Repairing Worn Dentition
Using the press technique, six anterior crowns restored the patient’s beautiful smile.
By Brad Jones, FAACD
Patients today demand youthful, attractive smiles. Dental professionals approaching esthetic restorative cases must take into account the entire esthetic zone, not just a single tooth.1,2 Undertaking cases of functionally compromised dentition requires comprehensive and multidisciplinary treatment plans that utilize all members of the dental team.1,2 To achieve consistent predictability and the best results, open communication between the dentist, technician, and patient, as well as proper technique and material selections, are a must to meet the demands of patients undergoing restorative dental work.1-3
Material Choice
When choosing a restorative material, dentists and technicians must consider all factors, including the esthetic desires of the patient, the functional requirements of the case, tooth color, core or abutment use, condition of the tooth, where the tooth sits in the mouth (anterior or posterior region), and whether the restoration will be cemented or bonded.4 With a variety of materials available on the market today, dentists have the unique ability to choose a product that offers them the best in functionality and esthetics while providing the greatest amount of characterization and placement options.4
The following case demonstrates how a lithium-disilicate glass-ceramic material was used to restore the dentition of a young female patient who presented with excessive wear and previous dental work. Through the use of the pressable technique and a team approach, the patient’s desire for a more esthetic smile was achieved, while function and strength were restored to the oral cavity.
Lithium-disilicate ceramic material contains approximately 70% by volume needle-like crystals in a glassy matrix. The matrix controls the size, shape, and density of the crystals, giving lithium-disilicate glass-ceramic greater strength and durability.5,6 Because the material displays a relatively low refractive index, optical qualities such as translucency allow for optimal esthetics.5-7
Currently available for two different processing techniques, lithium-disilicate ceramic material gives dentists and technicians the opportunity to provide highly functional and esthetic restorations in a variety of indications.6,8 In the pressable form (IPS e.max® Press, Ivoclar Vivadent, www.ivoclarvivadent.com), restorations are fabricated with a wax hot-press technique and demonstrate a flexural strength of 400 MPa.6,8 Using CAD/CAM technology, milled lithium-disilicate (IPS e.max® CAD, Ivoclar Vivadent) restorations can be created in either the laboratory or chairside in the dental office.6,8 Due to the difference in crystal size from the lithium-disilicate press, flexural strength of the mill material is slightly lower at 360 MPa.6-9
Available in a variety of translucencies, the esthetic nature of lithium-disilicate restorations can be further characterized and enhanced using either a cutback-and-layer or stain-and-glaze technique.5,10 In cases requiring the restoration of worn dentition and removal of previous restorative work and materials, the use of lithium disilicate is beneficial because it demonstrates high strength, esthetic qualities, ease of fabrication, versatility, and predictable results.6
Case Presentation
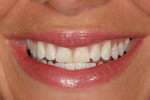
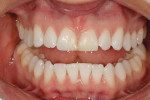
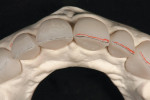
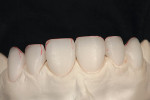
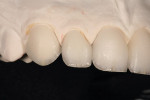
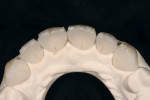
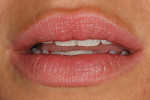
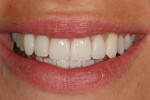
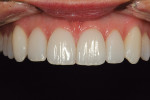
A 25-year-old woman presented with significant wear and an old composite build-up on teeth Nos. 8 and 9 to close a diastema ( Figure 1, Figure 2, Figure 3 and Figure 4 ). The patient wanted a glamorous smile, therefore it was decided that the treatment plan would include restoration of teeth Nos. 6 through 11. A diagnostic wax-up was completed to demonstrate the final results of the case to the patient and to ensure that the restorations would meet the patient’s goals (Figure 5).11,12 Once the patient accepted the treatment plan, a preparation appointment was made.
Clinical Appointment
Using a matrix made from the diagnostic wax-up, a mock-up was formed intraorally using a temporary material. A 0.7-mm depth-cutting bur was then used to cut into the mock-up. To ensure conservative preparation and preservation of sound tooth structure, consideration was made to avoid removing tooth structure when cutting into the plastic. A conservative approach was taken to avoid over-preparing the teeth.
After the initial preparation was done, 12 preoperative photographs were taken of the patient before the diagnostic wax-up was complete. After the preparation and margins were finalized, a photograph of the preparation color was taken to communicate the shade of the preparations to the laboratory. Final impressions and a bite registration were then completed.
To form the provisional restorations, the same matrix from the diagnostic wax-up was used. Photographs and impressions of the provisionals were taken one week after the preparation appointment, including an eyebrow-to-chin photograph of the patient smiling, the most important of all clinical images.13
Laboratory Protocol
To meet the requirements of the clinician and patient, laboratory technicians must have all necessary diagnostic tools and information available to them prior to building the restorations. These items include preoperative photographs, provisional photographs and impressions, master impressions, bite registrations, and a horizontal plane reference (stick bite).13 It is of the utmost importance to have an eyebrow-to-chin photograph of the patient, with the stick bite in place on the lower incisors, to communicate the needs of the case.13 Proper model work forms the foundation of the final restorative outcome.
In the laboratory, a matrix was initially formed over the cast of the provisionals. The matrix was used as a mold during wax injection onto the treated master dies. Through the lost-wax process, the final restorations were produced using lithium-disilicate glass-ceramic (IPS e.max®) HTBL1 ingots pressed at a temperature of 917°C.
After pressing, the facial–incisal edge was marked with a red pencil, followed by marking with a 0.3-mm lead pencil (Figure 6). The pencil marks were used to accurately indicate a line 0.5 mm lingually for facial reduction. This reduction was completed using a K6974 220 centered diamond disc (KOMET USA, www.kometusa.com). A red pencil was again used to mark the incisal interproximal area to be troughed out with the K6974 220 centered diamond disc (Figure 7). The trough was created to carry the gray-blue stain, which imparted an incisal effect similar to that of the patient’s natural dentition.
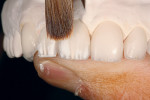
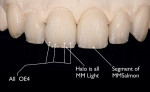
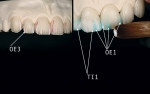
Universal stains were then applied to emulate the high and low value details found in the internal structures of the patient’s natural teeth (Figure 8 ). After building the center lobe with light and salmon mamelon powders (Ivoclar Vivadent), OE4 white dentin powder (Ivoclar Vivadent) was applied to create the mesial and distal internal lobes (Figure 9). To finalize the internal effects, light mamelon material was placed on the incisal edge using a fanned build-up brush in order to create a natural halo effect (Figure 10). Once this process was complete, the internal effects were fired (Figure 11).
Opal clear (OE1) and high-value enamel (TI1) powders (Ivoclar Vivadent) were then segmented carefully to maintain OE1 on the outermost incisal, mesial, and distal edges (Figure 12 and Figure 13 ). The contoured enamels were carefully placed on the restorations, which were then fired at the high temperature of 750°C. After firing, the facial lobes and surface texture were created using an 842r diamond bur (KOMET USA). The surfaces of the restorations were then glazed, polished, and ready for delivery.
Final Cementation
After the completed restorations were received from the laboratory, the patient returned to the office for the cementation appointment. Once the provisionals were removed and the teeth prepared for cementation, the patient was administered 15 mg of propantheline bromide 30 minutes prior to treatment. Propantheline was used because of its ability to stop most salivary flow for several hours, making isolation and cementation easier to achieve. However, care should be taken when using propantheline with patients who wear contact lenses. These patients should remove them prior to taking the medication since it will cause excessive drying of the eyes.
The patient was first fitted with a lip and cheek retractor (OptraGate®, Ivoclar Vivadent). The teeth were then etched with a 37% phosphoric acid system (Total Etch, Ivoclar Vivadent) for 10 to 20 seconds. To prevent postoperative sensitivity, a dentin surface conditioner (Systemp.® Desensitizer, Ivoclar Vivadent) was placed and air-dried. A single component bonding agent (Optibond® Solo Plus™, Kerr Corporation, www.kerrdental.com) was placed in the veneers, which had been prepared using a standard etching technique consisting of 5% hydrochloric acid and a silane agent. The bonding agent was then applied to the preparations, air-dried, and light-cured.
Resin cement (Calibra®, DENTSPLY International, www.dentsply.com) in a translucent base shade was then used to ensure proper midline symmetry of the restorations for the central incisors, which were seated and bonded. These were tacked with a 2-second cure directly on the facial using a 4-mm turbo tip. The restorations for the lateral incisors were then seated, followed by the canines, each with a 2-second turbo tack cure. Because all six restorations were to be seated in 2 minutes, efficiency and speed were required. After seating, an 11-mm curved curing tip was used for approximately 10 seconds to wave over the buccal and lingual aspects of all restorations.
Excess cement was then removed with a sickle scaler and floss. Glycerin gel was placed on all margins and a final cure was completed with an 11-mm tip for 20 seconds on both the buccal and lingual aspects. It was ideal to use two curing lights at the same time, one on the lingual of the tooth and one on the buccal, to ensure even curing and to prevent any shrinking of the cement toward or away from the light. Upon completion of the procedure, a beautiful esthetic outcome was achieved through the use of predictable methods and materials ( Figure 14, Figure 15, Figure 16, Figure 17 and Figure 18 ).
Conclusion
When undertaking cosmetic restorative treatments, it is important to consider all modalities of treatment and available materials. With this case, sustained and proper communication between the dentist and technician, as well as with the patient, allowed optimal results to be achieved.11,12
Exceptional outcomes are accomplished not only through experience, but also by the ability of the dentist and technician to closely predict the results of each and every case. By considering case selection, method of treatment, and material, and by visualizing the anticipated restorations, dentists and laboratory ceramists can succeed in delivering optimal esthetics and fulfilling patient desires.13
The author would like to thank Tim Huff, DDS, for his excellence in dentistry.
References
1. Powell T. Excellence and predictability: not an accident. Dent Today. 2009;28(9):122-124.
2. Ohyama H, Nagai S, Tokutomi H, Ferguson M. Recreating an esthetic smile: a multidisciplinary approach. Int J Periodontics Restorative Dent. 2007;27(1):61-69.
3. Koczarski M. Smile makeover utilizing direct composite resin veneers. Dent Today. 2008;27(12):76,78-79.
4. Spear FM. Treatment planning materials, tooth reduction, and margin placement for anterior indirect esthetic restorations. Advanced Esthetics and Interdisciplinary Dentistry. 2005;1(4):4-13.
5. McLaren EA, Phong TC. Ceramics in dentistry—part I: classes of materials. Inside Dentistry. 2009;5(9):94-103.
6. Tysowsky GW. The science behind lithium disilicate: a metal-free alternative. Dent Today. 2009;28(3):112-113.
7. Reynolds JA, Roberts M. Lithium-disilicate pressed veneers for diastema closure. Inside Dentistry. 2010;6(5):46-52.
8. Helvey GA. Chairside CAD-CAM. Lithium disilicate restoration for anterior teeth made simple. Inside Dentistry. 2009;5(10):58-67.
9. Dudney TE. Unlock that combination. Dental Products Report. 2009;43(3):60-62.
10. Fabianelli A, Goracci C, Bertelli E, et al. A clinical trial of Empress II porcelain inlays luted to vital teeth with a dual-curing adhesive system and a self-curing resin cement. J Adhes Dent. 2006;8(6):427-431.
11. Kahng LS. Patient-dentist-technician communication within the dental team: Using a colored treatment plan wax-up. J Esthet Restor Dent. 2006;18(4):185-195.
12. Nanchoff-Glatt M. Clinician-patient communication to enhance health outcomes. J Dent Hyg. 2009;83(4):179.
13. Terry D.A. Aesthetic & Restorative Dentistry: Material Selection & Technique. Everest Publishing Media. 2009:152-153.
About the Author
Brad Jones, FAACD, Owner, Professional Dental Arts, Boise, Idaho.