The Challenge of Restoring Teeth with Darkness in the Gingival Third
Thomas Dudney, DMD
In the past two decades, dentistry has developed to a point where achieving outstanding esthetic results is possible even when clinical situations are far from ideal. One such challenge is restoring teeth with dark preparation color extending subgingivally. Fortunately, dentists have more and better restorative options than ever to help solve this and many other esthetic dilemmas. While the ever-expanding array of options might be confusing, understanding these advanced alternatives could be crucial to maximizing an esthetic, functional, and stable outcome. The purpose of this article is to document an esthetic maxillary anterior case where full-coverage restorations were required and some of the teeth to be restored exhibited darkness in the gingival third.
CLINICAL SITUATION
A female patient presented with the chief complaint of being unhappy with her smile (Figure 1). She indicated that the porcelain-fused-to-metal crowns were dark at the gumline and not as light in color as she would like (Figure 2A through Figure 2C). The patient’s expectations were for a very esthetic result in the gingival third of her crowns with no visible margins, along with healthy looking soft tissue.
A clinical examination and x-rays revealed several failing restorations and worn mandibular incisors. Although gingival recession was obvious due to the exposed unsightly traditional metal margins, periodontally she was stable and her temporomandibular joints were healthy with no muscle soreness.
MATERIAL SELECTION
When selecting a restorative material, there are many factors to be considered, including: the shade variance between the stump shade and desired result, desired translucency, bite, strength, lip line, biocompatibility, preparation requirements, margin placement, margin design, tissue biotype, whether materials can be cemented conventionally or require adhesive bonding, and are there cores and/or build-ups, or implants. Captek™ (Precious Chemical Company, Inc, Altamonte Springs, FL), a metal composite material for crowns- and-bridges, is an important esthetic restorative solution. When fabricated thoughtfully, it can be a crucial tool in the restorative dentist’s armamentarium of products used to resolve simple and complex clinical esthetic dilemmas caused by the variables listed above.1
Homogeneous vs Heterogeneous Materials
In an article2 and lectures by Dr. Frank Spear, he finds it helpful to place materials into two categories when searching for esthetic solutions: homogeneous and heterogeneous. His belief, which is shared by the author, is that consideration should be given to the most conservative approach that can achieve the desired esthetic and functional result.2 The concept of being as conservative as possible yet achieving maximum esthetics makes understanding material properties very important.
Heterogeneous materials use an internal core over which porcelain veneering materials can be either stacked or pressed. Theoretically, systems with cores are helpful when the ultimate tooth shade relies solely on the restoration regardless of the underlying tooth structures. The internal core can have varied degrees of opacity and colors. Usually, preparation requirements need to allow for the thickness of the core material. Conversely, homogeneous materials are made from the same material throughout and tend to be developed for maximum translucency. As there is only one material to stack, press, or mill, preparation requirements might be different.2
In order to satisfy the patient’s request for smile enhancements and given the clinical situation, it was decided that some type of full-coverage heterogeneous restorations were necessary. Ten maxillary anterior Captek crowns were chosen as an esthetic solution to provide a consistent background for the ceramist yet still produce a warm, esthetic, and pleasing gingival third color in the crown as well as helping to support natural tissue esthetics. Composite metal, such as other metal ceramics, and including alumina- and zirconia-based restorations, are developed with a high-strength core. Composite metal is a thin, yet ridged, warm, gold-colored substructure that does not oxidize or corrode.3 There is strong potential with the thin, (0.25 mm) warm, gold understructure to impart natural vital colors into the porcelain and the surrounding soft tissues.4 Esthetics do not have to be compromised and in many instances are enhanced when metal is extended to the edge covered by porcelain. It is the author’s opinion that a warm, natural hue from composite metal has obvious advantages over traditional high noble, noble, and base alloys, as well as over the high value and chroma of zirconia and alumina cores. Zirconia and alumina, also heterogeneous in nature, can achieve light shades over dark underlying tooth structure but may look artificial in the gingival third because of the highly opaque white core. However, the composite metal—also referred to as "reinforced gold" technology—provides metal-ceramic strength factors,5 reduced plaque and bacteria,6 excellent marginal fit,7 versatility to accommodate a variety of margin designs (even within the same tooth), and the ability to cement conventionally. All of these attributes were deemed to be important in this case.
Although not appropriate for the case presented, composite metal can be cut back from the margin for an all-ceramic margin, thus taking on the characteristics of both a heterogeneous and homogeneous material. A clinician can derive the benefits of a high-strength core with the translucency in the gingival third of a homogeneous restoration. Small lower anteriors with thin-tissue biotype is a clinical example that might require the benefits of a composite metal; yet when a small 0.5-mm porcelain margin is placed buccally, it will then incorporate the behaviors of a homogeneous material as well. Conservative chamfer margins placed at the tissue height can accomplish outstanding esthetics yet be conservative.8 In most cases, deciding where to end the metal edge in relation to the ceramic and the preparation (ie, metal collar, metal-and-porcelain to the edge, or porcelain-butt margin such as 180° or 360° butt, 0.5- to 2-mm metal cut back) is important for practitioners and laboratories to keep in mind. Once again, in the case of dark gingival colors requiring a significant color shift, composite metal extended to the edge is indicated.
PREPARATION AND TEMPORIZATION
At the preparation appointment the old crowns from teeth Nos. 4 through 13 were removed, the teeth were cleaned and built up where necessary, and the margins were redefined (Figure 3). Definitive chamfer margins were chosen, using a 6848 016 medium diamond (Brasseler USA, Savannah, GA). It is the opinion of the author that this diamond is easy to use and creates enough room for "composite metal" margins veneered to the edge with porcelain, while still allowing for natural esthetics and proper emergence profiles. All sharp internal angles and points were removed. A new, medium grit diamond is efficient for gross reduction as well as final margination.9 After the preparations were completed, a face bow transfer (Artex Rotofix facebow, Jensen Industries, Inc, North Haven, CT), bite registration, stick bite for horizontal reference, and vinyl polysiloxane (Honeigum®, Zenith/DMG, Englewood, NJ) impression were taken. Additionally, preoperative photographs of the patient (full-face, close-up smile, retracted views, pictures of the preparations, and a stumpf shade recording) were included with the laboratory prescription.
Provisional restorations were made using a Sil-tech (Ivoclar Vivadent, Amhurst, NY) putty matrix of the diagnostic wax-up and Luxatemp® (Zenith/DMG) fluorescent shade BL temporary material. Great care was taken in the fabrication of the provisionals. The provisionals are an invaluable tool in dentist-laboratory and dentist-patient communication. It is the author’s opinion that in shade selection of provisionals, it is best to start with a lighter, brighter shade and then, based on patient feedback, decrease the value if necessary. In addition, provisionals are used to confirm the incisal edge position, length of centrals, occlusion, anterior guidance, and phonetics. To obtain and verify this information it is best to have the patient return postoperatively when anesthesia is no longer a factor. In this case, the patient returned the following day and the feedback was favorable. However, if changes had been made they would have been noted and communicated to the laboratory. Retracted and non-retracted pictures along with an impression (Status Blue®, Zenith/DMG) of the approved provisionals were taken and forwarded to the laboratory.
SEATING AND CEMENTATION
At the seat appointment the provisional restorations were removed and the preparations were cleaned with hydrogen peroxide. The definitive restorations (Figure 4A through Figure 4D) were seated to check for passive yet complete fit, margin fidelity, interproximal contacts, occlusion, and patient acceptance. All were satisfactory and the teeth were prepared for cementation. Composite metal restorations can be treated with 50-mm aluminous oxide at 40 psi (light pressure) and cemented conventionally, which can be advantageous when restoring posterior teeth and/or teeth with subgingival margins. The restorations were lined with cement (RelyX™, 3M ESPE, St Paul, MN) and seated. After cleaning the excess cement, the occlusion was checked again and the patient was reappointed for a postoperative evaluation. As with the provisional restorations it is important to confirm the incisal display, length, position, and shape of the definitive restorations when the patient’s lip is not anes-thetized. It is also important to recheck the occlusion at this time. At the postoperative visit, minor adjustments were made and the patient stated that she was very happy with the appearance of her new smile (Figure 5A through Figure 5D).
CONCLUSION
Even with the many esthetic restorative options available today, it is still difficult to find one material that is the perfect solution for every clinical challenge. Composite metal crowns-and-bridges can be altered at the margin to be a completely heterogeneous or to take on the properties of a homogeneous material. When altered appropriately, and in concert with the other optical properties composite metal provides, this can greatly assist the laboratory and restoring dentist to achieve predictable esthetic results when tooth condition, preparation color, and margin type vary within the same tooth and from tooth to tooth.
ACKNOWLEDGMENT
The author would like to acknowledge his gratitude to Adrian Jurim of Jurim Dental Studio (Great Neck, NY) for the fabrication of the restorations.
References
1. Dudney T. An innovative restorative option for the maxillary arch. Inside Dentistry. 2006;2(9):82-90.2. Spear F. Treatment planning materials, tooth reduction, and margin placement for anterior indirect esthetic restorations. Advanced Esthetics and Interdisciplinary Dentistry. 2005;1(4):4-14.
3. Shoher I, Whiteman A. Captek™: a new capillary casting technology for ceramometal restorations. Quintessence Dent Tech. 1995;18:9-20.
4. Nathanson D, Nagai S, Po S, et al. Preliminary evaluation of the effect of crown on gingival color. Abstract. Presented at: International Association for Dental Research meeting. March 10-13, 2004, Honolulu, Hawaii.
5. Juntavee N, Nathanson D, Giordano R. Load bearing capacity of Captek crowns and bridges. J Dent Res. 1995;74 (Special issue). Abstract 565.
6. Goodson JM, Shoher I, Imber S, et al. Reduced dental plaque accumulation on composite gold alloy margins. J Periodontal Res. 2001;36(4):252-259.
7. Juntavee N, Nathanson D, Giordano R. Marginal fit of Captek and conventional metal-ceramic restorations. J Dent Res. 1995;74 (Special Issue). Abstract 167.
8. Rubinstein S, Nidetz A. An esthetic alternative in full-coverage restorations. Contemporary Esthetics and Restorative Practice. 2004;8(11):36-40.
9. Goodacre C, Compagne WV, Aquilino SA. Tooth preparations for complete crowns: an art form based on scientific principles. J Prosthet Dent. 2001;85:363-376.
 | 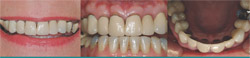 Figure 2A through Figure 2C Preoperative views. The patient was unhappy with the unrealistic look of traditional PFMs and the dark lines at the gum line. | |
| Figure 1 Preoperative smile. | ||
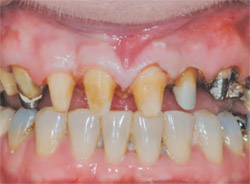 | Figure 3 Preparation of teeth Nos. 4 through 13. Notice variance of underlying condition and color between teeth to be restored. | |
| Figure 4A through Figure 4D Composite metal copings with the metal extended to the edge for maximum color control. | Figure 5A through Figure 5D Postoperative views. A lighter, healthier, more esthetically pleasing result was achieved. | |
| About the Author | ||
 Thomas Dudney, DMD Thomas Dudney, DMDPrivate Practice Birmingham, Alabama | ||





