Invisible Direct Restorations Using the Latest Composite Resin Technology
Christopher Pescatore, DMD
The growing public awareness and demand for more attractive tooth restorations is challenging modern dentists to acquire and improve their skills to meet their patients’ expectations. Advances in composite resin technology for direct esthetic restorations have enabled clinicians to re-create natural tooth esthetics and proper morphology. Many practitioners have embraced the practice of direct esthetic restorations because it allows them to explore their creative and artistic skills while building functional, lifelike restorations.
A significant advantage of direct adhesive composite systems is that they allow the clinician to preserve sound tooth structure during the decay-removal and preparation processes as compared to traditional direct posterior restorations, which consisted of either gold foil or silver amalgam.1 Because it is not necessary to create mechanical retention or reduce additional sound tooth structure to provide for the bulk of the material, the composite restoration preparation is quite conservative.2 The preparation generally consists of the removal of the carious lesion and/or defective restoration, the establishment of a proper cavity form consistent with enamel rod orientation, and placement of the restorative material. Another advantage of the composite resin restoration is the re-strengthening of unsupported or weakened tooth structure.3 A study has shown the longevity of the direct resin restoration to be equal or superior to the traditional amalgam restoration.4 Even using historical resins and techniques, composite restorations have been shown to be comparable in many situations to amalgam restorations.5
Currently, numerous composite restorative systems are available. A recently introduced system, Herculite® Ultra (Kerr Corporation, Orange, CA), employs the latest in nanoparticle technology. Herculite Ultra is a universal composite that features optimal handling and high polishability, lifelike esthetics, great wear resistance, and increased radiopacity. The resin matrix and Vita® shade matching, inherent with Herculite XRV™, have been retained in Herculite Ultra. A proprietary Point® 4 (Kerr Corporation) filler system allows chameleon-like restorations to be artfully achieved from a single shade. This capability enables the clinician to simplify shade selection by being able to use fewer shades to create the desired esthetic result.
Case Discussion
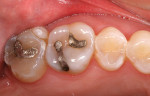
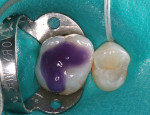
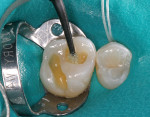
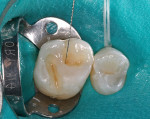
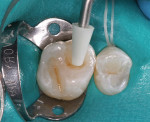
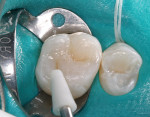
A patient presented with a preoperative scenario of failing existing amalgam restorations on their upper right first and second molars (Figure 1). After rubber dam isolation and the removal of the carious lesions, tooth preparation was completed (Figure 2). The preparation was cleaned to remove the smear layer with a 2% chlorhexidine solution and rinsed. The tooth was then etched with a two-step phosphoric-acid (37%) technique of etching the enamel first for 5 seconds and then filling the preparation (dentin) for 10 seconds (Figure 3). This enables the enamel to be etched for a total of 15 seconds. The preparation is then completely rinsed with generous amounts of water and the excess is then removed, being careful not to desiccate the dentin, but rather leave it moist. An antimicrobial desensitizer agent (Gluma Desensitizer, Heraeus Kulzer, South Bend, IN) is then applied to the preparation and the excess is removed with a combination of an absorbent brush and a contamination-free air dryer. This reestablishes the moist, matte finish. A single component adhesive (OptiBond® Solo Plus™, Kerr Corporation) was then applied and moved around the preparation to ensure the necessary agitation for maximizing penetration (Figure 4). The solvent, ethanol, was evaporated from the tooth surface for 3 to 5 seconds by again using a contamination-free air dryer. The adhesive bonding agent was polymerized with a LED light source (Demi LED Light Curing System, Kerr Demetron) for 10 seconds. Normally, a flowable composite resin would be added next because of its stress-absorbing potential during the polymerization process.6 But, because the preparations were not deemed deep enough by the clinician, this first flowable layer was not used. The first layer of Herculite Ultra was shade A1. This layer was sculpted easily up to the dentin-enamel junction to facilitate the underlying anatomy with a rolling instrument (CompoRoller™, Kerr Corporation), thus creating areas for later staining (Figure 5). It was cured for 20 seconds.
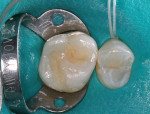
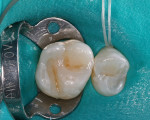
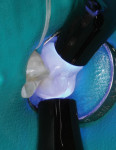
Tints were applied next to resemble the slight pit-and-fissure staining seen in the neighboring natural dentition. A brown tint was applied with a #06 endo file and cured (Figure 6). The last layer, the enamel substitute shade Light Incisal, was applied incrementally and smoothed before curing (Figure 7, Figure 8 and Figure 9). After the final increment was placed, the restoration was cured simultaneously on the buccal and lingual with LED curing light devices (Figure 10).
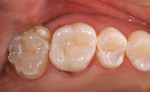
After rubber dam removal and any occlusal adjustments, the restoration was then finished and polished with a small football-shaped carbide finishing bur and assorted rubber points and cups. The final result exhibits not only natural esthetics, anatomic form, and function, but is also consistent with the surrounding dentition (Figure 11).
Conclusion
Today’s patients are concerned not only with maintaining and restoring the function of their teeth, but also with esthetic enhancements and beauty. Therefore, it behooves the dental professional to provide conservative options that will preserve as much sound tooth structure as possible, allowing them to display their artistic skill and ingenuity while reestablishing the dental architecture. Dental manufacturers have been able to develop products that are not only stronger and more wear resistant, but also more pleasing to the eye. These factors enable the clinician to create invisible restorations that may actually improve on nature as well as satisfy the public’s increased demand for esthetic restorations.
References
1. Leinfelder KF. A conservative approach to placing posterior composite resin restorations. J Am Dent Assoc. 1996;127(6):743-748.
2. Albers HF. Tooth Colored Restorations. 8th ed. Santa Rosa, CA, Alta Books: 1997:27-35.
3. Dietschi D, Spreafico R. Adhesive Metal-Free Restorations: Current Concepts for the Esthetic Treatment of Posterior Teeth. Carol Stream, IL, Quintessence: 1997:215.
4. Collins C, Bryant R, Hodge KL. A clinical evaluation of posterior composite resin restorations: 8 year findings. J Dent. 1998; 26(4):311-317.
5. Mair L. Ten-year clinical assessment of three posterior resin composites and two amalgams. Quintessence Int. 1998;29(8): 483-490.
6. Baratieri LN, Felippe LA, Perdigao J, et al. Direct posterior composite resin restorations: current concepts for the technique. Pract Periodontics Aesthet Dent. 1998; 10(7):875-886.
About the Author
Christopher Pescatore, DMD
Private Practice
Danville, California