A Progressive Process
A predictable, complex rehabilitation combining conventional and state-of-the-art techniques.
By Steve Hoofard, CDT, AAACD; and Dennis Higgins, DDS, PS
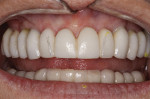
A 61-year-old woman presented seeking a return of function and esthetics in her maxilla. Her chief complaints were chipping of incisal edges and failing esthetics. The mandible had been previously restored with implant-supported, porcelain-fused-to-metal bridges.
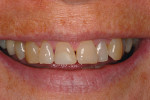
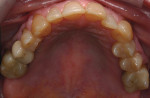
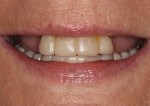
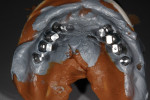
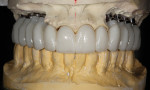
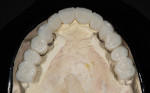
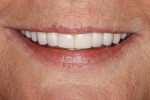
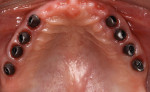
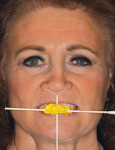
The medical history provided insight into the dental history and was integral to the subsequent treatment planning. The patient had a long history of gastrointestinal problems, which included significant gastroesophageal reflux. The maxillary dentition exhibited signs of chemical erosion and exaggerated attrition (Figure 1, Figure 2, and Figure 3). Cervical decay, enamel undermining, and chipping of the incisal edges were generalized. The significant biomechanical risk drove the treatment plan toward implant-supported restorations. Implant restorations could meet esthetic requirements and were not contraindicated by the relatively minor functional and periodontal considerations. The medical history also revealed that the patient had received a cervical fusion (C3-C7), which significantly limited the number of comfortable chair positions for the patient and clinical providers. Consideration was given to treatment planning that would allow for the least amount of chair time and the most predictable surgical and restorative options.
Fortunately, many other aspects of the case presentation were uncomplicated. The patient displayed a normal amount of tooth in both repose and full smile. There was no issue with excessive gingival display. The temporomandibular joints presented within normal limits radiographically and clinically, and the range of motion was adequate. The interior tissues and muscles of mastication were unremarkable. The occlusion was Class I with aligned midlines and slight crowding, and the patient demonstrated excellent oral hygiene habits.
Treatment Planning
Polyvinyl siloxane (PVS) impressions were taken along with bite records and digital images, and sent to the laboratory. After the preoperative models were fabricated and mounted, a diagnostic wax-up was developed of the maxillary arch at the estimated new vertical dimension of occlusion to propose final shape, form, and function of the definitive restorations—a blueprint. As the treatment plan was implant-based, several consultations were held with the patient, her spouse, the restorative dentist, and the surgeon. All possible options that met the space requirements and desired tooth display outcomes were considered as well as economics. Ultimately, it was determined to proceed with fixed bridges supported by eight implants. Patient management and economic considerations eliminated treatment plans that included additional implants, computer-guided surgery, and/or immediate provisionalization.
Clinical and Laboratory Procedures
Pre-Surgery
The wax-up was duplicated in stone and a suck-down stint of the model was used to create composite resin build-ups on teeth Nos. 7 through 10 (Figure 4). The build-ups were placed directly over the existing teeth without anesthesia, which strengthened the natural teeth for the provisionalization phase of treatment. The build-ups also allowed the patient to assess estimated tooth morphology, smile esthetics, and speech parameters. The proposed incisal edge position was available for evaluation and adjustment.
Surgery I
Teeth Nos. 3 through 6 and teeth Nos. 11 through 14 were extracted. Essential bilateral sinus lifts and bone grafts were also completed at this time. Postsurgical visits were performed.
Post-surgery: An Essex-type retainer was delivered to the patient with pontics of Triad material for teeth Nos. 5 and 6 and teeth Nos. 11 and 12, positioned just out of occlusion. The retainer allowed for the initial evaluation of the occlusal plane and created some esthetic improvement for the patient during the initial healing phase. Also, the use of an Essex-type provisional over fixture sites allows for undisturbed healing while integrating. In this case, the Essex was not intended for function but for evaluation of the occlusal plane and to provide some esthetics for the patient during the healing process. The patient was instructed to limit her function on the appliance.
Surgery II
After approximately 4 months of healing from the extractions, sinus lifts, and bone grafts, the patient received surgery to place the implants. The implants were placed without the aid of a surgical guide. Implants for teeth Nos. 3 and 14 were NobelActive™ 5.0 mm x 10 mm (Nobel Biocare, www.nobelbiocare.com). NobelReplace™ Tapered Groovy™ 4.3 mm x 13 mm implants (Nobel Biocare) were utilized for teeth Nos. 4 through 6 and teeth Nos. 11 through 13. All implants were torqued to 20 Ncm and covered with attached tissue. Regular postoperative observations were used to monitor healing.
Post-surgery: Adjustment to and maintenance of the build-ups and Essex‐type retainer continued.
Surgery III
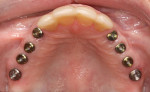
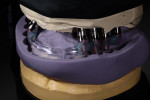
The patient underwent surgery after the implants had integrated for approximately 6 months. The implants were deemed ready for utilization. All eight implants were exposed and appropriate healing caps placed (Figure 5).
Post-surgery: The patient was seen after 3 weeks of soft-tissue healing. The healing caps were removed and topical anesthetic placed in each socket. (Interesting observation at this point: the two NobelActive sites exhibited far superior soft-tissue health as compared to the six NobelReplace.) Appropriate open-tray impression abutments were placed for teeth Nos. 3 through 6 and teeth Nos. 10 through 14, and a PVS impression material was placed in a customized tray. The abutments were locked onto the tray with fast-set acrylic in an attempt to increase the accuracy of the impression. In addition to the impression, a rigid polyvinyl bite registration was obtained, utilizing a leaf gauge on teeth Nos. 7 through 10 and closed-tray abutments on teeth Nos. 4 and 13. All healing caps were replaced on the implants. The impression, bite registration, original mandible cast, and digital images were delivered to the laboratory (Figure 6).
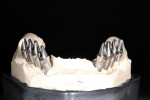
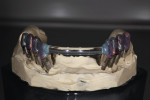
Once in the laboratory, analogs were secured to the transfer copings imbedded in the impression, and then working models were fabricated and mounted. Temporary abutments were modified and fitted to the model (Figure 7). After paralleling the temporary abutments, a matrix was made from the initial diagnostic wax-up to aid in the fabrication of Radica® provisionals (DENTSPLY Prosthetics, www.ceramco.com). The provisionals were comprised of three pieces—a splint on teeth Nos. 3 and 4, a bridge on teeth Nos. 5 through 12, and another splint on teeth Nos. 13 and 14 (Figure 8, Figure 9, and Figure 10). The provisionals and temporary abutments were returned to the dentist for placement.
The temporary abutments were seated on teeth Nos. 3 and 4 and teeth Nos. 13 and 14 at 20 Ncm. The screws were protected with PVS plugs. The provisional splints were re-lined with acrylic resin and temporarily cemented on teeth Nos. 3 and 4 and teeth Nos. 13 and 14 (the bridge on teeth Nos. 5 through 12 was kept for placement in phase IV). A new alginate impression of the provisional splints and teeth Nos. 7 through 10 allowed a new Essex-type appliance to be fabricated and subsequently delivered to the patient.
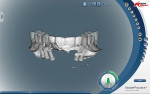
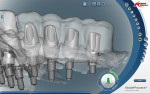
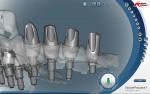
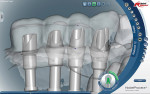
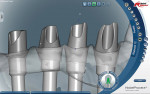
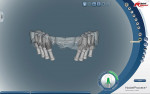
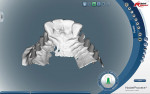
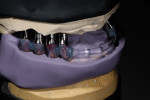
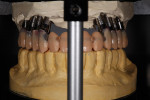
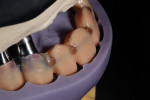
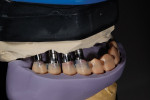
During this phase of clinical treatment, while posterior healing continued under temporization, the definitive custom titanium abutments were designed and fabricated. Utilizing the NobelProcera Scanner (Nobel Biocare), all of the unique geometry and fixture head positions of this case were captured and converted into digital information (Figure 11, Figure 12, Figure 13, Figure 14, Figure 15, Figure 16, Figure 17, Figure 18, Figure 19, and Figure 20). With Noble’s sophisticated design software, all aspects of the design could be customized, including margin placement, parallelism, axial wall position, and coronal height. Once designed, the digital file was sent via the Internet to Nobel’s manufacturing plant in New Jersey for fabrication. The completed custom abutments arrived back at the laboratory in 3 days. Triad® custom placement jigs (DENTSPLY Prosthethics, prosthetics.dentsply.com) were fabricated to help improve the accuracy and ease of placement. Then, they were delivered to the dentist in preparation for the next phase of treatment.
Just prior to phase IV surgery, the definitive custom titanium abutments were tried in with the aid of the custom placement jigs (Figure 21). Parallelism of the splinted positions was verified utilizing a rigid palatal index fabricated with Triad and Primotec® light-cured composite wax (primotec, www.primogroup.net). At this time, it was discovered that some adjustment was necessary to introduce more passivity. The definitive abutments were returned to the laboratory for the adjustments.
Surgery IV
The patient received her final surgery approximately 2 months after the implants were exposed. Teeth Nos. 7 through 10 were extracted. Appropriate bone grafts were utilized to maintain ridge height and contour. Postoperative monitoring of tissue contours and health continued through the rest of the restorative phase of treatment.
Post-surgery: The patient was seen immediately after the extraction surgery. Healing caps were removed from teeth Nos. 5 and 6 and teeth Nos. 11 and 12, and topical was placed. Four customized temporary abutments were torqued to place at 20 Ncm, and the screws were protected with PVS. The provisional bridge (teeth Nos. 5 through 12) was cemented with TempBond® cement (Kerr Dental, www.kerrdental.com), and adjusted for occlusion and incisal display (Figure 22 and Figure 23). The patient received subsequent adjustments to the provisionals for approximately 5 months. Occlusal, esthetic, phonetic, and hygiene issues were all addressed during this period of final healing.
Final Impression
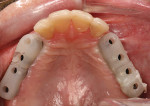
The final impression appointment proved to be complicated, as all of the information obtained during the months of healing had to be accurately recorded and relayed to the laboratory. The laboratory returned the eight custom-milled abutments, which were then positioned on the appropriate implants (Figure 24).
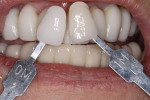
Digital images of the patient, including images of a stick bite, shade (patient desired a lighter shade anticipating re-doing the mandibular bridgework in the future), and approved provisionals were taken (Figure 25, Figure 26, and Figure 27). A new Kois Dento-Facial record (Panadent, www.panadent.com), model of the adjusted provisional, and bite registration of provisional to lower arch were obtained. The laboratory-fabricated Triad indices were placed over the abutments, and a CR bite registration was obtained. The posterior provisionals were then re-positioned and held the vertical while an anterior bite registration was recorded. (Closed-tray abutment copings on teeth Nos. 6 and 11 were used to secure and transfer the bite registration.) The final abutments and their relationship to healed soft tissues were recorded in a PVS impression obtained in a new customized tray over the Triad indices, for accuracy, utilizing the open-tray technique. The temporary abutments and Radica provisionals were reinserted, and the occlusion was readjusted. All records, along with the custom abutments, were returned to the laboratory for fabrication of the definitive metal-ceramic restorations.
When the records arrived at the laboratory, analogs were secured to the custom abutments imbedded in the impression. A soft-tissue material was injected around the analogs to allow the soft-tissue information to be removed and replaced during the fabrication process (Figure 28). The working models were completed and mounted using the records provided.
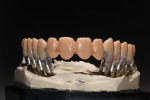
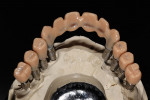
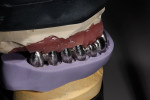
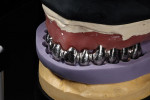
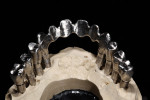
The custom titanium abutments were then placed on the working model (Figure 29), and fabrication of the metal substructure started. Primotec light-cured composite was used to form rigid copings on the abutments. Next, an acrylic bar was used to splint all copings together (Figure 30). They were all luted together with Primotec light-cured composite wax. This provided a stable, rigid structure to support the wax mock-up and maintain accuracy. A Siltek® matrix (Ivoclar Vivadent, www.ivoclarvivadent.com) formed from the original diagnostic wax-up was used to verify the position of the developing frameworks (Figure 31 and Figure 32).
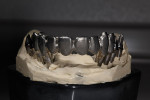
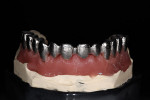
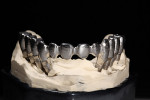
Beige THOWAX sculpturing wax (Yeti Dental, www.yeti-dental.com) was used to create the desired contours (Figure 33, Figure 34, Figure 35, Figure 36, Figure 37, and Figure 38). The wax-up was placed back on the Panadent articulator for verification of contours for porcelain support. Once the three framework designs were completed in wax, they were invested, burned-out, and then cast in a Neo Super Cascom vacuum and pressure casting machine (KDF, www.kdfus.com) (Figure 39, Figure 40, Figure 41, Figure 42, and Figure 43). The efforts of utilizing rigid materials in the wax-up stage paid off with a passive and very accurate fit immediately after de-vesting.
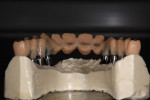
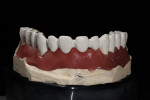
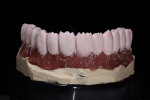
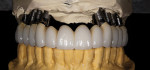
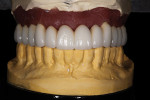
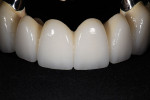
Final contours of the frameworks were established and confirmed again using the Siltek matrix and soft-tissue information (Figure 44, Figure 45, Figure 46, Figure 47, Figure 48, Figure 49, and Figure 50). The frameworks were then opaqued (Figure 51). IPS dSign® porcelain (Ivoclar Vivadent) was layered and fired to develop the desired contours. First, a thin layer of deep dentin was applied to the frameworks, along with filling the intaglio space on the pontics to develop the ovate contours desired. Next, dentin was layered and formed to almost full contour, leaving space for internal effects, enamels, and external effects (Figure 52). Internal effects and enamels were added, and then condensed. The interproximals were sliced to the framework (to eliminate lifting and tearing during firing), and then placed in the furnace to fire (Figure 53). A second and third enamel and effect firing followed to fill all desired contours (Figure 54). Final shape, anatomy, surface morphology, and surface texture were established (Figure 55). The restorations were then glazed and polished, with a final check for fit and occlusion (Figure 56, Figure 57, Figure 58, Figure 59, and Figure 60) and then delivered to the dentist.
Delivery
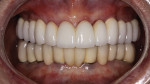
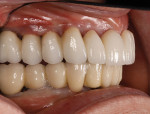
The laboratory returned the eight permanent abutments and the newly fabricated metal-ceramic bridges (the splint on teeth Nos. 3 and 4, the splint on teeth Nos. 13 and 14, and the bridge on teeth Nos. 5 through 12). Final abutments for teeth Nos. 5 and 6 and teeth Nos. 11 and 12 were seated and torqued to 35 Ncm. PVS material was used to protect the screw heads. The anterior bridge fit was confirmed and cemented with TempBond cement as this allowed for a more accurate occlusal adjustment, retrieval for final polish, and a trial period for speech and hygiene concerns. The anterior bridge was adjusted to hold shim stock on centric occlusal contacts on teeth Nos. 5 and 6 and teeth Nos. 11 and 12. Right and left working contacts were retained on these abutments. All excursive contacts were eliminated from the pontics. The posterior splints were then tried in, fit confirmed, adjusted to hold shim stock in centric, adjusted to contribute to group function in working function, and cemented with Unicem cement. There was very little adjustment necessary in centric or protrusive contacts, and no non-working interferences were present (Figure 61, Figure 62, Figure 63, and Figure 64).
The patient returned in 1 month and reported only minor issues, which were easily adjusted intraorally. The anterior bridge was removed, polished, and seated with permanent cement.
Conclusion
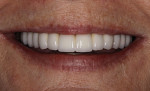
The patient was delighted with the final results. She presently experiences comfortable function without sensitivity or pain. She no longer fears tooth chipping or fractures. The esthetic results surpassed her expectations, a nice reward for the many trials and tribulations of long-term provisionalization. A result such as this is entirely dependent upon thorough communication among the patient, surgeon, technician, and clinician. All involved feel deeply rewarded by this effort and outcome.
Resources
1. Steel C, Behle C, Ballerino M, et al. Photo- graphic Documentation and Evaluation in Cosmetic Dentistry: A Guide to Accreditation Photography. Madison, WI: American Academy of Cosmetic Dentistry; 2004.
2. Blitz N, Steel C, Willhite C. Diagnosis and Treatment Evaluation in Cosmetic Dentistry: A Guide to Accreditation Criteria. Madison, WI: American Academy of Cosmetic Dentistry; 2004.
3. Kataoka S, Nishimura Y, Sadan A. Nature’s Morphology: An Atlas of Tooth Shape and Form. Chicago, IL: Quintessence Publishing; 2002.
4. Adolfi D. Natural Esthetics. Chicago, IL: Quintessence Publishing; 2002.
5. Chu SJ, Devigus A, Mieleszko AJ. Fundamentals of Color: Shade Matching and Communication in Esthetic Dentistry. 1st ed. Chicago, IL: Quintessence Publishing; 2004.
6. Fradeani M, Barducci G. Esthetic Rehabilitation in Fixed Prosthodontics. Vol. 2. Chicago, IL: Quintessence Publishing; 2008.
7. Kina S, Bruguera A. Invisible: Esthetic Ceramic Restorations. São Paulo, Brazil: Editora Artes Médicas; 2009.
About the Authors
Steve Hoofard, CDT, AAACD
Owner
Aesthetic Designs Laboratory
Hermiston, Oregon
Dennis Higgins, DDS, PS
Owner
Viewpoint Dentistry
Richland, Washington