Porcelain Veneer Preparations: To Prep or Not to Prep
Edward A. McLaren, DDS, MDC
In recent years, bonded porcelain restorations have geometrically expanded in their clinical use. Increased patient demands for esthetics coupled with the desire by the profession for conservative treatments have fueled this expansion. Early concerns about the fragile nature of the thin shells of ceramic have been allayed as multiple clinical reports have documented good to excellent clinical success. Because of this documented success, porcelain veneers have been used for more restorative situations and not for just esthetic enhancement. One exhaustive study that followed veneers for up to 15 years reported total failures of only 7%, equaling approximately a 1% chance of failure per year.1 Of the reported failures, more than half were fractures. Several other reports documenting the success or failure of porcelain veneers cite margin placement and whether or not the margins were placed in enamel as the primary causes of failure.
Bonding mechanisms and materials have improved over the years with bonding failure minimized because of these improvements. The main mode of failure with bonded porcelain is fracture and bond failure, which are interrelated. Many different causes can contribute to ceramic failure, including preparation design and proper tooth reduction. Confusion exists over the many different preparation designs, specifically whether or not to remove tooth structure, how much tooth structure to remove, and margin design and placement. This article is intended to give rational guidelines on preparation parameters for porcelain veneers, particularly the issue of “to prep or not to prep” and, if prepping, “how much.”
The ultimate goal in any dental treatment should be to be as conservative as possible to obtain the desired result. The same is true for bonded porcelain (porcelain veneers). Ideally, none or only a minimal amount of tooth structure should be removed. One decision that always needs to be considered is whether adjunctive orthodontics should be completed to place the teeth in the ideal position so that there is minimal or no reduction for bonded porcelain. In the authors’ experience, if the teeth require bonded porcelain anyway for reasons of form correction, color alteration, or replacement of failed restorations, and the amount of healthy tooth structure removal will be similar even if orthodontics is done, then bonded porcelain without adjunctive orthodontics should be accomplished. But if orthodontics significantly reduces the need for healthy tooth structure removal, specifically, if the preparation has to cross the dentinoenamel junction, then orthodontics should be completed.
Preparation Guidelines for Porcelain Veneers
Preparations are always dictated 3-dimensionally by how the final restoration is placed within the frame of the face, lips, and gingiva. This is determined by smile design with patient input and needs to be verified functionally. The clinician should work backward and remove tooth structure based on the specific material requirements for space (ie, thickness of the restorative material).
In the case of a translucent material such as a porcelain veneer, the desired color or shade change needs to be considered. Generally speaking, a veneer requires a minimum of 0.2 mm to (ideally) 0.3 mm of thickness for each shade change. For example, to go from an A3 to A0 requires 3 shade group changes and would need a minimum of a 0.6-mm to (ideally) 0.9-mm-thick veneer. In the laboratory, it is very difficult to fabricate a veneer less than 0.3-mm thick. Research done at the University of California, Los Angeles and the University of Oregon on 0.3-mm-thick veneers showed some cracking on cement polymerization when they wrapped around a corner as in the incisal edge (unpublished data). This data shows the veneers should be slightly thicker (at least 0.5 mm) if they wrap interproximally or over the incisal edge. Veneer thickness, which relates to tooth reduction, is largely determined by the amount of shade change desired and tooth position for esthetics.
To Prep or Not to Prep
It is generally recommended that the margins be placed circumferentially in enamel. Recommendations range from minimal to no preparation to a heavy chamfer. Many of the techniques for margin design and volume of tooth structure removal are dictated by manufacturers’ requirements for a specific material. Although this is acceptable if the clinical situation dictates it, many times this is not the case. Frequently, excessive tooth structure is removed so that a specific material or technique can be used, although another technique or material would have been the more conservative option. The material or technique should not be made to fit the clinical situation but rather the best material or technique should be chosen for the existing clinical situation.
If the porcelain cannot be supported by enamel, it is critical to design the preparation so the cemented veneer is subjected to minimal or no tensile or shear stresses. Laminated structures such as porcelain/enamel or porcelain/dentin by definition are a constant strain system.2 When a stress is applied in such a system, the material with the highest modulus of elasticity (stiffest) absorbs most of the stress. Because dentin is a lower modulus material (more flexible) than porcelain, it flexes more than enamel under a given load, thus subjecting the veneered porcelain to higher tensile and shear stresses. Being brittle, ceramics fail at a critical strain of 0.1%;3therefore, bonding to the more flexible dentin could lead to early failure. The stiffness of enamel and its ability to absorb stress clearly demonstrates the need to save as much enamel as possible and to ideally bond porcelain to enamel rather than dentin.
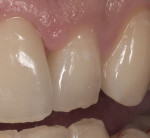
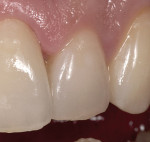
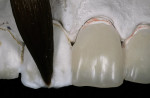
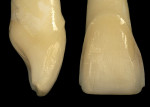
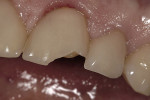
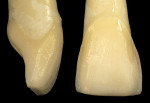
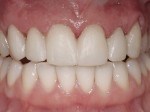
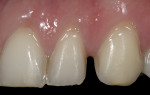
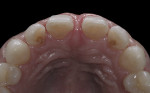
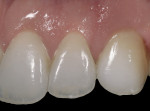
To prevent overcontouring and provide for proper masking, the authors prefer to prepare teeth in the gingival third, and prepare a light chamfer for a definitive finish line. The one exception to this is if the tooth is in slight lingual version and the finish line of the porcelain can be kept supragingivally (Figure 1 and Figure 2). From the laboratory perspective, it is extremely beneficial for the dentist to place at least a light chamfer finish line so the ceramist clearly knows where to build the porcelain. The authors recommend at least a light chamfer of 0.3 mm gingivally and interproximally. If there is peripheral enamel, the authors prefer to prepare the incisal edge to allow for 1 mm to 1.5 mm of incisal porcelain (Figure 3). This creates room to internally build the incisal effects, which are present to varying degrees on natural teeth.
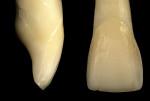
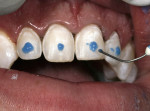
Incisal margin placement has generally followed 2 designs, the incisal wrap (Figure 4 and Figure 5) and the incisal window. The incisal wrap is recommended when there is a change in form and when there is going to be an incisal lengthening. The window preparation is recommended when only color changes are desired. Most ceramists find it difficult to work with the window preparation, as it is problematic to place incisal effects in the porcelain with this design. This incisal wrap creates more room for incisal porcelain, but creates a thin area of porcelain on the lingual that could have higher potential for fracture (Figure 6). If form alteration is one of the treatment goals, the authors prefer the more recent incisal margin placement (incisal shoulder preparation) (Figure 7). In this preparation, instead of wrapping over the lingual edge, the incisal edge is prepared for a shoulder. The facial incisal line angle is rounded slightly to minimize any stress concentration in the ceramic. This is by far the easiest incisal finish line design. In the authors’ clinical experience, there has been no issue with debonding of porcelain veneers with this preparation design, particularly when the veneer is bonded mostly to enamel. The only issue has been the retention of the provisionals (prototypes).To solve this problem, the authors use a small amount of flowable composite interproximally to lock in the veneer along with the spot-etching technique (Figure 8 and Figure 9).
Interproximally, the authors recommend staying slightly labial or facial to the contact area, which conserves interproximal enamel. The exception to this is if a tooth needs to be widened as in the case of a pegged lateral (Figure 10 and Figure 11). The finish line should then be taken more lingually toward the lingual transitional line angle so that the contour of the porcelain can be started from the lingual and be built up to properly close the interproximal space (Figure 12). The case demonstrated in Figure 13A; Figure 13B; Figure 13C; Figure 13D follows the principles of tooth preparation presented in this article. The case was fabricated with Vita VM® 9 porcelain (Vident, Inc, Brea, CA) on refractory dies.
Conclusion
Tooth reduction for any restorative technique should be as conservative as possible, especially for porcelain veneers. The reduction necessary for bonded porcelain is based on smile design and the desired 3-dimensional placement of the final restoration as well as the desired shade change. For porcelain veneers, a porcelain thickness of 0.2 mm to 0.3 mm is needed for each shade change. The authors also recommend at least a light chamfer at the periphery (especially the gingival margin) to prevent overcontouring in this region.
References
1. Freidman MJ. A 15-year review of porcelain veneer failure—a clinician’s observations. Compend Contin Educ Dent. 1998;19(6):625-630.
2. McLean JW. Long-term esthetic dentistry. Paper presented at: The Newport Harbor Academy of Dentistry; May 1993; Newport Beach, Ca.
3. Jones DW. The strength and strengthening mechanisms of dental ceramics. In: McLean JW, ed. Dental Ceramics: Proceedings of the First International Symposium on Ceramics. Chicago: Quintessence; 1983.
About the Author
Edward A. McLaren, DDS, MDC
Director, Center for Esthetic Dentistry
Founder and Director, Master Dental Ceramist Residency Program
Adjunct Associate Professor
The University of California, Los Angeles
School of Dentistry
Private Practice limited to Prosthodontics and Esthetic Dentistry
Los Angeles, California