Biomechanics and Function
Altering paradigms for treating a patient’s esthetic disability
By Kris Swanson, DDS, and Leon Hermanides, CDT
When evaluating a patient's smile and dentition for treatment, the starting point should always be a comprehensive and systematic risk assessment. This risk assessment becomes the compass, guiding treatment decisions to achieve a predictable, long-term outcome.1,2
An understanding of the biologic consequences of tooth preparation should inform any decisions about restoration design and material selection. It is not in the best interests of the health of the patient's dentition to decide what material to use and then recommend a tooth reduction requirement without first taking into account the compromised structural integrity of the remaining tooth. The challenge to any technician is to manage the esthetics of a case within the framework of limited tooth structure removal while also accommodating the requirements of the material.
Case Overview
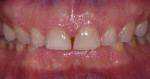
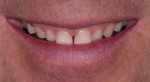
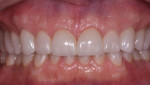
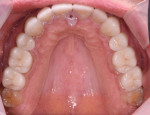
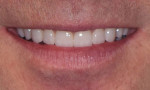
A male patient presented requesting larger, whiter teeth and was concerned about his anterior teeth chipping and breaking (Figure 1). He refused orthodontics because of his professional public speaking engagements but was willing to do anything else to have a "million dollar smile" (Figure 2). Using the Kois risk assessment and treatment planning protocol,1,2 a conservative plan was developed utilizing a combination of direct composites, full-coverage crowns, and some minimally prepared additive veneer onlays (AVOs). These additive onlays proved to be critical in achieving both the functional and the esthetic goals of the treatment.
Medical and Dental History
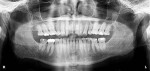
The patient's medical history revealed no significant concerns or contributors to his dental health. Upon examination, there was significant attrition and some evidence of erosion present (Figure 3). The patient tested negative for acid reflux, and it was determined that no dietary contributors for erosion existed. The patient's dental history included orthodontics from ages 15 to 17. He reported worn, chipped anterior teeth and that he needed to squeeze to get his posterior teeth to come together. The patient was very self-conscious about his smile, and after reviewing a historical photo, it became apparent he was asking for a smile he had never had.
Diagnosis, Risk Assessment, and Prognosis
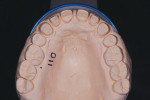
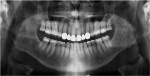
The patient had no evidence of periodontal disease and was thus considered low risk (Stage 1, Grade A) for periodontal disease with a good prognosis (Figure 4).
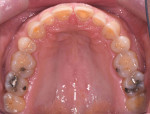
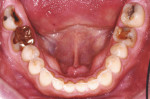
The patient presented with no active caries, but did have defective amalgam restorations, a missing onlay, structural compromises, and a broken tooth (No. 31). His anterior teeth presented with severe attrition and areas of erosion. The risk for tooth loss from structural concerns was moderate with a poor prognosis. Any aggressive tooth preparation protocol would result in an increased risk of damage to the structural integrity of his teeth (biomechanics), and this influenced many of the decisions regarding the restoration design and treatment protocols.
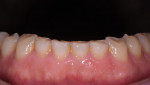
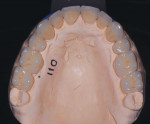
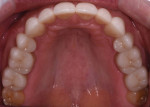
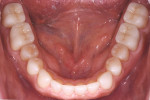
Severe attrition was evident on the palatal side of the maxillary anterior teeth and labial surfaces of mandibular anterior teeth (Figure 5 and Figure 6). This suggested a constricted chewing pattern which was confirmed by the positive answers on his dental history and the pattern of attrition on his anterior teeth.3,4 This placed him at moderate risk of tooth structure loss for functional concerns (normal forces) with a poor prognosis.
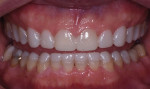
During both a normal and Duchenne smile, the patient demonstrated a "gummy" smile, small teeth, and a deficient buccal corridor (Figure 7). From the initial appointment, the patient made it clear that he had specific esthetic requirements due to his frequent public speaking engagements. He wanted his teeth to look larger and whiter, and to show less gingiva when he smiled. For the patient, this was a quality-of-life issue that he considered a disability.5 The esthetic risk for this patient, based on the visible tooth and gum in his smile, was high with a hopeless prognosis.
Treatment Goals
The treatment plan was designed to create a pleasing esthetic outcome, treat the constricted chewing pattern (CCP), and establish bilateral simultaneous posterior tooth contact. This would involve clinical crown lengthening for the maxillary anterior teeth and opening the vertical dimension6 with a combination of direct and indirect restorations in order meet his functional and esthetic demands without significantly raising the biomechanical risk.
Phase 1 Pre-Treatment: Deprogramming, Wax-up, and Consult
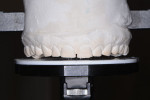
After wearing a Kois Deprogrammer for 3 weeks, a bite registration was taken in centric relation, and the Kois Dento-Facial Analyzer was used to locate the casts on a Panadent articulator. A diagnostic wax-up was then virtually designed using the Kois 10-step diagnostic approach. Ideal maxillary and mandibular incisal positions were used to determine the vertical dimension. Bilateral simultaneous centric contacts were established on the posterior teeth, and the envelope of function was flattened by increasing the occlusal vertical dimension (OVD). This would relieve the CCP, reduce the overbite, and allow for more ideal tooth proportions.
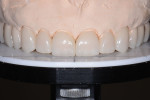
Polyvinyl siloxane (PVS) putty matrixes of both arch wax-ups were fabricated. A consult was then scheduled with the patient to present the proposed treatment plan. During the consult, the wax-up was tried in using Luxatemp (DMG America) and PVS matrices.7 On seeing the mock-up in his mouth and what his new smile would look like, the patient was thrilled and immediately accepted treatment (Figure 8).
Phase 2: Clinical Crown Lengthening and Bleaching
Using the Luxatemp temporary stents as a surgical guide, the patient had clinical crown lengthening (approximately 1 mm) in the periodontist's office. This procedure was necessary to achieve a less "gummy" smile. A 3-month healing period followed, during which the patient was able to use a custom tray to bleach his lower teeth.
Phase 3: Tooth Preparation and Provisionalization
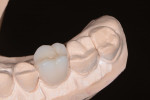
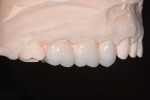
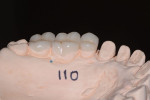
In the first appointment, the maxillary restorations were prepared and direct composite bonded to the lower teeth, and provisional restorations were fabricated from the PVS matrices (of the diagnostic wax-ups). The minimally prepared posterior AVOs required no interproximal reduction and were left mostly in enamel. These ultraconservative restorations retained the structural integrity of the teeth,8 facilitated opening the OVD, and filled out the buccal corridor, giving the patient the broad, full smile he envisioned (Figure 9 through Figure 12).
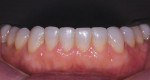
With financial considerations in mind—and in an effort to remove as little tooth structure as possible—direct bonding was completed on teeth Nos. 20 to 29 (Figure 13).9 The matrices were used to transfer the precise anatomy and occlusion of the diagnostic wax-up to the mouth.
The patient returned a week later to evaluate his provisional restorations. New photographs were taken to confirm esthetics and make any necessary adjustments to the final restorations during fabrication. In order to capture an occlusal record as close to the final OVD as possible, a small anterior deprogrammer was bonded to the palatal surface of the provisional between the maxillary centrals, slightly separating the posterior teeth by 0.5 mm. After removing the posterior provisional restorations, the record was taken using a PVS bite material (Regisil Rigid, Dentsply Sirona). Study models were made of the provisional restorations with a new facebow registration to transfer the information to the dental laboratory.
Phase 4: Fabrication and Seating of Indirect Restorations
PVS impressions (Aquasil, Dentsply Sirona) of the patient's prepared teeth and provisional restorations were poured in a Type IV die stone and scanned with a digital scanner. The restorations were virtually designed using the provisional restorations as a guide. The designs were then milled in zirconia and lithium disilicate and verified using dies, articulated working casts, and solid models for complete seating (fit), occlusion, and proximal contacts. The anterior restorations were micro-layered on the facials to replicate the natural dentition, while the posterior restorations were completed as monolithic prostheses to maintain the structural integrity of the material. The intaglio surfaces were prepared for delivery according to the manufacturer's recommendations (Figure 14).
The maxillary restorations were seated first (Figure 15).10 The anterior full-coverage restorations were fabricated in zirconia to keep the palatal surface as thin as possible, thus requiring less tooth reduction (Figure 16 and Figure 17). The crowns were seated using a self-adhesive resin cement (RelyX Unicem 2, 3M Oral Care). Next, the posterior lithium disilicate (IPS e.max, Ivoclar Vivadent) AVOs were seated using an adhesive bonding protocol (All-Bond 2, Bisco, and Variolink Esthetic, Ivoclar Vivadent). Finally, a new PVS impression was made of the mandibular preparations, and a bite registration was taken of the completed maxillary arch relationship to the mandibular preparations utilizing a 3D printed Kois Deprogrammer (Figure 18 and Figure 19).7
The patient returned several weeks later for the seating of the mandibular molar crowns (Figure 20). The printed deprogrammer was used to adjust the occlusion into bilateral simultaneous posterior contact.10 Impressions were taken for a maxillary nightguard and seated at a follow-up appointment. The patient asked to have the nightguard fabricated as he had always worn one, and he perceived it would protect his investment.
Discussion
As the patient's periodontal risk was classified as low, clinical crown lengthening provided the apical tooth length for the maxillary anterior restorations. These teeth required cohesively retained, full-coverage ceramic restorations due to the exposed palatal dentin. With the incisal edges requiring additional length, no additional incisal tooth reduction was required to meet his esthetic needs (Figure 21).
Space for maxillary anterior restorative materials was managed with increased tooth length, a change in vertical dimension, and the choice of restorative materials, thereby protecting the structural integrity of the teeth. A negative curve in the patient's maxillary posterior occlusal plane and the change in OVD provided sufficient interocclusal space for restorative materials on the maxillary posterior teeth (Figure 22).
Minimal axial reduction was needed to enhance the buccal corridor (horizontal volume) due to the additive capability of the AVOs and the slight palatal inclination of the posterior teeth. Using lithium disilicate with minimal occlusal reduction, it is possible to increase the vertical dimension restoratively without increasing biomechanical risk to the teeth.8 These preparations are kept mostly in enamel and are bonded using adhesive bonding protocols.
Conclusion
This treatment was successful for the patient in altering the visible tooth display in his smile and the size and proportion of his teeth with few anticipated long-term complications (Figure 23). Since this case was completed, the patient has had two 6-month recall appointments without reported complications. This case was a clinical success as the needs of the patient were met (his disability was treated) without increasing the risks for predictable negative outcomes for his dentition (Figure 24).
The patient shared how his new smile had changed his professional outlook and self-image: "At this point in my career, this has given me such a deep appreciation of the power of the simple smile. I feel so much better about my appearance and have a quiet confidence that counts when it really matters."
Acknowledgments
The authors thank John C. Kois, DMD, MSD, for providing the structure and fundamental protocols to create the vision necessary to treat this case successfully, as well as Protea Dental Studio for the indirect restorations.
About the authors
Kris Swanson, DDS
Kois Center Mentor
The Kois Center
Private Practice
Bellevue, WA
Leon Hermanides, CDT
Clinical Instructor and Scientific Advisor
The Kois Center
Owner/President
Protea Dental Studio
Redmond, WA