Immediate Replacement and Temporization of a Single Tooth: An Expedited Treatment Protocol
Russell A. Baer, DDS; Martin J. Marcus, DDS
Dental implants are currently well accepted as a safe and effective means for tooth replacement.1 One common application of implant rehabilitation is the replacement of a missing tooth or a failing single tooth. Despite the excellent treatment outcomes typically obtained, patients can be resistant to the extended time of conventional implant treatment. Dental implant treatment typically involves long healing periods between various treatment steps. This has historically presented a potential barrier to treatment for our patients. New protocols using placement at the time of extraction with immediate function and temporization have eliminated this obstacle to treatment and have increased patient acceptance.
Immediate function was first shown to be an acceptable treatment in the completely edentulous mandible2 and then in other areas of the mouth. Wohrle3 conducted one of the first multi-center studies to report the feasibility of immediate function in the single-tooth implant, and many authors have since demonstrated this.4 What can be concluded from these studies is that immediate function is very effective when:
- Occlusal loads are controlled.5
- An osseoconductive implant surface is used (eg, TiUnite® Nobel Biocare, Yorba Linda, CA).6
- Initial placement stability of the implant is at/or greater than 35 Ncm.7
Initial stability of the implant at the time of placement is determined by the ability of the practitioner to engage existing bone and by the design of the implant to be stabilized in this bone. Many practitioners have shown that the use of tapered implants allows for better initial stability in the bone.8 This stability can be increased by changing the shape of the osteotmy relative to the implant geometry.
Implant placement at the time of extraction not only shortens the time of treatment but also prevents collapse of the alveolar bony complex that has been reported to be up to 60% volume of the socket and 3 mm to 4 mm of bone loss in both the buccal-lingual and apico-gingival directions.9 By placing the implant and associated grafting material, the initial collapse can be prevented and, thus, the crestal bone architecture can be maintained at pre-extraction levels.
Case Report
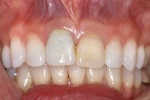
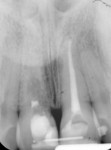
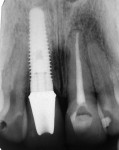
A 30-year-old woman presented to the authors’ clinic with a chief complaint of internal resorption in a maxillary central incisor secondary to previous trauma and discoloration of the adjacent tooth (Figure 1 and Figure 2). One of the patient’s concerns was the transition from tooth to final restoration and not having to wear a removable temporary appliance. A treatment plan was developed to extract the hopeless tooth and immediately place a dental implant with immediate temporization.
On the day of the procedure, the patient was anesthetized and an atraumatic extraction was performed using periotomes and forceps to elevate the tooth without damaging the surrounding bone. After thorough curettage of the socket to verify the presence of bone and removal of any soft tissue remnants, a 2-mm pilot drill was used to redirect the axis of the implant into the mid alveolus. An x-ray was taken to verify direction. The site was then enlarged to a 5-mm diameter using the NobelReplace™ Tapered (Nobel Biocare) drilling protocol. Placement was such that the implant neck was at least 0.5 mm palatal from the crestal bone and even with the labial crestal margin apical-coronally. Initial stability was verified with a manual torque wrench to verify 35 Ncm of resistance and an Immediate Temporary Abutment (Nobel Biocare) was placed. A full contoured temporary restoration was fabricated. Care was taken to eliminate all centric and excursive contacts and a combination of the patient’s own bone, collected during the osteotomy preparation, and bovine hydroxyapatite was used to occlude any excess space around the neck of the implant. The temporary restoration was cemented with TempBond™ (Kerr Corporation, Orange, CA) temporary cement and the patient was instructed not to eat directly on this area for at least 8 weeks. Postoperative medications included appropriate analgesics and oral antibiotics (500 mg penicillin VK four times per day [qid] for 1 week or 150 mg clindamycin qid for 1 week). The patient was also instructed to apply chlorhexidine rinse topically to the area throughout the healing period.
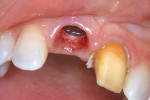
After 12 weeks of healing time, the temporary crown was removed and a stable implant biologic width was noted. The adjacent tooth was prepared for a NobelProcera™ Alumina (Nobel Biocare) veneer (Figure 3). An implant-level impression was taken capturing both the implant position and the veneer preparation. The impression was then sent to the laboratory for fabrication of a custom zirconium abutment, a corresponding NobelProcera Zirconia crown, and the adjacent NobelProcera Alumina veneer.
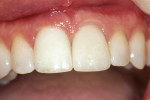
At the time of delivery, the temporary restorations were removed and the final abutment was placed on the implant. A radiograph was taken to verify proper seating of the custom abutment and the NobelProcera Zirconia crown was checked for contacts and occlusion. After adjustments, the abutment was torqued to 35 Ncm and the final crown was cemented with Improv (Alvelogro, Snoqualmie, WA) provisional cement. The NobelProcera Alumina veneer was bonded to the tooth using Calibra® (DENTSPLY, York, PA) bonding cement (Figure 4 and Figure 5).
Practitioners are often faced with the dilemma of restoring patients as quickly as possible. However, it often takes time to provide optimal treatment. Implant treatment, although the treatment of choice for single-tooth replacement, is not always the quickest. By incorporating new techniques and materials, we as practitioners are able to treat our patients with the most optimal treatment without making sacrifices due to the length of time it has previously taken to accomplish this treatment. A conventional 3-unit bridge would allow for a more stable temporary phase compared to the time it takes for conventional implant treatment as described by Brånemark.10 By using immediate placement and immediate function we can bring our patients through treatment in a stable, natural manner while better supporting the biological complex. The final restoration can take advantage of newer biologically compatible materials and provide a longer-lasting, more esthetic end result.
References
1. Misch CE. Contemporary Implant Dentistry. 2nd ed. CV Mosby; St. Louis, MO. 1999:3-12.
2. Schnitman PA, Wöhrle PS, Rubenstein JE. Immediate fixed interim prostheses supported by 2-stage threaded implants. Methodology and results. J Oral Implantol. 1990; 16:96-105.
3. Wöhrle P. Single tooth replacement in the aesthetic zone with immediate provisionalization: Fourteen consecutive case reports. Pract Periodontics Aesthet Dent. 1998;9: 1107-1111.
4. Kan J, Rungcharassaeng K. Interimplant papilla preservation in the esthetic zone: A report of six consecutive cases. Int J Periodontics Restorative Dent. 2003;23: 249-259.
5. Gapski R, Wang HL, Mascarenhas P, Lang NP. Clinical review of immediate implant loading. Clin Oral Impl Res. 2003;14(5): 515-527.
6. Rocci A, Martignoni M, Gottlow J. Immediate loading of Brånemark System TiUnite and machined-surface implants in the posterior mandible: A randomized open- ended clinical trial. Clin Impl Dent Relat Res. 2003;5(suppl 1):57-63.
7. Östman P-O. On various protocols for direct loading of implant-supported fixed prosthesis. Thesis. Göteborg University. 2007;74.
8. Rao W, Benzi R. First single lower molar implants with flapless guided surgery and immediate function: clinical and radiographic preliminary results of a prospective study. J Prosthetic Dent. 2007;97(suppl 1):S3-S14.
9. Ashman A, Bruins P. Prevention of alveolar bone loss post extraction with HTR grafting material. Oral Surg Oral Med Oral Pathol. 1985;60(2): 146-153.
10. Brånemark PI, Zarb GA, Albrektsson T. Tissue Integrated Prosthesis. Osseointegration in Clinical Dentistry. Quintessence Publishing Co. Hanover Park, IL; 1987: 202, 214-228.
About the Authors
Russell A. Baer, DDS
University Associates in Dentistry
University of Chicago
Chicago Illinois
Martin J. Marcus, DDS
University Associates in Dentistry
University of Chicago
Chicago, Illinois