Laser-Assisted Cosmetic Dentistry: Putting Technology to Work
Patrick J. Broome, DMD, MBA
Today, patients desire not only functional dentistry but dentistry that makes them feel better about themselves. Cosmetic dentistry is no longer limited to strictly anterior procedures; it now includes almost any procedure that is subject to the critical eye of patients. Mass media and direct-to-consumer marketing of dental products and procedures (whitening and orthodontic appliances) have increased the public’s awareness of modern dentistry’s potential. Patients are better educated about their dental health and better versed in dental materials and treatment options available to solve their respective dental issues.
By staying current with the latest materials and techniques as well as embracing technology such as digital radiography, digital imaging, computer-assisted design/computer-assisted manufacturing (CAD/CAM), and hard- and soft-tissue dental lasers, dentists can not only meet but routinely exceed patients’ expectations.
This case illustrates the value of technology in the dental practice and several ways it translates to a return on investment for the practitioner.
CASE PRESENTATION
The following patient presented because of a direct personal referral from an exist-ing patient who had recently experienced routine restorative dental treatment in the author’s office. The referring patient’s restorations were performed without anesthesia using an erbium-chromium– dosed yttrium, scandium, gallium, and garnet (Er,CR:YSGG) hard- and soft-tissue laser (Waterlase MD™, BIOLASE Technology, Inc, Irvine, CA). This positive experience led the patient to recommend the author’s practice to a friend who was interested in more complex treatment. This situation represents the power of great experiences and the impact every procedure, large or small, has on your practice. By leveraging technology, dentists can grow a practice as well as professional and personal satisfaction.
A 53-year-old man presented for a cosmetic evaluation. The patient’s chief complaint was general unhappiness with the color, shape, and worn appearance of his smile. Using digital images of his full face, smile, and retracted views of the dentition, a discussion ensued that included an in-depth review of his previous dental experiences as well as desired outcomes of future treatment. This initial meeting is perhaps the most important visit because it provides an invaluable opportunity to acquaint the patient with your practice philosophy and capabilities as it relates to his or her particular area of concern. The goal of this meeting is simply to learn about each other and exchange information. Although this patient’s primary concern revolved around cosmetics, he was also con-cerned with the progressive attrition of his teeth. Digital imaging provided a visual reference during the discussion of the functional issues that manifested themselves as attrition and chipping of the dentition. After the initial consultation the patient elected to move forward with the comprehensive diagnostic examination that involved a full-mouth series of digital radiographs, including bitewing, T-scan occlusal evaluation, facebow records, impressions for mounted diagnostic models, and digital photographs. Full-mouth periodontal charting/probing, a complete oral cancer examination, record of existing restorations, gingival levels, occlusal wear, and areas of abfractions was included in the comprehensive treatment plan for his entire dentition.
CLINICAL FINDINGS
Extraoral findings were unremarkable. An intraoral examination revealed recurrent caries approximating the margins of all full-coverage restorations; all periodontal readings were within normal limits of health. Radiographic examination revealed recurrent caries approximating several existing amalgam restorations. T-scan examination revealed anterior and posterior prematurities in centric occlusion as well as lateral excursive interferences. Gingival asymmetry was noted in the area around teeth Nos. 8 and 9. Crown lengthening was indicated to obtain ideal symmetry in the anterior segment from teeth Nos. 6 through 11. Generalized attrition was noted with significant maxillary and mandibular incisal wear (teeth Nos. 6 through 11 and teeth Nos. 20 through 28) (Figure 1 and Figure 2).
TREATMENT PLAN
A long-term solution to the patient's primary esthetic concern cannot be achieved without recognition and correction of the underlying functional issues contributing to the attrition of the dentition. Proper occlusion and load balancing is critical for long-term success of such a case.1-3
A comprehensive approach that involved treating the entire maxillary and mandibular dentition (teeth Nos. 2 through 15 and teeth Nos. 18 through 31) was proposed to obtain complete control over the functional issues as well as to deliver superior esthetics. The treatment plan was formulated in two phases to obtain maximum control over occlusion, esthetics, and phonetics.
Phase One
Phase one included the preparation of teeth Nos. 4 through 13 and teeth Nos. 20 through 29 for conservative porcelain restorations, the correction of existing gingival asymmetry via crown lengthening and gingival re-contouring, bite adjustments performed as needed, and observation for 3 weeks in temporary restorations to determine tolerance of the new length and occlusal contact distribution.
Phase Two
Phase two included the preparation of teeth Nos. 2, 3, 14, 15, 18, 19, 30, and 31 for porcelain restorations that replaced the existing porcelain-fused-to-metal crowns. Proper occlusal force distribution allows predictable and confident placement of all-ceramic restoration in the posterior dentition. Regardless of retention method (cementing vs bonding), proper resistance and retention form was required.
PREPARATION
Teeth Nos. 4 through 13 and teeth Nos. 20 through 29 were prepared for conservative powder-liquid (feldspathic) porcelain restorations. Due to the presence of a normal tissue (keratinization) and bone biotype, the correction of gingival asymmetry was accomplished in a single-visit procedure that used the Er,Cr:YSGG laser to first perform gingival re-contouring to obtain proper zenith location in relation to teeth Nos. 6, 7, 10, and 11.4,5 The alteration of the bony crest via a closed crown-lengthening technique was completed to re-establish the proper biologic width (3 mm) required from the restorative margin (Figure 3). The closed technique is best used for minor biologic width corrections and allows the completion of the restorative procedure without the necessary healing time required for open crown lengthening. The specific technique involves using a periodontal probe to sound to the osseous crest and establish the preoperative bony crest levels.6 By marking the laser tip at 3 mm from the working end with a sterile felt-tip marker, the clinician can use this line as a reference and follow the new free gingival margin level when repositioning the bone height. Holding the tip parallel to the tooth, a 600-µm tip is used like a periodontal probe and inserted into the sulcus and sounded to bone. The laser is activated and the tip is “walked” over the bony area that requires removal in a “sewing-machine” (ie, up-and-down) movement to a 3-mm depth. After the proper crest level is established, the bone is smoothed by changing the settings on the laser to a higher hertz setting (50 Hz) and moving the laser repeatedly in a mesial–distal direction. A periodontal probe is again used to verify that a ledge or negative defect does not exist. The final impression was made immediately after preparation because tissue migration does not occur due to a negligible zone of necrosis. Temporary restorations were fabricated using a composite mock-up on the preoperative model and a vacuum-formed matrix filled with bis-Acrylic temporary material (LuxaTemp® Fluorescence, Zenith Dental, Englewood, NJ).7,8 They were contoured, polished, and occlusion-adjusted using computer occlusal analysis (T-Scan® III, TekScan, Boston, MA) (Figure 4 and Figure 5).9,10
DELIVERY
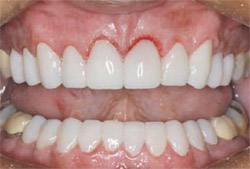
Careful observation of the patient continued for 3 weeks after preparation to verify phonetics, general tolerance of new length, and occlusal contact distribution (Figure 6).11,12 Once form and function were verified, additional information was communicated to the ceramist to aid in the fabrication of the definitive restorations. Four weeks postpreparation, the restorations were tried-in and the patient approved the esthetics (Figure 7A through Figure 8B). Restorations were bonded with light-cured resin cement (3M RelyX™ Veneer Cement, 3M, St Paul, MN), and occlusion adjusted using computer occlusal analysis (T-Scan III).
Phase two involved the preparation of teeth Nos. 2, 3, 14, 15, 18, 19, 30, and 31 for pressed porcelain restorations (IPS Empress® Esthetic, Ivoclar Vivadent, Amherst, NY); the remaining steps pro-gressed as in phase one. The final result (Figure 9A and Figure 9B) demonstrates the excellent tissue health 1 week after delivery. By using the characteristics of the Er,Cr:YSGG laser, the opportunity existed to obtain a predictable result without reflection of a traditional full-thickness flap. Use of the laser provided a significant time savings for the patient and the clinician by avoiding at least one additional restorative visit for a final impression once the tissue had healed and the preparation margins were finalized. Because of the minimally invasive nature of the procedure, the patient experience was enhanced by reducing or eliminating any postoperative discomfort.
Laser technology represents a new and exciting addition to our clinical armamentarium and should be considered as a possible option to performing traditional open-flap crown lengthening when tissue biotype and bony architecture make a minimal invasive technique possible.
CONCLUSION
Every day, clinicians have countless opportunities to make a positive impact on patients’ perception of dentistry. Patients do not care what technology you have in your office unless they know there is some benefit for them. Anything the practitioner can do to improve the patient’s experience will have a positive impact on the practice. New technology should be viewed as an investment in your practice and considered when the investment will improve clinical results, make a positive impact on the patient’s experience, and/or improve the overall efficiency/quality of the practice.
The above case illustrates the use of many technologies such as digital imaging, digital radiography, digital occlusal analysis, and a hard- and soft-tissue laser. This case was made possible by another patient who had a great dental experience that led her to make a personal referral to the author’s practice. In each case technology was used to improve efficiency, the overall clinical result, and patient experience.
ACKNOWLEDGEMENTS
The author would like to thank C.K. Kim, director of the Ultimate Esthetics division of Americus Dental Labs (Jamaica, NY), for the exceptional communication and ceramic artistry demonstrated in the case.
References
1. Kois JC. Altering gingival levels: the restorative connection. 1 Biologic variables. J Esthet Dent. 1994;6(1):3-9.2. Gargiulo AW, Wentz FM, Orban B. Dimensions and relations of the dento-gingival junction in humans. J Periodontol. 1961:32;261-287.
3. Ingber JS, Rose LF, Coslet JG. The “biologic width”—a concept in periodontics and restorative dentistry. Alpha Omegan. 1977;70(3):62-65.
4. Kimura Y, Yu DG, Fujita A. et al. Effects of erbium,chromium: YSGG laser irradiation on canine mandibular bone. J Periodontal. 2001;72(9): 1178-1182.
5. Moritz AF, Beer F, Goharkhay K, et al. Oral Laser Application, Hanover Park, IL: Quintessence Publishing Co, Inc; 2003.
6. Romano R, Bichacho N, Touati B. The Art Of The Smile: Integrating Prosthodontics, Orthodontics, Periodontics, Dental Technology, And Plastic Surgery In Esthetic Dental Treatment. Hanover Park, IL: Quintessence Publishing Co, Inc; 2005.
7. Magne P, Belser U. Bonded Porcelain Restorations in the Anterior Dentition: A Biomimetic Approach. Hanover Park, IL: Quintessence Publishing Co, Inc; 2002.
8. Gurel G. The Science and Art of Porcelain Laminate Veneers. Hanover Park, IL: Quintessence Publishing Co, Inc; 2003.
9. Garcia, VCG, Cartagena, AG, Sequeros, OG. Evaluation of occlusal contacts in maximum intercuspation using the T-Scan system. J Oral Rehabil. 1997;24(12): 899-903.
10 Kerstein RB. T-Scan II’s computerized occlusal analysis brings your practice Into the future. Contemporary Esthetics and Restorative Practice. 1999;6:90-94.
11. Kerstein, R, DuPont, G. Anterior guidance and muscle function. Contemporary Esthetics and Restorative Practice. 2001;8(2):96-109.
12. Maness, WL, Podoloff R. Distribution of occlusal contacts in maximum intercuspation. J Prosthet Dent. 1989;62(2):238-242.
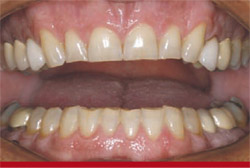 | 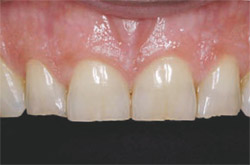 | |
| Figure 1 Preoperative retracted view. | Figure 2 Preoperative 1:2 view. | |
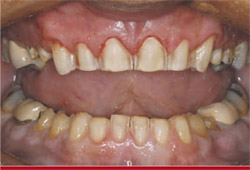 |  | |
| Figure 3 Retracted anterior view of completed preparations after gingival alteration on teeth Nos. 7 through 10 and closed crown-lengthening procedure on teeth Nos. 8 and 9. Impression is made at this visit, as tissue margin stability is predictable due to the benefits of the Er,Cr:YSGG laser technology. | Figure 4 T-Scan III unit. | |
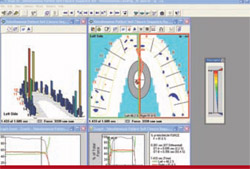 |  | |
| Figure 5 Example of T-Scan recording detailing timing and bite force per contact. | Figure 6 Retracted anterior view of temporary restorations polished and glazed immediately after laser tissue repositioning and crown lengthening. | |
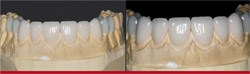 | 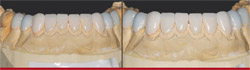 | |
| Figure 7A and Figure 7B Maxillary porcelain restorations on solid model. Restorations are examined for fit, color, and contacts before patient try-in. | Figure 8A and Figure 8B Mandibular porcelain restorations on solid model. Restorations are examined for fit, color, and contacts before patient try-in. | |
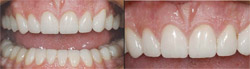 | ||
| Figure 9A and Figure 9B Retracted anterior view of completed restorations. Tissue health is excellent and the predictability of margin location is illustrated. A minimally invasive technique for hard and soft tissue corrections provided this case with ideal gingival contours as well as excellent porcelain esthetics. | ||
| About the Author | ||
 Patrick J. Broome, DMD, MBA Patrick J. Broome, DMD, MBACharlotte Center for Cosmetic Dentistry Charlotte, North Carolina | ||



