Chairside CAD/CAM
An overview of restorative material options.
A number of categories of materials are available for chairside CAD/CAM restorations that have demonstrated predictability and longevity. These materials include esthetic and high-strength ceramics,.composite resins for both final and temporary restorations, and newer nanoceramics that offer ease of handling and a glossy surface finish. Each category of materials has unique features designed for specific clinical applications. This article will examine currently available materials designed for chairside CAD/CAM restorations and the various ou.comes that are possible with this technologically advanced process.
Over the past 25 years, in-office.computer-aided design.computer-aided manufacturing (CAD/CAM) technology has continued its evolution as a highly accurate and efficient means of dentistry. The CEREC® Acquisition Center (AC) (Sirona Dental Systems, www.sirona.com) and the E4D™ Dentist System (D4D Technologies, www.e4d.com) are CAD/CAM systems capable of imaging a tooth preparation for the purpose of designing and fabricating monolithic restorations chairside.1,2 These types of restorations are.commonly referred to as “CEREC” or “E4D” restorations, which implies uniformity in both their.composition and clinical performance. The only uniformity is that both systems use CAD/CAM processes capable of imaging, designing, and milling a restoration. Both systems are capable of fabricating inlays, onlays, veneers, and single crowns. In fact, a wide variety of materials are available for use with these systems that provide a number of different possible ou.comes with the chairside CAD/CAM process.
Restorations fabricated with chairside CAD/CAM systems are monolithic—the entire restoration is a single homogenous material rather than a bilayered restoration consisting of a coping and a veneer layer. Monolithic materials for chairside CAD/CAM systems have several unique features. The industrial material fabrication process provides a homogenous, dense material without porosity or voids, which maximizes the material’s physical properties. The material is manufactured in a solid block form that is mounted on a milling mandrel unique to the specific CAD/CAM milling system (Figure 1). Both.commercial systems employ a subtractive wet-grinding process for shaping or milling the restoration from the preformed blocks based on the 3-dimensional (3-D) volumetric design created with the systems’ software programs.
The restoration should be able to be milled in an efficient time period suitable for delivery at the same appointment—generally less tn 20 minuhates—without damaging the material, as.compromised material could lead to early failure of the restoration. Additionally, post-milling processing time is a key consideration. The need for significant handling time or for procedures that may be required to create the final strength and surface characteristics of the restoration can detract from a material’s ability to be used in a one-appointment restorative procedure.
Restorative Materials for CAD/CAM
There are a number of categories of restorative materials available for chairside CAD/CAM restorations3 (Table 1). Each category of materials offers unique features designed for its specific clinical applications. The CAD/CAM system represents the process by which these materials are fabricated into a restoration, while the clinical ou.come of the restoration is more likely determined by the type of restorative material used.
High-strength ceramics offer a substantial increase in flexural strength and fracture toughness.compared to esthetic ceramic materials, but not at the level of polycrystalline ceramics such as zirconia. Recently introduced nanoceramic materials purport to offer the benefits of easy handling similar to.composite materials, with the strength and surface finish of ceramics. Two types of.composite resin blocks are available. One brand is designed for final restorations, and the other marketed.composite resin blocks are used for long-term temporary restorations.
Esthetic Ceramics
Esthetic ceramics are glass-containing materials with very good translucency and moderate flexural strength. The presence of the glass.component permits the materials to be etched with hydrofluoric acid, treated with a silane coupler, and adhesively bonded to the tooth. Adhesive bonding of these materials is critical to their long-term success, as they lack sufficient strength to permit conventional cementation with either resin-modified glass-ionomer or traditional glass-ionomer cements. The adhesive bonding not only provides retention for the restoration, but it also contributes to the restoration’s clinical strength to resist fracture.
Vitablocs® Mark II (Vident, www.vident.com) and CEREC® Blocs (Sirona Dental Systems) are feldspathic glass ceramics. Both materials are fine-grained, homogeneous feldspathic porcelain with an average particle size of 4 μm.4 The small particle size allows for a high-gloss finish and minimizes abrasive wear of the opposing dentition. Introduced in 1991, Vitablocs Mark II is available in the 10 most common Vita 3D-Master® shades. CEREC Blocs became available in 2007 and are also manufactured by Vita Zahnfabrik (www.vita-zahnfabrik.com).5 Blocks are available in six shades and three different degrees of color saturation (chroma): translucent (T), medium (M), and opaque (O). Both of these feldspathic ceramic materials are unique to the CEREC system and are not available on milling mandrels for the E4D system.
Vitablocs Mark II is also available in several multicolored blocks. Triluxe blocks (Vident) contain three different bands of color to recreate the shade and translucency of the tooth from cervical to incisal. Triluxe Forte blocks (Vident) feature a gradient of color and translucency from cervical to incisal with increased fluorescence and chroma in the cervical area. The most recently introduced RealLife block (Vident) has an innovative 3-D radial gradient of color and translucency from the internal portion of the block to the external part of the block to simulate the natural transition from dentin core to enamel veneer. CEREC Blocs also.come in multicolored block form. The CEREC Bloc PC features a three-layered structure; the bottom (cervical) layer has the highest pigmentation and lowest translucency, and the top (incisal) layer has the highest translucency and lowest color intensity. It is available in three different gradient shades.
Multicolor blocks offer an enhanced esthetic result.compared to conventional monochromatic blocks. The application that offers the maximum benefit for a polychromatic block is a crown, because an onlay tends to have a limited vertical dimension for visualizing the gradient of color. Further customization of either the monochromatic or polychromatic blocks can be a.complished by shade characterization and glazing using the Vita Shading Paste Assortment Kit. The kit is.compatible with both the Vitablocs Mark II and CEREC Blocs.
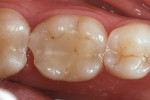
Being the oldest marketed chairside CAD/CAM material,6 there are many published clinical studies using Vitablocs Mark II restorations fabricated with the CEREC system. (Figure 2 through Figure 4 depict a Vitablocs Mark II ceramic onlay restoration.) A clinical study conducted on 2,328 inlays and onlays for 794 patients in a private practice reported 35 failures over 9 years.7 The Kaplan-Meier survival probability was 97.4% at 5 years and 95.5% at 9 years. Another study reported a Kaplan-Meier survival probability of 90.4% after 10 years for 200 Vitablocs Mark II restorations placed in 108 patients in private practice.8 In a follow-up report of the study, the authors reported an 88.7% success rate at 17 years.9 From 1991 to 2006 a series of papers reported the clinical status of 1,011 CEREC restorations for up to 18 years.10-12 After 5 years, the survival probability was 95%, and after 7 years it was 91.6%. At 10 years the survival probability was 90% and it declined to 84.9% at 16.7 years. A systematic review of 29 clinical studies, which included 2,862 inlays, reported a survival rate of 97.4% after a period of 4.2 years.13 The primary mode of failure was fracture of the ceramic restoration. Less.common failure modes included fracture of the tooth, wear of the cement, and postoperative sensitivity.
The first leucite-reinforced glass-ceramic CAD/CAM block, ProCAD (Ivoclar Vivadent, www.ivoclarvivadent.us), was introduced in 1998. It evolved to b.come the current IPS Empress® CAD (Ivoclar Vivadent) and is a 35% to 45% leucite-reinforced glass-ceramic similar to IPS Empress 1 but with a finer particle size of 1 μm to 5 μm. The blocks are available in nine.common shades in either a high-translucency (HT) or low-translucency (LT) version. The HT version has an increased translucency, while the LT version has a brighter value and is also available in four bleach shades. IPS Empress CAD is also available in a multicolor block form. Offering five popular colors, the block has a gradient of color and translucency ranging from cervical to incisal to simulate the transition of color and translucency in the natural dentition. Individual shade customization of either the monochromatic or multicolor blocks can be a.complished using IPS Empress Universal Stains.14 Paradigm C (3M ESPE, www.3MESPE.com) was a second leucite-reinforced glass-ceramic mill block, but it is no longer available for either the CEREC or E4D system.
A.comparison of the physical properties is a.common means of differentiating between various esthetic ceramics. Most in vitro studies involve a specific physical property, making it difficult to.compare between studies. However, one study evaluated a number of physical properties between the two types of blocks. The feldspathic block was significantly harder than the leucite-reinforced block. The authors suggested that the increased surface hardness may make the material more resistant to scratches and surface wear. The leucite-reinforced block had a significantly greater flexural strength, flexural modulus, and fracture toughness, which the authors suggested may make it more resistant to fracture under stress.15 The physical property values reported by the manufacturers for each material indicate insufficient differences in them to support the contention that a specific physical property would lead to different clinical ou.comes.4,5,14,16,17
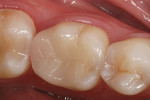
A few published clinical studies are available specifically on leucite-reinforced CAD/CAM restorations. Guess et al reported a prospective clinical investigation on the survival rate and long-term behavior of IPS e.max® Press (Ivoclar Vivadent) and ProCAD molar onlay restorations.18 The Kaplan-Meier survivability at 3 years was 97% for the ProCAD onlays and 100% for the IPS e.max Press onlays. The authors reported one ProCAD onlay fracture, which required replacement at 9 months. They concluded that wear of the resin cement at the occlusal margin was a critical factor in the long-term success of the restorations. Another randomized clinical study that included leucite-reinforced and feldspathic CEREC onlays cemented with a self-etching, self-adhesive resin cement reported no significant differences in the clinical performance between the two materials at 3 years19 (Figure 5 through Figure 7).
IPS Empress CAD is similar to Empress 1 in physical structure; therefore, a similar clinical performance may be anticipated. A literature review of longevity and clinical performance of IPS Empress restorations was reported in 2002.20 Six clinical trials on the performance of IPS Empress inlays and onlays and three clinical trials on the performance of IPS Empress crowns were identified in the literature. Survival rates for IPS Empress inlays and onlays ranged from 96% at 4.5 years to 91% at 7 years with most failures due to bulk fracture of the restorations. IPS Empress crowns had a survival rate ranging from 92% to 99% at 3 to 3.5 years, with failure also mainly due to fracture of the crown.
High-Strength Ceramics
IPS e.max® CAD (Ivoclar Vivadent) was introduced in 2006 as a lithium-disilicate CAD/CAM material with flexural strength (360MPa) two to three times that of esthetic ceramic materials. The increased strength affords the opportunity to either etch and adhesively bond the material to the tooth or use a conventional cementation technique.17 Most in vitro studies have indicated a significant increase in the strength of the restoration if the material is adhesively bonded rather than cemented to the tooth.21,22 Lithium disilicate was initially developed as a substructure material that offered greater translucency.compared to other high-strength ceramic core materials. However, it has gained popularity for use as a monolithic restoration in chairside CAD/CAM systems due to its enhanced strength. The CAD/CAM block form is available in nine A-D shades, two translucencies, and four bleach shades.
IPS e.max CAD blocks consist of 0.2-μm to 1-μm lithium-metasilicate crystals with approximately 40% crystals by volume. The block is a blue-violet color, which accounts for the.commonly used “blue block” description. This partially crystallized “soft” state allows the block to be easily milled without excessive diamond bur wear or damage to the material. After the restoration is milled, it must undergo a two-stage firing process in a porcelain oven under vacuum to.complete the crystallization of the lithium disilicate. The choice of glazing media affects the firing time; the spray-on glaze requires a 20-minute firing cycle, while the paint-on glaze demands a 28-minute firing cycle due to the presence of more organic.compounds in the paste. The crystallization firing also converts the blue shade of the pre-crystallized block to the selected tooth shade and results in a glass-ceramic with a fine grain size of approximately 1.5 μm and a 70% crystal volume incorporated in a glass matrix.23
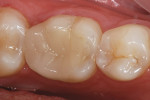
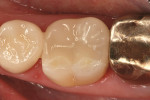
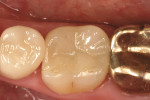
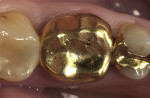
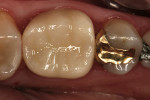
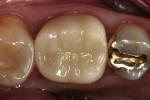
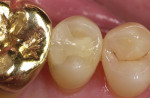
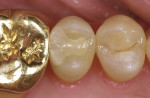
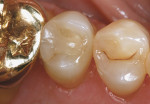
There are few clinical studies on IPS e.max CAD or its similar press-fit counterpart, IPS e.max Press, due to its limited time in clinical service. The previously mentioned study by Guess et al on the survival rate and long-term behavior of IPS e.max Press and ProCAD molar onlay restorations reported a Kaplan-Meier survivability at 3 years of 100% for the IPS e.max Press onlays.18 Reich and coworkers reported a clinical study on the performance of chairside-generated CAD/CAM e.max CAD crowns.24 A CEREC system was used to deliver 41 e.max CAD full-contour crowns in 34 patients. After 2 years, one crown exhibited secondary caries and two crowns received root canal treatment. An ongoing longitudinal clinical study is evaluating the clinical performance of 100 IPS e.max CAD full-contour crowns. The first 62 crowns were delivered with either a self-etching bonding agent and resin cement or a self-adhesive resin cement. A third group of 38 crowns was placed at a later time using a newer self-etching, self-curing cement (Figure 8 through Figure 11). Each of the full-contour crowns was placed during a single-treatment appointment with the CEREC system. There were no reported crown failures after 4 years for the first group of 62 crowns and after 2 years for the second group of 38 crowns. Perhaps more significant is that there were no reports of any clinically visible chipping or cracking of the crowns.25
Nanoceramics
A recently introduced unique CAD/CAM block is based on the integration of nanotechnology and ceramics. This nanoceramic material is purported to offer the ease of handling of a.composite material with the surface gloss and finish retention similar to a porcelain. Lava™ Ultimate (3M ESPE) contains three ceramic filler particles. Silica particles of 20 nm, zirconia particles of 4 nm to 11 nm, and agglomerated nanoparticles of silica and zirconia are all embedded in a highly cross-linked polymer matrix. The aggregated clusters are.comprised of 20-nm silica and 4-nm to 11-nm zirconia particles, with approximately an 80% ceramic load.
The manufacturer has reported a flexural strength of 200 MPa, which is greater than the flexural strength of feldspathic and leucite-reinforced porcelain blocks (140 MPa to 160 MPa), as well as that of veneering porcelains for porcelain-fused-to-metal (PFM) crowns (generally less than 100 MPa). Manufacturer testing indicates that the fracture toughness of the nanoceramic material is statistically greater than feldspathic porcelain and direct.composite materials while being less brittle than feldspathic glass-ceramics, and, therefore, it is less prone to cracking during try-in and function. The manufacturer r.commends an axial reduction of 1 mm and cuspal reduction of 1.5 mm, with both dimensions being about 0.5-mm less than what is conventionally r.commended for porcelain restorations.
The inclusion of nanoparticles in the Lava Ultimate block offers the potential for easy contour adjustment and creation of a high-gloss surface finish. A purported improvement in the nanoceramic material is the ability to retain a high-gloss surface finish over time, which tends to be a limitation of CAD/CAM.composite blocks. In vitro studies by the manufacturer indicate that Lava Ultimate has resistance to toothbrush abrasion along with retention of the initial glossy surface finish similar to glass-ceramics. Long-term clinical evaluation is needed to confirm this desirable property of the material. Lava Ultimate restorative will be available in eight shades in both low- and high-translucency forms for both CEREC AC and E4D chairside CAD/CAM systems. Additionally, the manufacturer will offer a 10-year warranty for replacement of the restorative material should it fail clinically.
Composite Resin for Permanent Restorations
Paradigm™ MZ100 (3M ESPE), introduced in 2000, is a polymer.composite block based on the Z100 composite chemistry and relies on a proprietary processing technique to maximize the degree of cross-linking.26,27 Paradigm MZ100 has zirconia-silica filler particles and is 85% filled by weight with an average particle size of 0.6 μm. It is radiopaque and available in six shades as well as a more translucent enamel shade. No working die is created with the in-office CAD/CAM process to use in refining the margins and proximal contacts prior to delivery of the restoration. Often times, there is a need to adjust and repolish these areas and refine the occlusal contacts since the lateral guidance cannot be replicated on the software design programs. The polymer chemistry of Paradigm MZ100 makes it easier to adjust and polish intraorally. Repair of porcelain restorations intraorally has not proven to be more than a moderately effective temporary technique.28,29 With Paradigm MZ100, the surface of the restoration is air-abraded with 50-μm silicon dioxide, and a hybrid.composite can be bonded to the abraded surface. Although untested for clinical longevity, this affords an easy, efficient intraoral repair procedure for Paradigm MZ100 restorations.
Kunzelmann et al reported an in vitro study using a chewing simulator to measure the occlusal wear of feldspathic porcelain (Vitablocs Mark II), leucite-reinforced porcelain (ProCAD and Empress), and.composite (Paradigm MZ100).30 The Paradigm MZ100 showed the greatest material wear—up to twice the amount of the ceramic materials—with the feldspathic block having less material wear than the leucite-reinforced materials. The Paradigm MZ100 showed the least amount of opposing enamel wear.compared to the porcelain materials. However, when.comparing the total occlusal wear, the Paradigm MZ100 showed the least amount of wear, which the authors stated would be preferred clinically because this would protect the opposing enamel.
Attia et al reported on the fracture load of Paradigm MZ100 crowns.compared to Vitablocs Mark II crowns and found no significant difference in the fracture load of the crowns if they were adhesively cemented.31 The authors suggested that although intuitively it may be expected that all-ceramic crowns would be stronger, the improved elastic properties of the.composite crowns may demonstrate a higher resiliency and a higher load absorption, leading to an increase in fracture load.
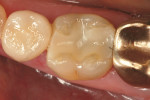
An ongoing clinical study reported the 3-year and 6-year results of a randomized clinical trial of 40 Paradigm MZ100 inlays and 40 Vitablocs Mark II inlays.32,33 More recently, the 10-year results have also been published.34 All restorations were evaluated using modified US Public Health Service (USPHS) criteria. One Vitablocs Mark II inlay had postoperative sensitivity that was resolved within 2 weeks. All other restorations had no sensitivity through the 10-year recall. The.composite inlays had no significant change in color match from baseline, while the porcelain inlays had a decrease in color match at 6 months that was unchanged afterwards, which was attributed to changes in tooth color. There was one.composite inlay fracture and five porcelain inlay fractures at 10 years (Figure 12 through Figure 14).
Composite Resin for Temporary Materials
Not all clinical situations are amenable to treatment with chairside CAD/CAM restorations. In an effort to.complement the laboratory fabrication process, CAD/CAM temporary blocks have been introduced for chairside fabrication of long-term temporary crowns and fixed partial dentures (FPDs). The CAD/CAM process avoids the air-inhibited layer found with conventional self-cure or visible light-cure (VLC) acrylics as well as polymerization shrinkage.
Vita CAD-Temp® (Vident) is a highly cross-linked, microfilled polymer that is available in extended block sizes, including lengths of 40 mm and 55 mm to a.commodate multiple-unit FPDs.35 It is offered in a monocolor block that.comes in four shades or a multicolor form with four shade layers for increased esthetics. Telio® CAD (Ivoclar Vivadent) has been introduced as a millable cross-linked polymethylmethacrylate (PMMA) block for temporary crowns and FPDs. The block is part of the Telio system that includes a self-curing.composite, desensitizer, and cement. It is available in 40-mm and 55-mm size blocks and in six shades.36
Conclusion
The recent focus on chairside CAD/CAM systems has been on the continuing evolution of the process for recording images of tooth preparations, software design, and restoration milling. The ease of use, efficiency of the process, accuracy of the ou.comes, and variety of applications continue to progress and expand with each new CAD/CAM innovation. Block materials available for clinical application have also expanded. All of the available ceramic and.composite materials demonstrate the desirable qualities of machinable materials and the capability of being milled efficiently for chairside use without damage to the restoration. Clinical studies to date have documented the predictability and longevity of chairside CAD/CAM restorations.
Disclosure
The author has received grant/research support from 3M ESPE and Ivoclar Vivadent.
References
1. Mörmann WH. The evolution of the CEREC system. J Am Dent Assoc. 2006;137(suppl):7S-13S.
2. Levine N. To the sky and beyond. Dental Products Report. 2009:116.
3. Fasbinder DJ. Materials for chairside CAD/CAM restorations. Compend Contin Educ Dent. 2010;31(9):702-709.
4. Vitablocs Mark II for CEREC. Materials Science and Clinical Studies. Brea, CA: Vident; September 2003.
5. CEREC Blocs – for CEREC/InLab. Operating Instructions. Charlotte, NC: Sirona Dental Systems, LLC.
6. Fasbinder DJ. Clinical performance of chairside CAD/CAM restorations. J Am Dent Assoc. 2006;137(suppl):22S-31S.
7. Posselt A, Kerschbaum T. Longevity of 2328 chairside Cerec inlays and onlays. Int J Comput Dent. 2003;6(3):231-248.
8. Otto T, De Nisco S..computer-aided direct ceramic restorations: a 10-year prospective clinical study of Cerec CAD/CAM inlays and onlays. Int J Prosthodont. 2002;15(2):122-128.
9. Otto T, Schneider D. Long-term clinical results of chairside Cerec CAD/CAM inlays and onlays: a case series. Int J Prosthodont. 2008;21(1):53-59.
10. Reiss B, Walther W. Survival analysis and clinical evaluation of CEREC restorations in a private practice. In: Morman WH, ed. International Symposium on.computer Restorations 1991: State of the Art of the Cerec-Method. Berlin, Germany: Quintessence Publishing; 1991:215.
11. Reiss B, Walther W. Clinical long-term results and 10-year Kaplan-Meier analysis of Cerec restorations. Int J Comput Dent. 2000;3(1):9-23.
12. Reiss B. Clinical results of Cerec inlays in a dental practice over a period of 18 years. Int J Comput Dent. 2006;9(1):11-22.
13. Martin N, Jedynakiewicz NM. Clinical performance of CEREC ceramic inlays: a systematic review. Dent Mater. 1999;15(1):54-61.
14. IPS Empress® CAD: Instructions for Clinical Use Chairside. Amherst, NY: Ivoclar Vivadent; September 2006.
15. Charlton DG, Roberts HW, Tiba A. Measurement of select physical and mechanical properties of 3 machinable ceramic materials. Quintessence Int. 2008;39(7):573-579.
16. Giordano R. Materials for chairside CAD/CAM-produced restorations. J Am Dent Assoc. 2006;137(suppl):14S-21S.
17. Tysowsky, GW. The science behind lithium disilicate: a metal-free alternative. Dent Today. 2009;28(3):93-97.
18. Guess PC, Strub JR, Steinhart N, et al. All-ceramic partial coverage restorations—midterm results of a 5-year prospective clinical split-mouth study. J Dent. 2009;37(8):627-637.
19. Fasbinder DJ, Neiva G, Dennison JB, Heys D. Clinical evaluation of CAD/CAM generated ceramic onlays [abstract]. J Dent Res. 2011;90(spec iss A). Abstract 0378.
20. El-Mowafy O, Brochu JF. Longevity and clinical performance of IPS-Empress ceramic restorations—a literature review. J Can Dent Assoc. 2002;68(4):233-237.
21. Hill TJ, McCabe P, Tysowsky G. Bonding and thickness effect on fracture load of CAD/CAM crowns [abstract]. J Dent Res. 2008;87(spec iss A). Abstract 2321.
22. Bindl A, Luthy H, Mörmann WH. Thin-wall ceramic CAD/CAM crown copings: strength and fracture pattern. J Oral Rehabil. 2006;33(7):520-528.
23. IPS e.max lithium disilicate: the future of all-ceramic dentistry. Material science, practical applications, keys to success. Amherst, NY: Ivoclar Vivadent publication 627329; March 2009:1-15.
24. Reich S, Fischer S, Sobotta B, et al. A preliminary study on the short-term efficacy of chairside.computer-aided design.computer-assisted manufacturing-generated posterior lithium disilicate crowns. Int J Prosthodont. 2010;23(3):214-216.
25. Fasbinder DJ, Heys D, Neiva G. A clinical evaluation of chairside lithium: 4 year report [abstract]. J Dent Res. 2012;91(spec issus A). Abstract 645.
26. Rusin RP. Properties and applications of a new.composite block for CAD/CAM. Compend Contin Educ Dent. 2001;22(6 suppl):35-41.
27. Paradigm™ MZ100 Block: Technical Product Profile. St. Paul, MN: 3M ESPE; 2000.
28. Leibrock A, Degenhart M, Behr M, et al. In vitro study of the effect of thermo- and load-cycling on the bond strength of porcelain repair systems. J Oral Rehabil. 1999;26(2):130-137.
29. Appeldoorn RE, Wilwerding TM, Barkmeier WW. Bond strength of.composite resin to porcelain with newer generation porcelain repair systems. J Prosthet Dent. 1993;70(1):6-11.
30. Kunzelmann KH, Jelen B, Mehl A, Hickel R. Wear evaluation of MZ100.compared to ceramic CAD/CAM materials. Int J Comput Dent. 2001;4(3):171-184.
31. Attia A, Abdelaziz KM, Freitag S, Kern M. Fracture load of.composite resin and feldspathic all-ceramic CAD/CAM crowns. J Prosthet Dent. 2006;95(2):117-123.
32. Fasbinder DJ, Dennison JB, Heys DR, Lampe K. The clinical performance of CAD/CAM-generated.composite inlays. J Am Dent Assoc. 2005;136(12):1714-1723.
33. Fasbinder DJ, Dennison JB, Heys DR, Lampe K. The clinical evaluation of CAD/CAM-generated.composite inlays: six-year report [abstract]. J Dent Res. 2006;85(spec iss A). Abstract 0543.
34. Fasbinder DJ, Dennison JB, Heys D. Clinical evaluation of CAD/CAM-generated.composite inlays: ten-year report [abstract]. J Dent Res. 2011;90(spec iss A). Abstract 0379.
35. Vita machinable polymers: product information. Bad Säckingen, Germany: Vita Zahnfabrik; 2010.
36. Telio CS and Telio-CAD: Instructions for Use. Amherst, NY: Ivoclar Vivadent Technical; December 2009.
About the Author
Dennis J. Fasbinder, DDS
Clinical Professor of Dentistry
Director, Advanced Education in General Dentistry Program
Department of Cariology, Restorative Sciences and Endodontics
The University of Michigan School of Dentistry
Ann Arbor, Michigan
To read another article on CAD/CAM Materials, visit: dentalaegis.com/go/id215
For product information on CAD/CAM Materials, visit: dentalaegis.com/go/id216