Implant Placement Planning and Surgical Guide Design
Technician develops a technique to overcome radiographic scatter
Jeffry Tobon, CDT
Planning implant cases has become an increasingly common service that dental laboratories offer as part of their digital workflow. However, there are challenges in the process that require some thought and significant insights to overcome. Among the challenges is capturing the appropriate tomography of the oral environment, including the location of the nerve, density of the bone, and other important landmarks. This is accomplished with the use of a radiographic technology called cone-beam computed tomography (CBCT or CT) scan, which emits low levels of radiation and captures multiple small "slice" views of the patient's anatomy. The aggregate of those slices, called a dicom file, provides the dentist, surgeon, and dental laboratory with all the necessary information to accurately and appropriately plan the execution of implant placement in the bone. The challenge remains when patients present with significant amounts of metal in their mouths in the form of metal-based restorations such as PFMs and other metal restorations. Metallic objects present as irregular spikes on the dicom file of the radiograph. These spikes are called scatter or noise and can oftentimes negatively affect the quality of the scan as well as hide or distort pertinent landmarks in the scan that are necessary to adequately plan implant placement and create a surgical guide. A technique to overcome these challenges is presented in this article, demonstrating how the utilization of CAD software could lead to overcoming these challenges and/or the need for radiographic stents.
The Case
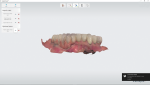
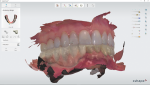
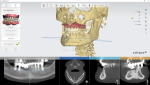
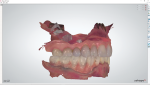
The patient presented with an existing full mandibular arch restored with a porcelain-fused-to-metal restoration (Figure 1). The restorative dentist decided on a treatment protocol that involved replacing the dated restoration by incorporating three implant sites on the mandible for teeth Nos. 26, 27, and 28. Therefore, a surgical guide would need to be designed and fabricated to assure the best implant placement for achieving the optimal restorative outcome. The dentist wanted to utilize his Trios intraoral scanner (3Shape, 3shape.com) to capture a digital impression (Figure 2) and use this data in combination with the CT data (Figure 3) to digitally plan implant placement. The laboratory would design and fabricate the surgical guide.
Scatter or Radiographic Noise
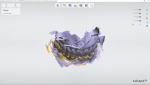
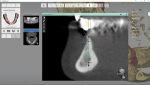
When the case came to the laboratory, the dentist told the author that there was a significant amount of scatter or radiographic noise on the lower-arch CT caused by existing PFM crowns. Distorted CT scan data is a common occurrence when patients have metal in their mouths. The dentist forwarded pre-operative digital impression scans as well as a standalone scan of the lower arch, showing the prepared teeth and abutments (Figure 4). The dicom files with scatter over the entire lower arch were sent to the laboratory by the surgeon (Figure 5). The patient was reappointed for surgery 3 days after the case was sent to the laboratory. The author realized that he needed to find a technique very quickly that would solve the scatter problem, and, if successful, would create a solution that would benefit other dental professionals presented with similar challenges when making tooth-borne guides in the presence of CT scatter or when making similar guides on edentulous arches.
The Digital Solution
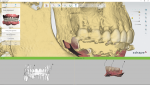
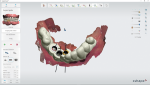
When creating a case digitally using dental laboratory CAD software, the designer needs to stitch or align the digitized model scans together with the bite scan (Figure 6). It doesn't matter if the files of the upper arch and lower arch are separate. They will always come into the "virtual realm" in the same orientation in which they were originally scanned. A critical component of the planning process is having all the pertinent data (scans and dicom files) converge into one usable rendering to virtually place implants with all the necessary information (Figure 7). Following that train of thought, the author identified areas on the dicom scan that were identical to the areas on the digital impression scan, which allowed the designer to align the two data sets. To do so, the designer would need to trick the CAD system to align each of the two scans with the opposite arch.
The technique utilized in this case was to import the upper arch first and the lower arch second. Even though there was scatter on the lower arch scan, it fell exactly in perfect orientation of the patient's vertical dimension (Figure 8). This technique works well as long as both the CT scan and the digital impression scan are taken with the patient in perfect centric occlusion.
An additional useful scan to facilitate fully integrated dicom and surface scans is a pre-op scan. The dentist sent a study model scan of the patient's upper and lower arches in centric occlusion (Figure 9) and also sent a standalone scan of just the lower arch for which the surgical guide must be designed and fabricated. In order to merge all of the imported data into their correct positions, the author used conventional methods to import the case into the 3Shape scan software. However, he "tricked" the system by importing scans in a different sequence than prompted by the software. The bite scan was accomplished with the patient wearing his existing PFM bridge. The preparation scan, however, did not have any landmarks that could be used to stitch to the bite scan. Below is the scan import sequence that will allow any dentist or laboratory to achieve a perfect vertical dimension on cases that don't have any landmarks on the bite scan. In this case, the arch being restored is the lower. For 3Shape users, the following protocol must be followed.
1. When the system asks for the upper arch scan, scan or import the upper arch.
2. When the system asks for the lower arch, scan or import the lower pre-op scan of the patient wearing temporaries or a bridge.
3. When the system asks for the pre-op scan, import the preparation scan and stitch or align it to the pre-op scan.
4. When the system asks to align to the bite scan, scan or import the upper preparation scan and the lower pre-op scan and stitch normally.
This import sequence allows the designer to set up all the scans in their correct position in relation to the patient. This integrated file, which contains all of these scans in the correct position in relation to the patient in centric occlusion, can now be imported into 3Shape Implant Studio.
Once the case is in 3Shape Implant Studio, the following steps must be followed. In order for this technique to work, the system has to be tricked once again.
1. When the system asks to import the lower surface scan, import the preparation scan with the prepared teeth.
2. When the system asks to import the lower pre-preparation scan, import the upper model scan.
3. When the system asks to import the head CT scan, import the dicom files.
4. When the system asks to import the upper surface scan, import the pre-op scan with the bridge.
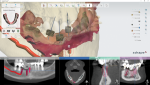
When the above steps are followed in the 3Shape Implant Studio workflow and a user selects a pre-op scan, the software will always stitch the pre-op scan instead of the preparation scan. What this allows the technician to do is trick the system and stitch to the arch that has identifiable landmarks-in this case the upper arch. The software will let the user stitch to what the software believes is the pre-operative scan but is actually the upper model scan or the antagonist. Because the upper and the lower scans are always in the position that was established in the virtual world, even though you are stitching to the upper, the software brings the lower in perfect vertical dimension as it pertains to the patient. As seen in Figure 10 and Figure 11, the author was able to design the lower surgical guide even though there was so much scatter it could not have possibly been stitched.
Conclusion
In theory, an edentulous case can be approached in the same way this case was approached. If the patient's denture is not radiopaque and he or she is scanned with a CT scanner, it should be possible to stitch to the opposing arch, as long as the scan is with the patient biting in centric occlusion and identifiable landmarks are present in both the intraoral scan and dicom file.
When the digital impression is taken, the denture will need to have a landmark that allows for both the denture and the tissue to be in perfect relation. The author would recommend opening a hole on the palate of the denture prior to surgery or creating a duplicate denture to scan and stitch both the denture and the tissue scan to each other, again providing a perfect relation between the two. This should be followed by a scan of the study model first, which consists of scanning the upper and the lower as one scan, and then doing a separate scan for the tissue. If scanning the upper arch, open a hole on the palate of the denture to allow the two files to be stitched, and if it is on the lower arch, every effort should be made to scan as much of the lingual tissue as possible. If it isn't possible to stitch on the lower for both the denture and the tissue, then a radiopaque guide may be required or the impression may be sent to the laboratory for a duplicate denture to be fabricated and a double scan taken.
In the end, this case worked out well, and the oral surgeon was able to use the surgical guide and place the implants. It is the author's intent and hope that this technique will help surgeons and laboratories plan and design surgical guides, even when there is scatter on the CT data file. As long as there are landmarks to stitch to on the upper or lower arches, this technique could be used to plan the case and fabricate a surgical guide successfully.
About the Author
Jeffry Tobon, CDT
DesignLab Dental Inc.
Westbury, New York
Acknowledgments:
Restorative dentistry was completed by Robert Berg, DMD, a private practitioner in New York City. Implant placement was completed by Jay Neugarten, DDS, MD, an oral and maxillofacial surgical member of the craniofacial team at New York Hospital Cornell-Weill Medical Center.