An Effective Removal System for Zirconia and Lithium-Disilicate Restorations
Proper instrumentation is key to success with today’s high-strength ceramics.
More than 2,500 years ago, in an ancient civilization situated in present-day western Italy, the Estrucans began using gold to replace and cover missing portions of teeth, effectively creating some of history’s earliest dental crown restorations.1 Ancient Egyptians, Greeks, and Romans also contributed to the development of prosthetic dentistry, as evidenced by the scores of ivory, wood, and gold dentures unearthed in centuries-old mummies, sarcophagi, and urns.2 As millennia and centuries passed, what has come to be known as prosthetic dentistry continued to evolve, with each dental generation envisioning novel methods and developing new materials for restoring teeth. Today’s generation is no different; like their ancestors, dentists today seek out ideal methods, materials, and instrumentation while striving to practice superior dentistry.
As modern-day dentistry strives for natural-looking esthetic restorations that also possess superior strength and durability, the dental crown restoration remains a firmly established solution for a broken or structurally compromised tooth. Although dental crowns historically have been fabricated of gold, composite, porcelain and gold (or other substructure metal), and an array of all-porcelain materials, traditional thought was that porcelain, which offers optimal esthetic qualities, was a relatively weak material. Today’s high-strength ceramics—such as zirconia and lithium disilicate—provide greater strength and durability than their predecessors, making them the materials of choice in many dental practices and laboratories. Furthermore, zirconia and lithium-disilicate crowns are considered “cosmetic” in nature when compared to various other options, and they are substantially stronger than many alternative crown materials.3,4
Although the first high-strength ceramic crowns were fabricated with zirconia copings layered or pressed with different types of porcelain, monolithic (full-contour) zirconia and lithium-disilicate crowns are growing in popularity, with numerous laboratories promoting them due to their combination of strength, esthetics, and affordability. Full-contour zirconia and lithium-disilicate crowns are extraordinarily strong, and many in the industry maintain that the esthetics equal those of their layered counterparts.5,6 While some choose to debate the notion of esthetic comparability,7 it is clear that high-strength ceramics are a reality in the modern dental practice, making it imperative for dentists to learn how best to work with and, when necessary, remove them.
The average lifespan of a crown ranges from 5 to 15 years.8 In addition, studies have found that 4% to 8% of crowned teeth require endodontic treatment within the 10 years following crown placement,9 with some suggesting percentages as high as 13.3%.9 Clearly, then, most crowns eventually require replacement. There is growing concern, though, that these stronger crowns can be very difficult to remove and that rotary solutions for this process are lacking. With the correct instrumentation and technique, however, it is possible to remove these crowns in a timely, user- and patient-friendly manner.
Diagnosis and Treatment Planning
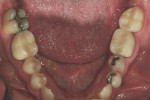
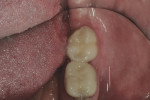
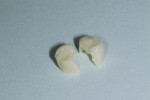
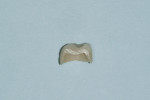
A 54-year-old man presented with a chipped layered zirconia crown on tooth No. 18 (Figure 1). After only 3 years of service, the distal–lingual portion of the layered porcelain had sheared away from the underlying zirconia coping (Figure 2). It should be noted that this is a relatively common problem with layered zirconia crowns.10,11 Consequently, some laboratories advocate the use of full-contour zirconia or lithium-disilicate crowns, which do not have the potential for porcelain shearing.
The patient was firm in his desire for the replacement restoration to be highly esthetic. To achieve his goals, several material choices were available, including lithium disilicate, leucite-reinforced porcelain, and zirconia.
In selecting any restorative option, multiple factors are taken into consideration, one of the first being flexural strength. The flexural strength of a layered porcelain crown with a metal or zirconia substrate7 is 120 MPa,12 while other studies have shown bonded leucite-reinforced porcelain in the range of 200 MPa to 220 MPa.13-16 By comparison, a full-contour lithium-disilicate crown offers flexural strength in excess of 360 MPa (CAD/CAM) and 400 MPa (pressed),17 while a full-contour zirconia crown boasts a strength of more than 1,000 MPa.12
Esthetics and cost are additional considerations. In terms of cost, many laboratories promote full-contour over layered restorations simply because the layering technique takes more time to complete, leading in turn to higher laboratory fees for the final restoration.5 In addition, the rising costs of metal alloys add to the overall cost of porcelain-fused-to-metal (PFM) crowns. This factor, paired with the impressive esthetic qualities of the new generation of high-strength ceramics, is leading more and more dentists and laboratories to switch from PFM crowns to all-ceramic restorations. Ultimately, many industry leaders expect all-ceramic options to gradually replace PFM restorations.18
After a discussion of the available options, the patient elected to have the tooth re-restored with a zirconia-based crown. The treatment plan called for the cementation of the restoration with a resin-modified glass-ionomer cement, a procedure documented for its ease and predictability.19 With proper coping design, combined with the appropriate technique for connecting the layered porcelain to the zirconia coping, layered zirconia crowns have demonstrated long-term reliability.20,21
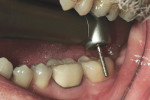
In most cases involving the removal of a layered zirconia or lithium-disilicate crown, the layered porcelain is easily detached, while the high-strength ceramic layer is much more difficult to penetrate.22 In the course of the cutting process, standard diamond burs tend to prepare and smooth the ceramic, often leaving the sectioned crown difficult to access with a separating instrument; the prepared section becomes rounded, making it difficult to torque the separated halves of a crown. It is, therefore, important to have on hand diamond burs specifically designed for use on zirconia and lithium disilicate. The ZR™ diamond line (Komet USA, www.kometusa.com) features a range of instruments precision engineered to cut, finish, and polish zirconia and lithium disilicate (Figure 3 and Figure 4). For example, the 4ZR™ 014 slices through the entire coping (Figure 5). This crown was removed in approximately a third of the time it has taken this author in the past when sectioning layered zirconia or lithium-disilicate crowns using standard diamond burs. It stands to reason, that in the case of a monolithic zirconia crown, the time savings would be far greater.
Technique Protocol
The patient was anesthetized with one carpule of Septocaine® (Septodont, www.septodontusa.com), and the teeth were isolated (Isolite™, Isolite Systems, www.isolitesystems.com). The fractured layered zirconia crown was removed using the 4ZR™ crown cutter and a high-speed electric handpiece (KaVo, www.kavousa.com).
The 4ZR™ 014 bur was used to section the layered porcelain and zirconia coping along the entire coping from lingual to buccal, across the occlusal surface (Figure 6). Once the crown was sectioned in half, the two halves were twisted and removed (Figure 7). The residual cement on the tooth was removed, and the preparation was refined with a series of crown-preparation diamonds: KS0, KS1SC, and KS3SC (Komet USA). The preparation was completed, and the final margin position was established and smoothed at a slow speed with the KS5SC, KS6SC, and 8856.021 burs. Care was taken to ensure an accurate and smooth margin with minimal disruption to the surrounding tissue. An antimicrobial scrub (Consepsis® Pumice Scrub, Ultradent Products, Inc., www.ultradent.com) was applied to the preparation and brushed across the teeth with a STARBrush® (Ultradent) using a slow-speed latch handpiece (KaVo). This removed debris and cleaned the preparation prior to the impression and provisional seating. The tooth was rinsed thoroughly with water and dried.
Final impressions were taken using polyvinyl siloxane impression material (Imprint™ 3 Garant, 3M ESPE, www.3MESPE.com), and the provisional restoration was formed (Protemp™, 3M ESPE) and seated with provisional cement (Fynal®, DENTSPLY, www.dentsply.com). The patient was provided with postoperative and hygiene instructions for care of the provisional over the following 3 weeks. Instructions were sent to the laboratory for fabricating the replacement layered-zirconia crown.
Crown Removal Appointment
All crown-removal procedures aim to be conservative, efficient, and quick. Zirconia and lithium-disilicate crowns, however, present significant challenges to these goals because of the inherent properties of the materials. As this case demonstrates, however, the 4ZR™ diamond sliced through the crown with relative ease, resulting in a clean cut (Figure 8). In addition, the edges were easily torqued to remove the two halves. In contrast, the majority of layered zirconia and lithium-disilicate crowns previously removed by this author using standard diamonds required additional sectioning; at times, additional tooth structure was removed as an unwanted “side effect” of crown removal.
Because of the speed with which the zirconia was removed in this case, heat generation was minimized. In past cases, sparks typically resulted due to extended contact between the material and the diamond burs, despite copious water spray. The resultant heat generation must be seen as an unnecessary risk, knowing that the ZR™ diamonds can accomplish the same task more quickly and without creating sparks.
Discussion
All-ceramic restorations are rapidly becoming the norm within the practice of restorative dentistry.18 The rising costs of alloys have played a large part in this trend, but so, too, have the significant advances in the chemistry of dental materials. Zirconia and lithium disilicate, in particular, have become the materials of choice for many laboratories, with a growing trend toward inexpensive, full-contour, high-strength ceramic crowns. Although evidence indicates that zirconia and lithium disilicate can be extremely difficult to remove, the materials continue to be used with increasing frequency.
Like all dental restorations, crowns made of high-strength ceramics like zirconia and lithium disilicate will not last forever. Inevitably, many crowns fabricated from these materials will eventually be replaced, whether due to structural failure, secondary caries, endodontic treatment needs, implant-related complications (such as screw-loosening), or other causes.8,9 When crown removal becomes necessary, it is crucial for the procedure to be accomplished effectively and safely. It is unacceptable for heat and vibration to damage the instruments or, more importantly, the patient’s underlying tooth. To protect patients and keep them comfortable, dentists must acknowledge that time spent in the dental chair must be kept to a minimum, and tooth structure must be conserved; therefore, it is imperative to use reliable instrumentation for this procedure.
Conclusion
Modern-day dentistry demands predictable esthetic materials, treatments, and results. Both dentists and patients seek strong, durable restorations. This has led to the development of materials that are significantly stronger than those available to previous generations. In this pursuit for strength, it is important to have equally effective means for removing the materials safely and efficiently.
References
1. Vukovic A, Bajsman A, Zukic, S, Secic S. Cosmetic dentistry in ancient times—a short review. Bull Int Assoc Paleodont. 2009;3(2):9-13.
2. Taylor JA. History of Dentistry: A Practical Treatise for the Use of Dental Students and Practitioners. Philadelphia, PA: Lea & Febiger; 1922:142-156.
3. White SN, Miklus VG, McLaren EA, et al. Flexural strength of a layered zirconia and porcelain dental all-ceramic system. J Prosthet Dent. 2005;94(2)125-131.
4. Fasbinder DJ, Dennison JB, Heys D, Neiva G. A clinical evaluation of chairside lithium disilicate CAD/CAM crowns: a two-year report. J Am Dent Assoc. 2010;141(Suppl 2)10S-14S.
5. Guazzato M, Proos K, Quach L, Swain MV. Strength, reliability and mode of fracture of bilayered porcelain/zirconia (Y-TZP) dental ceramics. Biomaterials. 2004;25(20):5045-5052.
6. Vichi A, Louca C, Corciolani G, Ferrari M. Color related to ceramic and zirconia restorations: a review. Dent Mater. 2011;27(1):97-108.
7. Engelberg B. Zirconia: clinical impressions: An in vivo comparison of the aesthetics of various zirconia crowns. Dent Today. 2012;31(7):106-109.
8. Cleveland Clinic. How Long do Dental Crowns Last? Available at: https://my.clevelandclinic.org/services/cosmetic_dentistry/hic_dental_crowns.aspx. Accessed November 14, 2012.
9. Whitworth JM, Walls AW, Wassell RW. Crowns and extra-coronal restorations: endodontic considerations: the pulp, the root-treated tooth and the crown. Br Dent J. 2002;192(6):315-327.
10. Cochran T. Achieving long-lasting results with 3M™ ESPE™ LAVA™ zirconia. Dental Lab Products. 2010;23;48.
11. Swain MV. Unstable cracking (chipping) of veneering porcelain on all-ceramic dental crowns and fixed partial dentures. Acta Biomater. 2009;5(5):1668-1677.
12. Yener ES, Özcan M, Kazazoğlu E. The effect of glazing on the biaxial flexural strength of different zirconia core materials. Acta Odontol Latinoam. 2011;24(2):133-140.
13. Albakry M, Guazzat M, Swain MV. Biaxial flexural strength and microstructure changes of two recycled pressable ceramics. J Prosthodont. 2004;13(3):141-149.
14. Fradeani M, Redemagni M. An 11-year clinical evaluation of leucite-reinforced glass ceramic crowns: a retrospective study. Quintessence Int. 2002;33(7):503-510.
15. Sorensen JA, Choi C, Fanuscu MI, Mito WT. IPS Empress crown system: three-year clinical trial results. J Calif Dent Assoc. 1998;26(2):130-136.
16. Drummond JL, King TJ, Bapna MS, Koperski RD. Mechanical property evaluation of pressable restorative ceramics. Dent Mater. 2000;16(3):226-233.
17. Tysowsky GW. The science behind lithium disilicate: a metal-free alternative. Dent Today. 2009;28(3):112-113.
18. Christensen G. The future: materials, challenges in dentistry, and education. Dent Today. 2012;31(2):102-106.
19. Komine F, Blatz MB, Matsumura H. Current status of zirconia-based fixed restorations. J Oral Sci. 2010;52(4):531-539.
20. Marchack BW, Futatsuki Y, Marchack CB, White SN. Customization of milled zirconia copings for all-ceramic crowns: a clinical report. J Prosthet Dent. 2008;99(3)169-173.
21. Marchack BW, Sato S, Marchack CB, White SN. Complete and partial contour zirconia designs for crowns and fixed dental prostheses: a clinical report. J Prosthet Dent. 2011;106(3)145-152.
22. Ozkurt Z, Işeri U, Kazazoğlu E. Zirconia ceramic post systems: a literature review and a case report. Dent Mater J. 2010;29(3)233-245.
About the Author
Brent Engelberg, DDS
Private Practice
Arlington Heights, Illinois