Fiber Posts: A Clinical Update
Howard E. Strassler, DMD
Restoration of an endodontically treated tooth presents a challenge to the restorative dentist. The tooth to be restore has been hollowed out as part of the endodontic treatment. Depending on the degree of instrumentation, that tooth has lost a significant amount of structural support due to the endodontic access to treat the pulp chamber and root canals. When assessing an endodontically treated tooth for restorative treatment, it has to be assumed that good judgments have been made previously concerning the periodontal status of the tooth, the remaining tooth structure, and the prognosis of the endodontic treatment. The tooth to be restored should exhibit a good apical seal when evaluating the radiograph, and also exhibit no sensitivity to percussion or palpation, no exudates, no fistula, no apical sensitivity, and no active inflammation.1
The decision to use a post when restoring an endodontically treated tooth should be based on remaining tooth structure after the removal of all caries and remaining restorative materials. If the coronal structures of a tooth are primarily intact, the primary preparation is the access opening for endodontic treatment, and the tooth has favorable occlusion (eg, an anterior tooth that has been traumatized but not fractured becomes nonvital), a routine restoration without a post would be indicated. When significant portions of the crown are missing due to caries and/or fracture or the presence of an existing restoration that restores multiple tooth surfaces, there may be the need to use a post to provide the coronal restoration with accessory retention.
The use of a post crown fabricated from gold or silver to restore a root-filled tooth was described more than 20 years ago by Fauchard.2 Today, it is accepted clinical practice to use a post to retain the coronal restoration after a tooth has been endodontically treated when significant amounts of the coronal tooth structure is missing.3 While the use of posts is the standard of care when restoring many endodontically treated teeth, there are disadvantages and risks, which include: requiring additional preparation of the root canal and removing dentin within the root canal, especially the apical end of the root; placing a post is an additional procedure when restoring the tooth; the post can interfere with endodontic retreatment through the root canal if retreatment is necessary; and the post can place undue force on the root and tooth in function that may put the tooth at risk in the future.
Endodontic posts can be classified into two groups: custom-made, laboratory-fabricated and prefabricated, direct-placement. Custom-made posts are usually fabricated by a laboratory with the coronal portion (core) attached, and are available in high-noble, low-noble, and base metals, or ceramic materials such as pressed porcelain. Prefabricated posts are available in metals, ceramics, and fiber-reinforced, resin-based substrates, and have additional subgroups of active and passive designs. Active posts engage the dentinal walls of the root canal by preparing the root canal with a slightly undersized post drill; primary retention is through a frictional fit to the walls. Passive posts require that the canal be prepared larger than the post; retention is accomplished by cementing the post into the canal with a luting material. Cements for prefabricated posts include zinc phosphate, polycarboxylate, glass ionomer, and resin.
Post design and shape has been based on both anatomic considerations and features that improve the retention of the post within the root canal, and the retention of the core material built in the coronal portion of the tooth. Post shapes include parallel-wall design, tapered design, hourglass, and hybrid parallel-tapered. Posts can have a variety of textures, such as smooth, serrated, or threaded to improve retention within the canal when cemented. The heads of some posts have retention features designed to offer additional retention of the coronal restorative material. In several research studies, the retention of posts within the root canal was improved with the addition of serrations and threads.4,5 Also, parallel-metal posts are more retentive than tapered posts when pull tests are done to evaluate retention.6,7
While metal posts (custom and prefabricated) have been the standard for many years, nonmetallic posts have been introduced to address the need for a more esthetic material in the anterior region. In the last several years there have been significant advances in the development of bondable, fiber-reinforced, esthetic posts to reinforce endodontically treated teeth.8-12 These fiber posts are improvements on other types of esthetic posts used in the past. The specific needs of light, translucent composite resins and ceramics to mimic the natural tooth require the use of translucent posts in the esthetic zone. The presence of a metal post can cause shadowing of the soft tissues adjacent to the root surface, which will adversely affect the esthetic results required of bonded resin and ceramic restorations in the anterior region.9,13,14
The earliest fiber-reinforced composite posts were introduced in the United States in 1995 and were fabricated with carbon fibers. They had excellent physical properties15 but because of the carbon, fibers were black. More esthetic fiber posts were developed and clinical trials with these earliest fiber posts (which have similar properties to the current generation of tooth-colored fiber posts) have been highly successful. In one study, over a period of 7 to 11 years, there was a 92% survival rate in 985 fiber posts.16 Other recent articles have supported the use of fiber posts to restore endodontically treated teeth.17-19 When compared to ceramic posts, esthetic fiber posts provide endodontically treated teeth with higher fracture resistance.20 In one study, it was found that serrated, parallel-sided, stainless steel posts were no more retentive than parallel-sided or tapered tooth-colored fiber posts.21
Fiber-reinforced posts are not as rigid as metal or ceramic posts. Some of the focus on fiber-reinforced posts has been on their ability to flex like the tooth. While it has been demonstrated that there is flexion in the function of teeth, the definitive restoration of any tooth should create an integrally sealed element that does not yield, bend, or flex. A number of studies have focused on functional stresses to the tooth crown when it is restored with a post and bonded composite resin versus restoring it with an integral cast-metal post and core. The results of these studies demonstrated that failure occurs at the interface between the restorative material and the tooth.22,23 The thinner the root, the greater the flexion, and the greater the failure. In fact, Reeh and coworkers24 evaluated reduction in tooth stiffness as a result of endodontic and restorative procedures, and found that the tooth was inherently stiff and resistant to flexion. Once a tooth was prepared, the rigidity was reduced. An occlusal cavity preparation reduced tooth stiffness by 20%, and loss of marginal ridge integrity with a mesial-occlusal-distal preparation reduced cuspal stiffness by 63%. In comparison, an endodontic access preparation reduced relative tooth stiffness by a mere 5%. Flexion of the post should not be the issue; instead, the focus should be on the ability of a post to dissipate the energy of function and trauma.
When a fiber-reinforced post is bonded within the root canal it dissipates functional and parafunctional forces, reducing the stress on the root.12 When catastrophic force is placed on the crown of the tooth, the post or crown will fracture instead of the post transmitting the energy of force down the root, creating a vertical root fracture.25-28 Nicholls described an engineering approach to restoring endodontically treated teeth in which the design includes a fail-safe system so that when failure occurs, it prevents irreparable damage to the root.29 Consequently, the criteria when selecting a post system should be that it is able to dissipate or absorb the function of energy and even overcome moderate trauma. Fiber-reinforced posts have demonstrated the ability to fracture at the coronal portion of a tooth restoration with the presence of catastrophic forces without fear of root fracture.30 This may be the single most compelling reason for their use. Also, research has demonstrated the ability of resin bonding with the root canal to reinforce endodontically treated teeth.31,32 Further, to ensure clinical success at least one quarter of the crown structure must remain for tooth preparation; less structure will contribute to flexion of the crown and potential post fracture.9 Also, by having at least one quarter of the crown remaining allows for the development of at least 1.5 mm to 2 mm of ferrule. Ferrule refers to the development of a preparation margin that has a width apical from the tooth with the margin extending 360° circumferentially around it. The influence of the remaining coronal tooth structure increases the fracture resistance of the restored endodontically treated tooth, especially in the anterior region. This amount of ferrule when preparing teeth will help ensure clinical success.33-37
How does one select what type of fiber-reinforced esthetic post to use? It should be translucent, to transmit light similar to that of tooth structure. The post and restorative material should minimize esthetic failure by maximizing light transmission through an all-ceramic crown, porcelain veneer, or composite resin. Even when a porcelain metal crown is used, root shadowing of metal posts can cause a "graying out" phenomenon. When a composite resin is being used either as a definitive restoration or as a foundation core for a crown, the post should bond to the composite resin, thereby creating a unified structure.38 Because the post is to be bonded to the dentin within the root canal, post length need only be the same as the height of the tooth crown or at least one half the length of the root canal. The post should also be chemically integrated into the color and translucency of the composite resin surrounding it.
The post should be easy to work with. Preparation of the canal, surface preparation of the post, adaptation of the post to the root canal, and cementation should involve a minimal number of steps to achieve the greatest clinical success. The post selected to restore the tooth should match the diameter of the root canal and not exceed one half the diameter of the root. Guttman outlined criteria for anatomic and biologic considerations when restoring endodontically treated teeth.25 He stated that thin tapering roots and anatomic irregularities and tooth thinness can contribute to perforation and root weakening during root canal preparation for post placement. When choosing parallel-sided posts, they should be sized so that additional tooth root preparation is not required to remove tooth structure where the root is thinnest, at the apical third.
When choosing an esthetic post system, there are a number of criteria that the post must fulfill to guarantee clinical success:17
- It has adequate light transmission to eliminate shadowing of the post within the tooth to maximize esthetics of the final restoration.
- It is bondable within the root canal for root reinforcement.
- It is tapered following the true shape of the root canal to avoid removing additional dentin to accommodate a parallel post, or does not require additional dentin preparation to achieve an apical seat.
- Its surface characteristics increase retention (eg, serrations or a retentive design of the post, a retentive head design for the core).
- Able to absorb and dissipate impact if the coronal portion of the tooth crown is traumatized.
- Ease of removal with an atraumatic technique if the post breaks or endodontic retreatment is necessary.
- Multiple sizes to fit different root canal diameters.
- Radiopacity.
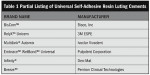
With the current generation of fiber-reinforced composite posts, many different systems will fulfill these criteria (Table 1, Figure 1).
Translucent fiber posts have been demonstrated to transmit light to eliminate the shadowing of the soft tissue adjacent to root surfaces that can adversely affect an esthetic result.9,13,14,17,39-41 Adhesion of the fiber post within the root canal has been shown to be clinically acceptable and root-reinforcing.26,42-45 These posts have been shown to have a fail-safe design where the post will fracture before the root will.25-28,43 Concern has been expressed that because the posts are fabricated from fiber-reinforced composite resin, removal will be difficult. In the case of a metal post, the technique has been to expose the post, apply ultrasonic forces to break the cement/post interface, and grasp the post with a post-pulling instrument for removal.46 Several evaluations of removal techniques have shown that the use of rotary instruments within the root canal can effectively and efficiently remove fiber posts essentially by hollowing them out of the root canal.47,48
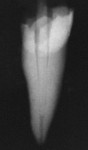
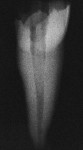
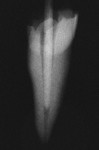
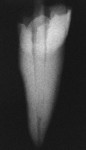
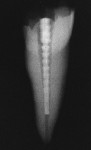
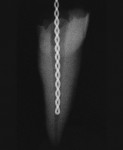
The radiopacity of fiber posts has great variability.40,49,50 Unlike metal posts that are very radiopaque and easily visible in radiographs, most fiber posts are similar to the radiopacity of dentin (Figure 2A; Figure 2B; Figure 2C; Figure 2D, Figure 2E).
Cementing Fiber Posts
Clinicians have many choices with the current generation of bonding systems, fiber posts, composite resins, and ceramics. The clinician needs to understand the chemistry and instructions to decide which materials to use for a given clinical situation. When bonding within a root canal with traditional total-etch adhesives, it is critical that the phosphoric-acid etchant be thoroughly rinsed from the root canal and that the canal be dried.8,9,17 Also, in many cases, the clinician may not know what type of sealer was used within the root canal. Studies have implicated eugenol provisional cements in the reduction of retention of restorations cemented with resin luting agents.51,52 Tjan and Nemetz53 investigated the effect of eugenol-containing endodontic sealer on the retention of prefabricated posts cemented with an adhesive resin technique, and found that the presence of eugenol within the root canal resulted in significant loss of retention. However, they also found that residual eugenol in the root canal could be removed without any effect on retention of the post by irrigating the canal with ethyl alcohol (ethanol) or etching with 37% phosphoric acid; irrigation with ethanol produced more consistent and reliable results. A substitute for ethanol irrigation is to use a 10-second phosphoric-acid irrigation to remove residual eugenol; rinse and dry the canal; follow with a second 15-second definitive etch of the canalwith phosphoric acid; rinse the canal with water using an endodontic irrigation syringe; and dry the canal of excess moisture using paper points and a microaspirator tip within the canal.9 For non-eugenol endodontic sealers, these additional steps are not necessary.
An area of recent investigation has been the compatibility of total-etch and self-etch adhesive systems with composite resin cementation. When using fiber posts, the choice of adhesives is based on chemical compatibility for cementation. Some fourth-generation, total-etch, multi-bottle adhesive systems have been shown to be acceptable with dual-cure and self-cure resin cementation. Many manufacturers have chemical reagents for specific use with dual-cure and self-cure composites. There is contradictory evidence that some single-bottle adhesive systems (fifth generation) do not bond well to self-cure and dual-cure composite resins because of the acidity of the single-bottle primer/adhesive. Studies demonstrating either a decreased bond or no effect have been reported.54-57 Some recent studies evaluating self-etch systems and compatibility with dual-cure and self-cure composite resins have demonstrated some changes in chemistry that have resulted in composite resin-adhesive compatibility.58,59
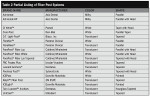
Another consideration is the depth of penetration of the curing light within the root canal to polymerize the adhesive that is placed.60,61 Total-etch, multiple-bottle (fourth generation) and dual-cure adhesives are the adhesives of choice when cementing a post within a root canal where light penetration and depth of cure will be limited. In recent years, self-etch, dual-cure composite resin cements have been introduced. These cements offer an alternative to multiple steps and potential contamination within the root canal. This family of new resin luting agents has self-adhesive capability and eliminates the need for separate etching, rinsing and drying, primer, and adhesive steps.62,63 Table 2 lists some of the cements in this category.
Case Presentations
Case 1
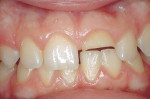
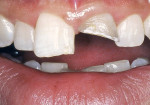
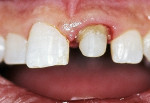
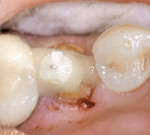
A 12-year-old boy was treated at the dental school for the fracture of a maxillary central incisor he sustained while playing ice hockey without wearing a protective mouthguard. After endodontic treatment, the tooth was restored with an adhesive composite resin without a post. During the course of 3 months, the restoration fractured and was repeatedly replaced. The third time the restoration failed (Figure 3), a thorough examination and radiographs revealed successful endodontic treatment. The tooth was negative to percussion and palpation.
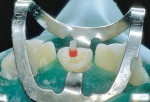
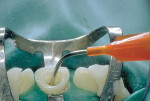
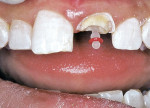
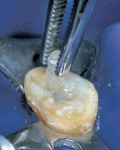
Because the previous restorations using an acid-etch bonding technique and pulp chamber for retention were insufficient for retention, it was decided to use a translucent fiber post to provide accessory retention to the composite resin restoration. After removal of the fractured composite resin, the post space was prepared and the fiber post fitted to the canal (Figure 4). For any fiber post, if it needs to be shortened, it should be cut to length using either a diamond bur in a high-speed handpiece with water spray, or a separating disk. Never use a fluted bur to cut a fiber post.
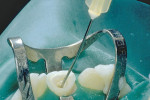
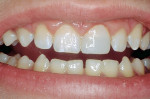
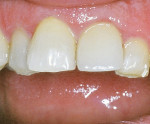
The post was cemented using a total-etch adhesive technique with a dual-cure composite resin cement. When using a total-etch in the root canal, it is important to thoroughly rinse the canal using water in an endodontic irrigation syringe (Figure 5). The canal must be thoroughly dried with air aspiration and endodontic paper points before the adhesive technique and cementation. Cementation within the root canal is best accomplished with a thin needle tip (Figure 6). The Class 4 incisal edge repair with composite resin using the fiber post for accessory retention has no evidence of shadowing due to the translucency of the post (Figure 7).
An athletic mouthguard was fabricated after the restoration was completed. If the tooth were to be traumatized again, the crown with the post would fracture without putting the tooth root in jeopardy of fracture.25-28
Case 2
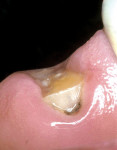
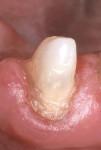
This patient was a 22-year-old with a past history (10 years previously) of endodontic treatment for the maxillary left central incisor and restoration with an adhesive composite resin, which fractured near the gingival line (Figure 8). Because of the missing tooth structure, the decision was made to retain the composite resin core with a translucent fiber post. The root canal was prepared and the gutta-percha removed using a Gates-Glidden drill. A translucent fiber post was sized for the canal (Figure 9). The selection of the fiber post was made based on its translucency and the additional retention that the head design of the post would offer.
The post was adhesively bonded to the canal using a total-etch, dual-cure adhesive/dual-cure, composite-resin cement technique. A dual-cure composite-resin core was placed. The tooth was prepared so that an adequate ferrule of 2 mm was established (Figure 10). The translucent fiber post created no shadows in the crown preparation. The tooth was restored with an all-ceramic crown that fulfilled the patient’s esthetic expectations (Figure 11).
Case 3
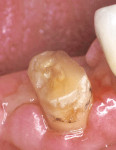
In some cases, a tooth fractures near the gingival line and an adequate ferrule cannot be attained. For this case, the mandibular canine was fractured near the gingival line (Figure 12). Crown-lengthening surgery removed the excess gingival tissues, leaving adequate tooth structure to create a ferrule in the final crown preparation (Figure 13).33-37 For this tooth, the decision was made to use a fiber post with an adhesive technique for additional tooth and root reinforcement because of the large access opening and instrumentation as part of root canal therapy.26, 42-45 When fitting the post to the root canal, it was necessary to cut the post to length using a separating disk (Figure 14). A total-etch, dual-cure adhesive/dual-cure composite-resin cementation technique was used to place the translucent fiber post (Figure 15). The tooth was then prepared with an adequate ferrule design to receive a porcelain-metal crown (Figure 16).
Discussion
Fiber-reinforced composite posts are indicated when restoring endodontically treated teeth to provide retention of the core and for root reinforcement.26,42-45 Although they do not have the rigidity of a metal post, fiber posts are indicated for: cases where a metal post would jeopardize the esthetic result; at-risk patients who have a past history of trauma to the orofacial region and the placement of a metal post would put an endodontically treated tooth at risk of root fracture; teeth with sufficient remaining coronal structure so that a 1.5-mm to 2-mm ferrule can be developed in the crown preparation; and teeth that have large root canals where additional intraradicular reinforcement of the canal would be beneficial.
Evidence for the clinical success of fiber posts when restoring endodontically treated teeth has been reported. Mannocci and co-workers64 compared restoring endodontically treated premolars with fiber posts and composite resin cores to restorations of premolars with amalgam. Treating 109 premolars, at the 5-year recall they found that restorations with fiber posts and composite were found to be more effective than amalgam in preventing root fractures but less effective in preventing secondary caries. Malferrari65 restored 180 endodontically treated teeth using fiber posts with a composite-resin core and, subsequently, all-ceramic crowns. At the 30-month recall, 1.7% of the restorations had failed due to the crown but no post, core, or root fracture was recorded.
Other clinical studies have duplicated these results and demonstrated clinical success in restoring endodontically treated teeth with fiber posts.10,27,66,67 Naumann and coworkers68 evaluated risk factors for failure of glass-fiber reinforced composite post restorations, and reported that in recalled cases restored with a resin-adhesive cemented fiber post and a composite-resin core followed by a full-crown restoration, higher failure rates were found in anterior teeth than posterior teeth, in teeth with no proximal contacts than in teeth with at least one proximal contact, and in teeth restored with single crowns compared with fixed partial dentures (FPDs). Their conclusion was that tooth type, final restoration type, and the presence of adjacent teeth were found to be significant predictors of failure rates in endodontically treated teeth restored with glass-fiber reinforced endodontic posts.
In recent years, other fiber-based restorative materials have been described for restoring endodontically treated teeth. One of the first fiber-based materials used to restore endodontically treated teeth was woven fiber ribbons that were originally used for periodontal splinting and direct-placement FPDs using an adhesive/composite-resin technique.26,69,70 Products in this family of materials that have been described for use in the root canal for retaining a core and for root reinforcement include Ribbond® (Ribbond, Seattle, WA) and Connect™ (KerrLab, Orange, CA). Another innovation combining the endodontic filling and post as an intregral unit is the FibreFill® Endodontic Obturation System (Pentron Clinical Technologies, LLC, Wallingford, CT). FibreFill consists of a single "master cone" fabricated from glass fibers in a resin matrix connected to gutta-percha so that the obturation of the canal and placement of a fiber post is accomplished in a single step. The cementing medium is a self-adhesive, thermoplastic, synthetic-resin polymer (Resilon®/Epiphany®, Pentron) that has been shown to be equivalent to conventional endodontic sealers.71 Most recently, a brush-like post system (SpirapostPFS™, Zenith/DMG, Englewood, NJ) fabricated from surgical stainless-steel wires twisted around biocompatible natural-color polyfiber strands was introduced (Figure 17A and Figure 17B). The design of this system allows for a self-centering placement in both straight and curved canals and, when combined with a composite-resin cement, reinforcement of the tooth and composite. It is an intriguing design that needs further evaluation.
Conclusion
Fiber posts have a definite place in a restorative dentist’s armamentarium. To achieve good clinical success, the clinician must choose the clinical circumstances where a fiber post is indicated, choose compatible materials and techniques for cementation, and be assured that the crown preparation for the tooth has an adequate ferrule. By understanding the concepts for clinical success with fiber posts as described in this article, the clinician can provide their patients with esthetic, long-lasting, successful restorations.
Image Credits
* Dentistry in Figure 8 through Figure 11 by Dr. James Braun of Saginaw, MI.
** Figure 12 through Figure 16 provided courtesy of Bisco.
*** Dentistry in Figure 17A by Dr. Howard Glazer of Fort Lee, NJ.
References
1. Johnson JK, Schwartz NL, Blackwell RT. Evaluation and restoration of endodontically treated posterior teeth. J Am Dent Assoc. 1976;93(3):597-605.
2. Fauchard P. The Surgeon Dentist Vol II. 2nd ed. Birmingham, Alabama. (Reprinted by the Classics of Dentistry Library.) 1980;173-204.
3. Rosenstiel SF. Restoration of the endodontically treated tooth. In: Contemporary Fixed Prosthodontics. Rosenstiel, Land, Fujimoto, eds. Elsevier-Mosby, 2006;272- 306.
4. Peroz I, Blankenstein F, Lange KP, et al. Restoring endodontically treated teeth with posts and cores: a review. Quintessence Int. 2005;36(9):737-746.
5. Standlee JP, Caputo AA. Effect of surface design on retention of dowels cemented with a resin. J Prosthet Dent. 1993;70(5):403-405.
6. Sorensen JA, Martinoff JT. Clinically significant factors in dowel design. J Prosthet Dent. 1984;52(1):28-35.
7. Standlee JP Caputo AA, Hansen EC. Retention of endodontic dowels: effects of cement, dowel length, diameter, and design. J Prosthet Dent. 1978; 39(4):400-405.
8. Strassler HE, Simon R, Hiatt H, et al. Using an esthetic post to restore and reinforce a maxillary incisor. Contemporary Esthetics and Restorative Practice. 2000;4(2):36-44.
9. Qualtrough AJ, Mannocci F. Tooth-colored post systems: a review. Oper Dent. 2003;28(1):86-91.
10. Ferrari M, Vichi A, Mannocci F, et al. Retrospective study of the clinical performance of fiber posts. Am J Dent. 2000;13(Special Issue):9B-13B.
11. Pitel ML, Hicks NL. Evolving technology in endodontic posts. Compend Contin Educ Dent. 2003;24(1):13-29.
12. Brown PL, Hicks NL. Rehabilitation of endodontically treated teeth using the radiopaque fiber post. Compend Contin Educ Dent. 2003;24(1):275-284.
13. Godder B, Zhukovsky L, Bivona PL, et al. Rehabilitation of thin-walled roots with light activated composite resin: a case report. Compendium. 1994;15(1):52-57.
14. Takeda T, Ishigami K, Shimada A, et al. A study of discoloration of the gingiva by artificial crowns. Int J Prosthodont. 1996;9(2):197-202.
15. Sidoli GE, King PA, Setchell DJ. An in vitro evaluation of a carbon fiber-based post and core system. J Prosthet Dent. 1997;78(1):5-9.
16. Ferrari M, Cagidiaco M, Vichi A, et al. Retrospective clinical study of fiber post restorations over 7-11 years. J Dent Res. 2006; (Special Issue B). Abstract #79.
17. Strassler HE, Cloutier PC. A new fiber post for esthetic dentistry. Compend Contin Educ Dent. 2003;24(10):742-748.
18. Desai S. Principles and technique of using bonded post and cores. Compend Contin Educ Dent. 2006;27:439-445.
19. Dallari A, Rovatti L, Dallari B, et al. Translucent quartz-fiber post luted in vivo with self-curing composite cement: case report and microscopic examination at a two-year clinical follow-up. J Adhes Dent. 2006;8(3):189-195.
20. Maccari PC, Conceicao EN, Nunes MF. Fracture resistance of endodontically treated teeth restored with three different prefabricated esthetic posts. J Esthet Restor Dent. 2003;15(1):25-31.
21. Qualtrough AJE, Chandler NP, Purton DG. A comparison of the retention of tooth-colored posts. Quintessence Int. 2003;34(3):199-201.
22. Libman WJ, Nicholls JI. Load fatigue of teeth restored with cast posts and cores and complete crowns. Int J Prosthodont. 1995;8(2):155-161.
23. Freeman MA, Nicholls JI, Kydd WL, et al. Leakage associated with load fatigue-induced preliminary failure of full crowns placed over three different post and core systems. J Endod. 1998;24(1):26-32.
24. Reeh ES, Messer HH, Douglas WH. Reduction in tooth stiffness as a result of endodontic and restorative procedures. J Endod. 1989;15(11):512-516.
25. Gutmann JL. The dentin-root complex: anatomic and biologic considerations in restoring endodontically treated teeth. J Prosthet Dent. 1992;67(4):458-467.
26. Newman MP, Yaman P, Dennison J, et al. Fracture resistance of endodontically treated teeth restored with composite posts. J Prosthet Dent. 2003;89(4):360-367.
27. Ferrari M, Vichi A, Garcia-Godoy F. Clinical evaluation of fiber-reinforced epoxy resin posts and cast post and core. Am J Dent. 2000;13(Special Issue):15B-18B.
28. Goodacre CJ, Spolnik KJ. The prosthodontic management of endodontically treated teeth: a literature review. Part 1. Success and failure data, treatment concepts. J Prosthodont. 1994;3(4):243-250.
29. Nicholls JI. An engineering approach to the rebuilding of endodontically treated teeth. J Clin Dent. 1988;1:41-44.
30. Mason PN. Bond studies of the composite-fiber post system. Presented at: Symposium on New Developments in Fiber Post Systems, Schaumburg, IL, September 18, 1999.
31. Lui JL. Composite resin reinforcement of flared canals using light-transmitting posts. Quintessence Int. 1994;25(5):313-319.
32. Saupe WA, Gluskin AH, Radke RA Jr. A comparative study of fracture resistance between morphological dowels and cores and a resin-reinforced dowel system in the intraradicular restoration of structurally compromised roots. Quintessence Int. 1996;27(7):483-491.
33. Fokkinga WA, Kreulen CM, Le Bell-Ronnlof AM, et al. In vitro fracture behavior of maxillary premolars with metal crowns and several post and core systems. Eur J Oral Sci. 2006;114(3):250-256.
34. Sorensen JA, Engelman MJ. Ferrule design and fracture resistance of endodontically treated teeth. J Prosthet Dent. 1990;63(5):529-536.
35. Ng CC, Dumbrigue HB, Al-Bayat MI, et al. Influence of remaining coronal tooth structure location on the fracture resistance of restored endodontically treated anterior teeth. J Prosthet Dent. 2006;95(4):290-296.
36. Pereira JR, de Ornelas F, Conti PC, et al. Effect of a crown ferrule on the fracture resistance of endodontically treated teeth restored with prefabricated posts. J Prosthet Dent. 2006;95(1):50-54.
37. Tan PL, Aquilino SA, Gratton DG, et al. In vitro fracture resistance of endodontically treated central incisors with varying ferrule heights and configurations. J Prosthet Dent. 2005;93(4):331-336.
38. Freedman G, Novak IM, Serota KS, et al. Intra-radicular rehabilitation: a clinical approach. Pract Periodontics Aesthet Dent. 1994;6(5)33-39.
39. Bassi M. Light diffusion through double taper quartz-epoxy fiber posts. Proceedings from the 5th International Symposium. 2001;21-26.
40. ADA Professional Product Review. Endodontic Posts. Publication of ADA Council on Scientific Affairs. Spring 2006;1:1-4.
41. Patyk A, Friedrich M. Translucency of glass-fiber-reinforced resin posts. J Dent Res. 2004;(Special Issue A) Abstract #1784.
42. Kurtz JS, Perdigao J, Geraldeli S, et al. Bond strengths of tooth colored posts. Effect of sealer, dentin adhesive, and root region. Am J Dent. 2003;16:31A-36A.
43. KPilo R, Cardash HS, Levein E, et al. Effect of core stiffness on the in vitro fracture of crowned, endodontically treated teeth. J Prosthet Dent. 2002;88(3):302-306.
44. Salameh Z, Sorrentino R, Papacchini F, et al. Fracture resistance and failure patterns of endodontically treated mandibular molars restored using resin composite with or without translucent glass fiber posts. J Endod. 2006;32(8):752-725.
45. Mannocci, Ferrari M, Watson TF. Intermittent loading of teeth restored using quartz fiber, carbon-quartz fiber, and zirconium dioxide ceramic root canal posts. J Adhes Dent. 1999;1(2):153-158.
46. Braga NM, Alfredo E, Vansan LP, et al. Efficacy of ultrasound in removal of intraradicular posts using different techniques. J Oral Sci. 2005;47(3):117-121.
47. Lindemann M, Yaman P, Dennison JB, et al. Comparison of the efficiency and effectiveness of various techniques for removal of fiber posts. J Endod. 2005;31(7):520-522.
48. Gesi A, Magnolfi S, Goracci C, et al. Comparison of two techniques for removing fiber posts. J Endod. 2003;29(9):580-582.
49. Finger WJ, Ahistrand MW, Fritz UB. Radiopacity of fiber-reinforced resin posts. Am J Dent. 2002;15(2):81-84.
50. Soares CJ, Mitsui FH, Neto FH, et al. Radiodensity evaluation of seven root post systems. Am J Dent. 2005;18(1):57-80.
51. Millstein PL, Nathanson D. Effect of eugenol and eugenol cements on cured composite resin. J Prosthet Dent. 1983;50(2):211-215.
52. Dilts WE, Miller RC, Miranda FJ, et al. Effect of zinc oxide-eugenol on shear bond strengths of selected core/cement combinations. J Prosthet Dent. 1986;55(2):206-208.
53. Tjan AHL, Nemetz H. Effect of eugenol-containing endodontic sealer on retention of prefabricated posts luted with an adhesive composite resin cement. Quintessence Int. 1992;23(12):839-844.
54. Tay FR, Pashley DH, Peters MC. Adhesive permeability affects composite coupling to dentin treated with a self-etch adhesive. Oper Dent. 2003;28(5):610-621.
55. Hillam R, Pasciuta M, Cobb D. Shear bond strength of primer/adhesives with proprietary dual cure resin cement. J Dent Res. 2002;81(Special Issue A):A-72, Abstract #369.
56. Pasciuta M, Cobb D, Denehy G. Shear bond strength of dual cure primer/adhesives with dual cure resin cements. J Dent Res. 2002;81(Special Issue A): A-76. Abstract #405.
57. Christensen G. Self-etch primer (SEP) adhesives update. CRA Newsletter. 2003;27(11/12):1-5.
58. King N, Tay F, Pashley DH, et al. Incompatibility profiles of all-in-one adhesives. J Dent Res. 2004;83(Special Issue A). Abstract #23.
59. Brown PL, Schiltz-Taing M, Sharp, HJ et al. Microtensile strength of adhesives using indirect and direct composites. J Dent Res. 83(Special Issue A). Abstract #1526.
60. Felix CA, Price RB. Effect of distance on power density from curing lights. J Dent Res. 2006;85(Special Issue B). Abstract #2468.
61. Strassler HE, Coletti P, Hutter J. Composite polymerization within simulated root canals using light transmitting posts. J Dent Res. 1997;76(Special Issue):82. Abstract #551.
62. Bitter K, Meyer-Lueckel H, Priehn K, et al. Effects of luting agent and thermocycling on bond strengths to root canal dentine. Int Endod J. 2006;39(10):809-818.
63. Naumann M, Preuss A, Frankenberger R. Load capacity of excessively flared teeth restored with fiber-reinforced composite post and all-ceramic crowns. Oper Dent. 2006;31(6):699-704.
64. Mannocci F, Qualtrough AJ, Wrothington HV, et al. Randomized clinical comparison of endodontically treated teeth restored with amalgam or with fiber posts and resin composite: five-year results. Oper Dent. 2005;30(1):9-15.
65. Malferrari S, Monaco C, Scotti R. Clinical evaluation of teeth restored with quartz fiber-reinforced epoxy resin posts. Int J Prosthod. 2003;16(1):39-44.
66. Monticelli F, Grandini S, Goracci C, et al. Clinical behavior of translucent-fiber posts: a 2-year prospective study. Int J Prosthod. 2003;16(6):593-596.
67. Fredriksson M, Astback J, Pamenius M, et al. A retrospective study of 236 patients with teeth restored with carbon fiber-reinforced epoxy resin posts. J Prosthet Dent. 1998;80(2):151-157.
68. Namann M, Blankenstein F, Kiessling S, et al. Risk factors for failure of glass fiber-reinforced composite post restorations: a prospective observational clinical study. Eur J Oral Sci. 2005;113(6):1-6.
69. Deliperi S, Bardwell DN, Coiana C. Reconstruction of devital teeth using direct fiber-reinforced composite resins: a case report. J Adhes Dent. 2005;7(2):165-171.
70. Vitale MC, Caprioglio C, Martignone A, et al. Combined technique with polyethylene fibers and composite resins in restoration of traumatized anterior teeth. Dent Traumatol. 2004;20(3):172-177.
71. Maltezos C, Glickman GN, Ezzo P, et al. Comparison of the sealing of Resilon, Pro Root MTA, and Super-EBA as root-end filling materials: a bacterial leakage study. J Endod. 2006;32(4):324-327.
About the Author
Howard E. Strassler, DMD
Professor and Director of Operative Dentistry
Department of Endodontics, Prosthodontics,and Operative Dentistry
University of Maryland Dental School
Baltimore, Maryland