Zirconia Restorations: Perception or Evidence?
Dennis J. Fasbinder, DDS
Ceramic material science advances and results in clinical acceptance.
Because of their improved esthetic appearance, chemical resistance, and biocompatibility, all-ceramic restorations are often preferred to porcelain-fused-to-metal (PFM) restorations. Recent developments in ceramic material science have resulted in improved strength properties of modern ceramic materials, and this has generated an increase in clinical acceptance of all-ceramic crowns.
Zirconia is a crystalline dioxide of zirconium that is the strongest ceramic for the dental market today. It is a polycrystalline material that does not contain an etchable glass phase. Zirconia has several possible crystalline structures depending on the temperature.1 Pure zirconia is monoclinic at room temperature. It shifts to a tetragonal crystalline structure at temperatures above 1,170°C. A variety of materials have been added to zirconium to stabilize the tetragonal crystalline structure at room temperature. The most common form studied in dentistry is yttrium-stabilized zirconia (Y-TZP).2 It is also known as tetragonal zirconia polycrystal (TZP). The yttrium-stabilized zirconia has better physical properties than other forms of zirconia due to the stress-induced transformation toughening of the material.3 As a crack begins to propagate through the material, the tetragonal form shifts to the monoclinic form with a concomitant volumetric expansion that exerts a compressive force on the leading edge of the crack, preventing its progression.
Zirconia offers some significant physical properties that are advantageous for dental restorations besides its high strength. It has a similar color to natural teeth, which reduces the need to opaque it or mask it as would be done for a metal substructure. Zirconia also has good opacity. This may be an advantage when trying to block out underlying discolored teeth or restorative materials. It may also be a disadvantage when trying to develop a more translucent appearance to the crown. Some manufacturers can color the zirconia substructure to simulate dentin shades to improve the desired esthetic result.2
Zirconia Processing
A bi-layered restoration in the form of a PFM crown has historically been relied on for high-strength, tooth-colored crowns. Many esthetic all-ceramic crowns are generally considered not strong enough to predictably support posterior tooth function over the long term. The bi-layered crown design is based on the idea that an esthetic surface layer is fused to a strong substructure resulting in the desired combination of esthetics and strength. Although a metal substructure can provide the desired strength for a PFM crown, the metal must be masked to provide the desired esthetic result.
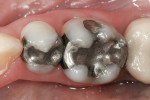
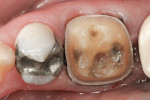
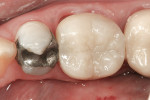
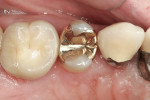
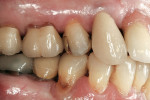
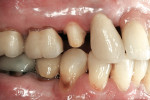
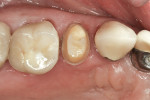
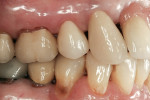
Zirconia has been considered a desirable substitute substructure for a bi-layer crown due to its high-strength properties and more tooth-like appearance. An obvious critical factor in the strength of the final restoration is creating sufficient space for the restorative material to ensure maximum strength. General guidelines for the tooth preparation for a zirconia crown include at least 1.2 mm of axial reduction, 1.5 mm of clearance in the central fossa, and 2 mm of clearance over functional cusps (Figures 1, Figures 2, Figures 3, Figures 4, Figures 5, Figures 6, Figures 7, Figures 8 and Figures 9).
There are also several specific features of the zirconia crown fabrication process that need to be addressed for a dependable result. Zirconia is a good thermal insulator. This means the substructure is a poor heat diffuser and will be slow to heat up and slow to cool down. This may be lead to problems during processing/firing the veneering porcelain. The crown must be cooled slowly or risk creating residual stress within the restoration that may lead to surface porcelain failures.
The design of the zirconia substructure is another aspect of the fabrication process that requires careful attention. Zirconia restorations require computer aided design/computer aided milling (CAD/CAM) systems to be designed and milled. Initial CAD programs had limited capability for customizing the shape of the substructure leading to uniform thimble-shaped copings. This resulted in porcelain veneering layers greater than 2 mm in thickness and placed the veneering porcelain at risk of fracture because of poor support from the coping. Comparing different coping designs, a higher fracture strength was found when zirconia core thickness was adjusted to provide uniform thickness of the veneering porcelain and good support.4 Current CAD systems have the design capability for the coping to be customized to ensure a uniform layer of veneering porcelain that is well supported by the coping. New design shapes of zirconia copings are being investigated to maximize the strength of the bi-layered restoration.
Despite a better understanding of the design and fabrication process since zirconia has been introduced, there is a perception that zirconia crowns may have an increased risk of veneering porcelain fracture compared to other esthetic crowns. But is this perception consistent with published clinical studies? A good question to consider is what constitutes acceptable data or information for an evidence-based decision? Both in vitro and in vivo studies are useful in making clinical decisions. Studies done in laboratory settings attempt to simulate clinical conditions in order to make comparative analysis of products. They may also help provide guidance during the development process of a material or technique. Once a desired level of success is achieved in the laboratory setting, clinical studies can be undertaken to ensure and document similar success in the clinical environment. No single clinical project is sufficient evidence of success. Awareness of the general trends across a number of clinical studies is a better predictor of clinical results.
PFM Crowns
PFM crowns have been in clinical practice for well over 50 years and may serve as a standard of comparison for similar bi-layer designed crowns. Reitmeier and coworkers evaluated the clinical performance of metal-ceramic (PFM) crowns placed in 10 different private practices;5 95 patients received 190 PFM crowns. The 7-year survival rate was 95.5%. There were 14 reported events (7%) of chipping or cracking of the porcelain veneer that did not require replacement of the crown. One crown was replaced due to fracture. Another article on the clinical performance of 688 single-unit metal-ceramic crowns placed in a prosthodontic practice between January 1984 and December 1992 reported the repair rate and failure rate of PFM crowns after 5 to 10 years in clinical service were both 3%.6
All-Ceramic Crowns
A number of ceramic materials have been introduced to replace the metal in a bi-layer crown design. And several systematic reviews of these all-ceramic materials have been published. Conrad and coworkers reported a systematic review of ceramic materials in peer-reviewed articles between 1996 and 2006.7 They included glass-ceramic, reinforced glass-ceramic, and alumina-based ceramic crowns in the review. The most common complication that required remake of a crown was fracture of the veneering porcelain and/or the ceramic coping. The most common major complication was fracture of the veneering porcelain and/or core fracture with complete fracture of the crown. The most common minor complication was surface chipping or cracking. They reported typical survival rates of 90% to 97% for all three categories of all-ceramic crowns after 5 to 10 years of service.
A separate review of the literature on all-ceramic restorations was completed between the years of 1993 and 2008.8 The authors indicated that most clinical trials for all-ceramic crowns have a reported survival rate of greater than 90% regardless of the time in service. A range of survival rates were reported for studies lasting at least 4 years: IPS Empress® (Ivoclar Vivadent; https://www.ivoclarvivdent.us), 92% to 95%; In-Ceram® (VITA, https://www.vita-vip.com), 92% to 99%; Procera™ (Nobel Biocare, https://www.nobelbiocare.com), 93% to 97%, and IPS Empress® 2, 95% to 100%. The main cause of failure reported for all studies was catastrophic fractures resulting in crown fracture and chipping of the veneer porcelain.
Another systematic review of the literature reported the survival rates of all-ceramic and metal-ceramic crowns from 1966 to 2006.9 A meta-analysis for the 5-year survival of all-ceramic crowns was estimated as 93.3% and metal-ceramic crowns were estimated at 95.6%. Reporting the results by material type, densely sintered alumina (Procera) had a 96.4% survival at 5 years; reinforced glass-ceramic crowns (IPS Empress) was 95.4%; and glass-infiltrated alumina (In-Ceram) crowns was 94.5%. Glass-ceramic crowns had a 5-year survival of 87.5%. There was no significant difference between the PFM crowns and the all-ceramic crowns with the exception of the glass-ceramic crowns. They also reported 5-year chipping rates of 3.7% for all-ceramic crowns and 5.7% for metal-ceramic crowns with the most common technical failure of all-ceramic crowns being fracture of the ceramic core. Of interest was that the authors reported that they were unable to identify any published randomized, controlled clinical trials comparing all-ceramic crowns with conventional metal-ceramic crowns in their search of the literature.
Zirconia Crown Studies
Zirconia is one of the more recent ceramic core materials to be considered for bi-layer crown designs and there is a lack of 5- to 10-year studies for comparison. Raigrodski and coworkers reported on a clinical study of anterior zirconia (Lava™, 3M ESPE, https://www.3mespe.com) crowns.10 The crown copings were custom designed with the Lava WaxKnife software to ensure sufficient support for the veneering porcelain. Twenty Lava zirconia crowns were placed in 18 subjects and recalled over 2 years. No fractures or chipping was reported. All restorations were rated successful at 2 years. One randomized, controlled clinical trial compared slip-cast glass-infiltrated alumina/zirconia and CAD/CAM zirconia all-ceramic crowns.11 By random assignment, 15 In-Ceram zirconia (slip-cast, infiltrated) crowns and 15 Cercon® Zirconia (DENTSPLY Ceramco, https://www.ceramco.com) (CAD/CAM) crowns were fabricated and cemented with a glass-ionomer cement in 20 patients. Patients were recalled yearly for 2 years. One crown from each group fractured and required replacement. Another study evaluated 78 posterior and anterior CAD/CAM zirconia (Cercon) ceramic crowns and 23 fixed partial dentures in 55 patients.12 Restorations were evaluated over 4 years. One crown failed at 12 months due to bulk fracture of the veneering porcelain. At 24 months, two crowns fractured the porcelain off the zirconia substructure. At 48 months, two crowns exhibited porcelain fractures. All of the fixed partial denture abutment crowns were clinically acceptable at 48 months.
Ortorp and coworkers reported the 3-year outcome of zirconia (Nobel Procera) single crowns placed in a private practice between October 2004 and November 2005.13 This was a retrospective evaluation of patient records. A total of 161 patients received 204 zirconia crowns. A sample group of 18 patients, with 25 crowns, was clinically examined at the 3-year recall. Most crowns (78%) were placed on premolars and molars. No zirconia core fractured and no caries was observed. There were 12 (6%) reported failures in 10 patients: abutment tooth was extracted (5/2.5%), remake of crown due to lost retention (4/2%), veneer fracture (2/1%) and persistent pain (1/0.5%). The cumulative survival rate was 92.7% at 3 years.
A longitudinal clinical trial evaluated the clinical performance of a zirconia material for CAD/CAM-generated restorations.14 Each ceramic restoration consisted of a CAD/CAM-generated, zirconia framework (e.Max® ZirCAD, Ivoclar Vivadent) veneered with a press-fit veneering porcelain (e.Max® ZirPress, Ivoclar Vivadent). One clinician placed 31 crowns and 10 fixed partial dentures in 33 patients. All restorations were cemented with a self-etching bonding agent and resin cement (MultiLink® Automix; Ivoclar Vivadent). The percentage of alpha scores for color match, margin discoloration, margin adaptation, and caries were 100% for both types of restorations over the 2 years. One crown failed due to veneering porcelain fracture at 16 months and another crown had veneering porcelain fracture at 24 months. Both crowns required replacement due to the degree of veneering porcelain fracture.
Conclusion
The published studies on zirconia crowns do not allow for 5- to 10-year comparisons because they are only 2 to 4 years in length. However, some trends can be identified. Other all-ceramic materials used for bi-layer crown designs have consistent reports that the major complication leading to crown replacement is fracture of the substructure. None of the reviewed studies on zirconia crowns have reported fracture of the substructure as a complication. All bi-layer crowns, both with metal or ceramic substructures, have been found to suffer from surface chipping and fracture of the veneering porcelain. As reported in the studies reviewed, this is generally in the 3% to 6% range for both metal-based substructures and ceramic-based sub-structures, and zirconia crowns seem to fall within this same range. So, in spite of the enhanced strength of the zirconia substructure, the veneering porcelain still seems to be at risk of chipping or fracture. But it does not seem to be of any greater rate than PFM or other all-ceramic crowns.
Disclosure
Dr. Fasbinder has received grant/research support from 3M ESPE and Ivoclar Vivadent, and has lectured at educational courses supported by 3M ESPE, Ivoclar Vivadent, and Sirona Dental Systems.
References
1. Cavalcanti AN, Foxton RM, Watson TF, et al. Y-TZP ceramics: key concepts for clinical application. Oper Dent. 2009;34(3):344-351.
2. Manicone PF, Iommetti PR, Raffaelli L. An overview of zirconia ceramics: basic properties and clinical applications. J Dent. 2007;35:819-826.
3. Yilmaz H, Aydin C, Gul BE. Flexural strength and fracture toughness of dental core ceramics. J Prosthet Dent. 2007;98:120-128.
4. Sundh A, Sjogren G. Fracture resistance of all-ceramic zirconia bridges with differing phase stabilizers and quality of sintering. Dent Mater. 2006;22:778-784.
5. Reitemeier B, Hänsel K, Kastner C, Walter MH. Metal-ceramic failure in noble metal crowns: 7-year results of a prospective clinical trial in private practices. Int J Prosthodont. 2006;19(4):397-399.
6. Walton TR. A 10-year longitudinal study of fixed prosthodontics: clinical characteristics and outcome of single-unit metal-ceramic crowns. Int J Prosthodont. 1999;12(6):519-526.
7. Conrad HJ, Seong WJ, Pesun IJ. Current ceramic materials and systems with clinical recommendations: a systematic review. J Prosthet Dent. 2007;98(5):389-404.
8. Della Bona A, Kelly JR. The clinical success of all-ceramic restorations. J Am Dent Assoc. 2008;139(Suppl):8S-13S.
9. Pjetursson BE, Sailer I, Zwalen M, Hammerle CHF. A systematic review of the survival and complication rates of all-ceramic and metal-ceramic reconstructions after an observation period of at least 3 years. Clin Oral Impl Res. 2007(Suppl 3);73-85.
10. Raigrodski AJ, Zhang H, Dogan S. Efficacy of zirconia-based anterior maxillary single crowns with customized copings. J Dent Res. 2009;88: Abstract 374.
11. Cehreli MC, Kökat AM, Akça K. CAD/CAM Zirconia vs. slip-cast glass-infiltrated Alumina/Zirconia all-ceramic crowns: 2-year results of a randomized controlled clinical trial. J Appl Oral Sci. 2009;17(1):49-55.
12. Barnes D, Gingelli JC, Rajaski J, et al. 48 Month Clinical Evaluation of Cercon Zirconia All Ceramic Restorations. J Dent Res. 2010; Abstract #449.
13. Ortorp A, Kihl ML, Carlsson GE. A 3-year retrospective and clinical follow-up study of zirconia single crowns performed in a private practice. J Dent. 2009;37(9):731-736.
14. Fasbinder DJ, Dennison JB, Neiva GF. Clinical evaluation of CAD/CAM zirconium crowns and fixed partial dentures. J Dent Res. 2008;Abstract 539.
About the Author
Dennis J. Fasbinder, DDS
Clinical Professor
Director, Advanced Education in General Dentistry
University of Michigan School of Dentistry
Ann Arbor, Michigan