The Diode Laser as an Adjunct to Implant Treatment
Safe cutting and hemostasis for improved workflow and outcomes
Diode lasers are a useful adjunct to soft-tissue modification to uncover dental implants or esthetically recontour the gingival margin. They provide better safety than electrosurgery, as they maintain a temperature profile within the safety zone of bone and do not cause tissue shrinkage, which can affect the esthetic outcome. One clear advantage of diode lasers over the use of a scalpel or tissue punch is their ability to provide simultaneous cutting and coagulation (hemostasis). This has a further benefit of allowing immediate impressions to be taken without site bleeding affecting the accuracy of the capture of the soft-tissue contours and position.
Issues with Scalpels and Electrosurgery
To initiate the prosthetic phase of treatment, soft tissue can be modified to uncover dental implants using several methods. Traditionally, a cutting instrument (ie, scalpel or tissue punch1) is used to incise through the soft tissue to the underlying implant. This results in a bleeding edge that can cause postoperative sensitivity and hamper the accuracy of how the soft tissue is captured in impressions, which could otherwise be taken at the same appointment. For traditional site preparation, this means a 2-week delay for healing of soft tissue.
Electrosurgery, which cauterizes cut edges and decreases postoperative bleeding, can be used as an alternative to the blade. However, a general recommendation is to avoid electrosurgery units in and around dental implants. Because electrosurgery requires a circuit to be formed between the monopolar tip intraorally and the surgical unit, a grounding plate is placed on the patient a distance from the oral cavity. When activated, current flows between the electrosurgery tip through the soft tissue to the grounding plate, completing the circuit with the metallic implant conducting the current along the path.2 It has been reported that temperature increases over a threshold of 10°C at the osseous interface with the implant may lead to bone loss and possible de-integration of the implant. Electrosurgery also affects cell layers deep below the surface, and combined with the temperature increase, tissue shrinkage is often reported.3 This necessitates a delay between uncover and impressions so that the gingival margin captured is stable when the prosthetic is returned for insertion.
Diode Laser Advantages
Diode lasers are becoming increasingly utilized in dental practices, both because they are less expensive to implement than CO2 and ND:YAG lasers and due to the wide range of effective treatments afforded by these devices. Diode lasers such as the Picasso (AMD Lasers, www.amdlasers.com) provide sufficient power to modify soft tissue in and around the dental implant for uncovery or alteration of the gingival margin to improve the esthetics while operating within the temperature range recommended to avoid negatively affecting bone around the implant.4 Additionally, coagulation can be controlled, allowing impressions to be taken at the time of uncovery without fear of blood interfering with the accuracy of the gingival aspect of the impression. Because, unlike with an electrosurgery unit, cutting the tissue with the diode does not affect deep layers of cells in the gingiva, tissue shrinkage is not a concern; therefore, it is not necessary for gingival healing to be complete before impressions can be taken.5-9
Case Presentation
A 30-year-old female patient presented with severely malposed maxillary central incisors tipped facially and a desire for esthetic improvement. Cone-beam computed tomography revealed minimal bone was present over the facial of the central incisors. Options for treatment presented to the patient included orthodontics to correct esthetics or extraction of the central incisors followed by placement of implants at these sites and restorations on the anterior teeth. The patient indicated that she did not wish to pursue an orthodontic treatment option due to the time involved.
The patient presented for surgery and the central incisors were atraumatically extracted under local anesthetic. The adjacent teeth were prepared for crowns, which would support a provisional bridge during the healing/integration period. A 4-mm-wide 24° co-axis implant (Keystone Dental, www.keystonedental.com) was placed into the osteotomy at each central incisor, orienting the prosthetic axis to a vertical position while the implant’s body followed the trajectory of the premaxilla. Use of the Co-Axis implant allowed angulation of the implant placement to fit within the triangle of bone in the premaxilla and direct the prosthetic axis to a restorable position. A healing screw was placed and osseous graft material (NovaBone, www.novabone.com) placed on the facial to thicken the resulting bone. The soft tissue was closed with resorbable PGA sutures. A stent created over the wax-up of the study models that had been modified was filled with an auto-cure provisional resin (Perfectemp® 10, DenMat, www.denmat.com) and seated over the anterior and allowed to set. Upon setting, the stent with provisional was removed intraorally and trimmed and polished. The material at the implant sites was shaped to a bullet shape to assist in forming an emergence profile in the soft tissue and preserve the papillas.
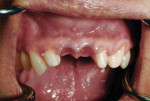
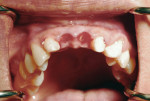
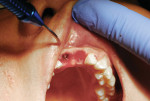
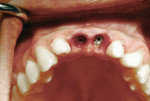
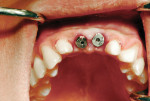
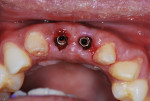
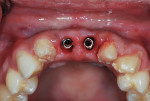
Six months after implant placement, the provisional bridge was removed, and preservation of the papillas was confirmed with a natural emergence profile within soft tissue (Figure 1 and Figure 2). Local anesthetic was administered. The Picasso diode laser was set at 2.5 W in continuous mode with an initiated tip. At the center of the depression in the soft tissue above the first implant’s cover screw, the laser was used in a circular motion, moving outward until the entire cover screw was exposed (Figure 3). The process cut the desired soft tissue and coagulated any bleeding from the cut edges. This was then repeated on the second implant (Figure 4). Open-tray implant impression abutments were placed into the implants and seating was verified radiographically. An impression of the maxillary arch was taken with Aquasil Ultra heavy body (DENTSPLY Caulk, www.aquasilultra.com) in a Miratray Implant Advanced impression tray (Hager Worldwide, www.hagerworldwide.com). Aquasil Ultra was syringed around the preparations and implant abutment heads. Healing abutments were reinserted into the implants (Figure 5) and the previously placed provisional bridge was then luted with a provisional cement ( GC Fuji TEMP LT™, GC America, www.gcamerica.com).
Two weeks later, the prosthetics returned from the laboratory (DenMat Labs) and the provisional bridge was removed. When the healing abutments were removed, the soft tissue demonstrated a lack of inflammation and good periodontal health where it had been modified by the diode laser (Figure 6 and Figure 7). Custom CAD/CAM milled abutments were inserted into the implants at the central incisors and a radiograph was taken to verify mating of the abutments to the implants. A torque wrench was used to tighten the fixation screws on the implants to 30 ncm. Ceramic crowns were tried in on teeth nos. 7-11 and were luted with PANAVIA™ SA resin cement (Kuraray Noritake Dental Inc, www.kuraraynoritake.com). Occlusion was checked and adjusted where needed.
Conclusion
This case illustrates several of the advantages of using diode lasers as an adjunct to implant treatment. Diode lasers are an efficient and effective option when modifying soft tissue, uncovering dental implants, or esthetically recontouring the gingival margin. Unlike electrosurgery, they maintain a temperature profile within the safety zone of bone and do not cause tissue shrinkage, which can affect the esthetic outcome. When compared with traditional methods such as a scalpel or tissue punch, diode lasers have the advantage of offering hemostasis, meaning impressions can be taken immediately without site bleeding affecting the accuracy of the capture of the soft tissue contours and position. This reduces chairtime and improves the efficiency of implant procedures while offering excellent outcomes.
Disclosure
Dr. Kurtzman received an honorarium from AMD Lasers for the preparation of this article.
About the author
Gregori M. Kurtzman, DDS, MAGD, DICOI, DADIA
Private Practice
Silver Spring, Maryland
For more information, contact:
AMD Lasers
866-999-2635
www.amdlasers.com
References
1. Zetz MR, Quereshy FA. Single-stage implant surgery using a tissue punch. J Oral Maxillofac Surg. 2000;58(4):456-457.
2. Wilcox CW, Wilwerding TM, Watson P, Morris JT. Use of electrosurgery and lasers in the presence of dental implants. Int J Oral Maxillofac Implants. 2001;16(4):578-582.
3. Goharkhay K, Moritz A, Wilder-Smith P, et al. Effects on oral soft tissue produced by a diode laser in vitro. Lasers Surg Med. 1999;25(5)401-406.
4. Gherlone EF, Maiorana C, Grassi RF, et al. The use of 980-nm diode and 1064-nm Nd:YAG laser for gingival retraction in fixed prostheses. J Oral Laser Applications. 2004;4(3):183-190.
5. El-Kholey KE. Efficacy and safety of a diode laser in second-stage implant surgery: a comparative study. Int J Oral Maxillofac Surg. 2014;43(5):633-638. doi:10.1016/j.ijom.2013.10.003.
6. van As G. Uncovering the tooth: the diode laser to uncover teeth, brackets and implants. Dent Today. 2012;31(1):168.
7. Yeh S, Jain K, Andreana S. Using a diode laser to uncover dental implants in second-stage surgery. Gen Dent. 2005;53(6):414-417.
8. van As G. The diode laser—The diode laser in second stage implant recovery. Dent Today. 2011;30(9):144.
9. Deppe H, Horch HH. Laser applications in oral surgery and implant dentistry. Lasers Med Sci. 2007;22(4):217-221.