Successful Proximal Management of the Minimal Class 2 Direct Composite Restoration
Randall G. Cohen, DDS; Michael V. Razzano, DDS
Dentistry has made great progress since GV Black described his “extension for prevention” principle of cavity preparation. The capability to restore proximal decay conservatively, without extension onto a caries-free occlusal surface to resist dislodging forces, is one great advantage of bonded composite materials in restorative dentistry.1 Similarly, composites do not require the undercuts for retention that are needed with amalgam restorations, thus reducing much of the stresses in tooth structure that accompany amalgam preparations.2 Accordingly, a preparation design that widens toward the occlusal surface is routinely performed in adhesive dental procedures. This preparation design greatly facilitates the placement of the restorative composite into tight areas, effectively reducing voids at the margins of the final restoration.3
There are many challenges, however, when creating a proper class II composite restoration, such as the potential to create an open proximal contact, a poor anatomic contour, and an inadequate marginal seal.4 Amalgam restorations have been performed clinically for many decades, and clinicians have used Tofflemyre matrices successfully to create the proximal contour. Although Tofflemyre matrices are efficient when used with amalgam, their use with composite resins often results in a poor contour and an open contact, partly because of the low resistance to deformation that is inherent within the material.5 Accordingly, clinicians, at times, have re-prepared these proximal surfaces and added more composite in an attempt to close the contact, resulting in a potentially destructive retentive area. Using a combination of highly filled flowable and packable composites, placed using a sectional matrix system, clinicians can create a direct composite restoration predictably, with the appropriate proximal contour and contact. For these restorations, clinicians should choose a composite material that will exhibit minimal polymerization shrinkage and work effectively on cut enamel as well as in the proximal boxes of deep restorations.6
Conservative Preparation
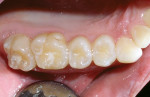
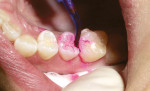
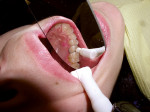
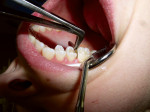
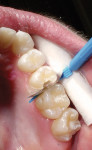
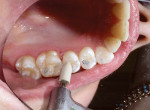
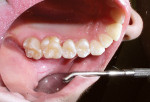
Often, clinicians must rely on a radiograph to detect minimal proximal lesions because they are often undetectable on clinical examination or visual inspection (Figure 1). After diagnosis, the proximal decay was approached occlusally using a No. 330 bur on the high-speed handpiece to create access. Then, a divergent proximal box was created using a flat-ended diamond, similar to that of a standard inlay preparation. Unless a preexisting restoration or occlusal caries is present, the preparation should be confined solely to the proximal third of the occlusal surface, without creating the isthmus that classic gold7 and amalgam restorations require. Caries removal was verified using a caries indicator solution (Caries Detector, Kuraray America, Inc, New York, NY) (Figure 2), and the remaining decay was removed with a No. 4 round bur under irrigation, followed by a No. 2 round bur, very slowly and without irrigation to improve visibility. The restoration did not require “extension for prevention” through the proximal contact. However, a tight contact creates difficulty in the placement of the sectional matrix, so the author finished the preparation by passing a ribbon saw through the contact. Finally, the preparation was cleaned using a slurry of coarse, fluoride-free pumice (Figure 3), and then rinsed.
Placement of Sectional Matrix Assembly
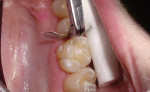
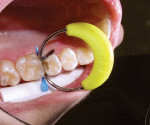
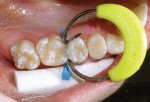
The cleaned preparation was isolated using parotid pads with cotton rolls. The sectional matrix system kit (Composi-Tight® Silver Plus, Garrison Dental Solutions, Spring Lake, MI) contained six different sizes of sectional matrices. The author chose the appropriate one by checking that it extended from beyond the gingival margin to the marginal ridge of the adjacent tooth. The included ring-placement forceps were used to grasp the sectional matrix (Figure 4) and hold it in position while the plastic wedge that is part of the system was inserted (Figure 5). The author chose the largest wedge that passed through the contact so that maximum tooth separation was attained (Figure 6).
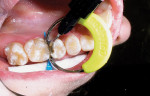
The ring mechanism was the last piece of the assembly placed. It was delivered to the preparation in a similar manner as a rubber dam clamp, using the specialized forceps to open the ring and seat it into position. In this way, the teeth were separated and the sectional matrix was wedged from the gingival and held firmly against the facial and lingual surfaces of the tooth by the ring (Figure 7). Lastly, the sectional matrix was burnished firmly, using one extension of a multifunctional instrument (TN009, Garrison Dental Solutions) against the adjacent tooth.
Placement of Restorative Materials
Next, the author applied the bonding adhesive, a sixth-generation, antibacterial, self-etching adhesive (Clearfil® Protect Bond, Kuraray America, Inc). The primer was applied for 20 seconds, then air-dried. Then, the fluoride-containing microfilled resin was applied, lightly air-dried, and then light-cured for 20 seconds. Next, a thin liner, consisting of a highly filled (81% by wt) flowable composite (Clearfil Majesty™ Flow, Kuraray America, Inc), was placed with a syringe to the base of the proximal box, and spread in a uniform, thin layer over all cut dentin using a small ball burnisher, then light-cured (Figure 8).
After the liner of flowable composite was polymerized, the needle tip was inserted into the preparation and a second layer was deposited without light-curing, followed immediately by placement of the restorative composite (Clearfil Majesty™ Esthetic, Kuraray America, Inc). The heavier-bodied material displaced most of the flowable composite, causing the second layer of flowable composite to extrude over the margins. The excess flowable and esthetic composite were removed and the composite contoured (Figure 9). To establish appropriate occlusal anatomy, the two angled carvers on the multifunctional instrument were used. If this had been a larger restoration, the esthetic composite would have been added incrementally to minimize polymerization shrinkage and maintain better control of the case.8
Removal of the Sectional Matrix Assembly
The Composi-Tight assembly was removed in the reverse order in which it was placed. First, the ring was removed using the forceps. Then the wedge was grasped with a mosquito hemostat and removed. Removal of the sectional matrix can be difficult because of the strong bond that is created by the bonding resins, but grasping it with a mosquito hemostat and pushing it gingivally, then occlusally, is an effective method. The author does not recommend using a separating agent on the internal surface of the band because some contamination of the restoration can occur.
Finishing and Polishing of the Restoration
The close adaptation of the matrix minimized the excess composite, so contouring and polishing was simple and took minimal chair time. The facial and lingual contours were finished with burs (Brasseler USA) and sandpaper disks (Sof-Lex™, 3M ESPE, St. Paul, MN). The occlusion was checked, and the prematurities adjusted using a shoulder-former diamond to maintain proper occlusal inclines. The proximal contact was then checked with floss to make certain that the tightness of the restoration was appropriate. The author then used a scaler to instrument the tooth and remove the resin or composite flash. After rechecking the occlusion, a white rubber point (Dedeco, Long Island, NY) was sharpened against an abrasive wheel (Mizzy Heatless Wheel, Keystone Industries, Cherry Hill, NJ) and used on the low-speed handpiece (Figure 10) under irrigation to finish off the small scratches on the occlusal surface. The final smooth, glossy surface was obtained using a slurry of coarse pumice, followed by a slurry of polishing compound on a prophy cup (Figure 11).
Discussion
While composites enable clinicians to preserve tooth structure in a way that was not possible with amalgam restorations, they require special attention to ensure the excellent proximal contours and contacts that are necessary for comfortable function of the restoration. The use of highly filled flowable and packable composite materials, in combination with a sectional matrix system, enables dentists to create appropriately tight proximal contacts and a composite restoration that restores the tooth to its original function and appearance.
Disclosure
Dr. Cohen has received honoraria from Kuraray America, Inc.
References
1. Burke FJ. From extension for prevention to prevention of extension: (minimal intervention dentistry). Dent Update. 2003;30:492-502.
2. Atlas AM. The direct class 2 posterior composite: restoration of the initial carious lesion using the controlled placement and delayed polymerization technique. Contemporary Esthetics and Restorative Practice. 2006;10(5):46-49.
3. Fonesca RB, Correr-Sobrinho SB, Fernandes-Neto AJ, et al. The influence of the cavity preparation design on marginal accuracy of laboratory-processed resin composite restorations. Clin Oral Invest. 2007;12(1):53-59.
4. Shuman I. Excellence in class II direct restorations. Dent Today. 2007;26(4):102-105.
5. Strydom C. Handling protocol of posterior composites—part 3: matrix systems. SADJ. 2006;61:18-21.
6. Tjan AH, Bergh BGH, Lidner C. Effect of various incremental techniques on marginal adaptation of class II composite resin restorations. J Prosthet Dent. 1992;67(1):62-66.
7. Tucker RV. Class 2 inlay cavity procedures. Oper Dent. 1982;7(2):50-54.
8. Idriss S, Habib C, Abduljabbar T, et al. Marginal adaptation of class II resin composite restorations using incremental and bulk placement techniques: an ESEM study. J Oral Rehabil. 2003;30(10): 1000-1007.
About the Authors
Randall G. Cohen, DDS
Private Practice
Newtown, Pennsylvania
Michael V. Razzano, DDS
Private Practice
Woodstock, Georgia