Innovations in Ceramics
Milled options are becoming stronger, more translucent
The art and science of dental materials are constantly evolving to create more efficient methods of producing stronger and more esthetic restorations. Digital technology appears to be playing a large role in this evolution for technicians and dentists. According to a recent survey,1 70% of full-service laboratories offer digitally manufactured restorations. Although a much smaller portion of dentists do their own milling, interest is slowly rising. A number of new restorative material options allow dental professionals to be more time-efficient in fabricating beautiful, natural-appearing restorations.
Veneered Zirconia Restorations
Zirconia is one of the only restorative materials that must be fabricated in the laboratory or the dental office by means of digital technology. Today this material is used as a full-contour monolithic single crown and as multiple-unit monolithic fixed partial dentures. Initially, partially sintered zirconia blocks were milled and stained prior to the sintering process, which was completed in 9 to 12 hours. For individual posterior single units, where esthetics are not as critical, a stained monolithic zirconia restoration has been acceptable.
In the anterior region, zirconia was first used as a substructure that was fully veneered with a presumably compatible porcelain. Problems began to surface with the delamination of the veneering porcelains. Chipping and bulk fractures of the veneering porcelain without exposure of the zirconia core were found to be occurring.2,3 Causes included a disparity between the coefficients of thermal expansion between the veneering porcelain and the zirconia substructure, low fracture strength of the porcelains, framework design flaws, and sliding contact fatigue.4-6 The bond strength of a feldspathic veneering porcelain can also be affected by the sintering process and the surface treatment of the zirconia substructure.7
For single and multiple anterior units (fixed partial dentures), advances include changes to framework design and fabrication methods. For example, the lingual aspect can be left exposed and milled to full contour while the facial aspect is milled, leaving space for veneering porcelains. For fabrication, hand-layering of the veneering porcelain has been replaced with a heat-pressed method similar to the press-to-metal technique.3,8 In theory, this technique–called "overpressing"9–would seem to have an increase in fracture resistance due to a reduction in air voids and fewer firing cycles.3
Another modification to the fabrication of a veneered zirconia bridge restoration is the CAD-on-restoration technique, where the veneering portion of the restoration is milled and then secured to the fully sintered zirconia framework. For example, a feldspathic material (VITABLOCS® TriLuxe Forte, VITA Zahnfabrik, www.vita-zahnfabrik.com) can be milled and then cemented to the framework with a resin cement, or a lithium disilicate (IPS e.max® CAD) can be milled and then attached to the fully sintered zirconia framework using glass fusion ceramics10 before the CAD material is crystalized or sintered.
Polychromatic Full-Contour Zirconia Restorations
Despite improvements, the susceptibility of porcelain-to-zirconia to chipping and delamination still exists. Lazari and colleagues11 reported that incomplete bonding between the veneering porcelain and the zirconia framework can affect the biomechanical behavior of the ceramic veneer, increasing chipping or fractures.
In recent years, there has been an increasing trend away from a bi-layered to a monolithic full-contour zirconia restoration, eliminating the veneering porcelain and all the problems associated with that combination. Full-contour zirconia single units were first used in the posterior regions mainly because of their inferior esthetic qualities, stemming from their large grain size and resulting high level of opacity.12,13 In the laboratory, the milled monolithic opaque crown would then require a time-consuming manual dip-coloring and drying process before the lengthy sintering process began. The introduction of pre-shaded blocks (eg, Zirlux®, Zahn Dental, www.zirlux.com) has helped to lessen the time required to produce an esthetic monolithic zirconia restoration.
Taking the pre-shaded concept even further, there are now multi-shaded zirconia milling disks that simulate the color gradients that occur in the natural tooth. Kuraray introduced polychromatic multi-layered zirconia milling disks, which eliminate the coloring and drying process.
Translucent Full-Contour Zirconia
The goal of ceramic manufacturers is to produce a restorative material that approaches the optics found in nature. The level of translucency in dental porcelains is determined by the size, chemical nature, and number of crystals in the matrix.14 The translucency in zirconia is derived by the level of alumina particles, impurities, and structural defects that cause the light to scatter. By decreasing the source of light-scattering particles, the level of translucency increases.15
The thickness of ceramic material also affects the translucency. Wang and colleagues16 reported that as the thickness of the ceramic material increases, the degree of translucency decreases. Therefore, the type of zirconia used for full-contour restorations, which has a greater thickness than the veneered porcelain-to-zirconia, must be modified to create the translucency required.
The strength of zirconia is increased with the addition of alumina.17 However, having a different refractive index18 than zirconia, the addition of alumina to the formulation reduces the translucency.
3M ESPE (www.3mespe.com) changed the distribution and content of aluminum oxide in its original Lava™ product to 0.1wt%, which creates a more translucent version and at same time maintains the strength of the original. The new Lava™ Plus High Translucency Zirconia still has less translucency than glass ceramics but four times its strength.19
Sagemax Bioceramics Inc. (https://sagemax-dental.com) introduced NexxZr-White in 2011, a material that has a biaxial flexural strength of 1150 MPa. In 2013, it launched a pre-shaded version called NexxZr-19 Pre-shaded, which has a flexural strength of 1300 MPa and is available in 19 different shades. The position of the restoration can be adjusted in the milling disk depending on the amount of color required throughout the restoration. This year, it has introduced NexxZr®T, which has a biaxial flexural strength of 1150 MPa, a 35% 1-CR translucent factor (1 mm), and a 50% light transmission at 0.6-mm thickness. This version is most translucent in the incisal area.
Zenostar® Full Contour Zirconia (Ivoclar Vivadent) is available in six different pre-shaded milling disks. The Zenostar Zr Translucent has a 40% light transmission at 0.6 mm, with less than 0.1% aluminum oxide and a flexural strength of 1200 MPa.
BruxZir® (www.bruxzir.com, www.bruxzir.com) is another zirconia restorative that can be utilized as a full-contour material. Having an average flexural strength of 1200 MPa, BruxZir milling disks are also available in pre-shaded versions.
Future Zirconia Esthetic Improvements
Increasing the esthetic qualities of full-contour zirconia restorations can be accomplished by reducing the porosity,20 decreasing the grain size,21 and making adjustments to the block or disk-processing technique21 and sintering parameters.22,23 Klimke and colleagues24 found that a particle size less than 40 nm was necessary to achieve a light transmittance of 50% through a specimen with a thickness of 1.0 mm.
Currently, there is interest in fully stabilized cubic zirconia (ZrO2), because of the high refractive index. Although, the flexural strength of the cubic form is approximately 600 MPa, much less than the tetragonal form (~1200), it is still stronger than lithium disilicate at 400 MPa25 and similar in translucency.
Manufacturers of dental ceramics have always focused on strength and esthetics in their development of restorative materials. Moving to monolithic restorations is a viable approach to eliminating potential failures. The creation of translucent ceramics while still maintaining the highest strength continues to be a high priority. Zirconia formulations and processing are constantly changing, including the methods of characterizing the restorations with improved stains and technique.
About the Author
Gregg A. Helvey, DDS, MAGD
Private Practice
Middleburg, Virginia
Adjunct Associate Professor
Virginia Commonwealth University School of Dentistry
Richmond, Virginia
Ceramic Materials Showcase
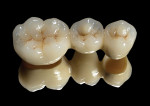
Figure 1 | BruxZir®
Made from the highest quality zirconia powder, BruxZir from Glidewell Laboratories is used to mill strong and esthetic monolithic solid zirconia crowns, bridges, and implant crowns.
800-854-7256
glidewelldental.com
Figure 2 | Lava™ Ultimate
Lava Ultimate from 3M ESPE is a unique CAD/CAM material that is resilient, not brittle, and incredibly durable and shock absorbent. It offers a polish that lasts and is backed by a 10-year warranty.
800-634-2249
3mespe.com
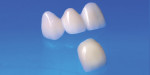
Figure 3 | IPS e.max® CAD
IPS e.max CAD from Ivoclar Vivadent is an innovative lithium disilicate glass-ceramic for CAD/CAM applications that combines highly esthetic quality with exceptional user-friendliness.
800-533-6825
ivoclarvivadent.com
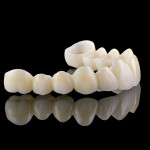
Figure 4 | Keller e.Z™
The new Keller e.Z crown is a strong zirconia crown with veneered porcelain in the esthetic zone. Virtually unbreakable, it can be used for anterior and posterior crowns and up to a 4-unit bridge.
800-325-3056
kellerlab.com
Figure 5 | NuSmile® Zr Pediatric Crown
With science based anatomy, optimized translucency, and a material strength nine times stronger than natural teeth, NuSmile ZR Pediatric Crowns provide exceptional quality, without needing ongoing repairs.
800-346-5133
nusmilecrowns.com
Figure 6 | Calypso™ FMZ
The new formulation and process of Modern Dental Laboratory's multilayered zirconia with color gradient gives greater flexibility to create beautiful smiles in the posterior and now in the anterior.
877-711-8778
moderndentalusa.com
Figure 7 | NexxZr® T
NexxZr® T is a millable full-contour zirconia from Sagemax, with a high translucency for esthetic crowns, bridges, and veneers. Discs are isostatically pressed to ensure material consistency, and milling efficiency.
877-386-0389
sagemax-dental.com
Figure 8 | cubeX2
Dental Arts Lab's new cubeX2 material combines the strength of zirconia with the translucency of lithium disilicate, making it ideal for anterior and posterior applications up to 3-unit bridgework.
888-242-1872
dentalartslab.com
References
1. Carr KF. State of the industry 2015, Part I: ‘challenging but good' according to majority. LMT. 2015;31(5):29-30.
2. Al-Dohan HM, Yaman P, Dennison JB, et al. Shear strength of core-veneer interface in bi-layered ceramics. J Prosthet Dent. 2004;91(4):349-355.
3. Coelho PG, Silva NR, Bonfante EA, et al. Fatigue testing of two porcelain-zirconia all-ceramic crown systems. Dent Mater. 2009;25(9):1122-1127.
4. Hung C-Y, Huang Y-S. Effect of veneering techniques on ceramic fracture of zirconia restoration. J Prosthodont Imp. 2012;1(2):66-70.
5. Coelho PG, Bonfante EA, Silva NR, et al. Laboratory simulation of Y-TZP all-ceramic crown clinical failures. J Dent Res. 2009;88(4):382-386.
6. Sailer I, Fehér A, Filser F, et al. Prospective clinical study of zirconia posterior fixed partial dentures: 3-year follow-up. Quintessence Int. 2006;37(9):685-693.
7. Ramos CM, Cesar PF, Lia Mondelli RF, et al. Bond strength and Raman analysis of the zirconia-feldspathic porcelain interface. J Prosthet Dent. 2014;112(4):886-894.
8. Helvey GA, Miolen K. Evolution of impression-free techniques for zirconia-based restorations. Inside Dentistry. 2007;3(10):72-76.
9. Stawarczyk B, Ozcan M, Roos M, et al. Load-bearing capacity and failure types of anterior zirconia crowns veneered with overpressing and layering techniques. Dent Mater. 2011;27(10):1045-1053.
10. Daou EE. The zirconia ceramic: strengths and weaknesses. Open Dent J. 2014;8:33-42.
11. Lazari PC, Sotto-Maior BS, Rocha EP, et al. Influence of the veneer-framework interface on the mechanical behavior of ceramic veneers: a nonlinear finite element analysis. J Prosthet Dent. 2014;112(4):857-863.
12. Dias MC, Piva E, de Moraes RR, et al. UV-Vis spectrophotometric analysis and light irradiance through hot-pressed and hot-pressed-veneered glass ceramics. Braz Dent J. 2008;19(3):197-203.
13. Tsukuma K, Yamashita I, Kusunose T. Transparent 8 mol% Y2O3–ZrO2 (8Y) ceramics. J Am Ceram Soc. 2008;91(3):813-818.
14. McLean, JW. The Science and Art of Dental Ceramics. Volume 1: The Nature of Dental Ceramics and their Clinical Use. 1st ed. Chicago, IL: Quintessence Publishing Co; 1979.
15. Fujisaki H, Kawamura K, Imai K. Transparent zirconia powder Zpex suitable to dental materials. Tosoh Res Tech Review. 2012;56:57-61.
16. Wang F, Takahashi H, Iwasaki N. Translucency of dental ceramics with different thicknesses. J Prosthet Dent. 2013;110(1):14-20.
17. de Moraes MCC, Elias CNE, Filho JD, Oliveira LG. Mechanical properties of alumina-zirconia composites for ceramic abutments. Mat Res. 2004;7(4):643-649.
18. Kumar P, Wiedmann MK, Winter CH, Avrutsky I. Optical properties of Al2O3 thin films grown by atomic layer deposition. Appl Opt. 2009;48(28):5407-5412.
19. Wang F, Takahashi H. Translucency and biaxial flexural strength of dental ceramics. J Dent Res. 2012;91(spec iss A):422.
20. Zhang HB, Kim BN, Morita K, et al. Effect of sintering temperature on optical properties and microstructure of translucent zirconia prepared by high-pressure spark plasma sintering. Sci Technol Adv Mater.2011;12(5)1-6.
21. Ilie N, Stawarczyk B. Quantification of the amount of blue light passing through monolithic zirconia with respect to thickness and polymerization conditions. J Prosthet Dent. 2015;113(2):114-121.
22. Stawarczyk B, Ozcan M, Hallmann L, et al. The effect of zirconia sintering temperature on flexural strength, grain size, and contrast ratio. Clin Oral Investig. 2013;17(1):269-274.
23. Jiang L, Liao Y, Wan Q, Li W. Effects of sintering temperature and particle size on the translucency of zirconium dioxide dental ceramic. J Mater Sci Mater Med. 2011;22(11):2429-2435.
24. Klimke J, Trunec M, Krell A. Transparent tetragonal yttria-stabilized zirconia ceramics: influence of scattering caused by birefringence. J Am Ceram Soc. 2011;94(6):1850-1858.
25. Helvey GA. Chairside CAD/CAM. Lithium-disilicate restoration for anterior teeth made simple. Inside Dentistry. 2009;5(10):58-67.