Improving Screw-Retained Prosthetics With Elimination of Ti Bases
Utilizing a novel screw concept
Dan Rosen, DDS, and Gregori M. Kurtzman, DDS
Screw-retained restorations, whether single units or hybrid prostheses, have become widely used when restoring implants. Cemented restorations can leave residual cement subgingivally in the sulcus, which may cause inflammation and result in bone loss around the implant crestally via peri-implantitis. Additionally, with a cement-retained restoration, the screw attaching the abutment to the implant may loosen, requiring either access to be created through the restoration or destruction of the restoration to access the screw and tighten it. Screw-retained restorations circumvent the potential subgingival inflammation related to residual cement by eliminating intraoral cementation of the restoration to an abutment. Should the screw loosen, or should the restoration require removal for periodontal maintenance or other reasons, an access channel at the occlusal or lingual portion of the restoration permits access to the fixation screw. The composite sealing the access channel is removed as well as any cotton pellet or PTFE tape, and the screw can be tightened or removed.
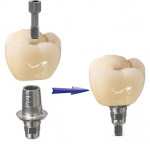
Traditionally, with screw-retained restorations, a Ti base is placed on a laboratory analog on the model at the laboratory. The restoration is fabricated to seat over the Ti base and is luted to the Ti base with a resin cement (Figure 1). It is then returned to the practitioner, who inserts it, tightens the fixation screw (Figure 2), and seals the access channel with either a cotton pellet or PTFE tape, followed by a composite.
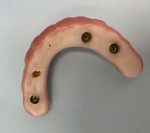
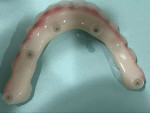
Unfortunately, problems can be encountered with Ti base restorations chairside. The restoration may separate under function from the Ti base to which it was luted. Ti bases available from the implant manufacturers are typically short, so less surface area is present where it is luted to the overlying ceramic restoration. When the prosthesis presents with separation between the Ti base and ceramic of one or more units, the solution is to intraorally relute the crown to the Ti base. This can be a challenge, as the crown may not fully seat onto the Ti base, increasing occlusal contact on the implant restoration and potentially leading to a need to occlusally adjust the restoration; if minor and not felt by the patient, the increased loading on the implant could lead to subsequent bone loss over time. Additionally, if left intraorally, residual cement can lead to periodontal issues as reported with cementable implant restorations. To avoid this, once the crown is recemented on the Ti base intraorally, following set of the cement, the restoration is removed, cement cleaned at the junction of the Ti base and ceramic, and then it is reinserted intraorally. This is a time-consuming procedure chairside. With regard to hybrid prostheses, the entire zirconia portion of the prosthesis is separate from all of the Ti bases intraorally, necessitating an attempt to relute it on the Ti bases intraorally. Yet, in some clinical situations, one or more of the Ti bases may separate while the others remain connected intraorally (Figure 3). This may not be detectable by the patient and will essentially decrease the number of implants that are supporting the prosthesis, as the units that have had Ti base separation will allow micromovement in the vertical access, which may lead to other units undergoing Ti base separation.
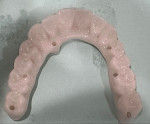
Laboratories have attempted to eliminate the use of Ti bases, having the zirconia contact directly to the multi-unit abutment (MUA) with no metallic component in the prosthesis at the connection (Figure 4). The fixation screws for the implants on the market have a flat bottom designed to seat in the Ti base. This causes stress concentration at the bottom of the screw head, where the zirconia is thin (Figure 5). As stress continues, fracture may result at the thin portion lateral to the MUA or restoration margin, leading to restoration failure (Figure 6 and Figure 7). These screws also do not create tensile loading when placed into the implant with or without a Ti base present, which leads to potential screw loosening, even when torqued to the manufacturer's specifications with a torque wrench.
A New Concept
In order to better serve patients in his practice, the primary author developed a custom solution to address those inherent problems associated with Ti base issues (separation of the restoration from the Ti base), screw loosening, and conventional screws with restoration marginal fracture: a screw that eliminates usage of Ti bases, so that nothing within the restoration is luted that may separate under function over time. This, depending on design, may connect the screw-retained restoration to an MUA on the implant or directly to the implant with no intermittent MUA present. It increases the thickness of the zirconia, decreasing its fracture potential under loading.
The screw has a tapered head, so that the flat bottom of conventional screws is eliminated (Figure 8). When the screw is threaded into the implant through the restoration, lateral tension locks the restoration to the implant, providing tensile load and eliminating potential screw loosening under functional loading (Figure 9). The geometry of the screw head locks the prosthesis and can be achieved with hand tightening alone, without use of a torque wrench. This can be used for prosthetics fabricated from resin, PMMA, graphite, or zirconia. Libraries are available for design of the restorations for milling to accommodate usage of this screw via various CAD software programs.
Restorative Examples
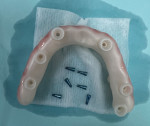
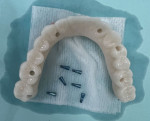
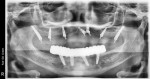
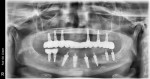
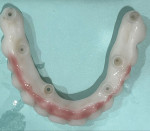
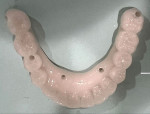
With regard to hybrid restorations, the prosthesis is designed to fit to the MUA, providing thicker material over the MUA to resist fracture potential under loading (Figure 10). The occlusal view of the hybrid prosthesis looks similar to those units using a Ti base, having a small access hole over each implant on the prosthesis (Figure 11). Radiographically, the design demonstrates an intimate fit to the MUA, with increased prosthetic material surrounding the MUA for improved fracture resistance of the prosthesis (Figure 12 and Figure 13).
Case Report
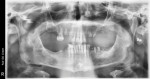
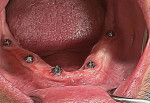
A 54-year-old male patient presented desiring implants to replace failing dentition in both arches. Examination and radiographs confirmed the remaining dentition was in poor condition (Figure 14). Treatment was discussed with the patient to include extraction of the remaining dentition, placement of six implants in the maxilla and six implants in the mandible, and restoration with screw-retained hybrid prosthetics in both arches utilizing a digital workflow with photogrammetry (ICam 4D, Imetric4D).
The patient returned for surgical treatment of the upper arch, which consisted of extraction of the remaining dentition under local anesthetic and placement of implants (Noris Tuff™, Noris Medical Inc) at six sites. MUAs were placed on the implants and the soft tissue was closed with sutures. Impression abutments were placed on the MUAs, and an impression was taken of the arch using a digitally designed and fabricated custom tray (Rosen Tray by Rany Ghobrial, Rosen Tray) that articulated with the teeth in the lower arch. A provisional maxillary hybrid prosthesis was fabricated without Ti bases and attached intraorally with the aforementioned screws developed by the author (Rosen Screw).
In the mandibular arch, the patient was again seen at an appointment, and following extractions, six more implants were placed. The implant at the lower left second premolar had insufficient insertion torque, so it would not be immediately loaded as part of the provisional hybrid prosthesis. As with the maxillary arch, MUAs were placed on the five implants that would be loaded, and an impression was taken with a custom tray to fabricate an immediate mandibular provisional hybrid prosthesis. A provisional maxillary hybrid prosthesis was fabricated without Ti bases and attached intraorally with screws.
The patient returned after 3 months of integration for finalization of the prosthetics. During that period of time, the patient had suffered a minor stroke, and it was decided to not subject him to surgery to uncover the buried implant; the lower prosthesis was functioning well on the five implants that had been loaded. The provisional hybrid prosthetics were removed, and an impression was taken of the implants and healed soft tissue for fabrication of the final zirconia hybrid restorations. The provisional restorations were reinserted, and the impressions were sent to the laboratory for fabrication of final zirconia hybrid prosthetics.
The laboratory designed the restorations in CAD software (DentalCAD, exocad) and utilized high-strength, multilayered zirconia (CopraSupreme Symphony, Whitepeaks Dental Solutions), milling them on a 5-axis dry mill (DWX-52D, DGSHAPE, a Roland Company). The restorations were sintered in a 14-hour cycle, and stained and glazed (GC Initial, GC America Inc).
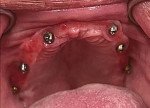
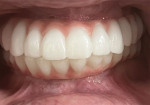
After the laboratory delivered the zirconia hybrids to the dentist, the patient returned for insertion (Figure 15 through Figure 18). The provisional prosthetics were removed from both arches (Figure 19 and Figure 20). The zirconia hybrids were inserted intraorally and fixated with 1.4-mm screws that were tightened by hand. The screw-access holes were then filled with a piece of PTFE tape, sealed with a flowable composite resin, and light-cured. Occlusion was checked and adjusted as needed, completing the treatment (Figure 21).
Conclusion
Screw-retained restorations may present issues related to marginal fracture of the prosthetic material, separation of the Ti base from the overlying restorative material, and screw loosening. The new concept discussed above eliminates those issues with a tapered screw head design and elimination of the Ti base. The screw may be tightened by hand without the need for a torque wrench, and sufficient tensile load is present to prevent screw loosening. This concept cannot be used in single-unit screw-retained crowns, as the MUA offers no anti-rotational mechanism between the crown and MUA, but it can be used effectively with splinted implants either in a bridge or full-arch hybrid prosthesis.
About the Authors
Dan Rosen, DDS
Owner
9 to 7 Dental Office
Panorama City, CA
Gregori M. Kurtzman, DDS
Private Practice
Silver Spring, MD