Solving a Complicated Prosthetic Case
Understand and incorporate a properly prosthetic-driven case plan.
Prosthetic planning for technical procedures should be driven by case design in order to achieve desired expectations for anterior esthetics and functional denture occlusion. For clinical procedures, biology is the main factor that drives treatment planning, although there must be consideration of biomechanical problems arising from the proposed prosthetic case plan. This case illustrates how if the treatment plan is changed—taking biomechanics into consideration—the problems that arise during try-in of the maxillary complete denture and mandibular precision partial should not affect anterior esthetics and functional occlusion.
The case presented represents planning of a full-mouth rehabilitation where many prosthetic variables must be considered and understood to coordinate the proper clinical and technical prosthetic sequence. One part of the prosthetic case conveys the functional implications of improper planning in full-mouth rehabilitation restorative cases and why this reset happened.
The Case
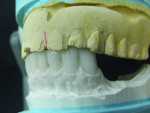
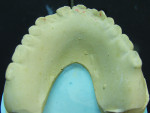
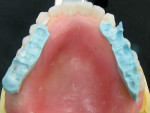
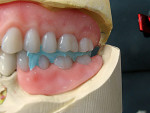
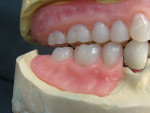
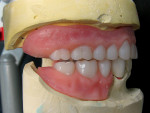
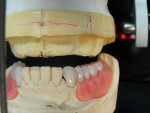
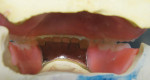
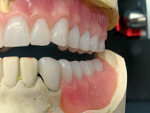
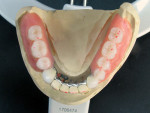
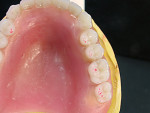
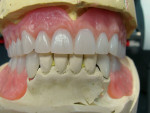
An existing maxillary complete denture with severely worn denture teeth was mounted to a mandibular cast for diagnostic waxing of teeth Nos. 22 through 27. The wax was brought up into Class I occlusion to the maxillary anteriors (Figure 1). An occlusal view of the existing maxillary complete denture shows substantial wear of anterior and posterior denture teeth (Figure 2). The cause of this denture tooth wear is decreased occlusal vertical dimension (OVD) and the incisal edge position of the maxillary anteriors. The loss of incisal and occlusal acrylic on the denture teeth should be a sign that the anterior and posterior teeth need to be slightly lengthened to compensate for wear if the dental technicians are to restore proper esthetics and function.
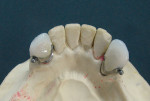
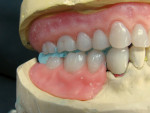
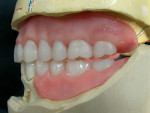
It was clinically decided to restore the mandibular anteriors with ceramic crowns based on the diagnostic wax-up for the temporaries. The patient’s desire was to have a very esthetic mandibular partial that would not show any clasps. The distal abutments on teeth Nos. 22 and 27 were designed to have Sagix attachments (Preat Corporation, www.preat.com) on the distal surfaces with lingual guiding arms (Figure 3).
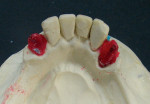
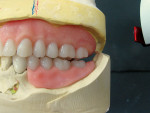
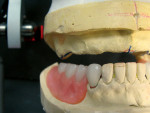
A pick-up impression of the mandibular canines with Sagix attachments was taken, and resin dies were created to have the canines seated on the master cast for design and fabrication of a cast removable partial denture framework (Figure 4). When possible, it is always advisable to have the attachment crowns on the working master cast rather than using transfer impression copings and model analogs. This provides an accurate representation of the attachment position and surface for guiding the partial denture framework.
After the wax try-in of the maxillary was complete and mandibular partial dentures were finished, the prosthetic case was returned to the laboratory with a new occlusal record to remount and reset the denture teeth. As in Figure 5, the buccal and lingual surfaces of the occlusal record should always be trimmed, exposing the buccal cusps of the maxillary and mandibular teeth in relation to one another. This provides a visual seat of the denture teeth during the remounting procedure on the dental articulator (Figure 6 and Figure 7).
The reset came with instructions to raise the maxillary anteriors and increase the curve of Spee for anterior disclusion. After the case was remounted and the occlusal records were removed, the interocclusal space for resetting the posteriors was inspected (Figure 8 through Figure 11). The vertical overlap of maxillary to mandibular anteriors is shown in Figure 10 and Figure 11. The problem with this prosthetic case was becoming obvious, because after the maxillary complete denture was designed, the teeth were then arranged to the mandibular crowns rather than having the crowns fabricated to the maxillary complete denture tooth placement. To prevent anterior guidance and establish a functional denture occlusion, the maxillary complete denture must first be set to ascertain proper incisal surface placement of opposing crowns.
When the maxillary visible light-cured base with waxed denture teeth was removed from the mounted cast, the limited maxillary residual ridge to mandibular occlusal surface space was seen. Note the tuberosity to the mandibular second molar space. If a steeper curve of Spee is desired for anterior disclusion, the mandibular molars must be raised, but they are limited by the posterior opposing anatomy (Figure 12 and Figure 13). As can be seen in the photographs, if the mandibular anterior incisal edges of the crowns were 1 mm shorter, this anterior guidance issue would not be a problem when resetting the denture teeth. The problem became more evident as all function was at this point dictated by the mandibular anterior crowns. Inspecting the interocclusal space from a posterior view shows the lingual occlusal contacts and working space for raising the molars (Figure 14).
The anterior teeth were raised 0.5 mm, and the posteriors were reset to increase the curve of Spee and posterior guidance for discluding anteriors. The esthetic and functional compromise is that by decreasing maxillary anterior functional guidance in excursive movements, anterior esthetics are affected by raising the incisal edges or smile line of the denture teeth.
A functional denture occlusion with a lingualized scheme (Figure 15 through Figure 17) was created to help minimize the anterior guidance problem. Another option would be to set fully anatomical posteriors with a steeper cusp angle to increase posterior guidance and anterior disclusion. As is apparent in Figure 2, which shows the posterior teeth on the existing maxillary denture, a patient could not adapt from an almost flat (0-10 degree) to a revised anatomical (30-40 degree) posterior denture tooth arrangement. A functional compromise was made by using the ortholingual posterior denture tooth setup to help this guidance problem while minimizing occlusal contacts and lateral interferences.
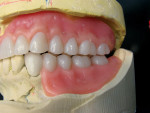
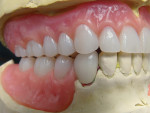
The completed maxillary and mandibular reset shows the position of the denture teeth in relation to the mandibular anterior crowns (Figure 18). If the case had been properly planned, the crowns would be made at this position to the maxillary denture teeth. This would have avoided any anterior guidance problems, and interferences would be worked out during the porcelain design, build-up, and contouring in all excursive movements.
An occlusal view of the mandibular cast with the partial denture in place shows the placement of teeth in relation to the ridge and incisal edge of the canines (Figure 19). The Wironium® (Bego USA, www.begousa.com) cast removable partial denture is adapted well to the lingual surfaces of the crowns. The red markings on the incisal edges show that there is still anterior contact in centric occlusion, which results in a guidance problem due to the length of the crowns. The anterior lingual contacts were adjusted, as seen in Figure 20, to eliminate contact in centric occlusion and help allow a down-forward movement of the mandible in protrusive.
Conclusion
The importance of a properly prosthetic-driven case plan cannot be emphasized enough in order to prevent problems that occur when sequencing clinical or technical procedures with a full-mouth rehabilitation prosthetic combination case. Only one very small part of the technical procedure for this case was discussed in this article, overlooking other variables that caused problems in achieving optimal esthetic and functional results. Too often the fixed restorative portion of a case is given priority and completed first, thus dictating the removable prosthetic design and function. It is the removable prosthetic dental technologist who must control the design and sequence of full-mouth rehabilitation combination cases if dental technicians are to consistently exceed esthetic and functional expectations.
Acknowledgment
The author would like to thank and acknowledge Yulia Gafurov, CDT, who did the technical prosthetic work and discussed this functional denture occlusion problem with him. Yulia received her formal education in dental technology at the Medical College in Almaty, Kazakhstan, and is currently the lead dental technician in the Removable and Implant Prosthetics division for Microdental in Dublin, California.
Case Planning Checklist
Dental technicians must always work as a multidisciplinary team and take an interdisciplinary approach to case planning to achieve optimal prosthetic results. Clinical and technical communication and collaboration are the keys to success in prosthetic dentistry.
Desired prosthesis
Prosthetic options
Mounted study casts
Casts of existing prosthesis
Facial and intraoral photos
Evaluate prosthetic space
Esthetic expectations
Functional occlusion
Evaluate smile line
About the Author
Robert Kreyer, CDT
Director of Removable Prosthodontics
Microdental/DTI
Dublin, California
Yulia Gafurov, CDT
Lead Dental Technician
Removable and Implant Prosthetics
Microdental/DTI
Dublin, California