3D Imaging in the Digital Workflow
Essential diagnostic tools for effective treatment planning
Scott D. Ganz, DMD
Although implant dentistry has evolved into one of the most predictable treatment alternatives for patients who are missing teeth,1 we are still striving to improve our surgical and restorative techniques. The foundation for all procedures should be a proper diagnosis to determine the appropriate treatment options. It is generally understood that two-dimensional (2D) periapical and panoramic radiography have limitations due to inherent distortion factors and cannot accurately communicate the three-dimensional (3D) spatial anatomy of adjacent vital structures.2,3 A lack of the right information in the diagnostic and treatment planning phases can lead to both surgical and restorative complications.
Implant Planning and Beyond
To help take the guesswork out of the diagnostic phase, 3D imaging modalities were first introduced through medical-grade computed tomography (CT), although it was originally very expensive with a high level of radiation exposure. Over the past 15 years, the initial catalyst for improving the accuracy of dental implant placement was the introduction and proliferation of cone-beam computed tomography (CBCT) imaging devices and improvements with interactive treatment planning software, such as Simplant® (DENTSPLY Implants, www.dentsplyimplants.com), NobelClinician® (Nobel Biocare, www.nobelbiocare.com), Invivo5 (Anatomage, www.anatomage.com), TxStudio™ (i-CAT, www.i-cat.com), coDiagnostiX™ (Dental Wings, www.codiagnostix.com), Planmeca Romexis® (www.planmeca.com), and Blue Sky Plan (BlueSkyBio, https://blueskybio.com).
CBCT has greatly impacted the clinician’s ability to diagnose in all dimensions,4 not just for dental implants but also as a cross-specialty tool for a variety of patient procedures. Clinicians who have moved from 2D to 3D imaging have gained a full appreciation of individual, patient-specific anatomy.
Specific to dental implants, clinicians now have a clear understanding of the existing quantity and quality of bone, trajectory of the alveolus, and location of vital structures aiding in educated decisions regarding treatment alternatives. 3D imaging also serves as a powerful communication tool for patients, colleagues, and dental laboratory technicians.
Digital Workflow for Implants
If clinicians wish to achieve the ideal goal of prosthetically driven implant reconstruction, there needs to be a complete understanding of the relationship between the tooth and the underlying bone.4,5 In addition, proper diagnosis may require certain prosthetic steps prior to the CBCT scan. The ideal pre-surgical workflow should include conventional impressions and mounted articulated study casts.6 A diagnostic wax-up can be utilized to fabricate a radiopaque scanning template or one containing fiducial markers, to be worn by the patient during the scan acquisition. Therefore, “it’s not the scan, it’s the plan” becomes the driving force in the new digital workflow.
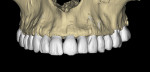
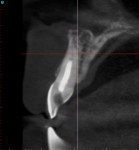
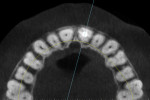
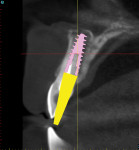
When a tooth is fractured or requires extraction, a dental implant is the only treatment option that will restore the root of the tooth, which can provide support for a new clinical crown. A CBCT scan can provide an accurate 3D-reconstructed volume as an aid in planning for an implant-supported restoration (Figure 1). The cross-sectional image reveals the precise location of the root within the alveolus, provides information on bone density, and shows that the tooth had previous root canal therapy (Figure 2). The axial image is important to help determine the morphology of the tooth root based upon the inferior-superior location of the slice (Figure 3). Depending on the interactive treatment planning software, the use of realistic manufacturer-specific virtual implants of known length and diameter can be simulated within the receptor site (Figure 4). The yellow projection is a helpful tool to aid the clinician in establishing the proper trajectory of the implant within the cross-sectional image and in relation to the desired restorative option (ie, screw- or cement-retained). It should be noted that this is only one slice, and that the final positioning of the implant should be determined only after all views have been considered.
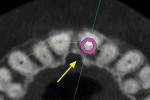
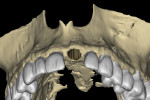
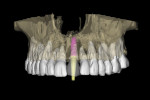
Recent software developments allow for a simulated implant to be visualized in the axial view in close proximity to the incisal canal (yellow arrow), and the periodontal ligament space of the adjacent tooth roots (Figure 5). Using advanced software features and the process of segmentation, the existing tooth root can be virtually extracted, leaving the remaining alveolus to be inspected (Figure 6). The use of “selective transparency” provides the necessary information regarding positioning the implant and avoiding the adjacent tooth roots (Figure 7). The proposed implant with an abutment projection can then be positioned to emerge through the desired restorative result, linking the implant to the envelope of the tooth.
The digital workflow has become more of a reality now that a great majority of dental laboratories have updated their equipment and knowledge of software-driven CAD/CAM technologies.7 Another recent catalyst has been the proliferation of desktop optical scanning devices for dental laboratories, followed by the introduction of in-office intraoral optical scanners for the clinician. Optical scanning devices now play a significant role in acquiring improved surface detail such as from a stone cast that can be merged with the data from the CBCT dataset, enhancing the accuracy of the planning software.8
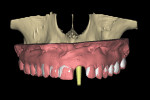
Utilization of a digitized diagnostic wax-up or duplicate of a patient’s denture scanning appliance provides an unparalleled ability to visualize the relationship between the desired tooth and the underlying bone. The virtual implant can then be positioned within the receptor site to fit within the envelope of the desired restoration. It is essential to place a virtual abutment or an abutment “projection” with an appropriate vertical height to visualize the spatial positioning of the abutment as it relates to the tooth to achieve restoratively driven outcomes (Figure 8). Once the implant position has been finalized, a surgical guide can then be fabricated, facilitating proper implant placement (Figure 9). Precise and accurate templates can be fabricated by either CAD/CAM or 3D printing technologies, which are becoming much more affordable for both dental laboratories and clinicians.
Conclusion
Today’s sophisticated CBCT scan devices have become indispensable diagnostic tools when combined with interactive treatment planning software applications. However, many clinicians are still not confident in their abilities to diagnose and plan in 3D. Some also do not have time to learn sophisticated software. Fortunately, clinicians can now feel confident in bringing the world of 3D imaging to their patients through many third-party entities that exist today, including dental laboratories and imaging centers who are equipped with the knowledge and software expertise to guide clinicians through the maze of technology. Currently, it is the synergy and merging of the various digital technologies that have become the focus and catalyst for significant behavioral change, all based on the initial data provided by CBCT imaging.
References
1. Ganz SD. Dental implantology: an evolving treatment modality. Compend Contin Educ Dent. 2013;34(8):628-629.
2. Angelopoulos C, Aghaloo T. Imaging technology in implant diagnosis. Dent Clin North Am. 2011;55(1):141-158.
3. Ganz SD. Computer-aided design/computer-aided manufacturing applications using CT and Cone Beam CT scanning technology. Dent Clin North Am. 2008;52(4):777-808.
4. Scherer MD. Presurgical implant-site assessment and restoratively driven digital planning. Dent Clin North Am. 2014;58(3):561-595.
5. Rinaldi M, Ganz SD, Mottola A. Computer-Guided Applications for Dental Implants, Bone Grafting, and Reconstructive Surgery. St. Louis, MO: Elsevier; 2015.
6. Ganz SD. Computer-aided design/computer-aided manufacturing applications using CT and Cone Beam CT scanning technology. Dent Clin North Am. 2008;52(4):777-808.
7. Ganz SD. Three-dimensional imaging and guided surgery for dental implants. Dent Clin North Am. 2015;59(2):265-290.
8. Lee CY, Ganz SD, Wong N, Suzuki JB. Use of cone beam computed tomography and a laser intraoral scanner in virtual dental implant surgery: part 1. Implant Dent. 2012;21(4):265-271.