Digital Restorative Dentistry: Bringing Value to the Practice
Daniel J. Poticny, DDS
Now a multifaceted entity, digital restorative dentistry has fundamentally altered the dental industry for both dentists and laboratories. Over the past 30 years, the types of restorative materials available and the ways in which indirect restorations have been produced have changed dramatically. The use of metal has dropped to historic lows, with silica-based glass, polycrystalline, and resin-hybrid ceramics taking its place. Moreover, both dentists and laboratories have adopted digital technologies, which has enabled each to rapidly prototype restorations and provide consistent, controlled results while reducing labor costs for producing crowns, fixed partial dentures, implants, inlays, onlays, and veneers.1 Resin-hybrid ceramics, in particular, have emerged as the “modern dental materials,” which could not exist without CAD/CAM.2
With the properly trained clinician and adjunct dental team, the digital process may reduce risks associated with traditional analog restorative methods, which rely on dimensionally unstable and potentially incompatible materials that are subject to errors associated with their repeated manipulation. With a direct, virtual construction model, efficiency gains are definitively realized. The CAD/CAM-mediated process consists of a scan of the preparation quadrant/arch, its antagonist quadrant/arch, and a closed bite scan of the same to render an articulated virtual model. The restoration is designed virtually and directly using software tools to shape, form, and control occlusion for the desired restoration. When design is complete, the information is converted to a dataset, which is used by a milling device to grind or mill the desired restoration from a solid, monolithic, homogenous, industrially processed block that by definition describes modern dental materials. As such, the majority of the restoration is adhesively placed with exception/option for polycrystalline materials (eg, zirconia).
The origin for CAD/CAM laboratory techniques traces its heritage to the first commercial introduction of chairside millable ceramics in 1985. Although this was first described and prototyped as early as 1973 by Francois Duret,3 it was Dr. Werner Mörmann and Marco Brandestini who began work in 1980 leading to the first successful application in 1985 for the direct treatment of patients with CAD/CAM technology and silica glass-ceramic (Vita MK I and later Vita MK II, VITA Zahnfabrik, www.vita-zahnfabrik.com) uniquely within the context of a single patient visit without laboratory intervention.4,5 The initial system was limited to adhesively bonded inlays and onlays until 1996 when crown options were introduced. The acronym “CEREC,” or Chairside Economical Restoration of Esthetic Ceramics, became a brand name first used by Siemens AG (www.siemens.com) in 1987, then Sirona Dental Systems in 1997 (www.sirona.com), and currently, as of 2015, Dentsply Sirona (www.dentsplysirona.com).
Any Restoration Imaginable
With CEREC reporting over 35 million completed, high survival rate restorations having been produced and approximately 15% chairside CAD/CAM utilization by dentists in the United States for all available systems, the adoption of this technology will continue as an alternative to laboratory manufacture.6-8 CEREC set the initial standard for performance of these materials using the CAD/CAM process in terms of durability, predictability, and effectiveness in the treatment of teeth using the monoblock/monolithic principle.9-13 Numerous other manufacturers are now in the marketplace with chairside CAD/CAM systems, such as Planmeca/E4D Technologies (www.planmecacadcam.com), CS Restore (Carestream Dental, www.carestream.com), IOS FastScan (Glidewell Laboratories, www.glidewell.com), and others that combine a scanner with a choice of commercially available milling units for lab or chairside use, such as TrueDef intraoral scanner (3M Oral Care, www.3M.com), iTero (Align Technology (www.iTero.com), and 3Shape Trios (3Shape A/S, www.3shape.com). Lastly, the adoption of digital technologies is greater in laboratories today, even surpassing chairside utilization, owing to their productivity efficiencies and demand for CAD/CAM reliant materials.
Today, available chairside CAD/CAM platforms can, to one degree or another, produce virtually any dental restoration imaginable. The wide range of material offerings includes glass-ceramics, reinforced glass-ceramics, zirconia, polymer-ceramics, nanoceramics, resin-based composites, and polymethyl methacrylate (PMMA) materials. Long-term survival for CAD/CAM chairside-processed restorations, as mentioned, is well documented. Other factors, such as esthetic integration and morphology, while less of a factor in terms of performance, are desirable nonetheless and synonymous with the term “lab quality.” These parameters are conveniently achievable with willingness, proper training, case selection, and summary execution in the dental office.14 For those not interested in chairside fabrication, a dentist can choose to separate the digital imaging from chairside manufacturing, submitting a digital file to the laboratory for restoration fabrication. This digital file eliminates impression materials and in many cases can be performed by the laboratory without a physical model.
Minimizing Damage
With the many choices available in terms of platforms and materials, dentists considering the incorporation of a chairside CAD/CAM system have various factors to consider. For example, what is the best use for a chairside CAD/CAM system as it pertains to the types of restorations and materials the dentist will be employing? Are there best practice applications for chairside CAD/CAM that more than justify the rationale for integrating the system into the dental practice? While these questions can only be assessed individually, the potential of chairside CAD/CAM to both the patient and dentist may still lie within the framework that parallels the intent of the inventors: direct delivery of an esthetic, durable restoration using adhesive concepts that minimize amputation of precious tooth structure.
Despite the availability of reliable treatment options that involve less removal of tooth structure, single crowns are a staple of care in the United States when patients present with broken/fractured cusps and large fillings secondarily involved with decay.15 Generally speaking, however, minimally invasive dentistry is the preferred treatment paradigm, and today’s technology makes such practice more practical than ever. The versatility of adhesive and CAD/CAM technology allows for conservation of tooth structure; thus, a tooth may be preserved with a partial-coverage prosthesis instead of a full crown. Partial-coverage restorations produced by chairside CAD/CAM in stress-bearing posterior applications, as described in the following case, are known to have long-term success, and, more importantly, this approach may offer better long-term survival for the tooth itself.16,17
Case Report
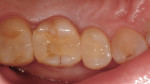
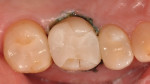
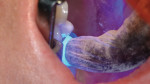
A 42-year-old woman initially presented with a defective composite restoration in tooth No. 3 with secondary carious involvement of the disto-lingual (DL) cusp (Figure 1). It was asymptomatic, vital, and absent of radiographic pathology. The patient desired an esthetic outcome; therefore, the clinician presented the following options: remove the existing restoration, perform core buildup, and place a full-contour, lab-fabricated, porcelain-veneered crown; or execute immediate and final treatment using the CEREC chairside CAD/CAM system (Dentsply Sirona).
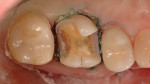
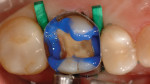
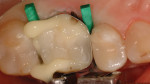
After discussion, the patient chose the chairside CAD/CAM procedure. At the start of treatment, an Isolite® isolation device (Isolite Systems, www.isolitesystems.com) was positioned comfortably as a means of field control for preparation and final placement. The existing restoration was then removed along with the involved DL cusp (Figure 2). The clinician considered the remaining residual tooth/cusp wall thickness and dentin support (2 mm)18,19 while following preparation principles for an indirect partial coverage restoration. Preparation principles involved a 2-mm reduction over the cusps and a 1.5-mm reduction in occlusally loaded fissures.20 Preparation geometries reflected smooth, rounded transitions devoid of sharp angles to reduce destructive tensile forces on ceramics and that are in accordance with the selected restorative material.21,22
A new class of millable materials offers the durability of ceramics with the favorable attributes of composite. The material used in this case was Lava™ Ultimate Restorative (3M, www.3m.com), which is a nanoceramic resin with excellent wear resistance, less abrasivity to opposing enamel than that of glass-ceramics, easy handling and surface finishing, and edge stability during milling for enhanced marginal adaptation.23,24 This material is an alternative to glass-ceramics because of its close approximation to the elastic modulus of teeth for improved fracture resistance but with less hardness than glass-ceramics.25 Margins are crisp and clean to facilitate imaging and enable optimal milling using the chairside CEREC Omnicam system (Dentsply Sirona).
A soft-tissue laser (Odyssey®, Ivoclar Vivadent, www.ivoclarvivadent.com) was used at 0.9 W to facilitate an unobstructed view of the margins, and a single 00 knitted cord soaked in ViscoStat® Clear (Ultradent Products, Inc., www.ultradent.com) aluminum-chloride solution was placed to control crevicular fluids. A final caries check was performed with Sable™ Seek® (Ultradent Products, Inc.) caries detection solution to ascertain complete removal of diseased dentin (Figure 2).
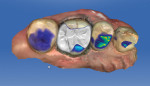
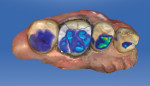
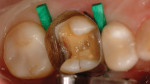
The CEREC Omnicam was used to scan the preparation into the design software (Figure 3 and Figure 4), and software proposals for the restoration were generated. These “proposals” are based on software analysis of the remaining intact preparation tooth structure, the surrounding dentition, and a morphologic library to generate the proposed, ideal statistical match. It is also virtually articulated to the opposing and neighboring teeth. The “proposals” are freely editable in any dimension using virtual tools, which in many ways emulate analog process through the addition or subtraction of material, reshaping, smoothing, or raising and lowering virtual surfaces. “Intuitiveness” of use is subjective and is often used in marketing these systems and will vary among them. Dentists and dental auxiliaries currently have varying levels of competence with both digital process and CAD/CAM materials. It should be noted that manufacturer- and distributor-dependent training for this and other systems is either mandatory or highly recommended to ensure rapid integration and predictable outcomes. In this instance, the assistant was trained to design with the clinician’s final approval prior to actual fabrication. The restoration was machined in the CEREC MC XL milling unit (Dentsply Sirona), recovered from the milling chamber, and after the Isolite was repositioned, dry-fitted to the preparation (Figure 5). Occlusion was pre-checked and adjusted. Immediately after the restoration was polished using a soft Abbott-Robinson® bristle brush with DiaShine® FS extraoral paste (VH Technologies, www.vhtechnologies.com), the intaglio surface was conditioned using air abrasion with aluminum oxide 30 µ, 2-bar pressure as required by the manufacturer.
A universal adhesive system (Scotchbond™ Universal Adhesive, 3M) with a complementary dual-cure adhesive resin cement (RelyX™ Ultimate, 3M) was used for cementation. This universal adhesive enables adhesion to all restorative materials and tooth structure.26 In the case of glass-ceramics and resin nanoceramics, silane in the adhesive’s formulation is needed to function as a priming agent/chemical coupler for adhesion to dissimilar surfaces (eg, tooth and restoration) with adhesive resin cement. The system used permits any desired etch mode, including total, selective, or self, to be utilized. Universal adhesives form effective bonds to dentin but less effective bonds to enamel because of higher pH values in these less acidic (compared to phosphoric acid) primers. Where present, enamel maximally benefits from phosphoric acid-etching as compared to the weaker acids found in the acidic primers for this class of product when used strictly in self-etch mode, thus optimizing enamel bonds and minimizing microleakage.27-29
A Tofflemire matrix band was wedged tightly below the proximal margin level as an optional aid to limit moisture contamination of the preparation to avoid contacting the soft tissues with acidic primers and adhesives, which often induce bleeding, and to limit the subgingival flow of the necessary adhesive resin cement, which all but eliminates time required for excess cement removal and subsequent margin finishing subgingivally (Figure 6). Adhesive (Scotchbond Universal) was applied to the restoration intaglio to chemically prime the restoration (dental assistant function) with simultaneous application to the preparation (dentist function) (Figure 7). Application to the tooth was performed using a scrubbing motion over the preparation surfaces for 20 seconds followed by air-thinning to evaporate the solvent and to sufficiently thin the adhesive; this was immediately followed by light-curing for 10 seconds.
RelyX Ultimate adhesive dual-cure cement was then syringed into the preparation, and the restoration was seated with the clinician noting consistent cement outflow from all margins. Excess was removed with a cotton-tipped applicator, which was easily facilitated by the matrix band (Figure 8).
The restoration was light-cured occlusally, two times for 20 seconds each (Figure 9). The band was then removed and curing was done buccally and lingually for 20 seconds each. The matrix band effectively eliminated the need for cured excess removal cervically, thereby greatly simplifying post-insertion cleanup. The cavosurface margins were finished with a 20-µ, 368-016 pointed football-shaped diamond, occlusion was reconfirmed, and touch-up polishing was performed with a soft, disposable prophy brush (Crescent Dental, www.crescentdental.com) with DiaShine intraoral polishing paste.
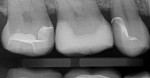
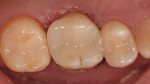
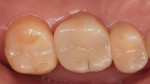
A postoperative radiograph was taken to assess integrity and the presence of excess cement (Figure 10). Immediate postoperative results and 2-week follow-up are depicted in Figure 11 and Figure 12, respectively.
Conclusion
Chairside systems will continue to evolve in terms of ease-of-use and their overall capabilities. With dentists now relying more on the use of silica glass, polycrystalline, and polymer ceramics, chairside CAD/CAM will continue to grow, recognizing it is not the sole realm of the dental laboratory. Like any new treatment modality, education and training is of paramount importance, particularly as it applies to revisitation of the potential of minimally invasive concepts, material applications, adhesion dentistry, and a novel way to control all aspects of restoration design in-house without the aid of a laboratory utilizing a true dental team approach. Digital process can only be as good as the operator, which is no different from the analog approach. In this clinical example, the entire procedure—a suitable alternative to a full-contour crown—was completed in less than 1 hour from the onset of anesthesia, maximizing time to the benefit of all. The restorative technique fulfilled the principles of defect-oriented treatment, leveraging adhesive dentistry and modern materials as opposed to the more traditional mechanical approach. Lastly and most importantly, when considering the enhanced capabilities of these systems today, it is clear how much overlooked value still resides in the same treatment modality, which was its only capability some 30 years ago.
References
1. Pigliacelli S. The future of the dental lab industry: The lab industry ain’t never gonna be the same. Dental Economics website. http://www.dentaleconomics.com/articles/print/volume-105/issue-7/macroeconomics/the-future-of-the-dental-lab-industry-the-lab-industry-ain-t-never-gonna-be-the-same.html. Accessed May 27, 2016.
2. Martino A. The shifting production of crowns and bridges. Dental Products Report website. http://www.dentalproductsreport.com/lab/article/shifting-%C2%ADproduction-crowns-and-bridges. Accessed May 23, 2016.
3. Duret F, Preston JD. CAD/CAM imaging in dentistry. Curr Opin Dent. 1991;1(2):150-154.
4. Mörmann WH. The evolution of the CEREC system. J Am Dent Assoc. 2006;137(suppl):7S-13S.
5. Mörmann WH. The origin of the Cerec method: a personal review of the first 5 years. Int J Comput Dent. 2004;7(1):11-24.
6. CEREC Much More Than Restorative. Sirona USA website. http://www.sironausa.com/ecomaXL/files/A91100-M43-B880-01-7600.pdf&download=1. Accessed May 27, 2016.
7. Poticny DJ, Klim J. CAD/CAM in-office technology: innovations after 25 years for predictable, esthetic outcomes. J Am Dent Assoc. 2010;141(suppl2):5S-9S.
8. Fasbinder DJ. Digital dentistry: innovation for restorative treatment. Compend Contin Educ Dent. 2010;31(spec no. 4):2-11.
9. Fasbinder DJ. Materials for chairside CAD/CAM restorations. Compend Contin Educ Dent. 2010;31(9):702-709.
10. Posselt A, Kerschbaum T. Longevity of 2328 chairside Cerec inlays and onlays. Int J Comput Dent. 2003;6(3):231-248.
11. Otto T, De Nisco S. Computer-aided direct ceramic restorations: a 10-year prospective clinical study of Cerec CAD/CAM inlays and onlays. Int J Prosthodont. 2002;15(2):122-128.
12. Martin N, Jedynakiewicz NM. Clinical performance of CEREC ceramic inlays: a systematic review. Dent Mater. 1999;15(1):54-61.
13. Reiss B, Walther W. Survival analysis and clinical evaluation of CEREC restorations in a private practice. In: Mörmann WH, ed. Proceedings of the International Symposium on Computer Restorations. The State of the Art of the Cerec-Method. Berlin, Germany: Quintessence Publishing; 1991:215.
14. Kollmuss M, Kist S, Goeke JE, et al. Comparison of chairside and laboratory CAD/CAM to conventional produced all-ceramic crowns regarding morphology, occlusion, and aesthetics. Clin Oral Investig. 2016;20(4):791-797.
15. Christensen GJ. Has tooth structure been replaced? J Am Dent Assoc. 2002;133(1):103-105.
16. Hickel R, Manhart J. Longevity of restorations in posterior teeth and reasons for failure. J Adhes Dent. 2001;3(1):45-64.
17. Arnetzl GV, Arnetzl G. Reliability of nonretentive all-ceramic CAD/CAM overlays. Int J Comput Dent. 2012;15(3):185-197.
18. Blank JT. Scientifically based rationale and protocol for use of modern indirect resin inlays and onlays. J Esthet Dent. 2000;12(4):195-208.
19. Stawarczyk B, Liebermann A, Eichberger M, Güth JF. Evaluation of mechanical and optical behavior of current esthetic dental restorative CAD/CAM composites. J Mech Behav Biomed Mater. 2016;55(3):1-11.
20. Lava™ Ultimate: Technical Product Profile. 3M website. http://multimedia.3m.com/mws/media/747392O/lava-ultimate-restorative-instructions-for-use-english.pdf. Accessed May 27, 2016.
21. Arnetzl GV, Arnetzl G. Biomechanical examination of inlay geometries—is there a basic biomechanical principle? Int J Comput Dent. 2009;12(2):119-130.
22. Arnetzl GV, Arnetzl G. Design of preparations for all-ceramic inlay materials. Int J Comput Dent. 2006;9(4):289-298.
23. Zhi L, Bortolotto T, Krejci I. Comparative in vitro wear resistance of CAD/CAM composite resin and ceramic materials. J Prosthet Dent. 2016;115(2):199-202.
24. Fasbinder DJ, Neiva GF. Surface evaluation of polishing techniques for new resilient CAD/CAM restorative materials. J Esthet Restor Dent. 2016;28(1):56-66.
25. Albero A, Pascual A, Camps I, Grau-Benitez M. Comparative characterization of a novel cad-cam polymer-infiltrated-ceramic-network. J Clin Exp Dent. 2015;7(4):e495-e500.
26. Scotchbond™ Universal Adhesive: Technical Product Profile. 3M website. http://multimedia.3m.com/mws/media/754751O/scotchbond-universal-adhesive-technical-product-profile.pdf. Accessed May 23, 2016.
27. Swift EJ. Critical appraisal. Options for dentin/enamel bonding: part IV. J Esthet Restor Dent. 2010;22(4):270-275.
28. Takamizawa T, Barkmeier WW, Tsujimoto A, et al. Influence of different etching modes on bond strength and fatigue strength to dentin using universal adhesive systems. Dent Mater. 2016;32(2):e9-e21.
29. Rosa WL, Piva E, Silva AF. Bond strength of universal adhesives: A systematic review and meta-analysis. J Dent. 2015;43(7):765-776.
About the Author
Daniel J. Poticny, DDS
Adjunct Clinical Associate Professor
University of Michigan
School of Dentistry
Ann Arbor, Michigan