The Inman Aligner
Alignment, bleaching, and bonding can enable clinicians to takea progressive approach to smile makeovers.
By Tif Qureshi, BDS
Cosmetic dentistry has been performed in a traditional way for some time. A patient typically visits a practice where digital photographs are taken and software imaging is performed to simulate a much "improved" smile. Teeth are lengthened, gum heights evened out, golden proportion corrected, and buccal corridors widened, with embrasures and connectors symmetrically reducing as the teeth go further back. While known to produce the technically perfect smile, this formula is also problematic; often implanting an image of a perfect smile in the mind of the patient, who accepts this as an ideal goal.
The patients never really have a chance to see their own teeth gradually improving, and make a choice to accept a compromise on the ideal smile. In many cases, a wax-up is then made, and the teeth are prepared to allow space for the veneers to be seated. If teeth are misaligned, the dentist simply cuts teeth back to allow space for the ceramic work, which could vary from minimal or no preparation in additive cases. However, significant amounts of healthy tooth structure are often removed when teeth are proclined or rotated.
The concept of progressive smile design offers a completely different approach. In the United Kingdom and Europe, education in the advanced use of the Inman Aligner has created an explosion in the use of this removable system as a way of aligning teeth quickly. The system is removable and very fast, and patients who were previously put off by brackets and months of treatment can now achieve alignment in 6 to 16 weeks, with a brace that can be worn for as little as 16 hours a day.
The aligner is removable and, therefore, it is easy to bleach during the last part of the alignment phase using sealed trays rubber trays, which allows patients to see their own teeth gradually but dramatically improving. Patients who had previously wanted an ideal smile offered through veneer placement commonly accept esthetic compromises because they can accept their own teeth looking better, which the following case will outline.
The Inman Aligner
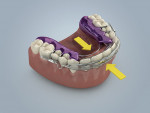
The Inman Aligner™ (www.inmanaligner.com) is a development of the traditional spring aligner (Figure 1). In 1974, Barrer described orthodontic movement of teeth using removable spring appliances.1 Donal Inman, CDT, invented the Inman Aligner in 2001. Inman created a patented design that uses the gentle, steady, and consistent forces generated by nickel titanium (NiTi).2,3 Piston-like lingual and labial components are driven by the NiTi coils parallel to the occlusal plane, which allows some true bodily movement of teeth. Ideally, Inman Aligners are only worn 16 to 20 hours a day. Studies show that the removal of orthodontic forces for 4 hours a day reduces the risk of root resorption, and that risk of root resorption is lower in removable appliances.4,5
More than 20,000 cases have been treated with Inman Aligners in 9 years, predominantly in the United Kingdom and the United States, according to the UK and US Inman Aligner labs Nimrodental and Inman Ortho Lab, Florida. The author and two associate trainers (Drs. Tim Bradstock-Smith and Dr. James Russell) are currently completing a 5-year clinical audit with 1,200 patients, and show a 94% success rate, with 6% failure from compliance issues. To date, the audit has shown a 0% incidence of loss of vitality, root resorption, or significant bone loss.
Clinical Case
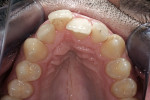
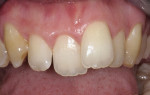
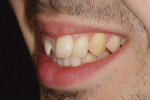
The patient presented with misaligned and discolored upper front teeth (Figure 2). He had previously attended another clinic to be assessed for a smile makeover. Computer imaging had been carried out, which had tried to address the problems with gum height, golden proportion, and narrow buccal corridors.10 Veneers had been planned, and the patient brought a printout of the ideal smile.
Part of the treatment plan required that endodontics would be carried out on the upper left central incisor. Gingival surgery was also to be carried out to harmonize the gum position. These two requirements had concerned the patient enough to seek out another opinion. The patient had considered the possibility of straightening his teeth before veneers were placed. Orthodontics was offered in the form of full clear braces, STO fixed, and full-mouth treatment.
The patient was not keen on clear braces, nor was he receptive to fixed braces being placed labially or lingually. The patient’s desire for removability and speed led to his selection of the Inman Aligner.
Arch Evaluation with Spacewize
Arch analysis was carried out to determine if the patient’s case was suitable and to calculate the amount of crowding present, to ensure enough space could be created. The amount of crowding present was calculated using Spacewize™. This software uses the principle of Hancher’s technique by taking two measurements.6 The software first measures the sum of the mesial–distal widths of the teeth to be moved. This distance is called the "Required Space" or "The Teeth."
The next step is to measure the ideal curve, described as the "Available Space" or "The Curve." The ideal arch form is then measured from the distal of the canine to canine, with the curve set up through the area where the contact points will be after orthodontics. One required occlusal photograph was taken chairside. One tooth was measured for calibration. The curve was set up digitally while directly observing the patient’s esthetic requirements and occlusion, and the amount of crowding was known immediately.
This case showed that 4.2 mm of crowding was present, which meant that this amount of space would need to be created to achieve the ideal curve. Many authors acknowledge the reduction of one half of the interproximal enamel on the mesial and distal of each incisor tooth as a safe technique.7,8 This equates to 0.5 mm per contact, making 2.5 mm of space possible between the canines. Up to 0.75 mm can be re-proximated between the canines and premolars, allowing another 1.5 mm to be created.
The total was close to the maximum allowable in the anterior region. As such, a combined midline expander was used on the Inman Aligner to create a small amount of extra space. These combined expanders allow for up to 2.5 mm of extra space to be created by tipping the canines and premolars away from the incisors.
Treatment
Impressions were taken, and the Spacewize trace was sent to the laboratory to ensure the proposed setup was clear.2 A couple of weeks later, the patient’s Aligner was fitted and the patient given oral hygiene instructions.
Minimal interproximal reduction was carried out strategically on the first appointment. The amount of stripping was carefully recorded by noting the tooth position and the size of the strip used per contact, then checking with leaf gauges. An application of topical fluoride was placed after the patient’s enamel reduction procedure. Studies have shown that there is no increased risk of caries if surfaces are smoothed correctly.9,10 Studies have also shown that, despite the decreased interproximal space, there is no increased risk of periodontal disease.11,12
Inman Aligner treatment uses progressive, anatomically respectful interproximal reduction. Despite calculating the amount of interproximal reduction needed, it is never carried out all at once. To ensure minimal risk, only a small amount of interproximal reduction (0.13 mm per visit per contact) was carried out. The patient was sent away with the Aligner. After 2 weeks, the gaps had closed due to the aligner forces. Interproximal reduction was again carried out using strips and discs. This ensured that the stripping was far more anatomically respectful than if burs had been used, and the risk of excess space formation/ gouging and poor contact anatomy had been reduced.
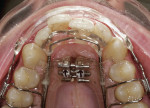
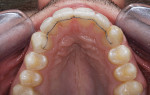
At the fitting appointment, the patient was given instructions on operating his midline expander, and was shown how to turn the screw to open the expander 0.25 mm at a time. The patient would do this once a week, and was reviewed every 3 weeks (Figure 3, Figure 4, Figure 5, Figure 6, Figure 7 and Figure 8). The patient wore the Aligner for 18 hours a day.
After 12 weeks, the patient’s teeth were starting to get close to alignment. Impressions were taken for bleaching trays. DayWhite® (Discus Dental, www.discusdental.com) was used for 35 minutes a day while the Inman Aligner was out of the mouth, and the patient was given careful instructions to ensure a good result.
Tooth whitening was performed during the last 2 weeks of aligner treatment. After this, the patient was very satisfied with the outcome, and decided not to pursue veneers. His perception of his current smile was far better than he had imagined, even though it may not fit the ideal smile design criteria. He simply asked if it was possible to do something about his irregular incisal outline.
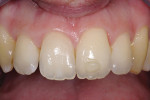
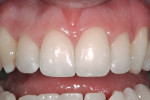
After 2 more weeks to allow color stabilization and increased bond strength, edge bonding was carried out with no preparation with IPS® Empress Direct (Ivoclar Vivadent, www.ivoclarvivadent.com) from B1 dentin and enamel shades. The patient’s lower fractured incisor was treated at the same time (Figure 9 and Figure 10).
Retention for anterior alignment is essential.13,14 A bonded canine-to-canine retainer was used. These are fixed retainers commonly made from .0195" or .0175" multi-strand stainless steel wire, which ensures that the flexibility of the arch wire allows for physiological tooth movement, and prevents bond fracture through occlusal forces. Periodontal ligament stability is also achieved.15
Conclusion
The Inman Aligner is not suitable for all case types and limitations do exist. Certain movements, such as side shifting in large space cases, are impossible. Anterior and canine guidance must also be protected but if good planning is carried out and both arches are carefully considered, it can actually be improved.
This case highlights how progressive smile design can allow a patient to make a far more informed and considered choice regarding his or her smile. It allows patients to see their teeth improve gradually but quickly, and make decisions based on what they find esthetic.
The Inman Aligner provides the ability to rapidly improve esthetic alignment at low risk to patients before irreversible techniques are used. This patient originally wanted veneers, but made his ultimate decision because he could preview the staged changes of alignment, bleaching, and bonding.
The Inman Aligner has changed cosmetic dentistry in the United Kingdom, and the concept of combined alignment, bleaching, and bonding is changing the approach toward smile design.
Disclosure
Dr. Qureshi runs hands-on courses on the Inman Aligner worldwide.
Acknowledgment
The author would like to thank Donal Inman, CDT, of Inman Orthodontics in Coral Springs, Florida and Nimrodental Lab in London, England, for his expertise.
References
1. Barrer HG. Protecting the integrity of mandibular incisor positioning through keystoning procedure and spring retainer appliance. J Clin Orthod. 1975;9(8):486-494.
2. Bowman SJ. The Inman Aligner. J Clin Orthod. 2003;37(8):432-442.
3. Warunek S, Willison B. Incisor alignment with the Inman aligner. Journal of Cosmetic Dentistry. 2005;20(4):80-92.
4. Kameyama T, Matsumoto Y, Warita H, Soma K. Inactivated periods of constant orthodontic movement forces related to desirable tooth movement in rats. J Orthod. 2003;30(1)31-7.
5. Ohm B, Linge L. Apical root resorption in upper anterior teeth. Eur J Orthod. 1983;(3):173-183.
6. Hancher P. Orthodontics for esthetic dentistry, part 1: The use of orthodontics to facilitate the esthetic restoration of anterior teeth. Journal of Cosmetic Dentistry. 2005;(20)4:74-80.
7. Sheridan, JJ. Air-rotor stripping update. J Clin Orthod. 1987;21(11):781-88.
8. Crain G, Sheridan, JJ. Susceptibility to caries and periodontal disease after posterior air-rotor stripping. J Clin Orthod. 1990;24(2):84-85.
9. El-Mangoury N, Moussa M, Yehya A, et al. In-vivo remineralization after air-rotor stripping. J Clin Orthod. 1991;25(2):75-78.
10. Radlanski R. Morphology of interdentally stripped enamel one year after treatment. J Clin Orthod. 1991;23(11):748-50.
11. Heins PJ. The relationship of interradicular width and bone loss. J Periodontol. 1988. 59(2):73-9.
12. Tal H. Relationship between the interproximal distance of roots and the prevalence on intrabony pockets. J Periodontol. 1984;55(10):604-7.
13. Reprinted: Case CS. Principles of retention in orthodontia. Am J Orthod Dentofacial Orthop. 2003;124(4):352-61.
14. Blake M, Bibby K. Retention and relapse: A review of the literature. Am J Orthod Dentofacial Orthop. 1998;114:299-306.
15. Becker A, Goultschin J. The multistrand retainer and splint. Am J Orthod. 1984;85:470-4.
About the Author
Tif Qureshi, BDS
President-Elect
British Academy of Cosmetic Dentistry