Harmony of Function, Balance of Responsibility
When a case fails, who’s to blame?
Dentists ask technicians for a wide assortment of restorations, requiring them to work with different materials with various handling techniques. Sometimes, despite the technician executing all the steps accurately, a case failure can still occur. The patient is upset, the dentist is angry, and the technician may be blamed for the failure.
Sometimes, the only fault may be a poor plan. This is why the technician should take the opportunity to analyze the treatment plan from a restorative perspective. For the technician to be an asset to the dentist-client and to have a more fulfilling career, the technician should know both what to do and what not to do in each situation. This balance of knowledge is necessary for confident execution.
Many laboratory technicians may feel frustrated or subjugated to their accounts. Consider teeth and dental restorations to have a yin and yang relationship. Crowns have to be both functional and esthetic. Problems can erupt when the focus of the two becomes unbalanced, especially when focus is lost on function. Focusing only on the esthetics of the ceramics is not recommended.
In today’s lecture circuit, clinicians typically discuss failures of certain materials and will mention incisal edge chipping as a common concern. One has to ask, “Is it the porcelain or the technician? Is it the technician or the treatment plan?” Too many times these questions are not asked. False claims are made based on assumptions, anecdotal evidence, or the manufacturers’ marketing materials.
To resolve this, the trend has been to switch to a harder material. This may keep that restoration from breaking in the near future, but what else is happening in the complex oral environment? Poorly made crowns created from extremely hard materials won’t break, but something else has to give. Why can some clinicians do a full mouth of composite restorations with 5 and 10 years of success, and some can’t do four veneers and keep them from fracturing or debonding in a matter of weeks or months? Is it because composite is super strong and porcelain is inherently weak? It certainly is not. Each situation is different, depending on a number of variables: function, the patient’s pathology, proper treatment plan, correct execution, and attention to detail. This article presents two case examples to demonstrate common problems.
Case 1
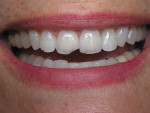
The following is an example of an esthetics-driven case with an overlooked functional component. A patient presented to the dentist, saying she did not like the shapes of her two central incisors. They were worn, and she didn’t think they looked attractive. She wanted them to be longer, less irregular, and more youthful. Although no pre-operative cast was included, the case had a nice study model showing the size and shape of the provisionals. The prescription was for all-ceramic crowns. The preparations were good, and the mounting was accurate. After verifying with a silicone matrix of the study cast, it was clear that the chosen material had sufficient space.
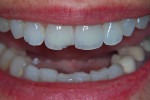
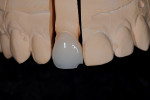
Crowns were made. The case was rushed at the request of the dental office because the dentist deemed the patient difficult. The dentist seated the crowns. Not soon after, the case was returned. The crowns had chipped and needed to be redone (Figure 1). The dentist conveyed how upset the patient was and how discouraged he was. He raised questions about the kind of porcelain used, whether the technician built the crowns poorly, and whether the technician was inexperienced.
This is all too familiar in the laboratory industry— beginning with a case and then blaming, acquiescence, doing a remake, losing revenue, and feeling frustration.
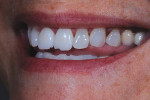
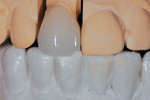
On further examination, the patient was considered difficult because she kept returning to the dental office to have her provisionals fixed. Upon further review, they seem to have been chipping (Figure 2).
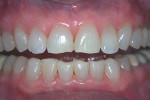
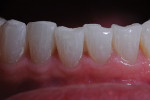
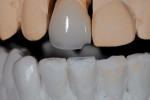
Why were her teeth short and “unattractive”? Upon further examination, they were found to be worn functionally (Figure 3). Whether it was in pure protrusive or extreme crossover or some combination, she wore down her teeth by moving her mandible the way she wanted to move it. She might be doing it during the day, while sleeping, or both. This functioning against her lower teeth was why her centrals were short and her provisionals and crowns were chipped (Figure 4).
The patient had worn the incisal edges of both her upper and lower teeth, which had previously found a balance, or homeostasis. (This arguably could have been seen in a pre-operative cast.) They functioned with one another, allowing her to move in the manner that was the most comfortable. Changing only one of the two components created the problem.
The patient was originally willing to treat only her two maxillary central incisors. They were the teeth that were her main concerns, and she didn’t want to spend additional money on what she thought were unnecessary procedures. Under pressure, the clinician agreed to provide her with only what she wanted. By not correcting the sharp irregularities on the mandibular incisors at the same time, the restorations were destined to fail. The provisionals broke, and eventually so did the porcelain restorations.
The solution for success was for the clinician to restore her lower anterior teeth with composite (Figure 5), giving the patient a smooth surface to balance with the upper restorations. This created harmony between arches, and the crowns could be fabricated stably.
The laboratory technician had to recognize where the causes of the fractures were originating, which was due to a functional wear pattern and isolating on irregularly sharp teeth, and not from poorly fabricated restorations. Or at the very least, he had to see that the desired shapes of the crowns were unrealistic. The dentist had to explain to the patient that although her upper teeth were her main concern, they could not be restored to a different position without also restoring her lowers. If she wanted her two front teeth to have the new shape, she would also need to restore the edges of her lower teeth. One can’t be changed without a change to the other. They have to be in balance.
Case 2
Crowns were fabricated and seated for teeth Nos. 8 to 10 for a seemingly straightforward case. The study cast of the provisionals was followed, and the shapes and shade were made to the dentist’s specifications on the prescription. After the crowns had been seated, the patient returned a week later with a chip in the crown on tooth No. 8. The clinician was able to remove the crown from the tooth and returned it to the laboratory (Figure 6).
In a case like this, it might easy to cast blame on the product. Figure 6 could be misused to show how one porcelain or ceramic system is inferior, preying upon a dentist’s fear of seating a crown that is going to fracture.
The failure in this case was not the ceramic system chosen; it was poor execution on the part of the technician.
Care was not taken to carefully work out function, specifically protrusive. The basic criteria were met, but the last crucial aspect to replacing teeth was overlooked. Balance is needed. The upper must work properly against the lower. That last movement needed to be worked out properly on the articulator, which is an often-neglected step.
The patient’s lower central incisor, tooth No. 25, was slightly more prominent than tooth No. 24. The incisal edges were irregular, causing an issue. A flat plane was coming into contact with an uneven one. When the patient moved into protrusive, the porcelain chipped (Figure 7).
The solution could be enameloplasty on the lower to eliminate the “corner” (Figure 8), or for the crown to be a subtly facial to allow for the lower to function as it is. This was not a material failure; this was technician error. The technician should have seen the functional imbalance that would be created and then consulted the dentist, who would have decided how to best proceed with the patient.
Conclusion
Technicians should be empathetic regarding the daily challenges that their dentist-clients face. Patients visit their offices with various concerns. Some want the minimum work done and will agree only to “dental triage.” Some regard dentistry like picking items from a catalog. They may view dental restorations as a fashion statement. Some may be anxious about any sort of treatment. Many patients have financial concerns. These concerns can modify treatment.
The dentists may provide patients with a thorough treatment plan that may involve multiple steps over an extended period. The dentist may explain that by doing all of the listed procedures, the patient will be at a more ideal level of dental health and be told that the patient only wants part of the work done or some of it deferred to another time. Patients don’t always choose what is best for them because they don’t necessarily understand that even one tooth is part of a greater system. Sometimes for legitimate reasons and to the dentist’s consternation, they refuse proper treatments. Other times they limit their own treatment because they just don’t understand their situations fully.
A balance between dentist and technician is needed as well. It is important for the technician to thoroughly analyze a case prior to beginning it, and then to be responsible for the proper execution. The clinician might have overlooked something due to a litany of reasons of which the technician may not be privy. The technician should bring any concerns to the client’s attention and help them. Subsequently, the dentist can present issues regarding proper treatment to the patient. Then the patient may choose to act on it. Everyone is informed, and the responsibilities lie where they should. Then expectations are reasonable, and surprises are limited. Interdisciplinary harmony is achieved.
About the author
Kyle Swan, CDT
Co-owner, Managing Partner Functional Esthetics
Lewisville, TX