Effective Utilization of Pink and White Esthetics in Smile Design
Soft tissue framework for anterior implants
Nantawan Kolakarnprasert, DDS; Richard Trushkowsky, DDS; Anabella C. Oquendo Parilli, DDS; Fadwa Alharthy, BDS, MS; and Peter Pizzi, CDT, MDT
Dental implants are currently considered the optimal means of replacing missing teeth.1 While conventional fixed partial dentures (FPDs) or adhesive FPDs are certainly deemed viable alternatives, if no adjacent teeth need to be involved in the restoration, their preparations may be considered invasive and, ideally, should be avoided. In addition to reestablishing function, a goal of tooth replacement should be the creation of an attractive smile. To achieve an esthetic result, adequate dimensions of both hard and soft tissue must be present, and if they are not, an attempt should be made to regenerate lost structures.2 The most common reconstructive therapy is guided bone regeneration (GBR). If soft-tissue augmentation is needed, an additional surgical procedure may be required. Occasionally, hard- and soft-tissue surgery may be combined with implant placement in one visit.3
One of the most difficult esthetic problems to correct is loss of gingival papilla and the alveolar ridge, which may be due to a variety of reasons. In its ideal form the gingival papilla serves to outline the size and shape of the tooth. Failure to reconstruct lost papilla can significantly modify the tooth contour. The interdental form of the papilla in the apicocoronal location is important in the creation of an ideal gingival architecture.4 The absence of interdental papilla may result in a number of problems, including esthetic compromise, food impaction, and phonetic impairment.5
In 1999, Jemt presented a papilla index that is based on the level of interproximal mucosa next to single-implant reconstructions.6 An additional index using visual analog scales was introduced for assessment of both the peri-implant mucosa and implant-supported crown.7 Numerous other indices to assess peri-implant soft tissue and the implant-supported restoration were proposed in later investigations, including the Implant Crown Aesthetic (ICA) index,8 the subjective esthetic score,9 the pink esthetic score (PES),10 the pink esthetic score/white esthetic score (PES/WES),11 the complex esthetic index,12 and the Copenhagen index score.13 Currently, the PES and PES/WES are the most-often used indices for single implants.14
In addition to papilla, sufficient volume of both supporting bone and soft tissues is required to achieve an ideal esthetic outcome.15,16 In cases where there is substantial facial bone loss and soft-tissue loss as a consequence of infection or trauma, regeneration of these lost tissues must be attempted. However, surgical procedures may not always successfully restore these lost tissues, and creative prosthetic solutions sometimes are necessary. In diagnosis and treatment planning, a prosthesis with an artificial gingiva may be considered, as it potentially can provide a more amenable result while requiring minimal or no surgical intervention. Also, Malament et al found that the use of pink porcelain allowed the technician to mimic the curves of normal mucosa and enabled the formation of ideal gingival symmetry.17
In the laboratory, creating "pink" ceramics can be challenging, as light reacts to tissue quite differently than it does to tooth structure, but it can certainly be achieved. Although technicians are always working toward optimizing the light interaction of their restorations, creating depth in pink ceramic tissue requires communicating much more shade information. Ceramic layering is also needed to create depth in minimal space, to enhance esthetics, and to be hygienic. Applying pink ceramic in limited space is one of the most difficult requirements in ceramics.
The following case report describes how achieving proper pink and white balance with appropriate planning may require a combination of procedures, and that to establish ideal pink and white esthetics, it is sometimes necessary to use prosthetic means to supplement surgical procedures.
Case Presentation
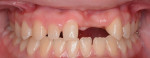
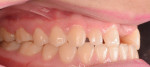
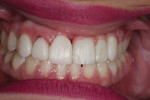
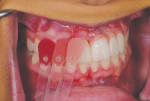
A 20-year-old female patient was referred to the Advanced Program for International Dentists in Esthetic Dentistry at New York University, Department of Cariology and Comprehensive Care by the school's Ashman Department of Periodontology and Implant Dentistry for fabrication of an implant-supported restoration in the No. 9 position. Her chief complaint was the appearance of her teeth and she desired an improved smile (Figure 1 and Figure 2).
The patient had undergone orthodontic treatment for 5 years. She had presented in the orthodontic clinic exhibiting a class III molar and canine relationship, proclined incisors, anterior cross-bite and reverse overjet and overbite, and congenitally missing upper left central and lateral incisors, teeth Nos. 9 and 10. The lower arch had been leveled and aligned first, then a bite plate had been placed to open the bite allowing brackets to be placed in the maxillary arch. This enabled correction of the midline but left spacing in the upper left anterior.
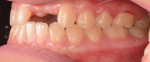
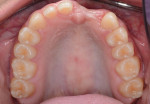
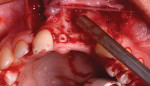
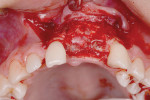
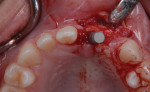
The patient was then referred to the Ashman Department of Periodontology and Implant Dentistry for restoration of inadequate vertical and horizontal hard and soft tissue in the upper left central and lateral incisor region (Figure 3 through Figure 6) and subsequent implant placement. She was anesthetized with three carpules of lidocaine 1:100,000. Vertical releasing incisions were placed by teeth Nos. 8 and 11, and a full-thickness flap was elevated. Bone decortication was performed and five tags made (Figure 7). Ultrasound-activated pins (SonicWeld Rx®, KLS Martin, klsmartinnorthamerica.com) were used to stabilize foil panels (Resorb-x®, KLS Martin) comprised of a polymer consisting of 100% amorphous, noncrystalline poly-D,L-lactic acid (PDLLA).
The essential component of this procedure is the ultrasound generator (SonicWeld Rx) that is used to produce ultrasonic waves of precisely defined frequency, which are then brought into focus with a sonotrode. The SonicPin Rx® (KLS Martin) is picked up with the sonotrode tip and placed onto a pilot hole. When the ultrasound generator is activated, the pin is set through vibration via the sonotrode. Heat is generated by the friction between the vibrating pin and the bone surface, liquefying the pin's exterior and enabling the pin to glide into the hole. By varying the state of aggregation, the pin even penetrates into bone cavities that typically cannot be reached using conventional procedures. Additionally, the head of the SonicPin Rx bonds with the Resorb-x foil or membrane to create a 3-dimensional construction.18 Combined with the use of a shell technique19 these properties produce new dimensions in horizontal and vertical augmentation. The foil panel polymer is inclined to hydrolysis due to the totally amorphous structure and gradually loses strength before metabolism. Resorption time observed in ultrasound follow-up was 12 to 30 months.20,21
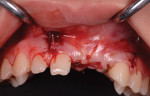
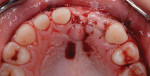
Bone substitute (Bio-Oss®, Geistlich Biomaterials, dental.geistlich-na.com) in the form of 0.2-cc large-particle (1 mm to 2 mm) cancellous granules was placed, and a resorbable bilayer collagen membrane (25 mm by 25 mm) (Bio-Gide®, Geistlich Biomaterials) was used to cover and stabilize the area (Figure 8). Tissue was closed with 4-0 chromic and 5-0 gut sutures (Figure 9 and Figure 10). The patient was instructed to use an Essix appliance instead of an acrylic removable provisional. After initial healing, the removable appliance was relieved and the patient used it for esthetic purposes. A 4.1-mm by 12-mm implant (Straumann® Bone Level Implant, Straumann, straumann.com) was placed at site No. 9 (Figure 11). Three months later a midcrestal incision over the No. 8-9 position was made for the removal of the cover screw and placement of a healing abutment followed by a temporary acrylic crown.
Subsequent to the implant placement, the patient presented to the NYU Department of Cariology and Comprehensive Care. She filled out an NYU esthetic evaluation form, enumerating her desired changes on the form. Extensive photographs, study models, and centric bite were obtained. The photographs consisted of both full-face and intraoral images.
Impressions for the study models were taken with vinylpolysiloxane (VPS) impression material (Reprosil® Putty and Reprosil® Regular Body, Dentsply Sirona, dentsplysirona.com) to create precise models. The models were then mounted with a facebow and articulator (Artex®) in centric relation, which had been determined using a leaf gauge. The patient had vertical bone loss between the mesial of tooth No. 8 and the mesial of tooth No. 11 prior to implant placement. The patient was presented the choice of either restorations with pink porcelain or additional surgeries to try to correct the vertical defect. She chose the prosthetic solution.
First, bleaching was done with a hydrogen peroxide, in-office whitening gel (Opalescence® Boost PF 40%, Ultradent Products Inc, ultradent.com), 20 minutes three times, on all maxillary and mandibular teeth not involved with the restorations. The patient's shade changed from A.3 to A.2.
After a diagnostic wax-up was preformed, a provisional restoration was made with bisacryl provisional material (Luxatemp®, DMG America, dmg-america.com) shade B1, and pink acrylic was added in the gingival area of No. 10 to simulate gingival tissue. The subgingival component of the abutment was also contoured to develop the proper emergence profile for the implant-supported restoration. This later was duplicated in the impression, which was used to assess whether the patient's concerns were being met and to provide guidance to the laboratory for the final restoration. A new wax-up was obtained from Nos. 6 through 11 for the purposes of closing spaces and improving proportions. A new laboratory-fabricated provisional then was made that incorporated these changes, with a temporary crown over the implant and with No. 10 cantilevered (Figure 12 and Figure 13). This approach enabled the patient to appreciate the potential of the proposed treatment.
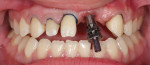
An impression coping was fitted to No. 9 and the fit was checked with an x-ray (Figure 14). To reproduce the gingiva, an implant analog with the temporary crown was placed at the center of a small disposable medicine cup. Wax was utilized on the bottom of the cup to hold the implant analog. Impression material was injected into the cup covering the laboratory analog and the gingival third of the temporary crown. The temporary crown was unscrewed and replaced with the appropriate impression coping. Using a flowable composite resin, the space between the impression coping and impression material was filled.
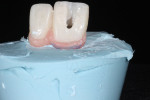
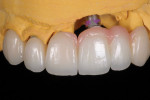
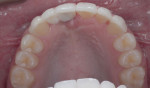
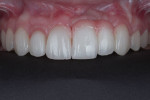
After the material set, the impression coping was removed and placed in the patient's mouth.22 Full-arch impressions were obtained of the maxillary and mandibular arches using heavy- and light-body polyether impression material (Impregum™ and Permadyne™, 3M Oral Care, 3m.com). The patient was sent to the laboratory to select final teeth shade and gingival porcelain. Final restorations consisted of window veneers for teeth Nos. 6 and 7, a porcelain laminate window veneer for tooth No. 8 with pink porcelain on the mesial to replace papilla, and a zirconia crown for tooth No. 9 with a cantilevered pontic with pink porcelain in the cervical areas. At the laboratory, both white and pink shades were addressed and photographs were taken for future reference (Figure 15 through Figure 18).
The veneers were returned from the laboratory and evaluated on the cast. The final restorations were tried in the mouth with the use of water, and the patient gave approval to proceed with cementation of the restorations. The internal surfaces of the veneers were etched for 90 seconds using 9% hydrofluoric acid gel (Ultradent® Porcelain Etch, Ultradent Products Inc), then thoroughly rinsed with water and cleaned with an alcohol solution in an ultrasonic device for 1 minute. Silane (Ultradent Products Inc) was placed on the internal surface of the veneers for 60 seconds and allowed to air-dry. The teeth were isolated with a lip and cheek retractor (OptraGate®, Ivoclar Vivadent, ivoclarvivadent.com) and cotton rolls. Size #000 cord (Ultrapak™, Ultradent Products Inc) was placed in the sulci, and Teflon® tape was placed at the mesial aspect of tooth No. 5 and the mesial of tooth No. 12 to protect those teeth. Bonding agent (Prime&Bond elect®, Dentsply Sirona) was applied to the dry surfaces of the laminates and its solvent was allowed to evaporate. Teeth Nos. 7 through 9 were etched for 15 seconds and rinsed for 30 seconds, bonding agent (Prime&Bond elect) was applied, and the solvent was allowed to evaporate.
Transparent shade composite (Variolink® II Base, Ivoclar Vivadent) was applied to the laminates, which were then seated on the teeth. The restorations were then tack-cured for 5 seconds, and excess partially cured cement (Variolink® Esthetic, Ivoclar Vivadent) was removed with an explorer. The restorations were then light-cured for 60 seconds. Any excess cement was removed and the occlusion verified. This was followed by final polishing. The process was repeated for tooth No. 11.
The implant abutment was screwed into placed and checked with an x-ray. The bridge was seated over the implant and the fit was checked. After the patient's approval, the abutment was screwed in place to a torque force of 35 Ncm. Teflon tape was placed inside the screw opening and a resin cement was placed in the crown of the cantilever bridge. The bridge was seated and the restoration was then tack-cured for 5 seconds. The excess cement (RelyX™ Unicem, 3M Oral Care) was removed with an explorer prior to light-curing for 60 seconds. An occlusal guard was fabricated to provide protection of the restorations. The final results, demonstrating the esthetic potential of proper utilization of pink porcelain for the restoration of lost soft-tissue volume, are shown in Figure 18 through Figure 22.
Discussion
The restoration of dental implants in the anterior maxilla should be both esthetic and functional; therefore, the 3-dimensional aspects of peri-implant hard and soft tissue must be considered.23 To do so requires a thorough understanding of the fundamental biological processes of bone and soft-tissue remodeling that occurs subsequent to tooth extraction.24 Excellent implant restoration demands both a visually attractive outcome and healthy and well-scalloped gingival tissue. Restoring hard- and soft-tissue outlines is often challenging. Ideally, the interdental papilla should closely resemble the adjacent dentition.25,26 Vertical and horizontal ridge augmentation using GBR is often a treatment option. Vertical bone augmentation to provide bone support for implants and enhance soft-tissue architecture is more difficult to achieve than horizontal bone augmentation. However, Urban et al reported that the use of bone-inductive growth factors may enhance the progress of mature lamellar bone, stating that purified recombinant platelet-derived growth factor-ßß used in combination with a deproteinized bovine block without a barrier membrane may possibly allow regeneration of a substantial amount of bone.27
In this clinical case, adequate soft-tissue volume had not been achieved, and the patient did not want to undergo additional surgery with a questionable outcome. A prosthesis that incorporated a pink element was needed to establish a more ideal PES/WES index. A variety of materials can be utilized for this purpose, including composite, resin, and pink ceramic. The use of acrylic and composite can enable a good color match and has the capability of being applied intraorally. A drawback of these materials, however, is the degradation that occurs over time requiring ongoing maintenance. There are available gum and gingiva shades (eg, GRADIA®, GC America, gcamerica.com; Anaxgum®, Anaxdent North America, anaxdentusa.com, and VITA) that are tissue-colored composites used for the esthetic rebuilding of gingival components. These materials can be applied by the dental technician in the laboratory or directly in the patient's mouth by the dentist. In this case, pink ceramic was the option selected, but obtaining a good color match to the surrounding soft tissue is not always readily achieved.28-32
Conclusion
Dental restorations that incorporate artificial gingiva are often indicated for patients with both horizontal and vertical defects. The main disadvantage in such cases is a complex prosthetic solution and the need for strict hygiene maintenance by the patient. The patient's lipline typically is a major consideration. A high lipline usually will display a significant amount of gingiva and require ideal papilla. Even a medium lipline will display the tips of the papilla, an issue that will need to be considered in the final restoration. A recent study demonstrated lip form in repose influences incisal and papilla display.33 Ridge restoration for implant placement may not provide sufficient tissue to develop papilla and, if this is the case, a prosthetic solution should be considered at the outset. Partial-defect cases may be considered as unilateral or bilateral. As in this case, unilateral cases can be more difficult to treat because there is an esthetic comparison to the contralateral side. Cases with missing papilla between the central and lateral incisors, especially long papilla of a thin biotype, are the most problematic.34
About the Authors
Nantawan Kolakarnprasert, DDS
Resident
Advanced Program for International Dentists in Aesthetic Dentistry
New York University College of Dentistry
New York, New York
Richard Trushkowsky, DDS
Clinical Professor
Cariology and Comprehensive Care
Associate Director
Advanced Program for International Dentists in Aesthetic Dentistry
New York University College of Dentistry
New York, New York
Anabella C. Oquendo Parilli, DDS
Clinical Assistant Professor
Cariology and Comprehensive Care
Director
Advanced Program for International Dentists in Aesthetic Dentistry
New York University College of Dentistry
New York, New York
Fadwa Alharthy, BDS, MS
Resident
Ashman Department of Periodontology and Implant Dentistry
New York University College of Dentistry
New York, New York
Peter Pizzi, CDT, MDT
Faculty
New York University
College of Dentistry
Advanced Program for International Aesthetics
New York, New York
Owner
Pizzi Dental Studio Inc.
Staten Island, New York
References
1. Baltacioğlu E, Korkmaz YT, Korkmaz FM, Bağiş N. A combined peri-implant plastic surgery approach for implants in the esthetic zone using a novel technique: a series of 10 cases. Quintessence Int. 2016;47(4):307-318.
2. Fagan MC, Owens H, Smaha J, Kao RT. Simultaneous hard and soft tissue augmentation for implants in the esthetic zone: report of 37 consecutive cases. J Periodontol. 2008;79(9):1782-1788.
3. Deliberador TM, Vieira JS, Bonacin R, et al. Connective tissue graft combined with autogenous bone graft in the treatment of peri-implant soft and hard tissue defect. Quintessence Int. 2015;46(2):139-144.
4. Chu SJ, Tarnow DP, Tan JH, Stappert CF. Papilla proportions in the maxillary anterior dentition. Int J Periodontics Restorative Dent. 2009;29(4):385-393.
5. Froum S, Lagoudis M, Rojas GM, et al. New surgical protocol to create interimplant papilla: the preliminary results of a case series. Int J Periodontics Restorative Dent. 2016;36(2):161-168.
6. Jemt T. Restoring the gingival contour by means of provisional resin crowns after single-implant treatment. Int J Periodontics Restorative Dent. 1999;19(1):20-29.
7. Chang M, Odman PA, Wennström JL, Andersson B. Esthetic outcome of implant-supported single-tooth replacements assessed by the patient and by prosthodontists. Int J Prosthodont. 1999;12(4):335-341.
8. Meijer HJ, Stellingsma K, Meijndert L, Raghoebar GM. A new index for rating aesthetics of implant-supported single crowns and adjacent soft tissues-the Implant Crown Aesthetic Index. Clin Oral Implants Res. 2005;16(6):645-649.
9. Evans CD, Chen ST. Esthetic outcomes of immediate implant placements. Clin Oral Implants Res. 2008;19(1):73-80.
10. Fürhauser R, Florescu D, Benesch T, et al. Evaluation of soft tissue around single-tooth implant crowns: the pink esthetic score. Clin Oral Implants Res. 2005;16(6):639-644.
11. Belser UC, Grütter L, Vailati F, et al. Outcome evaluation of early placed maxillary anterior single-tooth implants using objective esthetic criteria: a cross-sectional, retrospective study in 45 patients with a 2- to 4-year follow-up using pink and white esthetic scores. J Periodontol. 2009;80(1):140-151.
12. Juodzbalys G, Wang HL. Esthetic index for anterior maxillary implant-supported restorations. J Periodontol. 2010;81(1):34-42.
13. Hosseini M, Gotfredsen K. A feasible, aesthetic quality evaluation of implant-supported single crowns: an analysis of validity and reliability. Clin Oral Implants Res. 2012;23(4):453-458.
14. Tettamanti S, Millen C, Gavric J, et al. Esthetic evaluation of implant crowns and peri-implant soft tissue in the anterior maxilla: comparison and reproducibility of three different indices. Clin Implant Dent Relat Res. 2016;18(3):517-526.
15. Fagan MC, Owens H, Smaha J, Kao RT. Simultaneous hard and soft tissue augmentation for implants in the esthetic zone: report of 37 consecutive cases. J Periodontol. 2008;79(9):1782-1788.
16. Deliberador TM, Vieira JS, Bonacin R, et al. Connective tissue graft combined with autogenous bone graft in the treatment of peri-implant soft and hard tissue defect. Quintessence Int. 2015;46(2):139-144.
17. Malament KA, Pietrobon N, Neeser S. The interdisciplinary relationship between prosthodontics and dental technology. Int J Prosthodont. 1996;9(4):341-354.
18. Schneider M, Eckelt U, Reitemeier B, et al. Stability of fixation of diacapitular fractures of the mandibular condylar process by ultrasound-aided resorbable pins (SonicWeld Rx® System) in pigs. Br J Oral Maxillofac Surg. 2011;49(4):297-301.
19. Iglhaut G, Schwarz F, Gründel M, et al. Shell technique using a rigid resorbable barrier system for localized alveolar ridge augmentation. Clin Oral Implants Res. 2014;25(2):e149-e154.
20. Dorosz N, Dominiak M. Mandibular ridge reconstruction: a review of contemporary methods. Adv Clin Exp Med. 2018;27(8):1159-1168.
21. Carron MA, Zuliani G, Pereira L, et al. Stability of midface fracture repair using absorbable plate and screw system pilot holes drilled and pin placement at angles other than 90°. JAMA Facial Plast Surg. 2014;16(1):42-48.
22. Elian N, Tabourian G, Jalbout ZN, et al. Accurate transfer of peri-implant soft tissue emergence profile from the provisional crown to the final prosthesis using an emergence profile cast. J Esthet Restor Dent. 2007;19(6):306-314.
23. Ishikawa T, Salama M, Funato A, et al. Three-dimensional bone and soft tissue requirements for optimizing esthetic results in compromised cases with multiple implants. Int J Periodontics Restorative Dent. 2010;30(5):503-511.
24. Chappuis V, Araújo MG, Buser D. Clinical relevance of dimensional bone and soft tissue alterations post-extraction in esthetic sites. Periodontol 2000. 2017;73(1):73-83.
25. Nam J, Aranyarachkul P. Achieving the optimal peri-implant soft tissue profile by the selective pressure method via provisional restorations in the esthetic zone. J Esthet Restor Dent. 2015;27(3):136-144.
26. Viana PC, Correia A, Kovacs Z. The papillary veneers concept: an option for solving compromised dental situations. J Am Dent Assoc. 2012;143(12):1313-1316.
27. Urban I, Caplanis N, Lozada JL. Simultaneous vertical guided bone regeneration and guided tissue regeneration in the posterior maxilla using recombinant human platelet-derived growth factor: a case report. J Oral Implantol. 2009;35(5):251-256.
28. Viana PC, Kovacs Z, Correia A. Purpose of esthetic risk assessment in prosthetic rehabilitations with gingiva-shade ceramics. Int J Esthet Dent. 2014;9(4):480-489.
29. Papaspyridakos P, Amin S, El-Rafie K, Weber HP. Technique to match gingival shade when using pink ceramics for anterior fixed implant prostheses. J Prosthodont. 2018;27(3):311-313.
30. Coachman C, Salama M, Garber D, et al. Prosthetic gingival reconstruction in a fixed partial restoration. Part 1: introduction to artificial gingiva as an alternative therapy. Int J Periodontics Restorative Dent. 2009;29(5):471-477.
31. Salama M, Coachman C, Garber D, et al. Prosthetic gingival reconstruction in the fixed partial restoration. Part 2: diagnosis and treatment planning. Int J Periodontics Restorative Dent. 2009;29(6):573-581.
32. Coachman C, Salama M, Garber D, et al. Prosthetic gingival reconstruction in fixed partial restorations. Part 3: laboratory procedures and maintenance. Int J Periodontics Restorative Dent. 2010;30(1):19-29.
33. Kim J, Topolski R, Dickinson D, Ramos V Jr. The influence of lip form on incisal display with lips in repose on the esthetic preferences of dentists and lay people. J Prosthet Dent. 2017;118(3):413-421.
34. Coachman C, Van Dooren E, Salama MA, Mahn E. Treating two adjacent missing teeth in the esthetic zone. Part 1: the pink hybrid restoration and the unilateral versus bilateral defect concept. J Cosmetic Dent. 2018;34(3):50-62.