent (Scotchbond Universal™, 3M) was applied thoroughly and dried prior to being cured.
The lingual shelf and new incisal edge area were created using a freehand technique with a nanohybrid resin (Clearfil Majesty ES-2™, Kuraray America), which was selected for its strength and wear characteristics. After curing, a thin layer of white, opaque shade microfill resin (Renamel® Microfill, W-Shade; Cosmedent) was placed in the cervical area to help block out the darker area of the tooth, and it was extended into the middle third of the tooth in an irregular manner to help break up the outline. This material was also used in the incisal third to help block out any show-through and create some light diffusion in the area. Next, layers of two different bleach shades (Renamel® Microfill, SuperBrite 2 and 3; Cosmedent) were placed, blended, and fully contoured using a gold-grip esthetic contouring instrument and a titanium, interproximal composite instrument. Before curing, mamelons and effects were added to the incisal third. This step was cured, and then a final layer of translucent insical shade microfill (Renamel® Microfill, Incisal Light; Cosmedent) was placed and contoured. Prior to a final light polymerization, a No. 2 artist's brush was used to help smooth and blend the final layer.
This protocol was modified and used to treat the remaining teeth (ie, Nos. 4 through 7 and Nos. 10 through 13), which required minimal to no incisal reduction. Because they were lingually inclined, no facial reduction was needed on the premolars; however, they required light facial preparation with a medium course diamond bur to remove the outer enamel layer. Although no opaque/white shade was used on teeth Nos. 6 and 11, because they were naturally darker than the other anterior teeth, the darker bleach shade microfill was used to block out the remaining tooth structure to reduce their overall value. For teeth Nos. 4, 5, 12, and 13, a greater depression was placed on the mesial and distal areas, leaving a slight mid-facial prominence built from the darker bleach shade, and a thicker layer of translucent insical shade microfill was placed over top of it to help reduce the overall value.6,7
Contouring and Finishing
Once the teeth were fully cured, the contouring and finishing process was completed in a series of steps. Finishing and polishing finalize the esthetics and help produce a long-lasting result.8 Gross contouring was accomplished using a 12-fluted carbide bur and fine diamond burs with a high-speed handpiece and course- and medium-grit discs with a low-speed, latch-type handpiece. The interproximal and gingival areas were finished using a scalpel blade (Bard-Parker®, No. 12; Aspen Surgical), and any interproximal polishing was accomplished using finishing strips and discs in medium, fine, and superfine grits (FlexiDisc®, Cosmedent). Facial line angles were marked to help achieve proper contouring and to indicate developmental depression areas on the facial surface (Figure 7). After gross contouring was completed, it was noted that there was insufficient incisal translucency. To improve it, a fine, flame shaped diamond bur (No. 8862 Fine, Brasseler USA) was used on the incisal third of teeth Nos. 8 and 9 and to a lesser degree on the lateral incisors, because the overall incisal translucency diminishes from the centrals to the cuspids. The area was then microabraded using 50-µm aluminum oxide, rinsed thoroughly, and dried. Next, the area was etched with 35% phosphoric acid for 15 seconds, rinsed, and lightly dried. The bonding agent was applied thoroughly and dried prior to being cured. To further enhance incisal translucency, a violet colored tint (IPS Empress® Direct Color, Ivoclar Vivadent) was applied and lightly spread using an explorer (Figure 8). This was then cured for 15 seconds, covered with layer of translucent insical shade microfill, contoured, and then cured again for 15 seconds at a high-intensity setting.
Any areas or voids that had to be repaired were first enlarged with a fine-grit diamond bur and then microetched using 50-µm aluminum oxide. These areas were then isolated, etched with 35% phosphoric acid, rinsed, and dried thoroughly. Following etching, the bonding agent was reapplied and cured completely. New resin was then placed and contoured appropriately. To help define the developmental depression areas, create some surface texture, and distinguish the three planes of facial contours, a fine, flame shaped diamond bur along with a medium-grit diamond bur were used on a very low speed setting. Prior to final finishing, the occlusion was checked and any necessary adjustments were made using a 12-fluted carbide bur in centric relation. Final finishing was completed using a combination of discs in medium, fine, and superfine grits as well as blue and pink polishing points (FlexiPoints, Cosmedent). The final high-gloss polish was accomplished with a felt disc and aluminum oxide polishing paste. At the conclusion of treatment, the occlusion of her nighttime appliance was checked as well and adjusted accordingly.
Conclusion
Overall, the patient was very pleased with her new smile for the first time in years (Figure 9 through Figure 13). Although her quest for a "whiter and brighter" smile had started with tooth whitening that never reached her goals and then bonding that was never completed due to life circumstances, finally, her smile could give her newfound confidence going forward.
Direct resin veneers can challenge even the most seasoned dental professionals. However, they help clinicians develop a keen eye for tooth contours, color, and anatomy as well as enhance their ability to handle and finish composite resin. Direct resin veneers also require clinicians to develop their creativity and incorproate artistry into their work, which is needed to optimally design each restoration and arrive at the patient's ideal smile.
References
1. Gordan VV, Garvan CW, Blaser PK, et al. A long-term evaluation of alternative treatments to replacement of resin-based composite restorations: results of a seven-year study. J Am Dent Assoc. 2009;140
(12):1476-1484.
2. Fahl N Jr. A polychromatic composite layering approach for solving a complex Class IV/direct veneer-diastema combination: part I. Pract Proced Aesthet Dent. 2006;18(10):641-646.
3. Fahl N Jr. A polychromatic composite layering approach for solving a complex Class IV/direct veneer/diastema combination: Part II. Pract Proced Aesthet Dent. 2007;19(1):17-22.
4. Sensi LG, Strassler HE, Webley W. Direct composite resins. Inside Dentistry. 2007;3(7):76.
5. Senawongse P, Pongprueksa P. Surface roughness of nanofill and nanohybrid resin composites after polishing and brushing. J Esthet Restor Dent. 2007;19
(5):265-275.
6. Arimoto A, Nakajima M, Hosaka K, et al. Translucency, opalescence and light transmission characteristics of light-cured resin composites. Dent Mater. 2010;26(11):
1090-1097.
7. Dietschi D. Layering concepts in anterior composite restorations. J Adhes Dent. 2001;3(1):71-80.
8. Peyton JH. Finishing and polishing techniques: direct composite resin restorations. Pract Proced Aesthet Dent. 2004;16(4):293-300.
About the Author
Jeff Lineberry, DDS, FAGD, FICOI, AAACD
Carolina Center for Comprehensive Dentistry
Mooresville, North Carolina