Dimer Chemistry for Anterior and Posterior Restorations
Using a next-generation resin nano-hybrid composite with low-shrinkage, high-monomer conversion offers clinicians another option for universal use.
The general trend in general dental practices today is to place direct adhesive esthetic materials, especially composite resin, to restore anterior and posterior teeth. There are many excellent composites to choose from, most of which use the chemistry that was patented decades ago, such as bisphenol A and glycidyl methacrylate (Bis-GMA). In the past 10 years, there has been a reverse trend where some composites have been classified according to their specific usage—anterior or posterior—while other composites have been classified as being universal—both anterior and posterior. There have been criteria described for using this universal composite which include:
- multiple shades and translucencies to match the natural dentition
- wear similar to natural tooth structure
- no plastic deformation in function
- a simple technique for placement
- minimal shrinkage during polymerization
- high double-bond conversion of the monomer chemistry system
- excellent marginal adaptation and sealing
- radiopacity equal to or greater than enamel and dentin for ease of radiographic evaluation
- a quick, exact, non-tooth destructive finishing technique
- chemically compatible with all adhesive systems.1
Some of the deficiencies in clinical performance and postoperative patient complaints with adhesive composite resins relate to problems with resin shrinkage and gap formation at margins and at the dentin-composite interface during polymerization.2 This gap formation caused by resin polymerizaton shrinkage can contribute to loss of adhesion, bacterial invasion, recurrent caries, postoperative sensitivity, and pain on mastication.3
Polymerization shrinkage and the stresses associated with shrinkage have continued to present major challenges in the clinical performance of dental composites. During polymerization, the kinetics of resin-based composites, the initial double-bond concentration of the monomer, and the degree of conversion achieved during polymerization affect the final shrinkage results—gaps and stresses. These physical properties can have a direct effect on the longevity of composite resin restorations and can contribute to a lack of marginal sealing or microleakage problems.4-7 Also, the degree of polymerization based on the chemical reaction conversion of the double bonds of resin monomers within the composite have been questioned for their role in contributing to biocompatibility.8,9
Since 1962, the predominant chemistry of composite resins has been based on Bis-GMA. Reported problems related to Bis-GMA chemistries with composite resins include poor conversion of the dimethacrylate monomers into polymers, polymerization shrinkage, shrinkage stress and gap formation, water solubility, alcohol solubility with chemical softening of the resin, and composite wear.10,11 Recently, research has focused on substituting existing composite chemistries with improved resin-monomer systems. Researchers at the University of Colorado developed a unique monomer chemistry that significantly reduced polymerization shrinkage and increased the initial double-bond concentration of the monomer and the degree of conversion achieved during polymerization.7,12 They developed a novel diluent monomer based on dimer-acid chemistry when compared with conventional diluents and Bis-GMA resins. This technology was recently incorporated into a new low-shrink, high-monomer conversion composite resin, N’Durance™ (Septodont, www.septodontusa.com). The volumetric shrinkage of Bis-GMA nano-hybrid–based composites have a range of 1.85% to 3% while N’Durance has a reported polymerization shrinkage of 1.27%.13,14 Also, the use of optimized nano-fillers of ytterbium fluoride, barium glass, and silica make this composite easy to distinguish in radiographs and provide for wear resistance similar to existing nano-filled composites.13,14 With this significantly lower volumetric shrinkage and non-stick formulation, well-adapted composite resin restorations are more easily achievable.
Side benefits of this new chemistry include extremely low water sorption and solubility that contributes to color stability (no color shifting), marginal integrity, and stain resistance of the composite. This same dimer-acid, high-conversion chemistry is used for the N’Durance Dimer Flow flowable composite resin. A recent research study evaluated the N’Durance composite resin for anterior restorations 1 year after placement.15 The findings of this study demonstrated 100% alpha rankings for anatomic form, marginal adaptation, no marginal discoloration, no surface staining, and 100% retention of the restorations. The N’Durance composite produced good clinical results for anterior restorations at the 1-year evaluation with no postoperative sensitivity or gingival irritation.
Case Reports
N’Durance can be used for both anterior and posterior restorations. In all four cases demonstrated in this article, the restorations were placed with an etch-and-rinse (total-etch) adhesive technique. Several different phosphoric-acid etchants and fifth-generation adhesives were used. The finishing and polishing techniques used finishing burs, finishing disks, silicone polishers, and a polishing brush. N’Durance as a universal composite resin can be used with any adhesive, including total-etch fourth- and fifth-generation adhesives or with self-etch adhesives. The finishing and polishing can be accomplished with the burs, diamonds, and other abrasives of the clinician’s choice.
Case 1
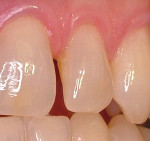
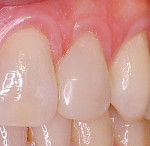
This patient had a chief complaint of a small maxillary lateral incisor with a prominent mesial space (Figure 1). Using a minimally invasive preparation design, the facial, mesial, and lingual surface of the lateral incisor was roughened with a medium-grit diamond using a high-speed handpiece. The tooth was etched, the adhesive was placed, and N’Durance composite resin was sculpted to place. The full-body, moderately heavy viscosity, non-sticky formulation allows for ease in placement. The completed restoration was highly esthetic (Figure 2).
Case 2
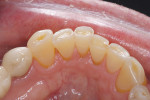
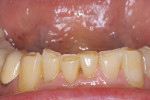
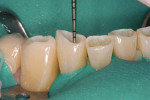
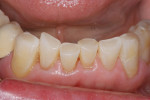
As patients are keeping their teeth longer, the clinical condition of attrition of the mandibular incisors has become more prevalent. For this patient, the wear through the enamel into the dentin was unsightly (Figure 3 and Figure 4). Using a minimally invasive technique that the author has had success with over the past 12 years, a 329 bur (1 mm in length) was used to prepare an intradentin preparation of the incisal edges to a depth of 1 mm, leaving an enamel shell intact (Figure 5).16 Usually these preparations can be accomplished without the need for local anesthesia. The depth of 1 mm assures durability of the restoration. Using an etch-and-rinse adhesive technique, the N’Durance composite resin was placed without changing the height of the mandibular anterior teeth (Figure 6).
Case 3
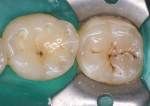
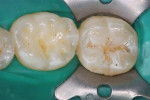
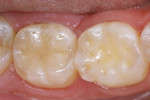
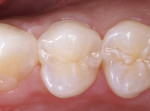
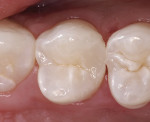
Occlusal caries provides the clinician with choices in preparation design. A conventional preparation of “extension for prevention” with an amalgam-like preparation design is no longer necessary. A minimally invasive preparation can be accomplished with smaller burs. For this patient, the occlusal surfaces of the mandibular first and second molars were diagnosed with caries using an LED caries-detection device (Midwest Caries I.D.™, Dentsply Professional, www.dentsply.com) (Figure 7). The second molar was prepared very minimally with a preventive resin-preparation design. The first molar had deeper caries in the area of the central fossa-lingual groove (Figure 8). Using an etch-and-rinse adhesive technique, the second molar was restored with a dimer chemistry flowable composite resin (N’Durance Dimer Flow) and the first molar was restored with more heavily filled N’Durance composite resin (Figure 9).
Case 4
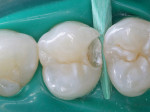
When the occlusal surface is free of caries (Figure 10), initial Class II caries can be removed with a minimally invasive slot-preparation design (Figure 11). To ensure an anatomic proximal contact, a wedge was placed before starting the preparation. This provides for rapid separation to compensate for thickness of the matrix band. For this case, a Triodent V3 Ring® matrix (Triodent, www.triodent.com) was used to restore the distal surface of the maxillary first premolar with an etch-and-rinse adhesive technique and the dimer chemistry nano-filled composite resin (Figure 12).
Conclusion
In another 3 years it will be the 50th anniversary of Bowen’s patent on composite resin using Bis-GMA resin with other monomer diluents with a silane-treated glass filler particle. Composite resins have improved over the past four decades with the improvements in size and type of glass fillers. Most composites today are still using the same chemistry, with problems of poor conversion of the double-bond dimethacrylate monomers into polymers, polymerization shrinkage, shrinkage stresses, water solubility, and solubility to alcohol. Recently, a unique monomer chemistry that significantly reduces polymerization shrinkage and increases the initial double-bond concentration of the monomer and the degree of conversion achieved during polymerization was commercialized as a new low-shrink, high-monomer conversion composite resin, N’Durance. Unlike some other new composite chemistries that limit their use to specific bonding systems, N’Durance can be used successfully with all existing etch-and-rinse and self-etch adhesives. These nano-dimer composite and dimer flow composites appear to be very promising.
References
1. Strassler HE, Goodman HS. Restoring posterior teeth using an innovative self-priming etchant/adhesive system with a low-shrink hybrid composite resin. Restorative Quarterly. 2002;5(2):3-8.
2. Uno S, Shimokobe H. Contraction stress and marginal adaptation of composite restorations in the dentinal cavity. Dent Mater J. 1994;13:19-24.
3. Terry DA. Mastering the technique of direct posterior composite resins. Contemporary Esthetics and Restorative Practice. 2001;5(6):14-26.
4.Ferracane JL. Using posterior composites appropriately. J Am Dent Assoc. 1992;123:53-58.
5.Peutzfeldt A. Resin composites in dentistry: the monomer systems. European J Oral Science. 1997;105:97-116.
6.Gerdolle DA, Mortier E, Droz D. Microleakage and polymerization shrinkage of various polymer materials. J Dent Child. 2008;75:125-133.
7.Ge J, Lemon MT, Lu H, Stansbury JW. Dimer acid-derived dimethacrylates as diluents monomers in restorative resins. J Dent Res. 2005;84(Special Issue A): Abstract 1470.
8.Goldberg M. In vitro and in vivo studies on the toxicity of dental resin components: a review. Clin Oral Investig. 2008;12:1-8.
9.Polydorou O, König A, Hellwig E, Kümmerer K. Long-term release of monomers from modern dental-composite materials. Eur J Oral Sci. 2009;117:68-75.
10.McKinney JE, Wu W. Chemical softening and wear of dental composites. J Dent Res. 1985;64:1326-1331.
11.Yap AU, Chew CL, Ong LF, Teoh SH. Environmental damage and occlusal contact area wear of composite restoratives. J Oral Rehabil. 2002;29(1):87-97.
12.Lu H, Newman SM, Bowman CN, Stansbury JW. Dimer acid derived dimethacrylate for ternary dental restorative resins. J Dent Res. 2006; 85(Special Issue A): Abstract 32.
13.Bracho-Troconis C, Rudolph S, Boulden J, Wong N, et al. Characterization of a new dimer acid based resin nano-hybrid composite. J Dent Res. 2008; 87(Special Issue A): Abstract 81.
14.Bracho-Troconis C, Rudolph S, Garnhart A, Boulden J. New low-shrinkage dimer acid based microhybrid composite physical properties. J Dent Res. 2007;86(Special Issue A): Abstract 1290.
15.Ritter H, Lee SS. Clinical evaluation of N’Durance nano-dimer conversion technology dental composite. J Dent Res. 2009;89(Special Issue): Abstract 1006.
16.Strassler HE, Serio CL. Conservative treatment of the worn dentition with adhesive composite resin. Dent Today. 2004;23(8):79-83.
About the Authors
Howard E. Strassler, DMD
Professor
Division of Operative Dentistry Department of Endodontics, Prosthodontics and Operative Dentistry
Dental School
University of Maryland
Baltimore, Maryland
Kristen Harvey, BS
Dental Student
Dental School
University of Maryland
Baltimore, Maryland
Erin Ladwig, BS
Dental Student
Dental School
University of Maryland
Baltimore, Maryland