Decision-Making in Comprehensive Dentistry
Systematic diagnosis, risk analysis, and collaborative treatment planning result in the most conservative treatments for patients
Kris K. Swanson, DDS; and Leon Hermanides, CDT
Dental professionals must consider what types of restorations are required by teeth on a daily basis. These decisions are based on many factors, and they can become more difficult to make when treating complex restorative cases. Regarding the creation of comprehensive treatment plans, restorative dentists are trained to incorporate the most conservative treatment options possible in order to achieve their functional and esthetic goals while benefiting the patient's long-term dental health.1,2 Determining whether it is best to commit a tooth to indirect restorative treatment, provide direct additive treatment or bleaching options, or pursue a combination of these three treatments requires excellent clinical decision-making, and the dental laboratory should be able to provide valuable input. Ultimately, the question of whether or not to use a tooth or teeth as a reference to base a restorative solution around must be answered. This article discusses the many factors that should be considered when making decisions about how to restore individual teeth in comprehensive treatment plans for complex cases.
Analyzing the Risks of Treatment
The cases presented utilize the diagnostic and risk management systems developed by John Kois, DMD, MSD, and taught at the Kois Center in Seattle, Washington. This philosophy relies on four diagnostic criteria—periodontal, functional, biomechanical, and dentofacial—to create a risk profile from which treatment options can be considered without unknowingly negatively affecting a patient's long-term dental health. Each patient's diagnostic risk profile and prognosis are determined from the information provided in his or her medical and dental health history and a thorough clinical examination.1-3 Patient management concerns, finances, and expectations regarding outcomes should also be considered4as well as the skills of the restorative team and its ability to develop and execute a plan to achieve the patient's vision.5 Finally, consideration should be given to the patient's life circumstances and quality-of-life concerns.6
All of the teeth that are periodontally and structurally sound need to be analyzed individually to determine how they relate to the rest of the teeth functionally and esthetically. There are many parameters that a dentist must consider when making these determinations, including the following:
• Patient expectations. Does the patient want a smile that they never had or the smile that they used to have? Is the patient willing to accept reasonable compromise?
• Tooth position. Is the vertical and horizontal alignment of the teeth in the arches and in the smile acceptable? Should orthodontics be considered as an option?
• Vertical dimension of occlusion. Is the vertical dimension being altered, and if so, will it require additive or subtractive measures? How can function and esthetics be best restored with longevity in mind?
• Color/vitality/characterization. Is the tooth color acceptable as is? If necessary, can it be bleached effectively, and will it be easy to match with indirect restorative materials?
• Previous restorations. Are the existing restorations questionable or defective? Can they be restored without negatively impacting the final result?
• Contour. Is the current tooth shape acceptable? Can it be easily modified with selective recontouring and/or direct composite?
• Structural integrity. Is there enough sound tooth structure left to maintain its structural integrity? If so, what is the least invasive restoration that can be placed that will still achieve the treatment goals?
• Black triangles. Has there been a loss of papilla in the anterior region that impacts the esthetics? Can direct composite be used as an additive technique to close the space and maintain the structural integrity of the tooth or are indirect restorations necessary?
• Gingival symmetry. Given the patient's lip dynamics, do the gingival levels exhibit relative symmetry during a normal and Duchenne (ie, exaggerated) smile, and if they are visible, are they pleasing to the eye? Are alterations to gingival levels necessary for esthetics?
• Achievability. Considering the tooth, the patient, the dentist's skill, and the laboratory's skill, is the anticipated outcome predictably achievable?
• Financial considerations. Are there financial constraints that will limit/affect the restorative treatment options or necessary sequence? Does the treatment need to be phased?
• Patient management. Does the patient have any limitations that would impact the ability of the clinician and laboratory to deliver ideal treatment?
When creating a customized treatment plan for a given patient, all of these factors need to be considered for each individual tooth and for the mouth as a whole. The following two case reports will demonstrate the use of the Kois risk management system in making these treatment decisions. Both of the cases, which were completed 5 or more years ago, illustrate how these systems/protocols can achieve predictable, longer-term results when properly used.
Case Report 1
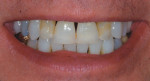
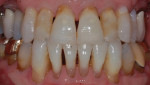
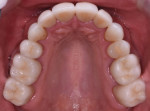
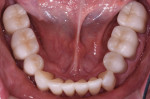
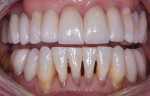
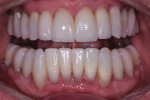
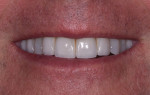
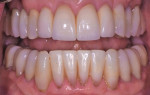
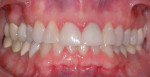
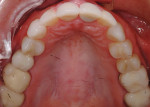
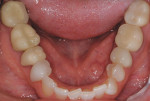
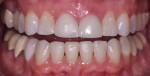
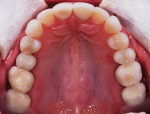
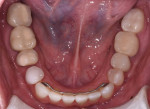
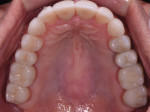
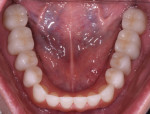
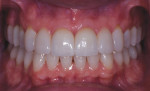
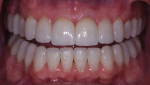
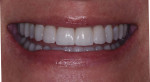
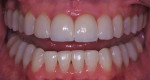
A 52-year-old male patient was referred by the periodontist for restorative rehabilitation. His chief concern was improving the appearance of his smile (Figure 1 and Figure 2). Having just completed clear aligner therapy (Invisalign®, Invisalign), the patient was seeking comprehensive restorative treatment that would be predictable, take the pressure off of his maxillary teeth, and look natural. He reported that he felt self-conscious about his smile and disappointed with his previous dental work. His medical history was noncontributory other than that he had undergone knee replacement, and his dental history indicated that he had received orthodontic treatment as a teenager. Radiographic and clinical examinations were performed, which revealed that he had generalized horizontal bone loss that was moderate in the posterior region and moderate to severe in the anterior region.
The patient's periodontal risk assessment was Stage 3, Grade A, with significant generalized recession, light plaque, and no bleeding, putting him in a category of high periodontal risk. Previously, he had undergone significant gingival grafting in the areas of teeth Nos. 6 to 11, 19 to 22, and 27 to 29. Although his posterior teeth were not clinically mobile, his anterior teeth demonstrated Class I to Class II mobility.
Functionally, the patient's occlusion was acceptable prior to clear aligner therapy; however, completion of the treatment had left him biting heavily on his anterior teeth. This, along with his periodontal condition, was contributing to the mobility of the anterior teeth.
From a structural integrity (ie, biomechanical) perspective, the patient was at high risk due to defective restorations on teeth Nos. 2, 3, 4, 7, 10, 13, 14, 18, 29, 30, and 31 and questionable restorations on teeth Nos. 11, 15, 19, and 20. In addition, teeth Nos. 4 through 13 and 20 through 29 exhibited significant abrasion, tooth No. 3 had recurrent decay, and teeth Nos. 8, 9, and 23 through 26 demonstrated attrition.
During evaluation of the patient's esthetics (ie, dentofacial analysis), he showed no gingival tissue during a normal smile and very little during a Duchenne smile. The patient's maxillary anterior teeth and maxillary occlusal plane were appropriately positioned in his smile; however, it was determined that his mandibular occlusal plane might require alteration due to the height discrepancy between his anterior and posterior teeth. In addition, the generalized loss of papilla around his anterior teeth had resulted in the appearance of significant black triangles.
The patient was informed that teeth Nos. 6, 11, and 13, which had only received minimal Class V bonding, were sound regarding their color, position, and remaining tooth structure and could possibly be treated by replacing the composite only. In addition, it was noted that the mandibular anterior teeth (Nos. 22 through 27) could either be restored with full-coverage restorations or directly bonded to close the large black triangles that were unsightly to the patient. Veneers were not an option due to the presence of significant areas of dentin exposure and the need to prepare through the proximal contacts to close the black triangles.7 Although the patient elected to pursue composite bonding, the cost of treatment was not the overriding factor in his decision. He stated that he preferred the idea of being as conservative as possible to maintain the structural integrity of his teeth, especially if there would be minimal compromise to esthetics, function, or longevity.4
The Treatment
Thorough consultation between the dentist and the laboratory technician was necessary to confirm that the positions of teeth Nos. 6, 11, and 13 would not negatively impact the final result. In addition, because the patient was particular regarding the esthetics and was satisfied with the shade that his natural teeth had achieved from bleaching treatment (Opalescence™ PF [15%], Ultradent), it was critical for the laboratory to evaluate if it would be able to closely match the color and vitality of these natural teeth with indirect restorations.8 When presenting conservative treatment options for the mandibular anterior teeth, it is of the utmost importance that the restorative dentist has the knowledge and skill necessary to use direct composite to close back triangles and idealize contours.5
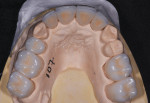
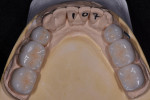
After significant evaluation and discussion, a comprehensive treatment plan was proposed and accepted. Because there were several existing composite restorations, significant dentin exposure, and proximal black triangles, full-coverage lithium disilicate restorations were fabricated for teeth Nos. 7 through 10 (IPS e.max®, Ivoclar Vivadent). Alteration of the vertical dimension was achieved with full-coverage lithium disilicate crowns on teeth Nos. 2 through 4, 14 and 15, 18 through 20, and 29 through 31.9 More specifically, the mandibular posterior occlusal plane was raised by 1 mm to 1.5 mm. By opening the vertical dimension, the heavy contact of the anterior teeth could be relieved without requiring significant reduction of the palatal surfaces of the maxillary incisors (Figure 3 through Figure 6).
In order to achieve bilateral simultaneous contacts on the posterior teeth, the occlusion was equilibrated using a deprogramming appliance (Kois Deprogrammer, Kois Center).10 Direct composite restorations were performed on teeth Nos. 6, 11, and 13 to replace the existing Class V composite restorations, and minimal incisal bonding was performed on teeth Nos. 6 and 11 to refine the occlusal plane (Tetric EvoCeram®, Ivoclar Vivadent; Tetric EvoFlow®, Ivoclar Vivadent). Finally, the closure of the black triangles and restoration of the incisal edges of teeth Nos. 22 through 27 was accomplished with direct composite bonding (Figure 7 through Figure 10).
Case Report 2
A 49-year-old female patient who was referred to the practice presented with difficulty chewing, chronic headaches, and occasional temporomandibular joint pain. She was also unhappy with the overall appearance of her teeth. After a review of the patient's medical and dental history, a comprehensive clinical examination was performed.
The patient, who received a periodontal risk assessment of Stage 1, Grade A, demonstrated minimal bone loss and was showing signs of a violation of biologic width at the margin of the restoration on tooth No. 9. She also displayed a thin gingival biotype on the mandibular arch.11
Biomechanically, due to the number of teeth that were previously restored with full-coverage restorations and concerns regarding the structural integrity of the patient's teeth, she was considered to be at a moderate risk for tooth loss. The patient also presented with active caries on tooth No. 14 as well as defective restorations on teeth Nos. 3, 14, 29, and 31. Significant to the design of the treatment plan for this patient was the fact that her maxillary cuspids and bicuspids had undergone minimal restorative dentistry and had a good prognosis (Figure 11 through Figure 14).
An evaluation of the answers to the questions in the patient's dental history and the attrition patterns on her teeth resulted in a diagnosis of occlusal dysfunction.3 Although an equilibration to improve the bilateral simultaneous contact of her posterior teeth would have been an appropriate treatment, the positions of her anterior teeth were not favorable to create an ideal result. This was primarily due to the proximity of the maxillary and mandibular anterior teeth (vertical and horizontal overlap) as well as their rotations, positions, and proportions. To create a more ideal occlusion in this case, orthodontic tooth movement was considered an appropriate treatment modality. The patient agreed to an orthodontic consultation and subsequently underwent orthodontic therapy to reposition the teeth into a more favorable occlusion. In addition, the orthodontic treatment served to resolve the biologic width violation associated with tooth No. 9.
Following orthodontic treatment, the patient's chief concern was the color of her teeth, and she was also interested in what she could do to further improve her smile and create a natural looking result. She was reevaluated to identify key dentofacial concerns. When evaluating the patient's repose (ie, lips at rest) photograph, it was determined that her maxillary cuspids were in a favorable position,12 but her incisors would benefit from approximately 1 mm of additional length. The apical position of the soft tissue associated with teeth Nos. 8 and 9 was approximately 1 mm to 1.5 mm coronal of the ideal; however, this discrepancy was not visible in her smile.
Due to the patient's low-risk periodontal condition, the gingival asymmetry of her maxillary anterior teeth could be treated with either clinical crown lengthening, orthodontic tooth movement, or a combination of both. In this case, after orthodontic tooth movement was completed, intrasulcular clinical crown lengthening was required to visually even out the tooth lengths of teeth Nos. 8 and 9. In order to maximize the esthetic results, the decision was made to perform the intrasulcular crown lengthening at the time of tooth preparation (Figure 15 through Figure 17).
The Treatment
After the orthodontic phase, the patient returned for her restorative treatment. She was encouraged to complete tooth whitening protocols (Opalescence™ PF [15%], Ultradent) for both the maxillary and mandibular teeth as soon as possible to achieve the brightness she desired and to allow for any relapse of the color. Because the tooth whitening procedures achieved a satisfactory result, the teeth with good prognoses (Nos. 5, 6, 11, and 12) would not require indirect restorations. These teeth received limited direct restorations to enhance their esthetic appearance.
The treatment plan, which was collaboratively developed by the restorative dentist and the laboratory technician, was agreed to by the patient. It involved restoring teeth Nos. 7, 8, 9, and 10 with conservatively prepared lithium disilicate (IPS e.max®, Ivoclar Vivadent) veneers/full coverage restorations and restoring the maxillary posterior teeth Nos. 2, 3, 4, 14, and 15 with indirect lithium disilicate restorations. The mandibular anterior teeth received limited direct composite restorations (Tetric EvoCeram®, Ivoclar Vivadent; Tetric EvoFlow®, Ivoclar Vivadent) to restore the incisal edges; however, the patient elected not to treat the black triangle between teeth Nos. 24 and 25 because it did not show in her smile. The mandibular posterior teeth were also restored with full-coverage lithium disilicate restorations. The existing implant at the site of tooth No. 13 was restored with a new CAD/CAM abutment (TruAbutment DS, TruAbutment) and a CAD/CAM multilayer zirconia restoration (Cercon® ht ML, Dentsply Sirona). This treatment allowed the maxillary occlusal plane to be idealized and slightly increased the vertical dimension to improve the anterior tooth relationship (Figure 18 through Figure 23).
Conclusion
Being able to smile with confidence is a quality-of-life benefit for patients.4 Understanding how to best develop the esthetic parameters in order to restore a pleasing smile requires evaluating objective measures of tooth position, lip position and travel, facial landmarks, proportions, and symmetry. When devising a comprehensive treatment plan for a patient who requires extensive restorative care, decisions regarding individual teeth should be made using a collaborative model. During the last 5 years, the patients from both of the cases presented have returned for ongoing preventive maintenance free of complications and with improved long-term dental health (Figure 10 and Figure 24). They have stated that they are extremely satisfied. Both cases illustrate the use of these diagnostic and risk management concepts that have proven to be predictably successful for many other patients.
References
1. Kois JC. New challenges in treatment planning: incorporating the Fundamentals of patient risk assesment- part 2. J Cosmetic Dent. 2011;27(1):110-121.
2. Kois JC. New challenges in treatment planning: shifting the paradigm toward risk assessment and perceived value- part 1. J Cosmetic Dent. 2011;26(4):62-69.
3. Huff C. A systematic method for accurate functional diagnosis. Compend Contin Educ Dent. 2017;38(5):308-316.
4. Sweier DG, Heys RJ, Truhlar MR, Bayne SC. Treatment planning for seniors with financial limitations. Decisions in Dentistry. 2015;Sept/Oct.
5. Swanson, K. Conservative cast gold inlays. Inside Dentistry. 2020;16(8):18-23
6. Baiju RM, Peter E, Varghese NO, Sivaram R. Oral health and quality of life: current concepts. J Clin Diagn Res. 2017;11(6):ZE21-ZE26.
7. Swanson K. Predictable, conservative closure of black triangles. Inside Dentistry. 2018;14(12):32-38.
8. Haywood VB. Considerations for vital nightguard tooth bleaching with 10% carbamide peroxide after nearly 20 years of proven use. Inside Dentistry. 2006;2(7).
9. Kois JC, Phillips KM. Occlusal vertical dimension: alteration concerns. Compend Contin Educ Dent. 1997;18(12):1169-1177.
10. Jayne D. A deprogrammer for occlusal analysis and simplified accurate case mounting. J Cosmetic Dent. 2006;21(4):96-102.
11. Van’t Spijker A, Kreulen CM, Bronkhorst EM, Creuger NH. Occlusal wear and occlusal condition in a convenience sample of young adults. J Dent. 2015;43(1):72-77.
12. Misch CE. Guidelines for maxillary incisal edge position—a pilot study: the key is the canine. J Prosthodont, 2008;17(2):130-134.
13. Arora R, Narula SC, Sharma RK, Tewari S. Supracrestal gingival tissue: assessing relation with periodontal biotypes in a healthy periodontium. Int J Periodontics Restorative Dent. 2013;33(6):763-771.
About the Authors
Kris K. Swanson, DDS
Swanson Dental Associates
Bellevue, Washington
Leon Hermanides, CDT
Protea Dental Studio
Redmond, Washington