Controlling Tooth Reduction and the Bonded Mock-up: Part 1
Esthetic dental restorations, whether porcelain veneers, all-ceramic restorations, or esthetic metal ceramics, have a specific space requirement for ideal esthetics. Understanding the individual esthetic materials requirements for esthetics and long-term durability is paramount for restorative success. Controlling the amount of tooth reduction for any given type of restoration has been historically problematic, with either over- or under-reduced preparations being impressioned and sent to the laboratory. Students and practicing dentists have demonstrated it to be very difficult to judge the amount of tooth structure removal and preparation taper.
Many techniques to control reduction have been discussed, from using depth cuts, a clear matrix to “see through” and judge the amount of space available, to relining shell provisionals with acrylic on the prepared teeth and then measuring space. All of these techniques are problematic. Clear, see-through matrixes are easily distorted and can be of varying thicknesses depending on the amount of heat and suction used to create them. The distortion caused just by removing them from the cast after fabrication prevents accurate seating during the preparation appointment. These should only be used to judge “gross” reduction during full-crown preparations. Relining shell temporaries with acrylic and then measuring the facial thickness to see if enough esthetic space is available is overly time consuming and has the potential problem of locking into undercuts, making temporary removal difficult.
Using depth cuts can be a very accurate way to remove specific amounts of tooth structure. The problem with this technique is that depth cuts are only useful if, once you remove a specified amount of tooth structure (ie, 0.7 mm for a porcelain veneer), you replace or “restore” that 0.7 mm, as the 0.7-mm depth cut is your only reference. This does not take into account the final 3-dimensional (3-D) form and positioning at which the tooth needs to end up. This is really a smile design issue, as the esthetic position of the teeth needs to be predetermined prior to a bur ever touching the tooth. What is needed is some method to design the smile, get the patient’s esthetic acceptance, and ideally try the new design out functionally to see if the patient will adapt to it, before a bur ever touches the tooth.
The Bonded Mock-Up
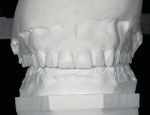
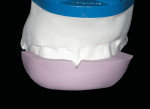
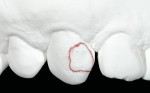
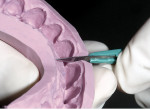
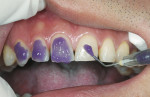
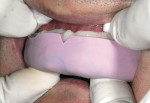
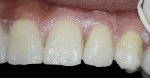
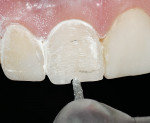
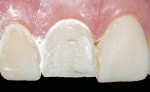
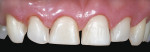
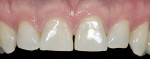
A smile design wax-up is completed based on the patient’s esthetic desires and functional needs(Figure 1). A matrix is made with lab putty(Figure 2) and tried in the mouth to verify complete seating. Many times in an esthetic design there are additive components to the design (ie, the teeth are being built up) but there are also subtractive parts of the design (eg, a line angle is being brought back lingually). If there was stone removed on the cast to reshape the teeth esthetically then similar amounts of tooth structure need to be removed by esthetic tooth recontouring to be able to seat the matrix, allowing for the subtractive design done on the preoperative casts (Figure 3). A notch is cut into the matrix in the frenum area to allow visualization of proper and complete seating(Figure 4).
Bonded mock-ups can be done with either composite or bis-Acryl temporary materials. For longer-term stabilization (more than 3 months) the bonded mock-up should be done with composite. Using bis-Acryl is much simpler than conventional composite. It has the disadvantage of much higher wear potential than composite and should only be used short term.
Generally, cotton roll isolation is adequate for these procedures as long-term bonding is not necessary or even desirable since in a short time the mock-up will be removed. The teeth are then etched with 32% or 37% phosphoric acid. It is extremely important to only etch a specific area. The etching pattern should cover the facial only (for veneers that are facial incisal veneers) and etch to 1 mm to 2 mm short of the anticipated final veneer margin. Do not etch the marginal area(Figure 5) because during the preparation appointment, when preparing the marginal area (finish line), this area of bis-Acryl will easily flake off, facilitating margin placement. Also, if this area has been etched and bonded to with bis-Acryl there is the potential of leaving small amounts at the final margin preparation, possibly affecting long-term marginal seal. After 20 to 30 seconds, the etching material is rinsed with copious amounts of water. The surface of the teeth is air-dried; since most of the time this procedure is done to enamel, over-drying is not a problem. The author uses a primer and adhesive combination on the whole surface of the tooth, even the unetched areas (Figure 6). This will create a minimal seal on unetched areas to help prevent leakage and staining at the margins during the trial restoration phase. The primer/adhesive is air-thinned and then light-polymerized(Figure 7). Bis-Acryl is then loaded into the matrix. The tip of the syringe should be placed in contact with the incisal edge or deepest area of the matrix(Figure 8) and slowly back-filled. This will minimize the chance of trapping air bubbles. An amount slightly more than is anticipated to be necessary in order to not have any voids should be placed in the matrix. The matrix is then completely seated in the mouth(Figure 9).
Once the matrix is seated the material is allowed to set until it reaches a rubbery or doughy stage. The excess material beyond the edge of the matrix is easily removed at this stage with an instrument(Figure 10). The material is allowed to set fully and the matrix is removed. If the matrix fits well there should only be a thin “flash” of material beyond the anticipated veneer margins(Figure 11). Any excess material is trimmed with composite trimming carbides(Figure 12). It is recommended to use carbides that have a round tip, as there is minimal chance to damage tooth structure. It is important to open up the gingival embrasure to ensure that the patient can floss in these regions as the mock-up is left splinted together. Occlusion is adjusted in centric and all excursive movements. It is not recommended to have the patient wear an occlusal splint at this point, as one of the goals of this phase of treatment is to see if the patient will adapt functionally to the proposed anatomical changes. The mock-up can then be adjusted as necessary for esthetic requirements. If additional material is needed then a bonding agent is applied to the area and flowable composite is built up freehand to the desired shape and cured. The patient wears this until esthetic and functional acceptance is obtained and has held up quite well for several weeks(Figure 13). This technique has proven to be a great patient motivator to accept proposed treatment.
Controlling Reduction
Once the smile design has been established and a 3-D model has been mocked up and bonded in the patient’s mouth, it is fairly easy to control reduction. Because the final 3-D positions of the teeth are known, depth cuts become useful and practical. As stated earlier, the amount of reduction is specific to a material. For bonded porcelain it is possible to fabricate veneers 0.3 mm thick. The thickness of the veneer is based on the desired color change from the color of the prepared tooth.1 For the benefit of illustration a 0.6-mm to 0.7-mm thick veneer is planned.
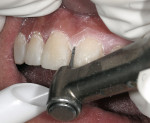
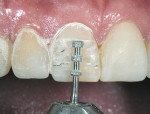
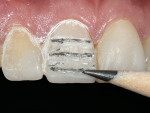
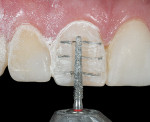
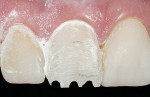
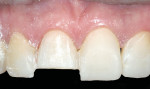
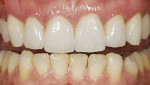
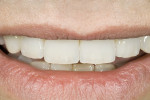
To obtain a relatively uniform preparation of 0.6 mm to 0.7 mm, a depth cutter of slightly less depth is used. This is because once the preparation is finished with fine diamonds it ends up removing 0.1 mm to 0.2 mm more than the depth cutter. For the reduction mentioned, a 0.5-mm depth cutter is used across the facial surface(Figure 14). A simple technique the author uses is to draw pencil lines at the base of the depth cuts(Figure 15). Then, a coarse diamond bur is used to a depth across the whole facial surface up to the depth of the pencil marks (Figure 16). The incisal reduction is done the same way in that a specific sized bur is used to create depth cuts(Figure 17 and Figure 18). The same bur is then used to remove material in between the depth cuts to obtain adequate incisal reduction(Figure 19). At this point the preparation is evaluated for any remaining mock-up material. Many times the preparation is still in the mock-up material. If this is the case, then the remaining mock-up material needs to be removed. With a diamond, lightly prepare down to the bis-Acryl interface. The material near the margin will just flake or fall away as it was not bonded to the tooth. The last step in the process is to place the margin. For conservative veneers the author uses a fine chamfer diamond to place a 0.3-mm to 0.4-mm chamfer finish line(Figure 20). Any sharp line angles, such as the facial incisal line angle, are rounded so as not to concentrate stress in the porcelain restoration. All of the teeth to be prepared could have been done simultaneously using this technique with equal results. Figure 21 demonstates the final preparations of teeth Nos. 5 through 12. Figure 22 is the pre-op condition of the case in this article. The benefit of this technique is conservation of tooth structure. As can be seen in this case, once ideal reduction was obtained, the preparation was still in the bonded mock-up material. Only a minimal amount of tooth structure was actually removed to establish the peripheral margin. With the normal technique of only using depth cuts with no beginning reference, unnecessary tooth structure would have been removed. Figure 23 and Figure 24 are the final bonded porcelain veneers done using the refractory technique.
References
1. McLaren EA. Porcelain veneer preparations: to prep or not to prep. Inside Dentistry. 2006;2(4)76-79.
About the Authors
Edward A. McLaren, DDS
Director
UCLA Center for Esthetic Dentistry
Founder and Director
UCLA Master Dental Ceramist Program
Adjunct Associate Professor
UCLA School of Dentistry
Los Angeles, California
Maggie Bazos
Senior Resident
UCLA Master Dental Ceramist Residency Program
Los Angeles, California