The Secret to Custom Shade Matching
Visualizing and navigating to desired results
Restoring a single anterior tooth is always a challenge for clinicians and technicians when it comes to custom shade matching. Selecting the correct color depends on the colors represented in the adjacent teeth. If the adjacent teeth have a great deal of color, then that indicates low value and detailed differences between those colors. They can be light, medium, or dark in interior color with crack lines and other characteristics that make matching the color a very difficult task. Surface textures can also present a challenge to the technician. This article will illustrate how to take a custom shade, demonstrate one type of material selection and restorative technique in detail, exemplify a step-by-step ceramic layering process, and show dental technicians how to finalize the restoration surface texture with a natural glaze.
Case Study
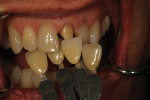
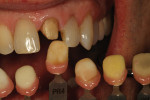
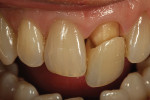
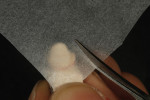
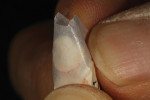
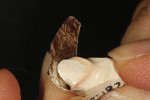
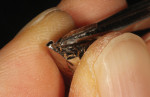
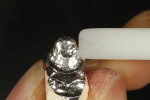
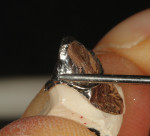
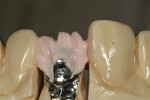
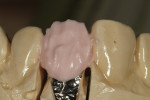
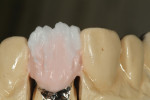
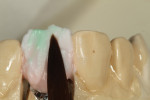
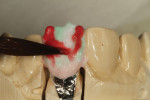
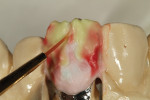
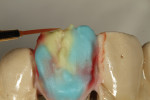
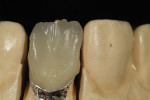
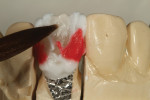
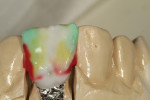
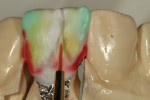
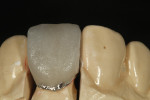
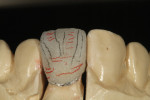
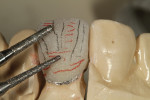
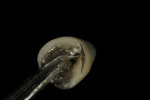
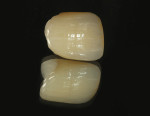
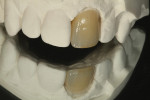
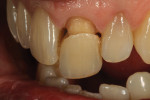
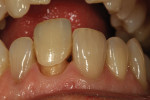
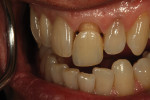
The author created a ceramic shade tab system inclusive of crack lines to distinguish colors within the A3 zone to try and match tooth No. 8 (Figure 1). The underlying preparation color is very important in determining the definitive color, especially when there is a lack of facial room. In cases like these, because the restoration will be translucent after layering, the coping seated in the patient’s mouth should have the same tone and hue, which is an important consideration when matching preparation color (Figure 2). At the try-in stage, dental technicians are given an important starting point and are asked this question: Can we achieve the same saturation and balance of tooth color variation (Figure 3)? The author started with the platinum foil technique when creating this restoration. The translucent paper was used as a platinum foil guide and as a measurement for tooth size (Figure 4). The paper was cut to shape as it was wrapped around the die (Figure 5), and then the foil was cut to size (Figure 6).
After the foil was cut, it was then pressed onto the die (Figure 7). As the author worked, he pressed the foil even more firmly to the die (Figure 8). Using tweezers, he carefully shaped the form of the die before cutting the wrap closely (Figure 9).
A plastic stick was used to press deeply into the margin area; the author further prepared the foil (Figure 10). Unnecessary foil was carefully cut away with scissors (Figure 11 and Figure 12) and shaped and wrapped accordingly (Figure 13 and Figure 14). The final cut made the foil quite small (Figure 15). Using tweezers, the author then finalized the technique (Figure 16). In the final step, the foil was burnished (Figure 17). After burnishing, the author measured the results again and decided to cut away even more excess foil (Figure 18). Using a metal stick, he was able to completely smooth down the edges of the foil over the die (Figure 19) until complete and even coverage was achieved (Figure 20).
When ceramic layering, the author gets best results from GC Initial™ Low Fusing Porcelain (GC America, www.gcamerica.com) (Figure 21). His first step was to apply dentin in an A3 color and inside dentin No. 41 (Figure 22 and Figure 23). Next he layered EOP4 (enamel opal) over the top (Figure 24). After cutting back, he applied Translucency Modifier 01 (Figure 25.) Low Fusing Translucent Modifier-05 was applied next (Figure 26). Grey translucency overlay was applied over the mesial, distal, and body areas (Figure 27 and Figure 28). The next step was to apply Enamel 13 in order to create a white stain (Figure 29). Over the Enamel 13 application, he layered Enamel 57 (Figure 30). Next, the author placed the layered restoration on the die in order to bake it for the first time (Figure 31). After firing (IBEX Summit porcelain oven, IBEX Dental Technologies, www.ibexdental.com), the restoration exhibited a nice translucent appearance (Figure 32).
The restoration was tried on the model for a fit check (Figure 33). Cervical translucency powder was applied (Figure 34) in formula No. 24. Translucency neutral was then applied (Figure 35), and a line was drawn down through the porcelain in order to create a crack line with a white stain (Figure 36). The restoration was baked again at 780°C (Figure 37), and the interproximal contact was checked on the model (Figure 38).
Surface texture markings were created (Figure 39) with a marker, after which the author used both thin and thick diamond disks to create irregular vertical and horizontal surface texture lines (Figure 40). Using Pico-Fit gold die spacer (Renfert USA, www.renfert.com), the author applied his final texture to the surface (Figure 41). With tweezers, he was able to carefully remove the remaining foil from the restoration (Figure 42). In a mirrored image, we can see the irregular surface texture between the teeth in the incisal area (Figure 43) as well as crack lines and mamelon. On the model, a mirrored image is again displayed (Figure 44).
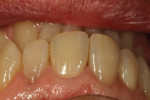
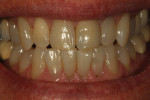
Next, the restoration was tried in the mouth. At this time, the technician could see the balance of color versus the adjacent teeth and positioning of the restoration (Figure 45 and Figure 46). Occlusal views with dehydration demonstrate the harmonized balance of color and tone (Figure 47 and Figure 48). Upon immediate insertion, we see the same translucency and reflection of size and lobe as the natural adjacent teeth (Figure 49). The convex area of the teeth is an almost perfect match with the patient’s dentition.
Conclusion
In order to achieve excellent custom shade matching results, we need proper navigation and an appropriate visualization of the outcome before we get started with the case. We also need to see the patient dehydrated and hydrated in order to take both into consideration as we create the restoration. Translucency (meaning grey, light grey, and clear coloring) or opacity (meaning orange, brown, pinkish grey, or yellow coloring) has to be decided beforehand as well. Crack lines are an additional task to be decided upon, and so is surface texture. Without those considerations, we will not have a matching restoration.
We look to the adjacent teeth for answers. Once we get them, it is not too difficult to adjust accordingly and create a match.
About the Author
Luke S. Kahng, CDT
Owner
LSK121 Oral Prosthetics
Naperville, Illinois