A Case for Comprehensive Dentistry
Traditional and transitional materials for an occlusally compromised patient
These are interesting times in dentistry and dental technology. Knowledge of occlusion has never been more important. Trends toward ultraconservative treatment strategies are happening at the same time as super high strength materials have become available. The idea that strength comes at the expense of beauty is becoming a thing of the past. Although these materials are indicated in many situations, they may not be the most conservative or esthetic solution for all patients.1 Traditional materials can be used in most situations, given comprehensive evaluation, diagnosis, and treatment (if necessary) of occlusal conditions. This article presents one such case where conservative preparations and natural esthetics were important to a patient who had experienced obvious and considerable occlusal trauma. Rather than simply choosing high-strength materials, a strategy of diagnosing and test-driving new joint and tooth positions was employed to maximize esthetics and minimize loss of tooth structure.
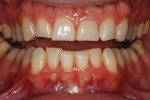
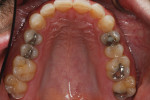
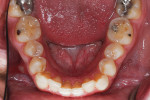
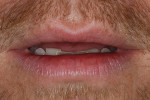
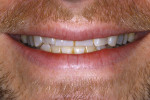
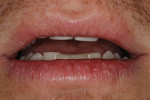
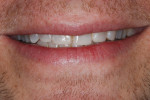
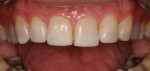
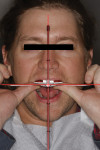
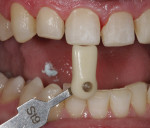
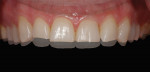
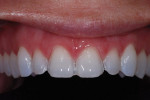
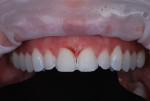
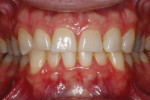
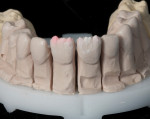
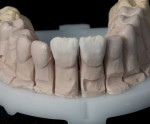
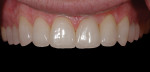
A 30-year-old man presented with concerns regarding the esthetics of his smile (Figure 1). He felt that the color of and wear to his anterior teeth made him appear much older than his age. The patient had a normal range of opening and reported no joint or muscle pain, but severe attrition was evident on his anterior teeth and moderate attrition on his molars and first pre-molars (Figure 2 through Figure 4). The patient reported a lack of awareness of any sleep bruxism. The severe wear made it obvious that solving his esthetic concerns would involve more than simply replacing missing tooth structure with restorative material. Minimally invasive preparations are not always possible but should always be the goal. When major color shifts or tooth position changes are desired, significant tooth reduction may be required.1,2 Many situations involving wear can, however, be treated in a mainly additive fashion. This allows doctors to keep preparations in the favorable enamel layer for bonding.3,4 Preparations in enamel also help maintain structural rigidity in the tooth, which can be compromised when teeth are prepared into dentine.5,6 Ceramists spend years learning how to layer porcelain to mimic internal structures of teeth that, when covered with enamel powders, create restorations that appear natural and lifelike. It is always favorable to achieve final restoration base color and value without preparing away the character naturally occurring in the teeth. To use the natural tooth to its advantage, a material that allows the desirable intrinsic character to be expressed, while selectively masking undesirable colors and prepared incisal edge transitions, should be selected. Monolithic materials (pressed or milled ceramics) in even thicknesses, such as would be used for conservative veneer preparations, are incapable of selective filtration or transmission of light reflected by underlying tooth structure. Feldspathic porcelain on refractory dies was chosen for its ability to do just that.
Treatment Plan
The patient desired a more esthetic smile and wanted to stop the wear that was occurring on his teeth. His lack of anterior tooth display was the major esthetic concern (Figure 5 and Figure 6).
The authors believe that esthetics should be determined visually and that function should be built in after esthetics are determined. Changes to occlusal vertical dimension (OVD) may be required to accommodate the desired esthetic. Incisal edge position, tooth length, and size are subjective and are the first things to be determined in seeing how much dentistry is required. The patient’s lack of symptoms other than tooth wear made him hesitant to accept that alteration of his occlusion was necessary before treatment. It was decided that treatment should include a trial period of directly placed bonded composite restorations to preview the new esthetic and proposed occlusal relationship. Transitional bonding is often used as a prototype material before moving on to definitive restorations. In this case, it would function as a kind of “living splint,” which would allow refinement of the final joint and tooth positions. A Kois Deprogrammer was used to establish an initial joint position. Composite was added to establish incisal edge positions and contacts to maintain this new position. Tooth No. 9 was mocked up to a length 1 mm longer than tooth No. 8 so the patient could preview different incisal edge positions (Figure 7 through Figure 9). The patient was allowed to fully function with the transitional bonding for one month. There was an absence of any symptoms or chipping with the new vertical dimension and incisal length.
Restorative Phase
A Kois Dento-facial Analyzer (Panadent, www.panadent.com) was taken to capture and communicate the esthetic considerations of the maxillary arch (Figure 10). Tooth No. 9 was chosen by the patient to be the more acceptable length and was referenced to be the vertical incisal edge position on the face-bow platform (Figure 11). The records, models, and digital photography were sent to the laboratory technician to fabricate a diagnostic wax-up for teeth Nos. 4 through 13 using tooth No. 9 as the reference point to build the esthetics. The technician was also instructed to refine the shapes of the mandibular tooth cusp tips at the established OVD during the maxillary wax-up. Tooth preparation was finished entirely in enamel and restoration margins were placed supra-gingivally in anticipation of the contact lens effect of the feldspathic veneer restorations. Provisionals were fabricated directly using a matrix that duplicated the contours of the wax-up.
Laboratory
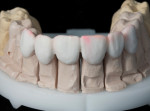
Having a model system that allows a technician to make material selection decisions on the fly is a real luxury. In this case, the technician and dentist had planned on using the refractory die technique. Often, however, ideal material choices can only be made after a first pour model and master dies have been fabricated. The Giroform® model system (AmannGirrbach, www.amanngirrbach.com) makes this decision process simple. The master dies were duplicated using the Giroform flasking system and 16-shore silicone (Elite® Double 16, The Zhermack Group, https://en.zhermack.com), which was cured under a pressure of 60psi (Figure 12). Refractory dies (G-CERA® ORBIT VEST, GC America: www.gcamerica.com) were poured, allowed to bench cure, and then oven cured per manufacturer’s recommendations. The model was reassembled and the ceramist proceeded with ceramic layering. Evaluation of the clinical photographs led the technician to determine that the only major challenge to creating successful restorations would be management of the transitional zone between preparation of the incisal edge and extended ceramic material (Figure 13). The technician should always be provided with photographs of preparations taken with the teeth wetted (Figure 14). The surface of desiccated preparations appear chalky and hide both desirable and undesirable internal structures (Figure 15). In this case, pretreatment photographs suggested that enough tooth structure had been lost through attrition that incisal translucency/opacity nuances would be absent in the prepared teeth and, therefore, would not have to be replicated in ceramic (Figure 16). The transitional zone could thus be handled using simple mixtures of dentine and transitional dentine. Under conditions where ample layering spaces exists, the author uses two firings of clear porcelain to establish connection to and seal the refractory dies. When space is severely limited, the technician should develop the connection to the dies using washes of the enamel porcelains he or she intends to use to complete form. This affords the ceramist the greatest opportunity to influence value or filter out undesirable character in the prepared teeth.
The dies were soaked in distilled water until bubbling of air from the pores of the dies ceased. A thin wash of a mixture of high-value enamel powders was applied to the wetted dies. The dies were completely dried and fired in a calibrated ceramic furnace. The mass of refractory die has the effect of absorbing heat that would normally be transferred to the ceramic.7 The author has found it is necessary to vary the final temperature and/or heat rate from those recommended by the manufacturer of the ceramic material to ensure complete maturation. Test firings should be carried out by ceramists in order to adjust firing cycles for individual ovens. After cooling, the process was repeated to complete the sealing of the dies. Although the dies are effectively sealed at this point, it is important to completely soak them in distilled water prior to each subsequent layering phase.
Management of the transitional zone between extended porcelain and the prepared tooth was accomplished using dentine and transitional dentine powders (mixtures of dentine and enamel) in a pattern that mimicked typical internal dentine structures of teeth (Figure 17). Enamel and internal effect powders were layered, fired, evaluated, and adjusted (Figure 18). Various enamel powders were layered to complete the final forms (Figure 19).
Shapes and surface morphology were refined using diamond burrs and rubber wheels. Natural glaze firing and polishing with rubber wheels and pumice completed the fabrication. The veneers were divested by using 50-micron glass beads in an air abrasion unit at 30 psi. They were fit to the dies and margins were perfected. Finally, they were acid-etched and delivered to the dental office.
The final porcelain restorations were placed using an adhesively retained bonding protocol (Figure 20). The occlusion was refined using the deprogrammer. An upper occlusal splint was made to prevent any damage if para-function was indeed present.
Conclusion
Fulfilling a patient’s esthetic desires may be an end goal, but the treatment plan should include minimizing risk and improving the prognosis. Simply replacing missing tooth structure with restorative material when conditions of malocclusion exist puts restorations made of all but the toughest materials at risk. If high-strength materials are placed in an occlusal situation that is breaking down, the system may still be at risk due to destructive forces. Restorations may survive at the expense of teeth. The dento-facial requirements in this case were the first to be established using direct composite applied to the incisal edges in a noninvasive approach. The Kois deprogrammer allowed the clinician to find, establish, maintain, and verify an acceptable joint position and OVD throughout the process. The functional needs and esthetic requirements were met initially through the additive protocols of transitional bonding. This proved valuable to the clinician in that it allowed the newly designed occlusion and smile to be evaluated before beginning the final restorative process. The patient, in turn, benefitted from being able to preview a new incisal length and chewing system before committing to porcelain restorations. Committing to this process allowed the technician to select materials he felt would be the most esthetic for the case and not simply opt for materials possessing the greatest strength. Proper communication between the dentist and the laboratory technician was important to appropriately satisfy the expectations of the patient. The intra-oral composite mockup and transitional bonding gave the laboratory technician set parameters from which to build the case esthetically and functionally. The use of the deprogrammer in this case was an integral component for the dentist, patient, and laboratory technician. The biomechanical and periodontal risks were not increased because the tooth preparations were supra- gingival and remained in enamel. The functional risk was managed but not eliminated. The patient was made aware that his bruxism put him at increased risk for future chipping of the restorations. Nightly use of the night guard will help manage but not eliminate those risks. The result exceeded the patient’s expectations and was accomplished using a predictable and conservative approach.
References
1. McLaren EA, Cao PT. Ceramics in dentistry—part 1: classes of materials . Inside Dentistry. 2009;5(9):94-103.
2. Spear F, Holloway J . Which all-ceramic system is optimal for anterior esthetics? J Am Dent Assoc. 2008;139(suppl 4):19S-24S.
3.Calamia JR, Calamia CS. Porcelain laminate veneers: Reasons for 25 years of success . Dent Clin N Am. 2007;51(2):399-417.
4. Calamia JR. Etched porcelain facial veneers: a new treatment modality based on scientific and clinical evidence . N Y J Dent. 1983;53(6):255-259.
5. Karlsson S, Landahl I, Stegersjö G, Melleding P. A clinical evaluation of ceramic laminate veneers . Int J Prosthodont. 1992;5(5):447-451.
6. Magne P, Douglas WH. Cumulative effects of successive restorative procedures on anterior crown flexure: intact versus veneered incisors . Quintessence Int. 2000;31(1):5-18.
7. Young G. All-Ceramic Bonded Posterior Restorations . Inside Dental Technology. 2011;2(1):52-59.
About the Authors
Brad Patrick, BSc
Owner
Patrick Dental Studio
Bend, Oregon
Amanda Seay, DDS
Private Practice
Park West Dentistry
Mount Pleasant, South Carolina
To view the complete clinical case of this article featured in the 2012 November/December issue of Compendium, visit dentalaegis.com/go/idt363