Oral Cancer Screening: a Paradigm Shift for the General Practitioner
Fred Balzac
William L. Balanoff, DDS, MS, is nearing the end of his presentation on oral cancer screening when he drives the take-away message home with a cautionary tale. It involves a 59-year-old male patient who had refused to give his dentist, Dr. Balanoff, permission to do an innovative new screening examination. As Dr. Balanoff recounts the case, it is 1 year later and he and one of his hygienists are performing that same screening exam (ViziLite® Plus, Zila Inc, Phoenix, AZ) (Figure 1).
The method consists of a chemiluminescent light source for identifying mucosal abnormalities and a pharmaceutical-grade tolonium chloride formulation (TBlue630™ Oral Lesion Marking System) used to mark lesions differentiated by the light source. The chemiluminescent light locates a lesion on the floor of the patient’s mouth, and the growth retains the blue dye of the tolonium chloride formulation (Figure 2). Dr. Balanoff refers the patient to an oral surgeon, who reports back that the floor of the mouth is not an area he works on. The patient is then referred to an otolaryngologist (ENT), who performs an endoscopy and discovers a stage IV adenocarcinoma of the esophagus. The patient subsequently dies from the cancer.
“What if he had agreed to the dentist doing an oral cancer screening a year earlier?” Dr. Balanoff asked in a presentation at the 2nd Annual Oral Cancer Symposium held at Tufts University in Boston. “I don’t know if the patient would have lived or not, but he certainly would have had a shot at living.”
With an estimated 34,000 new cases of oral squamous cell cancer diagnosed each year, oral cancer represents approximately 3% of all cancers in the United States. It has 3 times the incidence and 2 times the mortality (with an estimated 7,450 deaths per year) of cervical cancer. And as with other forms of malignancy, late diagnosis of oral cancer is associated with poor outcome.1
There are several screening methodologies available to practitioners, including chemiluminescence and autofluorescence. ViziLite Plus, the screening examination Dr. Balanoff advocates, can be performed by hygienists in almost every state in the country. The method does not require general practitioners to become experts at identifying lesions. Rather, the dentist only needs to be up front with his or her patients about the risk for oral cancer and then to be cognizant enough of what constitutes an abnormality to send the patient to a specialist.
“Our job is to talk about cancer,” Dr. Balanoff observed. “That’s what we do. We’re dentists.... Hygienists are allowed to do the screening because they are not diagnosing—they are preassessing. Even if you get a ViziLite-positive lesion and a TBlue-positive lesion, has the general dentist diagnosed anything, really? He’s just preassessing also, and off it goes to the oral surgeon or the ENT to make the final evaluation.”
In speaking to dental professionals over the years, Dr. Balanoff has found that hygienists often emphasize how busy they already are and resist the idea of adding one more step to their daily protocol. “‘When you’re finishing your adult re-care or your perio-maintenance, how long does it take for the doctor to come into the office?’” he said, relating a typical conversation. “The hygienist will usually answer, ‘5 to 10 minutes.’ I tell them, ‘Great—that’s how long that light stays lit. So go ahead and do a ViziLite examination. You’ll be doing a better examination, and you won’t be taking away any more time. It is enhancing the standard of care for your practice.’”
IT’S A VISION THING
Dr. Balanoff maintains that he has become passionate about oral cancer screening because, as a dentist who has been practicing for a long time, he realized that many things are going on in the mouths of his patients that he simply cannot see. He needed an adjunctive tool to aid his and his hygienists’ vision. “There are some academicians who will make the argument that you should be able to see all this stuff,” said Dr. Balanoff. “But I’m telling you that we don’t. If we did, we wouldn’t be missing things.”
As a paid consultant to Zila Pharmaceuticals, Dr. Balanoff travels around the United States speaking about the critical need for oral cancer screening and the efficacy of ViziLite Plus. His passion for this particular screening tool stems from the case that occurred almost 4 years ago involving another patient of his—a retired lawyer living in South Florida who had a history of long-term smoking and alcohol consumption. A ViziLite exam made by the hygienist revealed a white lesion, 2 mm in diameter, on the lateral border of the man’s tongue. The patient was then referred to an oral surgeon.
“The oral surgeon, who I knew as a colleague from the local dental school, calls me up and says, ‘Bill, it’s such a small thing, why do you want to biopsy it?’” Dr. Balanoff recounted. “I said, ‘I can’t explain [the lesion] away. You’re supposed to biopsy it, so please do that.’ He does, and it turns out to be carcinoma in situ.
“What did we do? We found the cancer at a very early stage.”
The patient was able to keep his tongue, although he did die about 18 months later. “He dies of heart disease, but he doesn’t die because of me,” said Dr. Balanoff, who added that the case was reported in Newsweek Online about 3 years ago.2 “In the article, I get the credit, but my hygienist really was the brains behind the operation.”
SPEAKING ABOUT THE UNSPEAKABLE
In Dr. Balanoff’s view, the need for screening in the general dental practice is based on two fundamental realities: the unacceptably high prevalence of oral cancer and the likelihood that practitioners are going to miss an equally unacceptable number of lesions without the use of an adjunctive screening tool.
The National Cancer Institute defines cancer screening as a “means of detecting disease early in asymptomatic people,” including the proviso that “positive results in cancer screenings are usually not diagnostic but identify persons at increased risk for the presence of cancer who warrant further investigation.”1 Cancer also occurs, of course, in individuals who are not considered high risk. Dr. Balanoff cited a 1998-2000 retrospective study finding that 33% of patients with squamous cell cancer had no history of smoking.3 “So we know that smoking is not the only thing we should be paying attention to,” he said. “Of course, we perform manual examinations, but we miss abnormalities.”
One reason why abnormalities are missed is a characteristic that appears to be inherent in a general dentist’s office. “We’re busy, we’re churning it out,” he said. “We don’t have a lot of time to be looking around. We rely very heavily on the hygienists, but they are just as busy. So we need something adjunctive.”
According to the results of a large retrospective study conducted in Ireland, of patients found to have oral squamous cell cancer, only 6% had a biopsy before it was eventually diagnosed.4 “It means 94% of the time we’re missing,” Dr. Balanoff said.
Even the use of the word cancer in the dentist’s office seems to be controversial. “In my office in Fort Lauderdale, which is two blocks off the beach, everything’s very high-end prosthetics,” Dr. Balanoff explained. “So in an office where we’re banging out veneers and implants, [imagine] the idea that somebody like me, in this highfalutin practice in Fort Lauderdale, was going to talk about cancer! When we decided to introduce this product about 4 years ago, I was afraid to talk about cancer.”
He thinks television shows such as Extreme Makeover and The Swan may be doing the public a disservice. The programs discuss bleaching and veneering teeth and occasionally even periodontal disease, but they never mention oral cancer, according to Dr. Balanoff. “We have to turn that pyramid upside down,” he said. “The very first thing we need to talk about with our patients is cancer. We need to screen them for cancer. And if we’re able to keep them alive, then we’ll diagnose the disease and, at the end of the day, if we want to make it look pretty, we can.
“I don’t have a problem talking about cancer any more. We now talk about cancer all the time. My screening is to accelerate the possible need for a biopsy.”
THE WISDOM OF HANDING OFF
In dentistry, on a day-to-day basis, the average GP does not need to know about molecular biology or pathology. “I’m here to argue that it’s not my job to know all this stuff,” Dr. Balanoff declared. “What we need to know is, what is abnormal? And, if there is something abnormal, get it out of your office and into the hands of a specialist.”
He draws on a medical analogy involving his own health. He had decided to increase his disability insurance and had to be screened for several disorders, including cardiovascular disease. He underwent an electrocardiogram, which turned out to be abnormal. “Does my GP diagnose any potential heart disease that I have?” Dr. Balanoff asked. “No, he gives me a boot out of his office into the hands of the cardiologist....
“My argument for the general [dental] practitioners, who see a majority of the patients, is you have an obligation to screen patients just the way our medical colleagues do for different diseases. When you find something abnormal, you don’t have to go through this long list for a differential diagnosis.”
Screening saves lives, but the diseases practitioners routinely screen for do not always correspond to the epidemiological realities. Dr. Balanoff pointed to the 55 to 60 million Pap smears done per year to screen for a cancer that has one third the rate of oral cancer.5 “These are the kinds of take-home messages that we need to talk about in our offices,” he said. “There’s a poster that Zila has that says one American dies every hour from oral cancer. We have that poster in our office. That sends a message to the patient that this is important.”
He presented a series of slides showing squamous cell cancers and other malignancies that were initially misdiagnosed and/or treated as such conditions as trauma or irritation (Figure 3; Figure 4; Figure 5; Figure 6). “Very often when I give presentations around the country, the dentists and the hygienists will be sitting there, and they’re trying to figure out what this is,” he said. “And I always tell them relax. You don’t need to know what this is. All you need to know is that this is abnormal and then get it into the hands of the specialist.”
Dr. Balanoff referred to a protocol indicating that, if an abnormality does not resolve within 14 days, the practitioner should send it off to a specialist.6 “Different offices have different protocols,” he said. “I’ll tell you what my protocol is: if I find something abnormal that I cannot explain away, I want it out of the office that day.
“What’s my rationale for that? If I’m the patient, and say I’ve got a leukoplakia or an in situ or a cancer and I wait 14 days before the evaluation of the diagnosis of that lesion is made. You know what I’m thinking? I just lost 14 days of treatment.... I’ve seen a lot of cancer patients because of my specialty. I see them before and after the radiation oncologist, and I see them after the oral surgeon. They’re not looking so good at that point, and they start counting those 14 days toward the end.”
TANGLED UP IN BLUE
Dr. Balanoff devoted the remainder of his presentation to a discussion of the ViziLite Plus system, including several clinical studies supporting its efficacy. Studies have shown TBlue630 to have a sensitivity ranging between 84% and 100% and a specificity between 44% and 100%.7 Based on such results, Dr. Balanoff now does a ViziLite examination of every single patient he sees.
“If I have a ViziLite-positive lesion and I use TBlue and it stains blue, studies indicate that there is a 80% positive predictive value that within 44 months it will become cancer,” he said.8 “That is huge. Finally, research scientists are speculating that we’re taking advantage of this TBlue binding to these cells and having a certain amount of prediction as to where this patient is going to be later on down the pipeline.”
CONCLUSION
At the end of his lecture, Dr. Balanoff took some pains to make one point especially clear: general dentists do not diagnose oral cancer. “They just don’t,” he said. “They’re not trained in it and rarely are they doing biopsies.”
The care of patients with oral cancer, he concluded, is best left to a team consisting of such specialists as an oral maxillofacial surgeon, an ENT, and a radiation oncologist, with a prosthodontist or maxillofacial prosthodontist involved if radical surgery is suggested.
References
1. Data on file. National Cancer Institute. Available at: www.cancer.gov. Accessed November 7, 2007.2. New screening tools could help dentists save lives through the early detection of oral cancer. Should insurance companies be paying for the test? Available at: www.newsweek.com/id/55516. Accessed November 7, 2007.
3. Schmidt BL, Dierks EJ, Homer L, Potter B. Tobacco smoking history and presentation of oral squamous cell carcinoma. J Oral Maxillofac Surg. 2004;62(9): 1055-1058.
4. Bromwich M. Retrospective study of the progression of oral premalignant lesions to squamous cell carcinoma: a South Wales experience. J Otolaryngology. 2002;31(3):150-156.
5. Melnikow J, Birch S. Human papillomavirus triage of atypical squamous cells of undetermined significance: cost-effective, but at what cost? J Natl Cancer Inst. 2006;98(2):82-83.
6. Golden DP, Hooley JR. Oral mucosal biopsy procedures: excisional and incisional. Dent Clin North Am. 1994;38(2):279-300.
7. Epstein JB, Silverman S, Epstein JD, et al. Analysis of oral lesion biopsies identified and evaluated by visual examination, chemiluminescence, and toluidine blue. Oral Oncol. 2007 Nov 7;[Epub ahead of print].
8. Zhang L, Williams M, Poh CF, et al. Toluidine blue staining identifies high-risk primary oral premalignant lesions with poor outcome. Cancer Res. 2005;65(17): 8017-8021.
 | 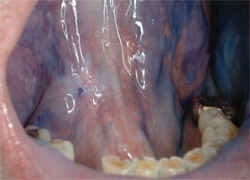 | |
| Figure 1 The ViziLite Plus. | Figure 2 Clinical photograph depicting a precancerous lesion under ViziLite and TBlue630 staining. | |
| Figure 3 through Figure 6 courtesy of Sol Silverman, Jr, DDS. | ||
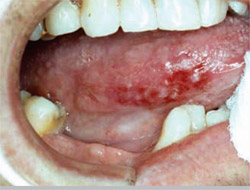 | 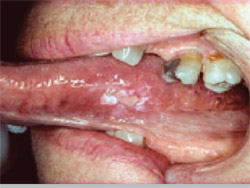 | |
| Figure 3 Squamous cell carcinoma presumed to be a benign chronic irritation. | Figure 4 Squamous cell carcinoma treated as trauma before referral. | |
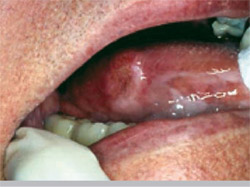 | 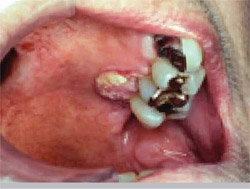 | |
| Figure 5 Squamous cell carcinoma treated as an irritation fibroma before referral. | Figure 6 Gingival carcinoma misdiagnosed and treated as a periodontal infection. | |



