Interim and Definitive Metal-Free Partial Dentures
The design of the prosthesis should be based on an understanding of properties and behavior of the particular system chosen.
Functional and esthetic restoration of the partially edentulous patient includes a range of treatment options, each with its own degree of invasiveness and reversibility along with risks and benefits. Especially for the patient who suddenly faces partial edentulism, final treatment decisions and commitment takes time. In such cases, steps toward final restoration can include an interim prosthesis. In addition to offering an esthetic preview, an interim removable partial denture (RPD) should minimally impact future treatment. The use of an interim metal-free RPD is convenient for the dentist, relatively inexpensive, patient-friendly, and is often completely reversible.
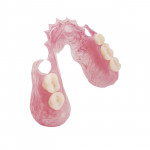
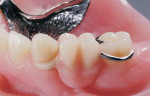
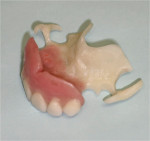
While specific design criteria for interim RPDs remain unclear, manufacturers of metal-free flexible RPD polymers have established guidelines based on material properties. Laboratories familiar with the behavior of specific materials have additional insight regarding critical factors such as connector design and dimensions, clasps, and the retention of artificial teeth to ensure reliability. With the emergence of novel materials and strong patient demand for metal-free RPDs, the distinction between interim and definitive prosthesis has become blurred. Survival of interim RPDs beyond the interim period resulted in clinical claims for long-term use of products that cannot be repaired, relined, or clinically modified when needs arise. The purpose of this article is to assist laboratories and clinicians in material selection and design featuring two popular thermoplastic, flexible RPD products, nylon-based Lucitone® FRS (DENTSPLY Trubyte, www.trubyte.dentsply.com), and acetal resin-based Thermoflex (DENTSPLY Prosthetics, www.prosthetics.dentsply.com) (Figure 1 and Figure 2), each with unique advantages.
Properties and Design Principles
A major addition to the metal-free RPD market has been nylon, offered in various formulations. Depending on the carbon chains that carry the carboxyl and amino groups comprising nylon, physical properties vary. Specific product chemistry information may be proprietary and hard to obtain. Nylon chemistries are well tolerated biologically so nylon product selection is independent of allergy or toxicity concerns. The design of the prosthesis, however, should be based on an understanding of properties and behavior of the particular nylon chosen. Resiliency (stiffness) and strength differences suggest the importance of designing nylon RPDs in accordance with manufacturer recommendations and laboratory familiarity. As a class, all nylons demonstrate higher water sorption and creep than most dental polymers.1-3 In general, toughness (resistance to fracture), flexibility, design simplicity and exceedingly rare allergy response are the features supporting nylon RPD popularity.
Another addition to the metal-free RPD market is polyoxymethlene (polyacetal) referred to simply as acetal resin in dentistry. Chemistry differences that may exist among acetal resin products are indeed subtle. All acetal resins meet ISO specifications limiting water sorption and all exhibit lower creep and superior abrasion resistance with higher surface luster than nylons.4,5 The higher stiffness of acetal resin supports conventional clasp designs, connectors, and other components with some compensation required. In one report comparing clasp flexibility and retention, the author suggested acetal clasp dimensions should be 30% shorter with 40% greater cross-sectional area versus cast metal.6,7
While these numbers indicate acetal framework bulkiness, some bulk reduction is possible by using portions of the major connector, minor connectors of even guide planes for direct retention. No formal design recommendations exist for deliberate engagement of undercuts using framework components other than clasps, but the practice is common and has resulted in no problems identified by the authors. Certainly engagement of deeper undercuts than what would be possible using cast metal helps prevent food traps, improving hygiene and retention of the RPD. What is most interesting about acetal RPDs is that conventionally styled frameworks can be constructed with acrylic bases processed onto the frame. This offers advantages with respect to relining, repairing, and retaining artificial teeth on the RPD.7
Following are short case reports highlighting a Lucitone FRS (nylon) and a Thermoflex (acetal) RPD with justification for material selection and prosthetic design.
Case 1
A new patient made an appointment to discuss a short-term solution to the problem her dentist was having securing a no-preparation, resin-bonded FPD replacing congenitally missing teeth Nos. 23 and 26. After consultation with her regular dentist, who confirmed her referral to a specialty practice for grafting and implant placement, she asked what we could do to get her by for a few months. Committed to definitive treatment but needing time to get things in order, she requested a metal-free interim RPD.
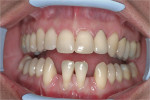
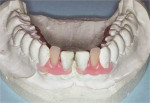
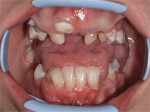
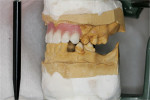
After treatment plan discussions with her general dentist and obtaining informed consent, alginate impressioning for construction of a Lucitone FRS (DENTSPLY Prosthetics) RPD was completed. While explaining proposed treatment to the patient and her dentist, concern was expressed that the interim RPD would be carefully monitored for soft tissue impingement, which could complicate future treatment. As nylon exhibits much higher creep than conventional prosthodontic materials, rest seats on FRS partial dentures are ineffective. Lucitone FRS was chosen because of its unique nylon network, which offers superior creep resistance with slightly higher stiffness than other nylons. Porcelain teeth were selected because nylon formulations can be challenging to bond to artificial teeth. Through-the-tooth diatoric retentions are required weakening acrylic teeth, especially incisors. A pinned porcelain tooth (Bioform, DENTSPLY Prosthetics) was the strongest option. Figure 3 hows the pretreatment condition, Figure 4 shows the RPD on the master model with sufficient height of the artificial teeth to functionally balance anterior guidance incisal-edge matching.
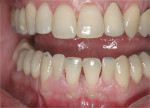
Figure 5 shows the anterior contacts and guidance. It is important at this time to confirm no movement of the denture base, which could compress soft tissues accelerating gingival recession. Figure 6 shows the final result; note how nylon's translucency contributes to gingival esthetics.
Case 2
This female patient, a very shy adult patient seeking only limited care, presented in a nearby public health clinic requesting removal of malpositioned, retained deciduous teeth C and G (Figure 7).
After review of a panoramic radiograph, missing teeth Nos. 6, 7, 9, 10, and 11 were confirmed absent. Tooth No. 8 was vital and healthy but only partially erupted with an underdeveloped root form. The patient was asked if she would consider wearing a partial denture resting atop tooth No. 8. Her reply was: “I'm not a vain person.” She was then asked her if she could bite a sandwich, and she replied, “I cut things like sandwiches with a knife.” After a prophylaxis and removal of the malpositioned deciduous teeth, alginate impressions were made with a static maxillo-mandibular relation record. Models were articulated and artificial teeth were assembled on a wax baseplate for try-in (Figure 9 and Figure 10). The try-in confirmed the esthetics, resulting in a very surprised patient who cautiously asked, “Can I take home a photograph to show my husband?”
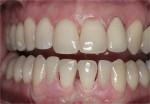
When the patient returned with her husband, both consented to treatment including an RPD. A cast framework partial was ruled out due to cost as well as patient reluctance to accept irreversible mouth preparation. Acetal resin was then suggested for the framework with processed conventional acrylic base, which could be relined. The products selected included Thermoflex (DENTSPLY Prosthetics) framework with Eclipse acrylic base and bonded Portrait IPN teeth. Delivery was without incident and the acrylic base was relined 12 weeks later when healing was complete. At that appointment the patient smiled and said, “I now know how it feels to bite into a sandwich” (Figure 11 and Figure 12).
Conclusion
RPDs can be transitional, interim, or long-term prosthetic devices. A variety of partial denture materials are available and satisfactory results can be achieved with most materials under the right conditions. Metal-free, flexible partial dentures are preferred by patients who cite “comfort” as the primary reason.8
Both nylon and acetal resin are materials worthy of consideration when treatment planning patients for RPDs. Thermoflex offers the advantage of a conventional styled framework with acrylic denture base materials whereas nylon offers excellent gingival esthetics and reduced allergy concerns compared to acrylic resins.
Disclosure
Dr. Kurtzman is a current consultant for DENTSPLY. Dr. Sundar is an employee of DENTSPLY.
References:
1. Stafford GD, Huggett R, MacGregor AR, Graham J. The use of nylon as a denture-base material. J Dent. 1986;14(1):18-22.
2. Yunus N, Rashid AA, Azmi LL, Abu-Hassan MI. Some flexural properties of nylon denture base polymer. J Oral Rahabil. 2005;32 (1):65-71.
3. Stafford GD, Bates JF, Huggert R, Glantz PO. Creep in denture base polymers. J Dent. 1975;3(5):193-197.
4. Arikan A, Ozan YK, Arda T. Akalin B. Effect of 180 days of water storage on the transverse strength of acetal resin denture base material. J Prosthodont. 2010;19(1):47-51.
5. Arikan A, Ozkan YK, Arda T, Akalin B. An in vitro investigation of water sorption and solubility of two acetal denture base materials. Eur J Prosthodont Restor Dent. 2005;13(3):119-122.
6. Wu JC, Latta GH Jr, Wicks RA, et al. In vitro deformation of acetyl resin and metal alloy removable partial denture direct retainers. J Prosthet Dent. 2003;90(6):586-590.
7. Turner JW, Radford DR, Sherriff M. Flexural properties and surface finishing of acetal resin denture clasps. J Prosthodont. 1999;8(3):188-195.
8. Unpublished data. Dentsply Prosthetics Clinical Research Center Clinical comparison of patient preference and performance of acetal RPDs with Eclipse versus Vitallium with Eclipse. 2003-2006.
About the Author
Nels O. Ewoldsen, DDS, MSD
Private Practice
Rockville, Indiana
Gregori Kurtzman, DDS
Private Practice
Silver Spring, Maryland
Veeraraghavan Sundar, PhD, MBA
Manager, New Product Commercialization
DENTSPLY Prosthetics
York, Pennsylvania