Enhanced Communication
An open dialogue between the dentist and ceramist offered this patient an esthetic and functional solution to teeth discolored by bonded orthodontia.
By Jonathan Ferencz, DDS, FACP; and Pasquale Fanetti, RDT
Increases in the clinical use of all-ceramic restorations and advancements in material sciences have enhanced the physical properties of modern ceramics, allowing dental ceramists and their dentist clients to use metal-free restorative options in new ways.1 Concurrently, new techniques such as chairside and laboratory CAD/CAM fabrication and porcelain layering and pressing have made the process of creating highly esthetic and functional restorations faster and easier than before.2
Though the underlying concepts of ceramic restorations have remained the same since their inception, new materials enable the creation of restorations with enhanced strength and esthetics, requiring less damage and preparation to the underlying and surrounding dentition.2 By using minimally invasive techniques, dentists can offer patients treatments with little to no discomfort during and after procedures, and correct issues that typically have been difficult to address.1 However, working closely with the laboratory is of paramount importance to the success of any case, since esthetic considerations, preparation design, and clinical parameters dictate material selection.
Lithium Disilicate
Of the metal-free materials available, glass-ceramic lithium disilicate contains approximately 70% needle-like crystals by volume in a glassy matrix.3,4 As a direct result of the controlled size, shape, and density of the crystalline structure, lithium disilicate demonstrates greater strength and durability than most all-ceramic systems.3,4 The material’s low refractive index produces optimum optical properties, such as translucency, and esthetics that satisfy patients and practitioners.5
Currently available for two processing techniques, lithium disilicate can be conventionally pressed or it can be milled using CAD/CAM technology.4 Pressable lithium disilicate restorations (IPS e.max® Press, Ivoclar Vivadent, www.ivoclarvivadent.com) are fabricated using a hot-wax press technique, and milled CAD/CAM restorations (IPS e.max CAD) are fabricated using either laboratory or chairside CAD/CAM technology.4,6
Because of its crystal size and length, the flexural strength of pressable lithium disilicate (400 MPa) is higher than CAD/CAM-milled lithium disilicate (360 MPa).4 However, all other characteristics of the material are similar, and the choice of two different processing techniques enables dental professionals to address various issues in the oral cavity that might otherwise limit the indications for metal-free restorations.4 The greater strength and presence of a glassy matrix also allow dentists to either conventionally cement or adhesively bond restorations composed of lithium disilicate.7,8
When cases require crowns, lithium disilicate offers advantages compared to conventional full-crown materials. Because the preparation for this material is minimal, the risk of pulpal damage is reduced.9 Also, veneers and crowns created from lithium disilicate decrease a patient’s chances for developing postoperative periodontal issues, because the margins are thin and typically end at, or just above, the free gingival margin.9 Anterior guidance and occlusion also can be maintained when fabricating restorations from lithium disilicate.9
Case Planning
When using lithium disilicate for fabricating anterior restorations, as with any restorative case, it is necessary to first discuss treatment options with the patient, and the laboratory ceramist also should be involved in this process.10 Once a specific option is considered, diagnostic tools should be used in order to completely understand the patient’s expectations and any limitations of the proposed restorative therapy. It is the combined responsibility of dentists and ceramists today to use the plethora of diagnostic tools available to develop the restoration visually, before subjecting patients to what is, in most cases, irreversible treatment.10
Among the tools used by laboratory technicians and dentists in the diagnosis and treatment-planning processes are preoperative photographs11 and radiographs, mounted diagnostic cases,12-15 the provisional restorations that replicate the proposed final restorations,16 and, on occasion, white-wax “mock-ups” of the final case that can be tried in. Preoperative photographs illustrate the condition of the patient’s teeth before a procedure and, when manipulated with imaging software, show how they might look after restorative treatment.17 Proper coloring, shading, size, and contouring can be determined in part by examining and manipulating images of the patient’s smile and discussing the proposed changes with the patient,17 ensuring that the final treatment will meet everyone’s expectations.
Mounted diagnostic casts based on preoperative impressions enable ceramists and dentists to identify occlusal and/or functional problems that may impact restorative and material decisions. Then diagnostic wax-ups can be developed to facilitate patient assessment of the proposed treatment, as well as allow technicians and dentists to predict potential problems that could arise during treatment.13,14 By using wax-ups, proper contours for the final restorations can be easily developed and replicated, as wax-ups provide a detailed and accurate guide during the restorative process and form the basis for other intraoral tools, such as the silicone matrix.13-15
Although typically created after assessing the patient’s preoperative condition, studying the diagnostic models, and completing and evaluating the wax-up, provisional restorations still serve a diagnostic function. In particular, and most importantly, provisional restorations afford ceramists and dentists the opportunity to gain direct feedback from the patient about the fit, function, and esthetics of the proposed restorations.16 This information is extremely useful because, ideally, the only difference between provisional and definitive restorations is the material used.16
Case Presentation
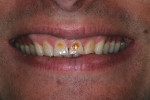
A 35-year-old man presented with a chief complaint about the appearance of his smile. He had worn bonded orthodontic brackets for an extended time as a teenager, and he disliked his discolored anterior teeth, which had been that way for as long as he could remember. As a result, he had been extremely self-conscious about his appearance.
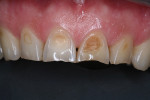
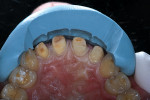
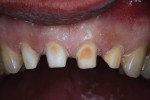
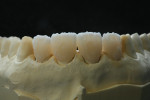
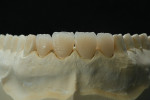
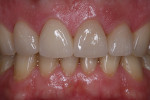
A comprehensive examination and esthetics consultation was performed, during which the laboratory ceramist, who worked in-house, participated in the discussion. The examination revealed severe discoloration and erosion of teeth Nos. 7 through 10 (Figure 1), to which a diet consisting of large amounts of citrus juice each day may have been a contributing factor. The patient also exhibited a high smile line (Figure 2), as well as some wear on the lingual aspect of the four incisors.
Collaborative Treatment Planning
Although porcelain-laminate veneers were discussed, the lingual wear on the maxillary incisors directed treatment toward four crown restorations for teeth Nos. 7 through 10. However, to be as conservative and esthetic as possible, a lithium-disilicate material (IPS e.max) was chosen.
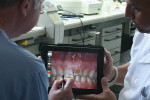
Then, to create a treatment plan for the proposed restorations, preoperative photographs and radiographs were uploaded onto a handheld, touch-screen viewing device (iPad®, Apple Inc, www.apple.com) and used to virtually design the proposed esthetic changes. The ceramist and dentist drew the desired length and esthetic outcome of the final case (Figure 3).
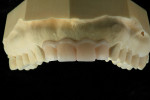
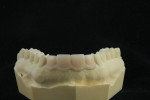
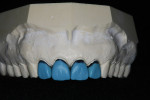
Once this information was discussed and the goals of treatment agreed upon, a diagnostic wax-up was created. This wax-up incorporated the desired length and form of the planned IPS e.max crowns (Figure 4).
Clinical Preparation
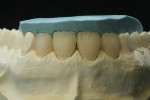
After the patient approved the proposed treatment and esthetic enhancement, provisional restorations were fabricated in the in-house laboratory, according to the diagnostic wax-up using a powder/liquid-based resin (Telio Lab, Ivoclar Vivadent) (Figure 5).
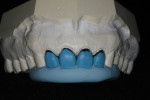
The teeth were prepared using a silicone matrix (GCLT Laboratory Putty, GC America, www.gcamerica.com) taken from the diagnostic wax-up (Figure 6). After cutting the silicone impression through the incisal edges, it was placed over the prepared teeth to verify that adequate tooth reduction was achieved. This would ensure fabrication of the final crowns to the exact dimension of the diagnostic wax-ups.
A minimally invasive margin placement was completed, because it was not necessary to place the cervical margins very far below the gingival margin (Figure 7). Such margin placement would be far more likely to provide long-term soft tissue health than aggressive sub-gingival preparation. Because the crowns would be fabricated from highly esthetic lithium disilicate (IPS e.max) and the low-translucency (LT) IPS e.max ingot was selected, the discoloration of the labial aspect of the preparation would not be an issue; the labial thickness of the final crowns would block out any preparation discoloration.
Final impressions were taken, and the patient received the provisional restorations.
In the laboratory, the final impressions were poured, and a white wax mock-up was created based on the length and form determined by the diagnostic wax-up (Figure 8). At the patient’s next appointment, this mock-up was tried in the patient’s mouth to provide an opportunity to preview the length, contour, surface texture, and form of the final crowns. The patient was encouraged to give his opinion of the esthetics, because changes are easier to make in wax than in the final ceramic. After the patient, dentist, and ceramist approved the white wax mock-up, a shade was selected and the provisional restorations were re-cemented.
Laboratory Procedure
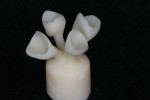
The crowns were waxed on the master cast (Figure 9). This process was simplified by taking a silicone impression of the white wax mock-up and injecting molten pressable ceramic wax (Pressable Ceramic Wax, Hi-Tech Wax, Inc, www.hi-techwax.com). This transferred the exact form defined by the white wax mock-up to the wax patterns to be pressed. The margins were sealed with a specially designed margin wax (Black Margin Wax, Hi-Tech Wax, Inc).
The wax patterns were cut back to allow layering of the translucent enamels and create a lifelike translucency at the incisal edge and labial surface (Figure 10). A putty impression of the white wax mock-up was used to ensure adequate reduction of the incisal and labial surfaces of the wax patterns.
The completed wax-ups were sprued, invested, burned out, and pressed using the IPS e.max LT ingot in shade A2 (Figure 11). The pressed crowns were de-vested and placed in a dissolving liquid to eliminate the surface reaction layer. The crowns were cut from the sprues and were ready for layering with the IPS e.max ceramic veneering powders (Figure 12).
A thin wash of Dentin A2 was placed at the cervical area of the crowns to ensure an even color tone during staining and glazing (Figure 13). Then, a thin layer of Opal Enamel 1 was placed on the labial surface to create a natural opal-blue effect. The Transpa Neutral and Transpa Incisal shades of veneering powders were then placed in thin layers over the labial surface, from mesial to distal, to impart the necessary translucency. Once this first layer was completed, the crowns were fired at a temperature of 750ºC.
After the first bake, the crowns were placed on the master cast with the lingual index to verify length (Figure 14). This also allowed the ceramist to verify that the effects placed on the incisal edge were acceptable prior to applying Transpa Incisal 3 and completing the second bake at 750ºC.
The crowns were fit back on the master cast after the second firing, and the desired surface texture was created in the wet ceramic before final firing (Figure 15). Diamond burs and rubber wheels were used to complete the final crown contours (Figure 16). Finally, the crowns were glazed at 725ºC and hand-polished with a diamond paste to create a lifelike luster (Figure 17).
Final Seating
After the provisional restorations were removed and the preparations properly cleaned, the final restorations were tried in to verify fit, occlusion, and esthetics (Figure 18). The lithium-disilicate crowns were placed using a dual-cure universal resin cement (Multilink®, Ivoclar Vivadent). The patient returned to the office for final verification of the occlusion and an additional check on the removal of excess cement (Figure 19). With the esthetics and chip-resistance of the IPS e.max lithium-disilicate crowns, the patient was very pleased with his treatment outcome.
Conclusion
With enhanced strength and optical properties, materials like IPS e.max lithium disilicate enable ceramists and dentists to satisfy patient requests for highly esthetic restorations while simultaneously fulfilling clinical and functional requirements.2 Additionally, the material’s capacity for conventional cementation and minimally invasive preparation designs provide patients with conservative options, even when full-coverage crowns are necessary.
However, regardless of the material used to fabricate esthetic crowns, restorative and esthetic success is predicated on thorough communication and collaboration among the dentist, ceramist, and patient. Incorporating proven diagnostic and treatment planning tools into the communication process enhances the predictability treatment outcomes.
References
1. Fasbinder DJ, Dennison JB, Heys D, et al. A clinical evaluation of chairside lithium disilicate CAD/CAM crowns: a two-year report. J Am Dent Assoc. 2010;141(Suppl 2):10s-4s.
2. Kurbad A, Reichel K. CAD/CAM-manufactured restorations made of lithium disilicate glass ceramics. Int J Comput Dent. 2005;8(4):337-348.
3. McLaren EA, Phong TC. Ceramics in dentistry: classes of materials. Inside Dentistry. 2009;5(9):94-103.
4. Tysowsky GW. The science behind lithium disilicate: a metal-free alternative. Dent Today. 2009;28(3):112-113.
5. Reynolds JA, Roberts M. Lithium-disilicate pressed veneers for diastema closure. Inside Dentistry. 2010;6(5):46-52.
6. Helvey GA. Chairside CAD/CAM. Lithium disilicate restoration for anterior teeth made simple. Inside Dentistry. 2009;5(10):58-66.
7. Dudney TE. Unlock that combination. Dental Products Report. 2009;43(3):60-62.
8. Fabianelli A, Goracci C, Bertelli E, et al. A clinical trial of Empress II porcelain inlays luted to vital teeth with a dual-curing adhesive system and a self-curing resin cement. J Adhes Dent. 2006;8(6):427-431.
9. Terry DA, Leinfelder KF, Geller W, eds. Aesthetic and Restorative Dentistry: Material Selection and Technique. 1st ed. Stillwater, MN: Everest Publishing Media; 2009:152-153.
10. Donovan TE, Cho GC. Diagnostic provisional restorations in restorative dentistry: the blueprint for success. J Can Dent Assoc. 1999;65(5):272-275.
11. Ahmad I. Digital dental photography. Part 2: Purposes and uses. Br Dent J. 2009;206(9):459-464.
12. Garcia LT, Bohnenkamp DM. The use of diagnostic wax-ups in treatment planning. Compend Contin Educ Dent. 2003;24(3):210-212, 214.
13. Denehy GE. A direct approach to restore anterior teeth. Am J Dent. 2000;13(Spec No):55D-59D.
14. Vanini L, Mangani F, Klimovskaia O, eds. Conservative restoration of anterior teeth. Viterbo, Italy: ACME. English edition; 2005.
15. Behle C. Placement of direct composite veneers utilizing a silicone buildup guide and intraoral mock-up. Pract Periodontics Aesthet Dent. 2000;12(3):259-266.
16. Reshad M, Cascione D, Kim T. Anterior provisional restorations used to determine form, function, and esthetics for complex restorative situations, using all-ceramic restorative systems. J Esthet Restor Dent. 2010;22(1):7-16.
17. Helvey GA. How to increase patient acceptance for cosmetic dentistry: Cosmetic imaging with Adobe Photoshop Elements 4.0. Dent Today. 2007;26(2):148-153.
About the Authors
Jonathan Ferencz, DDS, FACP
Clinical Professor of Prosthodontics
University College of Dentistry
New York, New York
Pasquale Fanetti, RDT
Dental Laboratory Technician
NYC Prosthodontics
New York, New York