Cast Gold: The Standard of Care for Operative Dentistry
Bruce W. Small, DMD, MAGD
The longevity of a properly diagnosed, prepared, constructed, seated, and finished cast gold restoration has always exceeded that of all other tooth-colored materials (ie, direct or indirect, composite or ceramic).1-3 Still the standard of care for operative dentistry, cast gold has been used for thousands of years to adorn and restore teeth. As early as 2500 B.C., the Mayas were accomplished smelters and forgers of gold and silver, and—to a lesser extent—bronze.4 Small inlays of jade and turquoise were placed on the facial surfaces of teeth after small preparations were made, first with jade then later with copper tubes similar to a drinking straw. The Romans became skilled in restoring carious teeth using gold crowns and in replacing missing teeth with fixed bridgework.4 Throughout the Middle Ages, many physicians (eg, Guy De Chauliac and Pietro d’Ardelata) filled teeth with gold and gold leaf. It was during the Middle Ages that the first references to a dentist—referred to as “dentatore”—were made.4
During the Renaissance, men such as Leonardo Da Vinci, Hieronymus Fabricius ab Aquapendente, and Eustachius added to the anatomical knowledge of teeth,4 and numerous advances were made in the understanding of the physiology of the oral cavity. Over the centuries, various restorative materials were used (eg, gutta-percha, low-fusing metal poured into cavities, silver and tin foil, and crude dental amalgam made from shavings of silver coins mixed with mercury4). Many American dentists in the early 1800s began using gold foil, which remains in use to this day.
In 1907, William H. Taggart perfected the use of his patented casting machine to make accurately fitting gold inlays.4 The process at that time consisted of carving wax directly in the mouth, which was then removed, invested in a special plaster, and burned out in an oven. Gold was melted using a blowpipe and then forced into the plaster mold using Taggart’s casting machine. This process, with many refinements, is still in use today.
Modern-day Teaching of Cast-gold Techniques
Most dental schools continue to teach cast-gold techniques, but only a small part of the existing body of knowledge is being transferred to dental students. This is partially a result of the requirements for licensure and state board examinations. Another reason is that in dental schools, many of the clinical instructors who know cast-gold techniques have retired or chosen not to teach. However, in a few schools in the United States, selective/elective courses in cast gold have become popular with some students. These classes, always filled to capacity, are taught at institutions devoted to the Tucker Technique (eg, University of Washington, UCLA School of Dentistry, University of Medicine and Dentistry of New Jersey, and University of Pennsylvania), which is described later. Helped in part by the fact that operative textbooks contain chapters on cast gold,5-7 complete texts8 are available, and a Web site9 is now online specifically about the Tucker Technique, the numbers of gold operators is increasing worldwide.
The Academy of Richard V. Tucker Study Clubs
One of the primary reasons more cast-gold restorations are being placed is a result of the formation of the Academy of Richard V. Tucker Study Clubs. This group includes 63 operating study clubs (ie, a group of eight to 12 dentists working on patients under the supervision of an experienced mentor) in the United States, Italy, Germany, Canada, and Peru, and the number of groups is increasing. All study club members observe each other’s preparations and completed restorations, as well as share in a critique session after the operations. Each year there is an annual session at which members from all of the clubs meet, operate, and socialize, providing an excellent method for learning the cast-gold technique. In addition, there is an annual, weeklong course mentored by Dr. Tucker and others at the University of Washington Dental School, which is open to all.
The Academy of Richard V. Tucker Study Clubs “is an organization designed to foster excellence in restorative dentistry through a relatively uncompromising format in postgraduate education. It is a unique approach to dental learning which features discipline and perfection in operating procedures that is inspired and shared by fellow study club members.”9
Dr. Tucker, the academy’s founder, is recognized as one of the finest gold operators in the world. Donovan et al10 published a clinical review of Dr. Tucker’s cast gold restorations. They evaluated 1,314 castings placed between 1 and 52 years. More than 20 years later, 72% of the restorations were still in service; the overall survival rate was 95.4% for all restorations evaluated.
The Tucker Technique
The only avenue for learning the Tucker Technique is joining or forming a study club to master the nuances of each case under the supervision of a Tucker mentor. There are some basic principles that must be followed to ensure long-term success. These will be briefly mentioned here and demonstrated with clinical examples.
The Tucker Technique is a systematic clinical discipline with very specific steps. Each step must be completed before beginning the next. The overall goal is a conservative preparation with a smooth and flowing outline form, precise and even taper of all walls, and very sharp margins. Attention should be placed on attaining adequate draw, flare, and depth, as well as sufficient resistance and retention form. If all the steps are accomplished properly, the technician will be able to construct an ideal casting that will be easily seated, cemented, and polished.
Basic Class II Preparation
Using the classic G.V. Black Class II preparation as an example, the individual steps necessary for success are described below.
Removal of Existing Restoration and Caries
Before the operation, the environment of the operating tooth should be evaluated (ie, attention should be given to the neighboring as well as opposing teeth). Any contact areas, occlusion, gingival condition, and fracture lines should be examined.
After anesthesia is administered, a rubber dam should be placed for isolation or retraction. Note: it is imperative that a dam be used not only for dryness, but also for visibility, access, and patient comfort. Four-handed dentistry can more easily be accomplished without pulling of cheeks and tongues.
Any existing restoration and caries are carefully removed with minimal or no removal of healthy tooth structure. A close inspection of the cavity is performed under magnification to identify potential internal cracks that may be present. If cracks are present, particularly extending onto the pulpal floor or proximal walls, a change in the preparation goal may be indicated.
Placement of Block-Out
The next step is to place a build-up or block-out material in the cavity. The purpose of the block-out typically is to allow the operator to create an ideal depth, draw, and flare of the preparation. It fills in any undercuts created by the removal of the existing restoration and caries, thus allowing the operator to limit the outline form. It is suggested that a large-particle paste/paste self-curing composite be employed for this purpose and that it not be bonded to the tooth structure. In most cases, the block-out will be removed before seating, and the bonding procedure would make this more difficult. In addition, the large-particle composite is much simpler to prepare and instrument than a light-cured composite. Composite has the ability to absorb fluid, particularly from a vital tooth, and should be replaced by a more inert material (eg, a zinc oxyphosphate cement) with less probability for dimensional change.
Outline Form
After complete polymerization of the block-out, the instrumentation of the cavity commences. Creating the outline form is the first step of this process. A No. 56 bur (Brasseler USA, Savannah, GA; and SS White Burs, Inc, Lakewood, NJ) is recommended for bicuspids and a No. 57 bur (Brasseler USA and SS White) is recommended for molars. Being careful not to overcut, the outline of the preparation is started. A minimal pulpal depth of 2 mm and a draw of 6° to 10° are optimal at this time. When breaking through the proximal walls, the flare should be kept conservative, especially on the mesiobuccal, if possible, because of esthetics. A minimal display of gold is recommended whenever possible.
Proximal Box
After completion of the outline form, the proximal box is prepared. When possible, the gingival floor is dropped 3 mm to 4 mm below the pulpal floor, and the proximal walls are flared to be parallel to the enamel rods and to sufficiently allow the bur to pass through the buccal and lingual aspects without hitting the adjacent tooth surface. The axial depth should be no more than 1.5 mm in a two-surface preparation. The gingival floor should be flat, perpendicular to the long axis of the tooth, and not run uphill or downhill. All attempts should be made to keep the proximal walls of the preparation with the same taper or draw as the occlusal. For optimal esthetics and resistance form, the proximal walls should be straight and not tip to the mesial or distal. The axial wall should be on the same plane as the opposing occlusal wall and have the same draw toward the middle of the preparation. All walls should be smooth and on the same plane without steps or any irregularities. This can be accomplished under magnification by using the handpiece carefully and lightly “painting” the walls with the bur to allow a smooth and precise preparation and easy withdrawal of the wax pattern.
Hand Instrumentation
The extent of the preparation has been defined by the use of the bur; it is now ready for refinement using hand instruments. Carbon-tipped instruments are recommended for this purpose because they maintain their sharpness longer than stainless steel instruments.
Using a 42S off-angle chisel (Tru-Bal, Suter Dental Manufacturing Co, Inc, Chico, CA), the pulpal and gingival floors are first flattened and smoothed. Any surface irregularities can be accomplished easily in two or three swipes. Next, the proximal line angles are instrumented using the 42S for the mesioproximal and the 43S (Tru-Bal) for the distoproximal. The proximal line angles are refined, as well as the entire surface of the proximal walls. Primary attention should be given to the cavosurface margin of the proximal walls; a one-plane straight wall should be the goal. There should be no reverse curve, similar to an amalgam preparation. Two or three swipes with a sharp instrument should suffice to smooth and plane these walls.
On two-surface inlay preparations in bicuspid teeth, an internal bevel or acuteness is often recommended to assist in intimately seating the casting. This is placed on the mesial using the Tucker 232 regular gingival margin trimmer (Suter Dental Mfg) and a Tucker 233 trimmer on the distal, both of which have a 30° angle. Note: when using these instruments, it is important to keep them parallel to the long axis of the tooth and not create a bowl-like effect; the acuteness should be flat and parallel to the gingival floor.
The axial wall then is smoothed, typically using the 42S on the distal wall and the 43S on the mesial wall. A slight ditch—usually created previously when instrumenting the proximal walls—should be removed during the smoothing of the axial wall. Finally, the external bevel is placed using the Tucker 232 on the distal and the Tucker 233 on the mesial bevel. Similar to the internal acuteness, this bevel should be straight and flat on one plane. This is the only true bevel on a Class II preparation, and the length should be between 0.5 mm to 0.75 mm.
Occlusal Bevel
Following hand instrumentation, a new 7901 or 7404 finishing bur (Brasseler USA and SS White) is used to lightly remove any unsupported enamel rods, creating a “microbevel.” The purpose of this step is to help create a smooth and flowing outline form while also removing any irregularities at the cavosurface margin. If the proximal walls are long and on more than one plane, they can be quickly brought to one plane with a sandpaper disk.
To refine the line angles of the preparation and simultaneously remove any debris present, a sharpened carbon steel explorer with a stream of air can be used to accentuate all of the line angles in the preparation. The preparation is complete at this point.
Impression
After ensuring a precisely detailed preparation, obtaining an equally precise and detailed impression is the next step. If retraction of the gingiva is indicated, the rubber dam septum(s) is cut with scissors and two cotton cords are carefully placed. The dam is removed after the appropriate amount of time, and the tooth is isolated with a cotton roll holder (if on the mandibular arch) or cotton rolls and a Dri-Angle® (Dental Health Products, Inc, Youngstown, NY) covering the parotid duct (if on the maxillary arch). The cord is removed slowly with an air stream and observed for absolute dryness. If no leakage or blood is present, the impression is taken using a high-walled metal check bite tray. Note: it is recommended to hold the patient’s mandible during the setting of the impression material to prevent any movement. The impression is checked for any pulls, tears, voids, or other inaccuracies, and then poured as soon as possible using a powder-to-liquid ratio appropriate for the material and environment. The casting should fit the tooth properly.
Seating and Cementation
Before trying in the casting, the patient should be anesthetized and a rubber dam placed. The casting is carefully tried in. If it is an occlusal or small slot restoration, it should not be completely seated because of possible difficulty in removal. Tucker-quality castings should not merely “drop in,” but should instead have an exquisite and intimate fit.
After the fit has been checked, the block-out generally should be removed and the zinc oxyphosphate cement mixed. Note: other cements may be used, but historically zinc phosphate has been time-tested and exhibits the major advantage of being able to adjust the working time by how it is mixed. Cement should be placed in the cavity and on the inside surface of the casting, after which it is placed in the tooth. The casting is then tapped into complete seating position using a leather foil mallet and wooden stick while pressure is continuously applied, driving the casting into the cavity. The casting is gently tapped until no more cement is expressed from the margins.
Finishing and Polishing
The final step after cementation is the finishing (ie, leveling the gold with the cavosurface margin of the tooth in three planes using disks) and polishing (ie, removing any scratches and using finer disks and powders to make it glow) of the casting. The three disks recommended are paper disks of medium garnet, fine sand, and fine cuttle grit on a slow-speed straight mandrel. Note: on occasion, it is more appropriate to use a short mandrel on a contra-angle on the lingual surface when the straight mandrel cannot gain proper access. Always rotate the disks from gold to tooth. The powders are applied using a soft rubber cup that is ribbed, not webbed, to avoid scratching the gold using a slow-speed latch-type contra-angle. The first powder is a No. 4 flour of pumice (Patterson Dental, St. Paul, MN) used wet; the second a 15-µm aluminum oxide (Universal Photonics, Inc, Hicksville, NY), also used wet; and the last is a 1-µm aluminum oxidel, typically used dry.
Additional Retention Techniques
Other retention techniques are occasionally necessary in a preparation because of a short clinical crown with short walls, a large wide open proximal box, and other reasons. There are a few ways to create very retentive restorations. Rather than going to an onlay, which may further shorten the walls of a preparation, there are different types of pins, bales, and slots that can be employed. Experience will guide the operator toward what is most appropriate. Some alternatives are described below.
Tapered Fissure Pins
Pins are small holes made in a preparation using a .027 twist drill (Colténe/Whaledent, Cuyahoga Falls, OH) and then carefully impressed to become part of the casting. These are placed in smaller preparations (eg, a pin-ledge or distal hollow grinds).
Bales
A bale (ie, a finger) is similar to an occlusal lingual on a maxillary first molar. It is most commonly found on mandibular molars where the casting may include a small buccal pit. A No. 7404 bur is used to create the bale. Note: always hold the bur in the long axis of the tooth for proper draw.
Tapered Fissure Slot
Another method to increase retention is to place a slot into a preparation, which then is impressed and becomes an integral part of the casting. This can be done with a No. 170L carbide (Brasseler USA and SS White), placing the slot at a point farthest away from where there is a lack of retention. It should be deep enough (ie, 1.5 mm to 2 mm) to do the job and have the same draw as the entire preparation. If necessary, more than one may be used.
Tucker Pin
Typically in a larger restoration where retention is minimal, this is a larger pin made with a Midwest TF 7404 bur (Midwest Dental Products Corp, Des Plaines, IL). Placement of the bur within the long axis of the tooth and preparation is suggested.
Case 1
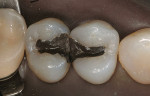
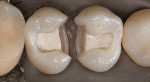
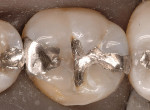
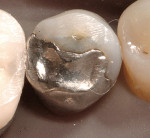
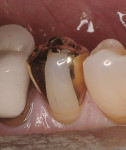
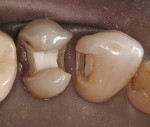
A patient presented with two failing amalgam restorations (Figure 1). They demonstrated years of wear on the occlusal and interproximal surfaces. The amalgam was removed and block-out was placed to help limit the outline form of the inlay preparations (Figure 2). Two two-surface cast gold inlays were placed with more ideal interproximal and occlusal contours (Figure 3).
Case 2
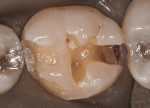
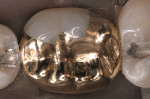
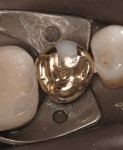
A patient presented after having sheared off the mesiolingual of his mandibular first molar (Figure 4). In addition, there was a large wear facet on the distal-occlusal, and he exhibited distal caries. All amalgam was removed (Figure 5) and block-out placed. It was determined to prepare a modified seven eighths crown with a pin for extra resistance form and retention. The functional buccal cusp was left as intact as possible (Figure 6). The finished casting (Figure 7) was seated, finished, and polished (Figure 8).
Case 3
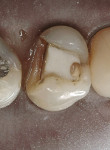
A patient presented with a large failing amalgam and obvious occlusal wear (Figure 9). Amalgam was removed, block-out was placed, and a preparation was made for another modified seven eighths crown (Figure 10). The specific No. 7404 carbide was used to remove the occlusal wear and create a cast-gold stop for the opposing tooth (Figure 11 and Figure 12).
Case 4
A patient was prepared with a tapered fissure slot on the mesial of the pulpal floor (Figure 13). A precise impression was taken, which allowed the technician to construct a two-surface inlay with a slot (Figure 14).
Case 5
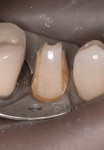
A patient presented with distal caries on a maxillary cuspid. A distal slot preparation was prepared (Figure 15). An external bevel and internal acuteness were necessary on the finished casting (Figure 16). When a restoration is required on the mesial of the adjacent tooth, this approach facilitates access for the operator. The finished restorations were seated, finished, and polished (Figure 17).
Conclusion
One of the primary goals of cast-gold dentistry is to be conservative, making every possible effort to preserve tooth structure. It is possible in many cases to construct intracoronal restorations and prevent the removal of additional tooth structure involved with full-crown preparations. Other equally important reasons to place cast-gold restorations are their function and longevity, which are possible only with this underused material. If the technique described is learned and practiced properly, restorations can be placed that have the potential to last many years longer than any other material in use in dentistry today.
Acknowledgment
All of the laboratory work featured in this article was completed by Penny Marrazzo at Stoneybrook Noble Gold in Newtown, PA.
References
1. Erpenstein H, Kerschbaum T, Halrin T. Long-term survival of cast-gold inlays in a specialized dental practice. Clin Oral Investig. 2001;5:162-166.
2. Hickel R, Manhart J. Longevity of restorations in posterior teeth and reasons for failure. J Adhes Dent. 2001;3:45-64.
3. Mjör IA, Medina JE. Reasons for placement, replacement, and age of gold restorations in selected practices. Oper Dent. 1993;18:82-87.
4. Ring ME. Dentistry: An Illustrated History. St. Louis, MO: Mosby; 1985:48, 113, 119-123, 206, 305.
5. Summitt JB, Robbins JW, Schwartz RS. Fundamentals of Operative Dentistry: A Contemporary Approach. 2nd ed. Chicago, IL: Quintessence Pub. Co.; 2001.
6. Baum L, Phillips RW, Lund MR. Textbook of Operative Dentistry. Philadelphia, PA: Saunders; 1981.
7. Sturdevant CM. The Art and Science of Operative Dentistry. 3rd ed. St. Louis, MO: Mosby; 1995.
8. Shillingburg HT, Hobo S, Fisher DW. Preparations for Cast Gold Restorations. Chicago, IL: Buch- und Zeitschriften-Verlaz Die Quintessenz; 1974.
9. The Academy of Richard V. Tucker Study Clubs. www.rvtucker.org.
10. Donovan T, Simonsen RJ, Guertin G, et al. Retrospective clinical evaluation of 1,314 cast gold restorations in service from 1 to 52 years. J Esthet Restor Dent. 2004;16:194-204.
About the Author
Bruce W. Small, DMD, MAGD
Associate Professor of Restorative Dentistry
University of Medicine and Dentistry of New Jersey
Newark, New Jersey
Private Practice
Lawrenceville, New Jersey