Remineralization with a Unique Delivery System
Robert C. Margeas, DDS
For the caries process to begin, a series of demineralization/remineralization events involving enamel and dentin must be at work. The process is initiated with the dissolution of tooth mineral (demineralization) by organic acids (lactic and acetic) produced by the action of plaque bacteria on dietary carbohydrates.1
If the demineralization process predominates, this carious lesion progresses to form a cavity. Remineralization (deposition of tooth mineral) can repair or arrest the caries lesion if caught in a timely manner. This can prevent cavity formation and the need to restore the tooth with a restoration.2
Teeth need calcium, phosphate, and fluoride. Healthy saliva contains these minerals and, in conjunction with certain salivary proteins, is able to deliver bio-available calcium and phosphate to the tooth surface during the demineralization/remineralization process, which neutralizes the acid produced by dental plaque, promoting remineralization. Unhealthy saliva or lack of saliva, as in xerostomia, reduces the clearance of bacteria and food from the mouth. The reduced buffering of acid and a diminished ability to remineralize the enamel puts the patient at greater risk of tooth decay. How do we know if the patient’s saliva is adequate to buffer the acid attacks? Saliva-Check is innovative saliva analysis tool (GC America, Inc, Alsip, IL), which helps detect possible problems in a patient’s saliva that can lead to demineralization and caries. Saliva-Check evaluates hydration, salivary consistency, resting pH, stimulated salivary flow, stimulated pH, and saliva buffering capacity.
Numerous strategies for caries treatment have focused on minimizing bacterial growth, neutralizing the acids formed, and using remineralizing agents. Reynolds and colleagues at the University of Melbourne investigated the anticariogenic properties of milk products in the early 1980s. They identified the role of casein phosphopeptides (CPP) in the stabilization and localization of amorphous calcium phosphate (ACP) at the tooth surface. More recently, they have shown that CPP-ACP can repair early lesions by promoting subsurface remineralization.3
Cariogenic biofilms thrive in an acidic environment, which is partly created by food and beverage ingestion.4 An acidic environment also can develop if the saliva is of poor quality that is manifested as low pH.5 The Minimum Intervention dentistry concept (MI concept) developed by GC America helps contribute to the improvement of dental health by providing techniques, materials, instruments, equipment, and information for the identification of caries risk, the prevention of caries, and the control of caries.
MI Paste
Recognizing decay at an early stage is critical to making MI dentistry work. MI paste (GC America) is a new product, which is a water-based sugar-free paste containing Recaldent™ (CPP-ACP). When MI paste is applied to tooth surfaces, it binds to biofilms, plaque, bacteria, hydroxyapatite, and the surrounding soft tissues, localizing bio-available calcium and phosphate. The Recaldent (CPP-ACP) technology releases calcium and phosphate when a patient’s saliva is acid-challenged by the normal digestive process. Under optimum circumstances, when fluoride, calcium, and phosphorus are available in the erupting tooth, the mix develops into a tooth that is resistant to all acid challenges.2 It has been shown that fluoride also works better when it is used with calcium and phosphorus.6 Saliva enhances the effectiveness of CPP-ACP. The longer CPP-ACP is maintained in the mouth, the more effective the result. A delicate balance exists between health and disease. It involves acids and bacteria-laden plaque competing with protective factors provided through normal salivary flow and good oral hygiene.
Indications for Use
There are several indications for the use of Prospec™ (Professionally Specified) MI paste (GC America), including postwhitening sensitivity.7 For this application, the protocol is to generously extrude the paste into a custom whitening tray after it has been rinsed out. The paste should be allowed to come in contact with the teeth for 3 minutes. The patient should not rinse the paste away. Instead, he or she should expectorate the remaining paste, which will help seal any exposed dentinal tubules. A prophy cup application can also be used after scaling and root planing to decrease postoperative sensitivity.7 MI paste is not a toothpaste, and should not be applied like toothpaste (ie, teeth should not be brushed with it). MI paste not used in a whitening tray should be applied with a finger and allowed to come in contact with the teeth for 3 to 5 minutes and then expectorated. For maximum benefits, a water rinse after the application is not recommended.
In some situations, MI paste can be used to reverse white spot lesions with orthodontic treatment and fluorosis. In these defects, there are subsurface voids, which can be very effectively remineralized by application of MI paste. This application has been shown effective using optical and also radiographic tests at the University of Melbourne7. Other clinical applications for MI paste include treating dentinal hypersensitivity, treatment of erosion and incipient carious lesions, caries prevention, and promoting fluoride uptake.7
Clinical Case
A patient reported sensitivity after an overnight tooth-whitening treatment. MI paste was recommended to be used in the whitening trays after each session. The MI paste was dispensed in the tray (Figure 1) and placed on the teeth for approximately 5 minutes (Figure 2). The patient did not rinse. After the treatment, the patient informed us that the sensitivity had diminished. This treatment is an option when patients experience sensitivity as a result of tooth whitening.
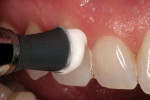
Another indication for the use of MI paste is sensitivity after scaling and root planing or gingival recession causing sensitivity. For these cases, the MI paste is used on a prophy cup (Figure 3) and the patient should not rinse, just expectorate the excess. This application can help tremendously with postoperative sensitivity.
Conclusion
MI paste is a clinically proven preventive tool, which can help dentists treat patients with saliva deficiencies. It is easy to use, buffers plaque acid, and can work as an in-office treatment as well as an at-home follow-up. This new technology has a unique ability to deliver bio-available calcium and phosphate when they are needed most.
References
1. Loesche WJ. Role of Sterptocococcus mutans in human dental decay. Microbiol Rev. 50:353-380, 1986
2. Anusavice KJ. Efficacy of non-surgical management of the initial caries lesion. J Dent Educ. 61:895-905, 1997
3. Reynolds EC. Remineralization of enamel subsurface lesions by casein phosphopeptide-stabililzed calcium phosphate solutions. J Dent Res. 76:1587-1595, 1997
4. Bradshaw DJ, Marsh PD, Hodgson RJ, et al. Effects of glucose and fluoride on competition and metabolism within in vitro dental bacterial communities and biofilms. Caries Res. 2002;36(2):81-86.
5. Sanchez CA, Fernandez D, Preliasco MV. Salivary pH changes during soft drinks consumption in children. Int J Paediatr Dent. 2003;13(4): 251-257.
6. Featherstone JD. The science and practice of caries prevention. J Am Dent Assoc. 2000;131(7):887-889.
7. Reynolds EC, Walsh LJ. Additional aids to the remineralisation of tooth structure. In: Mount GJ, Hume WR eds. Preservation and Restoration of Tooth Structure. 2nd ed. Brighton, Australia: Knowledge Books and Software; 2005: Chapter 8.
About the Author
Robert C. Margeas, DDS
Adjunct Professor
University of Iowa College of Dentistry
Department of Operative Dentistry
Iowa City, Iowa
Private Practice
Des Moines, Iowa