Use of Ceramic Abutments in the Esthetic Zone to Enhance Implant Esthetics
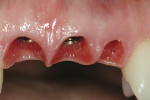
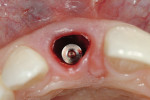
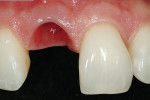
The use of dental implants to replace the natural tooth system in edentulous and/or extraction sites has become commonplace in the contemporary surgical and restorative dental practice.1-5 Advancements in the surgical discipline of implantology have allowed the oral surgeon to place a provisional at the time the implant is placed; this has led to the development of predictable soft-tissue emergence profiles around implant sites, which is especially important in the esthetic zone.6-11 These contours, as seen in Figure 1, lend themselves to not only a natural-looking implant restoration, but one that is periodontally sound for the long term.
To complement the attainability of these esthetic tissue contours, the use of ceramic or zirconia abutments for the final abutment can lead to an even more natural-appearing implant restoration that can support an all-ceramic crown. Additionally, the concept of a tissue-supporting abutment, one that is contoured to provide support for the obtained tissue-emergence profiles that support the esthetics and periodontally sound peri-implant environment, is paramount in the overall esthetics and long-term maintainability of the implant system.12
This article will review a predictable surgical procedure to establish esthetic soft-tissue emergence profile contours, a provisional abutment system, and two abutment options: a ceramic tissue-maintaining abutment and a zirconia tissue-maintaining abutment, which can achieve and maintain esthetic soft-tissue contours in the esthetic zone.
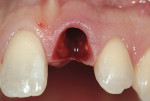
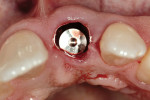
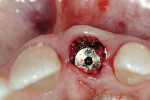
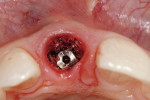
The surgical procedure followed has been well documented in the dental literature.13 In the procedure, after an atraumatic tooth removal (or in an edentulous site) and the creation of an extraction-type of ridge defect(Figure 2), the implant is placed following a flapless surgical approach. This is important to preserve the soft-tissue contours after the extraction, or those created in the edentulous site. The preservation of these contours is the initial step in laying the foundation for esthetics that will be maintained in the final restoration. After the insertion of the implant, any required peri-implant grafting is then accomplished from the flapless bone grafting approach(Figure 3 and Figure 4). This will serve to support the surrounding alveolus, and in the case of a compromised alveolar environment, provide for a contained area in which the graft can be placed. Once this has been accomplished, a plastic provisional abutment is then selected, seated on the implant, and then prepared out of the oral cavity(Figure 5 and Figure 6). The abutment is then placed back on the implant, and either the natural tooth shell or a surgical guide-provisionalization system is retrofitted to serve as the immediate provisional placed at the time of implant placement(Figure 7 and Figure 8). The aforementioned procedure has been well documented in the literature, and has shown that esthetic, supportive soft-tissue contours can be obtained at the initial surgical visit and maintained throughout the healing and integration phase.
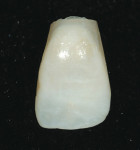
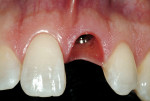
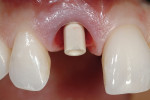
After a prescribed healing phase of 4 to 6 months, the final impression for the derivation of the definitive abutment required will be accomplished. The removal of the immediate provisional restoration(Figure 9) allows for inspection of the final emergence profile contours. This precedes the insertion of the transfer coping. A standard impression is then obtained, and then sent to the laboratory for the creation of either a custom pressed-ceramic abutment(Figure 10) or a CAD/CAM-derived zirconia abutment(Figure 11)
In every restorative case, after implant placement and temporization each remaining step of the laboratory process is critical. Before the impression is taken and sent to the laboratory, the surgeon contours the tissue and develops the profile at the time of surgery. Four to 6 weeks after implant placement, the impression is taken using a heavy body polyvinyl siloxane material to copy the location of the tissue in exact detail.
The impression is poured in the laboratory using die stone after placing the implant replica. A soft-tissue model is not used so that the detail that has already been created intraorally by the surgeon will be preserved. At this time, if additional contouring is needed the changes are made on the stone model before customizing the final abutment. A diagnostic wax-up is done before the final abutment is completed. This wax-up will dictate the angulation and position of the final abutment. The abutment is then cast; prior to pressing, opaque is used to hide the metal. Next, the abutment is seated on the model; wax is added and allowed to flow throughout the tissue profile areas to maintain the tissue contour developed by the surgeon.
The abutment is then ready to be pressed, using the chosen ceramic material in the selected shade. The custom-pressed abutment is then seated on the model and checked for a firm fit. This is one of the most critical steps because it will guarantee no recession of the tissue. The final abutment will maintain the exact profile that the surgeon developed at the provisional stage. If the fit is not exact, there is a possibility of tissue loss over time, provided that poor hygiene is also not a factor.
At this time the abutment can be stained and glazed as needed. A provisional crown is then fabricated using the same diagnostic wax-up used earlier during customization of the abutment. The diagnostic wax-up dictated the proper angulation of the abutment, ensuring that when the provisional and final restorations are fabricated, the restoration will be properly aligned.
In the case presentation that follows, the custom-pressed abutment and provisional were sent to the periodontist, and a final all-ceramic crown was fabricated using Authentic™ Porcelain (Ceramay GmbH + Co KG, Stuttgart, Germany) and sent to the restorative dentist. By treatment planning in this manner, the restorative dentist saved time as well as a client visit by not having to take an impression of the final abutment or having to remove the final abutment and sending it to the laboratory for crown fabrication. Implementing this type of treatment plan allowed the restorative dentist to take photographs and shades before implant placement, which could be sent to the laboratory at the same time the abutment was being fabricated. This offered the dental team the best-case scenario in deciding on the type of crown and materials to use.
The custom pressed abutment was created in an attempt to achieve optimal results in the esthetic zone, in conjunction with an all-ceramic crown. In most clinical cases this technique would allow the practitioner to provide an all-ceramic restoration adjacent to another all-ceramic crown, veneer, or, as in this case, a natural tooth. This technique was the only way to fabricate an all-ceramic crown over an implant abutment before the release of the zirconia abutment by Atlantis Components, Inc (Cambridge, MA).1 With the availability of the zirconia abutment, the esthetic results that have been achieved with the custom press abutment can also be successfully accomplished.
A zirconia abutment is as strong, if not stronger than a titanium abutment.2 When the authors choose to use a zirconia abutment, the impression is sent directly to their own laboratory, not to the implant’s manufacturer. The authors’ laboratory pours and mounts the models, and changes are made on the stone model if the emergence profile needs to be altered. To ensure accuracy, a diagnostic wax-up is done to dictate the position of the final restoration and correct position of the abutment.
This particular case was sent to Atlantis; the model and wax-up were both scanned in order to create the abutment. When sending a case directly to Atlantis , the authors receive back an e-mailed file that contains 3-dimensional images of the model, diagnostic wax-up, and the abutment in place. If changes need to be made, they can be done at that time. This allows the dentist to maintain control during the development stage of the abutment. After a case is received from Atlantis, the abutment can then be stained as needed and a provisional, a final, or both types of restorations can be fabricated on the final abutment.
A large percentage of the authors’ esthetic-zone abutments are fabricated by Atlantis using its CAD/CAM scanning system. In their opinion, the zirconia abutment offers esthetic properties and a precise fit in regard to the hex and the tissue profile. The final abutment and restoration presents a perfect match next to an adjacent natural tooth, veneer, or all-ceramic crown.
Once the final abutment has been fabricated, the final all-ceramic restoration is then created. The porcelain is custom stained to match the surrounding dentition according to the specific requirements of the patient. When this is completed, the abutment is inserted on the implant, the center screw is torqued to 32 Ncm, and the final restoration is bonded or cemented over the final abutment.
The following case presentation will describe the aforementioned procedure for the treatment of an endodontically failed, maxillary central incisor, with demanding esthetic requirements.
Case Presentation
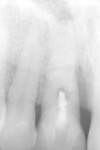
A 36-year-old, non-smoking female presented for treatment of an endodontically failed and periodontically compromised maxillary right central incisor(Figure 12). The preoperative periapical radiograph can be seen in Figure 13. Note the deep vertical bone defect on the mesial of tooth No. 8, which was probing to 10 mm. The decision was made to extract tooth No. 8 and replace the natural tooth system with an implant; the procedure chosen was the immediate extraction, implant placement, and immediate provisionalization procedure, with flapless implant placement and bone-grafting procedures accomplished simultaneously. Additionally, the patient’s pre-existing ceramic restoration would be retrofitted to serve as the immediate postoperative provisional restoration.
After a local anesthetic was administered, a silicone index was obtained by registering the incisal edges of teeth Nos. 7 through 9. The rationale for this step is that when retrofitting the existing porcelain crown to the provisional abutment, the registration of the incisal edge and contact points will allow the retrofitted provisional to be placed in the exact relationship to the adjacent natural teeth as the preoperative position.
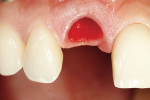
Removal of the porcelain restoration was initially accomplished with a crown remover, followed by an atraumatic tooth removal that preserved the surrounding gingival tissues(Figure 14). After debridement of all remnants of the periodontal ligament and any granulation tissue present, a surgical guide was positioned and the initial coring of the osteotomy site was obtained. A solution of the patient’s own Platelet-Rich Plasma (PRP),14-17 fabricated preoperatively from a 20-mL blood draw, was placed into the osteotomy site and over the implant surface. The implant collar was then placed in relationship to a line drawn from the facial height of contour of the alveolar bone at the left maxillary central incisor. This placement technique is used by the authors on a routine basis in the esthetic zone(Figure 15).18 Before the provisional abutment connection and temporary retrofitting procedure, reconstruction of the lost buccal plate was accomplished.
A full-thickness elevation was accomplished in a flapless method (a tunnel) and performed at the buccal free gingival margin of the edentulous tooth No. 8 site between the periosteum and facial buccal plate. This procedure allows for tactile inspection of the buccal plate to determine any facial dehiscence or fenestrations that require treatment, and the creation of a contained pouch into which grafting material can be placed to reconstruct any dehiscence or fenestrations present. After this tunnel was created the cover screw was placed over the implant and the defect on the facial aspect of the implant between its surface and the buccal plate was evaluated(Figure 16). Using a specially designed elevator/condenser, a graft complex (PRP-enhanced Puros grafting material [Tutogen Medical, Alachua, FL) was condensed between the implant surface and the buccal plate, as well as between the buccal plate and periosteum(Figure 17). Once this was accomplished, the PRP was then placed over the surgical site while the provisional connection procedure was being completed outside of the mouth.
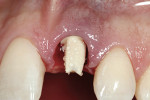
Removal of the healing screw preceded the placement of the plastic provisional abutment (HLPT-3, Zimmer Dental, Carlsbad, CA) for inspection and preparation in relationship to the mesial and distal aspects of the site, and occlusally in relationship to the mandibular arch(Figure 18). Once the abutment had been prepared out of the mouth, it was re-inserted on the implant and the central screw was hand-tightened. The pre-existing porcelain shell was then filled with composite material, placed into the silicone registration (obtained preoperatively), placed over the provisional abutment, and light-cured. Then the retrofitted provisional and provisional abutment were removed and placed on an analogue. This allows for the correction of the margins between the provisional restoration and the provisional abutment, which usually cannot be registered because of the surrounding gingival tissue and must be accomplished chairside. The provisional complex was then reshaped with polishing discs. After these procedures were completed, the provisional abutment was then placed back into the implant, the screw hand-tightened, and the retrofitted pre-existing porcelain restoration cemented to the provisional abutment with strong temporary cement. The immediate postoperative clinical view can be seen in Figure 19, and the immediate postoperative digital radiograph can be seen in Figure 20. Note how the gingival emergence profiles have been maintained throughout the surgical procedure.
At the 1-month postoperative visit, the provisional abutment/temporary complex was removed for impression techniques needed to fabricate the final abutment and a tissue-sculpting provisional restoration. The obtained tissue contours can be seen in Figure 21. Note the sculpted emergence profile of the soft tissues maintained from the preoperative levels throughout the surgical phase, and the initial postoperative phase as well. Routine implant impression techniques were then completed and the impressions forwarded to the laboratory. Following the procedure outlined earlier in the text for a custom-made all-ceramic abutment, the abutment was fabricated along with a new provisional restoration that would continue to sculpt and maintain the soft-tissue environment of the free gingival margin.
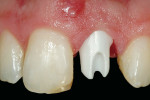
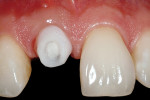
Two months after implant placement, the initial provisional/abutment complex was removed, the final custom pressed-ceramic abutment was inserted, and the center screw-tightened to 30 Ncm(Figure 22). Note how the custom abutment follows and supports the soft-tissue emergence profiles obtained and maintained from the time of the extraction. This abutment design has been observed clinically in the authors’ practices to maintain the soft-tissue emergence profile and papillary contours on a long-term basis. The tissue-maintaining provisional was once again cemented with temporary cement(Figure 23). Three months postoperatively, the restorative clinician took the final impression of the abutment and soft-tissue relationships for the creation of the all-ceramic final implant-supported restoration.
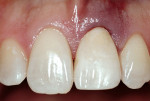
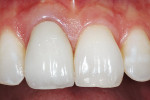
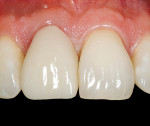
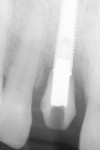
The case’s complete clinical view can be seen in Figure 24, and the case’s complete digital periapical radiograph can be seen in Figure 25. Note how not only the soft-tissue contours have been maintained throughout the entire implant process, but the bone levels as well. Compare Figure 25 to the preoperative radiograph (Figure 13). The defect present on the mesial of tooth No. 8 has been corrected, and the interdental bone contours preserved.
Conclusion
Enhancement of the natural dentition is routine in the contemporary dental practice with the use of dental whitening systems and the various veneer options available to patients seeking to change their smile appearance. When the necessity for tooth replacement is required, consideration must be given to the esthetic requirements of the patient. With the availability of new surgical options, the preservation of pre-existing soft-tissue emergence profiles can be accomplished or, in many situations, created where they did not exist. In cases where the final esthetics are paramount, custom-made ceramic and/or CAD/CAM-derived zirconia abutments can be used to sculpt and maintain soft-tissue contours, to increase the esthetics of the final implant-supported restoration, and, often, form a stronger bone between the abutment and crown complex.
The authors advocate the use of CAD/CAM-derived zirconia abutments in the esthetic zone and anterior sextants of the maxillary and mandibular arches, extending the second premolar regions in many cases. In the molar regions, because of the heavy forces of occlusion, the authors advocate the use of either custom-made gold or milled titanium abutments, which are routinely used to support a ceramic-metallic full-coverage restoration.
Disclosure
The author has received financial support from Zimmer Dental.
References
1. Kois JC. Altering gingival levels: The restorative connections. Part 1: Biological variables. J Esthet Dent. 1994;6: 3-9.
2. Spear FM. Maintenance of the interdental papilla following anterior tooth removal. Pract Periodontics Aesthet Dent. 1999;11(1): 21-28.
3. Garber DA, Belser UC. Restoration-driven implant placement with restoration- generated site development. Compend Contin Educ Dent. 1995;16(8):796-804.
4. Grunder U, Spielman HP, Gaberthuel T. Implant-supported single tooth replacement in the esthetic region a complex challenge. Pract Periodontics Aesthet Dent. 1996;8(9):835-842.
5. Touati B. Improving esthetics of implant-supported restorations. Pract Periodontics Aesthet Dent. 1995;7(9):81-92.
6. Saadoun AP. Single tooth implant restorations: surgical management for esthetic results. Int J Dent Symp. 1995;3(1):30-35.
7. Saadoun AP, Le Gall MG. Periodontal implications in implant treatment planning for esthetic results. Pract Periodontics Aesthet Dent. 1998;10(5):655-664.
8. Salama H, Salama M. The role of orthodontic extrusive remodeling in the enhancement of soft and hard tissue profiles prior to implant placement: a systematic approach to the management of extraction site defects. Int J Periodontics Restorative Dent. 1993;13(4):312-333.
9. Petrungaro PS. Immediate restoration of implants utilizing a flapless approach to preserve interdental tissue contours. Pract Proced Aesthet Dent. 2005;17(2): 151-158.
10. Kan JY, Rungcharassaeng K. Immediate placement and provisionalization of maxillary anterior single implants: a surgical and prosthetic rationale. Pract Periodontics Aesthet Dent. 2000;12(9):817-824.
11. Petrungaro PS. Immediate implant placement and provisionalization in edentulous, extraction, and sinus grafted sites. Compend Contin Educ Dent. 2003; 24(2):95-113.
12. Petrungaro PS. Replacing the natural tooth system in the esthetic zone: Flapless implant placement and simultaneous restoration to preserve tissue contours and guarantee esthetics. Inside Dentistry. 2005;1(2):76-78.
13. Petrungaro PS. Implant placement and provisionalization in extraction, edentulous and sinus grafted sites: A clinical report on 1500 sites. Compend Contin Educ Dent. 2005;26(12): 879-890.
14. Petrungaro P. Platelet-rich plasma for dental implants and soft-tissue grafting. Interview by Arun K. Garg. Dent Implantol Update. 2001;11(6):41-46.
15. Petrungaro PS. Using platelet-rich plasma to accelerate soft tissue maturation in esthetic periodontal surgery. Compend Contin Educ Dent. 2001;22(9):729-746.
16. Marx RE, Garg AK. Bone graft physiology with use of PRP and hyperbaric oxygen. In: Jensen OT, ed. The Sinus Bone Grafts. Chicago, IL: Quintessence Pub.Co; 1999.
17. Anitua E. Plasma rich in growth factors: preliminary results of use in the preparation of future sites for implants. Int J Oral Maxillofac Implants. 1999; 14(4): 529-535.
About the Authors
Paul S. Petrungaro, DDS, MS
Director
The Institute for Advanced Dental
Education, Inc
Lake Elmo,Minnesota
Michael D. Smilanich, DDS
The Institute for Advanced Dental
Education, Inc
Lake Elmo,Minnesota
Edgar Jimenez, CDT
The Institute for Advanced Dental
Education, Inc
Lake Elmo,Minnesota