Convenient Cleanup and Consistent Cementation for Optimal Restorations
New self-adhesive resin cement offers clinical advantages
Jason H. Goodchild, DMD
All indirect restorations must be cemented for final delivery into the patient’s mouth, but selecting the optimal cement for each clinical situation is challenging. Factors that must be considered include: remaining dentin and enamel, preparation design, required bond strength, restorative material (substrate), ability to isolate the field, and esthetics.
For many years, the majority of indirect restorations included cast metal and cementation with zinc phosphate cement or zinc polycarboxylate cement. However, both cements have limitations that are clinically significant.
Introduced in 1879, zinc-phosphate cement contains phosphoric acid and the exothermic setting reaction can cause postoperative sensitivity. Additionally, it does not chemically adhere to the tooth and it is soluble intraorally. Introduced in 1968, zinc-polycarboxylate cement offers adhesion to the tooth and a setting reaction that is less exothermic but, unfortunately, also causes pulpal irritation and is soluble intraorally.1
While both zinc-phosphate cement and zinc-polycarboxylate cement are still available, they have largely been replaced by four major cement categories: glass-ionomer cement (GIC), resin-modified glass-ionomer cement (RMGIC), self-adhesive resin cement (SARC), and adhesive resin cement (ARC).
First introduced in 2002 and the newest of the four major categories, SARC is designed to offer procedural and clinical advantages over the other categories. The ease of use of SARC is similar to GIC and RMGIC but provides higher bond strengths, improved esthetics, and dual curing. Also, because SARC is resin-based, it can be used for cementation of glass-ceramics (eg, lithium silicates) where GIC and RMGIC are usually not recommended. Compared to adhesive resin cements, SARC does not require an additional bonding step; however, both require isolation for effective use.
Some of the other potential clinical advantages of SARC are:
• SARC has better physical properties compared to conventional cements.2,3
• The dispensing and handling of SARC is easy. Several formulations of SARC exist including capsules, hand-mixed paste-paste, and automix paste-paste.4
• SARC is self-adhesive without pretreatment of the prepared tooth and requires no additional bonding step. Because multiple-step adhesive resin cements are technique-sensitive, the single-step application of SARC is a viable alternative for glass-ceramic and zirconia restorations.5,6
• SARC generates a bond similar to that of adhesive resin cements on dentin.7 However, for maximum performance on enamel, using a selective enamel etching technique with 37% phosphoric acid is ideal.8-10 In this case, enamel margins should be etched for 15 seconds followed by water rinsing to completely remove the acid.
• SARC is dual-cured. The setting reaction of SARC can be initiated both chemically (self-cure) and by light exposure (light-curing). Interestingly, the degree of conversion of monomers to polymers will influence the performance of SARC. An immediate higher degree of conversion, improved mechanical properties, and decreased solubility can be achieved if SARC is activated via dual-curing. Clinically, this can be achieved first by tack-curing the material and cleaning excess cement within a gel phase window (ie, within the working time of the material) followed by definitive light-curing of 20 seconds per surface.11,12
• SARC is associated with a low incidence of postoperative sensitivity.13-16 Compared to the classic total-etch technique of adhesive cementation, the misuse or overuse of phosphoric acid can remove the smear layer, open dentinal tubules, and create a pathway for bacteria and monomers to penetrate the pulp.17 In general, self-adhesive resin cements have less influence on the dental pulp than other cement categories.6,18
SARC Challenges
Despite the advantages of SARC, a possible clinical challenge is removing all excess cement to prevent postoperative problems. Many dentists tack-cure resin cements to initiate a gel phase during which the material can be easily removed with an explorer or hand instrument. However, some existing products have a very small window for tack-curing, allowing the dentist only 1 to 2 seconds of light-curing before the material cannot be removed with a hand instrument. In this case, the hardened material must be removed with a bur, which can be very difficult and messy, especially in the posterior interproximal areas.
To help dentists prevent over-curing during this critical phase, Dentsply Sirona Restorative (www.dentsply.com) has introduced Calibra® Universal Self-Adhesive Resin Cement. This newly introduced self-adhesive resin cement offers a wide tack-cure window of up to 10 seconds (ie, 5 seconds buccal and 5 seconds lingual) and an extended 45-second gel phase. This means that dentists can now benefit from the convenience of tack-curing without the stress of over-curing, allowing enough time to thoroughly remove excess cement and avoid using a bur that could traumatize surrounding gingiva and damage the new restoration.
The indications for Calibra® Universal include use with endodontic posts, metal crowns and porcelain-fused-to-metal (PFM), alumina and zirconia crowns, and with all-ceramic restorations, all without the need for a separate bonding step. With a choice of five shades featuring Shade Stable™ technology to virtually eliminate shade shifting over time, the patient and dentist can be assured of long-lasting restorations.
Clinical Case
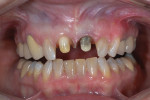
A 52-year-old woman presented for replacement of PFM crowns on teeth Nos. 8 and 9. After verifying the patient’s medical history and administering one cartridge of 4% Articadent™ DENTAL with epinephrine 1:100,000 (Dentsply Sirona) via buccal and palatal infiltration, the existing crowns were removed. The preparations were refined with a Midwest® ONCE™ tapered flat-end diamond bur (Dentsply Sirona Restorative) on high speed (Figure 1). A final impression was captured in a one-step, two-viscosity technique using Aquasil Ultra Smart Wetting® Impression Material (Dentsply Sirona Restorative). The preparations were then provisionalized using Integrity® Multi-Cure Temporary Crown and Bridge Material and Integrity® Temp Grip Temporary Crown and Bridge Cement (Dentsply Sirona Restorative).
Approximately 3 weeks later, the patient returned for final delivery of lithium-silicate crowns on teeth Nos. 8 and 9. The provisionals were removed and the excess cement was cleaned. The crowns were adjusted for interproximal contacts, occlusion, and esthetics. The intaglio of the restorations were pretreated with Porcelain Etchant 9.5% hydrofluoric acid (BISCO, www.bisco.com) followed by Calibra® Silane Coupling Agent (Dentsply Sirona Restorative) according to manufacturer’s instructions.
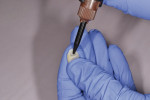
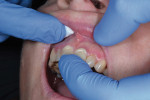
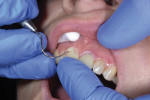
The Calibra® Universal Self-Adhesive Resin cement opaque shade was prepared for use by bleeding the dual-barrel automix syringe prior to attaching a mix tip to ensure both base and catalyst were expressing evenly. Then, the mix tip was installed and a small amount of material was dispensed onto a mixing pad to again ensure adequate mix of the cement components. A thin, uniform layer of cement was dispensed onto the entire internal surface of the restoration directly from the mixing tip (Figure 2). The crowns were then immediately seated onto the cleaned and slightly moist preparations (Figure 3).
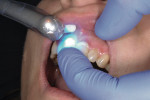
The buccal and palatal aspects of the restoration were tack-cured for 5 seconds using a SmartLite® Focus® Pen-Style LED Curing Light (Dentsply Sirona Restorative), initializing a gel phase (Figure 4). The cement was gently removed using an explorer; great care was taken to avoid causing gingival bleeding (Figure 5). Interproximal excess was removed by stabilizing the restorations and flossing the areas, horizontally removing the floss after each area was verified.
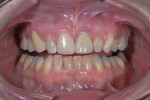
After successful removal of excess cement, the restorations received a 20-second light-curing from the buccal, palatal, and incisal. Final verification of interproximal contacts, occlusion, and esthetics was completed and the patient was released (Figure 6).
Conclusions
SARCs can offer clinical advantages over other cement categories. In clinical situations where the preparation has sufficient crown height, is not over-tapered, and can be isolated from contamination, SARCs offer convenience without sacrificing strength and esthetics. Calibra Universal offers an extended gel phase when used in both the light-activated and self-cure modes for indirect restorations. As a result, clinicians can now better leverage SARC technology without the stress of cleaning up excess cement.
Disclosure
Jason H. Goodchild, DMD, is an employee of Dentsply Sirona Restorative.
References
1. Rosenstiel SF, Land MF, Crispin BJ. Dental luting agents: a review of the current literature. J Prosthet Dent. 1998;80(3):280-301.
2. Burgess JO, Ghuman T, Cakir D. Self-adhesive resin cements. J Esthet Restor Dent. 2010;22:412-419.
3. Ferracane JL, Stansbury JW, Burke FJ. Self-adhesive resin cements—chemistry, properties and clinical considerations. J Oral Rehabil. 2011;38(4):295-314.
4. Makkar S, Malhotra N. Self-adhesive resin cements: a new perspective in luting technology. Dent Update. 2013;40(9):758-768.
5. Zorzin J, Belli R, Wagner A, et al. Self-adhesive resin cements: adhesive performance to indirect restorative ceramics. J Adhes Dent. 2014;16(6):541-546.
6. Weiser F, Behr M. Self-adhesive resin cements: a clinical review. J Prosthodont. 2015;24(2):100-108.
7. Rodrigues RF, Ramos CM, Francisconi PA, Borges AF. The shear bond strength of self-adhesive resin cements to dentin and enamel: an in vitro study. J Prosthet Dent. 2015;113(3):220-227.
8. Behr M, Hansmann M, Rosentritt M, Handel G. Marginal adaptation of three self-adhesive resin cements vs. a well-tried adhesive luting agent. Clin Oral Investig. 2009;13(4):459-464.
9. De Munck J, Vargas M, Van Landuyt K, et al. Bonding of an auto-adhesive luting material to enamel and dentin. Dent Mater. 2004;20(10):963-971.
10. Duarte S Jr, Botta AC, Meire M, Sadan A. Microtensile bond strengths and scanning electron microscope evaluation of self-adhesive and self-etch resin cements to intact and etched enamel. J Prosthet Dent. 2008;100(3):203-210.
11. Aguiar TR, de Oliveira M, Arrais CA, et al. The effect of photopolymerization on the degree of conversion, polymerization kinetic, biaxial flexure strength, and modulus of self-adhesive resin cements. J Prosthet Dent. 2015;113(2):128-134.
12. da Silva Fonseca AS, Mizrahi J, Menezes LR, et al. The effect of time between handling and photoactivation on self-adhesive resin cement properties. J Prosthodont. 2014;23(4):302-307.
13. Piwowarczyk A, Schick K, Lauer HC. Metal-ceramic crowns cemented with two luting agents: short-term results of a prospective clinical study. Clin Oral Investig. 2012;16(3):917-922.
14. Azevedo CG, De Goes MF, Ambrosano GM, Chan DC. 1-year clinical study of indirect resin composite restorations luted with a self-adhesive resin cement: effect of enamel etching. Braz Dent J. 2012;23 (2):97-103.
15. Blatz MB, Mante FK, Saleh N, et al. Postoperative tooth sensitivity with a new self-adhesive resin cement—a randomized clinical trial. Clin Oral Investig. 2013; 17(3):793-798.
16. Shetty RM, Bhat S, Mehta D, et al. Comparative analysis of postcementation hypersensitivity with glass ionomer cement and a resin cement: an in vivo study. J Contemp Dent Pract. 2012;13(3):327-331.
17. Saad Del-D, Atta O, El-Mowafy O. The postoperative sensitivity of fixed partial dentures cemented with self-adhesive resin cements: a clinical study. J Am Dent Assoc. 2010;141(12):1459-1466.
18. Manhart J, Chen H, Hamm G, Hickel R. Buonocore Memorial Lecture. Review of the clinical survival of direct and indirect restorations in posterior teeth of the permanent dentition. Oper Dent. 2004;29(5):481-508.
For more information, contact:
Dentsply Sirona Restorative
800-532-2855
www.calibracement.com
About the Author
Jason H. Goodchild, DMD
Clinical Associate Professor
Department of Oral Medicine
University of Pennsylvania School of Dental Medicine
Philadelphia, Pennsylvania
Clinical Education Manager
Dentsply Sirona Restorative
Milford, Delaware
Private Practice
Havertown, Pennsylvania