Salivary Diagnostic Testing
As the physician of the mouth, the dentist is uniquely qualified to administer salivary diagnostic tests.
Jack Behn, DDS
In its genesis in 1984, deoxyribonucleic acid (DNA) fingerprinting was not applied to the diagnosis of disease, but rather to police forensics to enable detectives to positively identify criminals.1 DNA fingerprints, like physical fingerprints, are unique to each person, but in DNA fingerprinting, detectives would use DNA evidence found at a crime scene to see if it matched the DNA of the suspect(s).
Over the past few decades, DNA tests have evolved to having hundreds of medical applications that actually benefit living human beings.2 For example:
- Screening embryos for disease and/or possible birth defects
- Finding out if a person carries a gene for a specific disease
- Testing for genetic diseases in children and adults before they cause symptoms
- Confirming a diagnosis in a person who has disease symptoms
- Pharmacogenetic testing to provide individualized drug therapies for the treatment of diagnosed disease(s)
DNA tests can be broken into five categories: diagnostic testing, predictive testing, pre-symptomatic testing, carrier testing, and prenatal testing.
- Diagnostic tests are used to confirm a diagnosis when a person has signs or symptoms of a genetic disease.
- Predictive tests can show which individuals have a higher chance of getting a disease before symptoms appear.
- Pre-symptomatic testing shows which family members are at risk for a certain hereditary condition.
- Carrier testing can indicate if someone is a carrier of a gene alteration for an inherited disorder called an autosomal recessive disorder that could be passed on to their children.
- Prenatal testing is used to screen for common genetic disorders such as spina bifida and Down syndrome. It is typically performed on pregnant women who are age 35 or older because they are at higher risk for having a child with a chromosomal abnormality.
The Emergence of Salivary DNA Tests
DNA is part of every cell of every multicellular living thing, and can be extracted by taking a specimen from virtually any part of the human body, such as hair, skin, finger or toenails, and also from bodily fluids including blood, saliva, sweat, and semen.
When genetic DNA tests were first introduced, drawing blood was the most common way to obtain the DNA sample for analysis. For decades, blood was the bodily fluid of choice for conducting any type of genetic test.
Yet virtually any DNA test that uses blood to obtain the DNA can also be performed using saliva as the DNA source, because saliva contains serum, mucosal skin cells, and white blood cells. It also contains bacterial cells, which is why saliva is an excellent source for identifying certain disease-causing pathogens: the DNA extracted from bacterial cells in saliva tells us what types and species of bacteria are present in the mouth.3-7
It makes perfect sense to use saliva as the DNA specimen for several reasons. First, blood extraction can be painful for the patient. In addition to the discomfort associated with the needle, some patients pass out at the sight or even just the thought of a needle. Secondly, when it comes to administering a blood test, even the most skilled clinician can have difficulty “finding” the right vein in some patients, which can require multiple needlesticks, thereby increasing the patient’s anxiety and also causing more pain. Salivary DNA testing is more comfortable for the patient as well as easier for the administering clinician.
What DNA Clues are Found in Saliva?
In addition to what human DNA can tell us about a person’s genetic code, another kind of DNA test can reveal the presence of other living organisms within a host medium (saliva, blood, tissue, etc), such as pathogenic bacteria, by identifying the DNA of the bacteria. In fact, when screening for pathogens, saliva is a superior DNA specimen medium. That is because saliva consists of several bodily fluids: gingival crevicular fluid, which has a composition similar to blood serum, and fluid released from the salivary glands.
Furthermore, bacterial DNA can be extracted whether the bacteria in the specimen are alive or dead. Therefore, there is no need for special handling or immediate sample analysis, as is a requirement with tests that must use living samples to work properly.
How DNA is Identified
As mentioned, saliva contains both human and bacterial DNA. Both kinds of DNA can be extracted and analyzed through a laboratory process called polymerase chain reaction.2 In molecular biology, polymerase chain reaction, or PCR, is a technique for cloning a particular piece of DNA in a test tube. To perform PCR, the laboratory must know at least a portion of the sequence of the DNA molecule they wish to replicate. This process was developed in 1983 by American biochemist and Nobel laureate, Dr. Kary Banks Mullis. PCR is an indispensable technique for cloning DNA so that it can be analyzed for the identification of hereditary diseases, as well as the detection and diagnosis of infectious disease.2
The PCR process works like this: Once the saliva samples are received at the laboratory, tiny drops of the sample are syringed into separate reaction tubes in a testing block. Specific polymerase enzymes, such as Taq polymerase, as well as other primers and buffers, are added to each sample. These are necessary components for DNA synthesis in the laboratory. The sample-containing tubes are then placed into a thermocycler device. PCR usually consists of a series of up to 40 repeated temperature changes called thermal cycles. The thermocycler heats and cools the reaction tubes to achieve the temperatures required at each step of the reaction process.
When the DNA sample is heated to 90oF, its strands separate and mix with the primers. If the primers find their complementary sequences in the DNA, they bind to them; this effectively creates a duplicate of that DNA strand. The process is repeated, and those two DNA strands are separated and once again polymerized, resulting in four strands. The process is exponential—those 4 strands become 16, those 16 become 256, and so on. After 30 complete thermocycles (requiring approximately 90 minutes in total), over 1 billion DNA strands are produced from the original single strand.
PCR plays an integral part in the early diagnosis of diseases and also in confirming the presence of a genetic polymorphism, or variant, which can tell if a person has a predisposition or increased susceptibility to a specific disease or condition. PCR also permits identification of mycobacteria, anaerobic bacteria, or viruses from several sample sources, including saliva. The basis for PCR diagnostic applications in microbiology is the detection of infectious agents and the discrimination of non-pathogenic from pathogenic strains by virtue of specific genes.
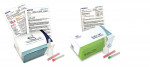
As the physician of the mouth and gatekeeper of systemic health, the dentist is a well-qualified and appropriate clinician to administer salivary diagnostics tests. Dentistry is already leading the charge on this front. For example, the UCLA School of Dentistry, headed by oral biology professor David Wong, has been conducting extensive research in the use of salivary biomarkers for diagnosing cancer and other diseases for several years. However, according to recent reports, product development and commercialization are still several years away.8 At the current time, only OralDNA® Labs, Inc. (www.oraldna.com), a subsidiary of Quest Diagnostics, is providing dentists with three non-invasive salivary diagnostic tests in the United States (Figure 1).
- MyPerioPath® identifies the type and concentration of specific perio-pathogenic bacteria that are known to cause periodontal disease and helps support clinicians with better risk assessment and personalized treatment options for more predictable patient outcomes.
- MyPerioID® PST® identifies individual genetic susceptibility to periodontal disease and enables clinicians to establish which patients are at increased risk for more severe periodontal infections due to an exaggerated immune response.
- OraRisk® HPV is a non-invasive, easy-to-use screening tool to identify the type(s) of oral HPV, a mucosal viral infection that could potentially lead to oral cancer, and in turn, enables the clinician to establish increased risk for oral cancer and determine appropriate referral and monitoring conditions.
All three of the tests consist of a sterile saline ampule, funneled collection tube with screw cap, two barcode labels (one for patient chart), and a plastic specimen bag. To begin the testing process, the patient’s name and date of birth are recorded on the barcode label. The label is then affixed lengthwise to the collection tube.
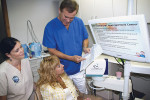
Saliva collection is then performed (Figure 2). It must be done prior to any cleaning, polishing, rinsing, or other disturbance of the oral environment. First, the patient is instructed to vigorously swish the entire ampule of saline around the entire mouth. For the OraRisk HPV Test, patients are required to gargle deeply as well, in order to collect DNA from the back of the throat.
After 30 seconds, the patient expectorates into the funneled specimen collection tube. The funnel is removed and the cap is tightly screwed onto the collection tube, then placed into its own plastic specimen transport bag. Test order information is entered into the OralDNA secure website. The saliva specimen is then shipped from the dental office via the pre-paid FedEX® envelope to OralDNA Labs, headquartered in Brentwood, Tennessee.
All of the DNA-PCR testing is done by OralDNA Labs and reports are sent back to the clinician within 5 to 10 business days via secure online web portal, depending on the test being performed. Test results should be shown to and discussed with the patient, as they serve to support the clinician’s diagnosis and help make their condition “real” (ie, “seeing is believing”). Depending on the severity of the periodontal disease, or whether the OraRisk HPV test result is positive for a high risk type of oral HPV infection, the clinician can follow his/her standard referral protocol.
Conclusion
The application and clinical relevance of DNA-PCR testing should hold equal importance among virtually all professional dental disciplines, including general practitioners, periodontists, prosthodontists, and pediatric dentists alike.
DNA testing has become increasingly commonplace in the medical field to assist doctors in the early “pre-symptom” diagnosis of patients with a family history of diseases such as those affecting the lungs and heart, degenerative disorders (such as Parkinson’s), brain diseases (such as Alzheimer’s), and certain types of cancer.7 Now that salivary DNA testing is available to the dental profession, it too can benefit from the clinical and hereditary insights the test results can provide.
References
1. de Lange C. Alec Jeffreys: The “father of DNA evidence.” New Scientist. September 30, 2009.
2. National Human Genome Research Institute. Polymerase Chain Reaction (PCR) Fact Sheet. Available at: https://www.genome.gov/10000207. Accessed May 16, 2011.
3. Malamud D, Tabak L. Saliva as a diagnostic fluid. New York: New York Academy of Sciences, 1993.
4. Kaufman E, Lamster IB. The diagnostic applications saliva: a review. Crit Rev Oral Biol Med. 2002;13(2):197-212.
5. Choo RE, Huestis MA. Oral fluid as a diagnostic tool. Clin Chem Lab Med. 2004;42(11):1273-1287.
6. Samaranayake L. Saliva as a diagnostic fluid. Int Dent J. 2007;57(5):295-299.
7. Segal A, Wong DT. Salivary diagnostics: enhancing disease detection and making medicine better. Eur J Dent Educ. 2008;12(Suppl 1):22-29.
8. Arellano M, Jiang J, Zhou X, et al. Current advances in identification of cancer biomarkers in saliva. Frontiers in Bioscience. 2009;1(1):
296-303.
About the Author
Jack Behn, DDS
Private Practice
Plantation, Florida