Repairing Severely Worn Dentition
Producing optimal esthetics through proper communication and predictable techniques.
By Brad Jones, FAACD | Jared Slovan, DMD
More and more, patients are presenting to the dental office demanding the best in smile design and the desire for a more youthful and attractive appearance.1 While the tools and materials that the dental professional chooses are integral to producing such results, a few additional factors can mean the difference between success and failure.
First is the need for multidisciplinary treatment approaches and proper communication between the dentist, technician, and most importantly, the patient.1 Another essential in achieving the restorative goals is previewing, or test-driving, the restorations.
With advances in technology and provisional materials, dental professionals can now provide patients the opportunity to see how their new restorations can and will appear.1-3 By allowing patients to test-drive their restorations, dentists and technicians can undertake cases with a better understanding of their desires, while improving the accuracy and predictability of even their most challenging cases.1-3
Lithium Disilicate
Although the test-drive technique can be crucial to success, material selection is still of the utmost importance.1-3 Using this technique, this case demonstrates the use of pressable lithium disilicate to restore severely worn teeth and a reverse smile line in the anterior region with thin, minimally invasive veneers.
Lithium-disilicate glass-ceramic (IPS e.max®, Ivoclar Vivadent, www.ivoclarvivadent.com) is an innovative all-ceramic that contains approximately 70% by volume needle-like crystals in a glassy matrix.4,5 The controlled size, shape, and density of the material's unique crystalline structure allows for greater strength and durability, while presenting a relatively lower refractive index. Demonstrating excellent optical properties, like translucency, lithium disilicate offers optimal esthetics when compared to traditional veneering materials.4-6
Currently available in two unique processing forms, lithium disilicate can be used for a variety of indications. Lithium disilicate for computer-aided design and manufacturing (IPS e.max® CAD, Ivoclar Vivadent) can be used with either laboratory or chairside CAD/CAM technology and demonstrates a flexural strength of 360 MPa.5,7 Comparatively, pressable lithium disilicate (IPS e.max® Press) is fabricated using a wax hot-press technique and demonstrates a strength of 400 MPa.5,6 Although both products are composed of the same materials, the difference in strength can be attributed to the size and length of the lithium-disilicate crystals in the two forms. All other properties, however, are similar and the ability to utilize two different techniques is beneficial.
Additionally, because restorations composed of lithium disilicate demonstrate greater strength and due to the presence of the glassy matrix, restorations may be conventionally cemented or adhesively bonded.5,8,9 With greater edge strength, lithium-disilicate restorations can also be finished thinner—without concerns of chipping. Therefore, restorations can be pressed as thin as 0.3 mm and lithium disilicate is indicated for use in minimally invasive inlays and onlays, partial crowns and crowns, bridges in the anterior and premolar region, minimally invasive veneers, and for implant superstructures.6,10,11 Available in a variety of translucencies, including high translucency (HT, 16 A-D and 4 BL Shades), low translucency (LT), medium opacity (MO), and impulse ingots (Value, Opal), lithium-disilicate CAD and Press (IPS e.max) restorations are ideal even in the most challenging cases.
Case Presentation
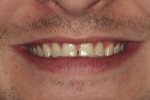
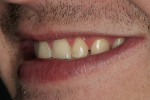
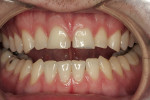
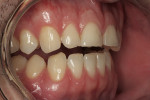
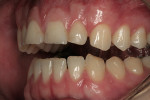
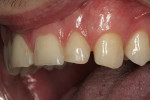
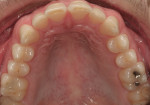
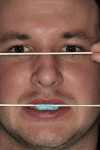
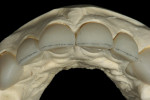
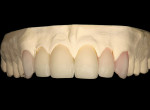
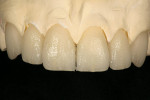
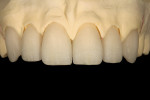
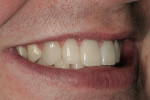
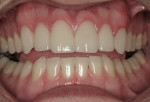
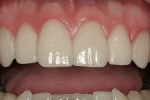
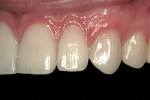
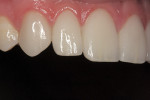
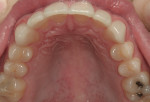
A 27-year-old man presented with severely worn maxillary dentition on teeth Nos. 6 through 11 and a reverse smile line (Figure 1 through Figure 7). The patient was very conscious of his worn teeth and he subconsciously restricted his smile, often covering his maxillary teeth with his upper lip. After examining the patient further, treatment options were discussed for teeth Nos. 6 through 11, including in-office composite veneers and laboratory-fabricated veneers—the latter was ultimately chosen.
Treatment Plan
Overall, it was decided that the main focus of treatment would be the achievement of correct incisal edge positioning, which would be determined in part by the resting position of the maxillary incisal edges on the lower lip, along with phonetic formation. This was examined and adjusted during the test-drive process, then communicated to the laboratory. Due to its lingual placement and negative reflectance on the buccal corridor, tooth No. 12 was also included in the process.
To give the patient a better understanding of how the laboratory-fabricated veneers would appear on his teeth with the reverse smile line corrected, a test-drive provisional technique was suggested. Upper and lower polyvinyl siloxane (PVS) impressions were taken, followed by a bite registration with stick bite and photographs of the patient with the stick-bite impression in place. Additionally, a photograph of the patient holding a dental swab stick across the pupils of both eyes, which is parallel to the swab across the incisal edges of his maxillary teeth, was also taken for the stick bite.
The patient was then photographed in his forehead-to-chin smile and relaxed poses. These photographs were sent with the aforementioned diagnostic information to the laboratory, where a wax-up model of the six maxillary anterior teeth was fabricated. The laboratory also created a pressure-formed temporary stent of the waxed-up teeth at this time.
After receiving the wax-up model and stent, the patient returned to the office. The stent was tried in first to obtain an orientation point for insertion and to visually identify landmarks. Therefore, the midline was marked on the facial of the stent with a marker, as was each tooth position. Then, the temporary stent was filled with A2 temporary material and placed into the patient's mouth, while applying pressure on the facial and lingual gingival areas to "pinch off" the excess material. This was completed without primer or bonding agent being applied to the tooth surfaces. After the remaining flash on the gingival areas and other teeth was cleaned off, a photograph was taken of the patient smiling with his test-drive provisional in place; one copy was given to the patient to take home, another was placed in his chart.
The Test-Drive Process
The idea behind the test-drive process is to allow the patient to wear their new smile for 4 to 5 hours at home, with loved ones, or with friends. This enables the patient to gain feedback and confidence in their new smile through understanding how the completed restoration will appear to themselves and others. However, the test drive is only for esthetic purposes and should not be in place when eating. Typically, after 4 to 5 hours, the test drive is complete, and the temporary can be removed simply by pinching the front teeth with a dry paper towel and removing the unit as a whole. Any remaining pieces of the temporary material can then be removed via flossing and brushing.
Clinical Preparation
In this particular case, after the patient saw the results of the provisional restorations, he was committed to the veneer process. He did not wish to leave the office and wear the temporaries for 4 to 5 hours. Instead, he wanted to start the veneer process right then and there. Therefore, the entire American Academy of Cosmetic Dentistry preoperative photograph series was taken.
First, five carpules of 4% articaine with 1:100,000 epinephrine with local infiltration were administered to anesthetize the patient. Red articulating paper was then used to check the occlusal position of the lower anterior maxillary dentition, ensuring that the preparation would not invade the contacts. It was also important that the occlusion was on natural tooth structure, not on porcelain. Teeth Nos. 6 through 12 were the first to be prepared for laboratory-fabricated lithium-disilicate glass-ceramic veneers (IPS e.max Press) by breaking the contacts. Electrosurgery was then completed on the facial surfaces of teeth Nos. 9 through 11 to adjust the facial height and create harmony. Shade selection began with photographs of stump shades and the patient's existing teeth Nos. 3 through 5 and Nos. 13 through 15. Because the patient wanted the veneers to blend into the existing dentition, without overtly "sticking out," the shade chosen for the centrals was A1 (IPS e.max Press), blending back into the premolar shades of A3 (IPS e.max Press). By choosing these particular shades, it was possible to create a gradual transition of shading.
After choosing the proper shades, photographs of the preparations were taken at multiple angles, close up, and with retractors. A stick bite of the preparations and the accompanying photographs provided invaluable information to the laboratory for the development of the definitive restorations. The final impression was then taken with heavy- and light-body PVS impression material in a custom tray.
The temporary stent was filled with A1 temporary material and placed into position, using the prior marker identifications for guidance. The stent was then fully seated and pressure was placed on the facial and lingual gingival areas to "pinch-off" the excess temporary material. After the provisional material had fully set, the temporary stent was removed along with the majority of the excess provisional material. Any remaining flash material was "flaked off" the gingiva and the single-unit temporary was carefully removed. Fine adjustments were made along the facial surfaces, and the interproximal areas were contoured so that they would not impinge on and push the gingiva away from the temporary restorations.
Once the correct facial and interproximal gingival contours were established, the temporary restorations were polished. A layer of a low-viscosity, light-curable resin was placed on the temporaries to obtain a glossy and lifelike appearance, and light-cured. The preparations were spot-etched on the facial and rinsed. A single-component adhesive (OptiBond® Solo, Kerr Corporation, www.kerrdental.com) was then placed on the facial and the temporary restorations were placed and cured.
This method was preferred over the "shrink-wrap" method because it gave the dentist the ability to control the facial and interproximal gingival contours more precisely by adjusting them on the temporary restorations extraorally, while still being able to insert and remove them to check and verify fit.
With the provisionals bonded in place, photographs were taken of the temporary restorations from the front, left and right, up-close with retractors, full-face, with the stick-bite, and with pupil parallelism (Figure 8, Figure 9 and Figure 10).
Clear stick-bite material is always used during this process in all cases to provide a clear incisal position to the laboratory—relating to the other teeth and stick-bite position. It is important to note that in this case, the patient did have a posterior interference on the left side, which was corrected with an occlusal adjustment after which the patient was sent home with 800 mg of ibuprofen and a bottle of peroxyl to use to rinse his mouth. This allowed treatment to be continually focused on the anterior gingiva that had been adjusted.
All diagnostic and necessary information was then sent to the laboratory to allow for the creation of the definitive restorations.
Laboratory Fabrication
After receiving all pertinent diagnostic and case information from the dentist, the laboratory technician could begin creating the definitive restorations from IPS e.max Press.
To begin the laboratory process, a matrix was formed from casts of the provisional restorations and molten wax was injected. Then it was necessary to refine the shape and contours and seal the margins. Completed wax-ups were then sprued, invested, burned-out, and pressed using the new Impulse Opal 2 lithium-disilicate ingots (IPS e.max Press). After pressing, the restorations were de-vested and placed in a dissolving liquid to eliminate the surface reaction layer. The lithium-disilicate veneers were then cut from the sprues and compared to the model of the provisionals.
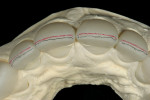
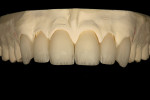
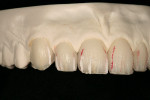
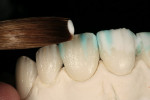
After pressing was complete and accuracy confirmed, the facial incisal edge was marked with a red pencil, followed by marking with a 0.3-mm lead pencil (Figure 11). The pencil marks were used to accurately indicate a line 0.5 mm lingually for facial reduction. Reduction was then completed using a K6974 220 centered diamond disc (KOMET USA, www.kometusa.com) (Figure 12). Using the red pencil once again, the incisal interproximal area to be troughed-out was marked and troughing was completed with the K6974 220 centered diamond disc (KOMET USA) (Figure 13). This trough was created to carry the gray-blue stain, which imparted an incisal effect similar to that of the patient's natural dentition (Figure 14).
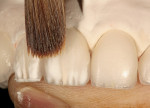
Universal stains were then applied to emulate the high- and low-value details found in the internal structures of the patient's natural teeth (Figure 15). After building the center lobe with light and yellow orange mamelon powders (IPS e.max), OE4 white dentin powder (IPS e.max) was feathered apically with a specialized dental porcelain build-up brush to create the mesial and distal internal lobes (Figure 16). Upon completion of this process, the internal effects were fired (Figure 17).
After firing, OE1 (opal clear) and TI1 (high-value enamel) powders (IPS e.max) were carefully segmented to maintain OE1 on the outer most incisal, mesial, and distal edges (Figure 18). Once the contoured enamels had been placed, they were fired (Figure 19). Upon completion of firing, the facial lobes and surface textures were created using an 842r diamond bur (KOMET USA) (Figure 20). The restorations were then glazed, polished, and ready for delivery (Figure 21).
Final Seating
To follow-up on the healing of the gingival tissues and to discuss the patient's views on the temporary restorations, in regards to their size, shape, and shade, the patient returned to the office for a 1-week postoperative examination. Because no changes to the provisionals were required, delivery and final seating of the veneers on Nos. 6 through 12 could begin.
The patient was found to be healing very well and had been compliant in his use of the peroxyl rinse. After administering four carpules of 4% articaine with 1:100:000 epinephrine with local infiltrations, the patient was fully anesthetized and fitted with a lip and cheek retractor. The provisionals were sectioned, removed, and the preparations cleaned. At this point in the treatment it was very clear that the gingiva was in excellent condition. The IPS e.max Press veneers were then tried-in, requiring only minimal adjustment interproximally. The restorations were then dried and silanized with a universal primer (Monobond S, Ivoclar Vivadent). Light air was blown on the veneers and preparations to remove any contaminants and to dry the primer.
A self-etching and self-curing primer (Multilink A and B, Ivoclar Vivadent) was then mixed and applied to the preparations for 15 seconds and light air was applied. Multipurpose adhesive cement (Multilink Automix, Ivoclar Vivadent) was placed on the veneers, and the veneers for Nos. 8 and 9 were seated from the front of the patient to ensure proper alignment and position—as opposed to seating from one side or another.
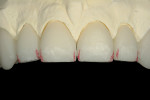
Upon seating the veneers on teeth Nos. 8 and 9, excess cement was removed around the margins and interproximally with a #6 sable brush, while applying seating pressure. When the excess cement was removed, the restoration was tack-cured on the facial and lingual surfaces by placing the curing tip half on the veneer and half on the gingiva. The remaining cement was cleaned through the use of a sickle scaler and dental floss. Glycerin gel was then placed on all margins and a final cure was completed on the veneers from the lingual, facial, interproximal, and incisal for 20 seconds on each surface. The remaining veneers were then placed in sets of two—Nos. 7 and 10; Nos. 6 and 11; and, finally, No. 12. After all veneers were in place, cured, and cleaned, the contacts were verified and cleaned. At this time, the occlusion was also adjusted and the restorations polished.
Once treatment was concluded, the patient was fitted for a full-upper nightguard to protect the dentition and veneers from parafunctional habits. Overall, the patient was very satisfied with the pressed lithium-disilicate restorations—specifically, the harmonious and lifelike blending with the natural dentition that was created through the selection and placement of the veneers using the test-drive process (Figure 22, Figure 23, Figure 24, Figure 25, Figure 26, Figure 27, Figure 28, Figure 29 and Figure 30).
Conclusion
In cases of severely worn dentition and reverse smile lines, it is crucial that the dentist, laboratory technician, and patient remain in constant communication throughout the entirety of treatment. By providing the laboratory with all necessary diagnostic information (eg, clinical photographs, stick-bite, impressions, etc), the dentist can be sure that the definitive restorations will fit, function, and display the esthetics desired by the patient. And the test-drive process offers greater predictability in cases by gaining a better understanding of how the finished restorations will appear and function in the patient's mouth, while gaining direct feedback from the patient throughout treatment.
References
1. Ohyama H, Nagai S, Tokutomi H, Ferguson M. Recreating an esthetic smile: a multidisciplinary approach. Int J Periodontics Restorative Dent. 2007;27(1):61-69.
2. Reshad M, Cascione D, Kim T. Anterior provisional restorations used to determine form, function, and esthetics for complex restorative solutions, using all-ceramic restorative systems. J Esthet Restor Dent. 2010;22(1):7-16.
3. Powell T. Excellence and predictability: not an accident. Dent Today. 2009;28(9):122-124.
4. McLaren EA, Phong TC. Ceramics in dentistry: classes of materials. Inside Dentistry. 2009;5(9):94-103.
5. Tysowsky GW. The science behind lithium disilicate: a metal-free alternative. Dent Today. 2009;28(3):112-113.
6. Reynolds JA, Roberts M. Lithium-disilicate pressed veneers for diastema closure. Inside Dentistry. 2010;6(5):46-52.
7. Helvey GA. Chairside CAD/CAM: Lithium-disilicate restoration for anterior teeth made simple. Inside Dentistry. 2009;5(10):58-66.
8. Dudney TE. Unlock that combination. Dental Products Report. 2009;43(3):60-62.
9. Fabianelli A, Goracci C, Bertelli E, Davidson CL, Ferrari M. A clinical trial of empress ii porcelain inlays luted to vital teeth with a dual-curing adhesive system and a self-curing resin. J Adhes Dent. 2006;8(6):427-431.
10. Ritter RG, Rego NA. Material considerations for using lithium disilicate as a thin veneer option. J Cosmet Dent. 2009;25(3):111-117.
11. Lowe RA. No-prep veneers: a realistic option. Dent Today. 2010;29(5):80-86
About the Authors
Brad Jones, FAACD
Owner
Smile, Inc.
Boise, Idaho
Jared Slovan, DMD
Private Practice
Mt. Pleasant, South Carolina