Meeting Implant Challenges with a Patient-Specific Solution
The telescopic implant bridge is finalized in the conclusion of this case
By Arian Deutsch, CDT | This article is the second in a two-part series.
In Part 1 of this MasterClass, the need for patient-specific implant solutions was highlighted, and the initial steps in obtaining accurate clinical records were explained to the wax try-in stage. The technical steps were also explained. It is noteworthy that these steps—ie, initial impression with impression transfers, verified impression and cast, and screw-retained wax rim and try-in—should be the baseline standard for most implant rehabilitations today.
To read Part 1 of this MasterClass, visit insidedentaltech.com/idt1058.
Digital Workflow
The verified master cast has fiduciary markings cut into the buccal outer model surfaces with a handpiece. This was used to stitch and relate putty matrices to the model digitally.
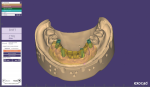
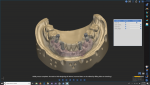
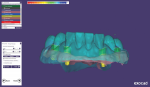
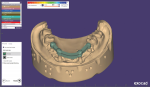
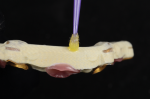
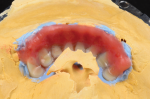
Using the master verified cast, the wax try-in and soft tissue material were removed. Scan flags were secured to the implant analogs and the case and patient information were entered into the exocad software (exocad, exocad.com), including materials selection, restoration type, etc. In this case, the author used the telescopic module for telescopic abutments in solid titanium. Using the ScanApp interface, the model was sprayed with scan spray and scanned. The scan flags were removed, and the model was scanned at this level as a base scan. The soft tissue was placed on the model and another scan was performed as a soft tissue scan. Next, the wax try-in was placed onto the master verified cast, the screws secured into the implant analogs, and scanned again as a pre-op or situation scan (Figure 1). Lastly, using the silicone putty matrix of the wax try-in, the individual teeth were removed from the wax try-in and placed into the putty matrix. The putty matrix was also sprayed with scan spray.
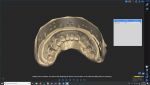
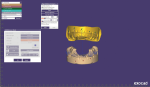
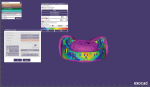
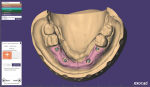
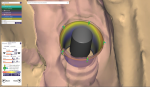
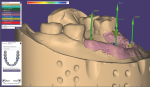
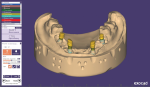
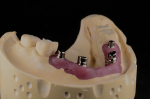
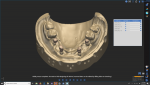
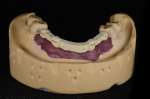
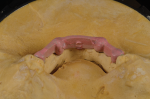
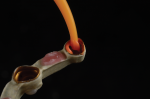
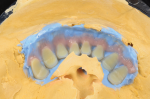
A new prescription was created, and the putty matrix was scanned as an antagonist scan and saved as an STL file (Figure 2). Opening the original prescription with all original model scans, Expert mode was entered and the Add/Remove Mesh option was selected. The antagonist scan was then selected and stitched or related to the model scan using the common fiduciary points from the putty matrix and the model (Figure 3 and Figure 4). At this point, the author had a completely digital 3-dimensional rendering of all levels of the model, implants, gingiva, and both inner and outer surfaces of the dentition (Figure 5). In essence, the author could peer into and between all of the volumes of restorative space to work with and start to design a truly patient-specific solution based on these very individual measurements.
Design
By either going through ScanApp or clicking the Design tab in exocad, the design phase began. For this case, the author designed four custom telescopic abutments in solid titanium.
In the initial stages of design, it was required to enter the appropriate scan flag and select the material/properties—in this case solid titanium. The scan flags were then related to the selection using Best Fit Matching.
For each custom abutment site, the soft tissue margin was outlined (Figure 6), and the insertion path/axis was selected as All Same so that the telescopic abutments remained perfectly parallel to each other. Next, the emergence profile of the custom telescopic abutments needed to be outlined. It was very helpful to use the Visualization selection so that the level of tissue compression could be seen while designing (Figure 7). Once completed, it was necessary to select the insertion path/axis of all of the telescopic abutments. There were a variety of determining factors when it came to insertion axis selection. Particularly, it was desirable to stay as close as possible to 90° to the occlusal plane to avoid any possible dislodging of the prosthesis from habitual tongue thrusting by the patient (although it is quite unlikely that patients can physically dislodge a telescopic restoration with their tongue). Other considerations included the anatomy of the tissues being covered. For example, if there was a large undercut in an area that must be added to gain soft tissue support, then the insertion axis may have had to be tweaked to satisfy both of the aforementioned concerns (Figure 8).
Once these design aspects were all addressed, the software generated preformed telescopic abutments that could be edited in an unlimited fashion, giving the designer complete control over the design details within each restorative space scenario at each implant site (Figure 9).
The last phase of the design process was to add or remove and smooth specific areas of the custom telescopic abutments (Figure 10). This feature proved very useful, particularly on the top of the abutments close to the edges and screw accesses (Figure 11). Once the abutments were finalized, they were saved as individual STL files and submitted to the milling center for manufacturing.
Post CAM Work
When the abutments were milled and sent to the laboratory, they still required handwork to achieve the highly polished surfaces necessary in successful telescopic solutions. To ensure that the abutments were perfectly parallel with highly polished surfaces, hand milling was required. Additionally, in order to protect the analogs in the master verified cast from the heat and pressure that occur during the milling process, a milling model transfer was made. The milling model transfer could have been performed by using either a transfer spider or the author's preference, a tool developed by Claus Kuchler (telemaster.de), the C.K. Telemaster Using the C.K. Telemaster along with the Implant Fix parts and some GC Pattern Resin, it was possible to very precisely transfer the custom abutments with an additional set of analogs to the C.K. Telemaster without the use of gypsum. This also allowed hand milling with a minimal rotation of the abutment in order to mill all surfaces very precisely (Figure 12).
Once transferred, the custom abutments were milled with a series of three milling burs (Figure 13), followed by felt polishers and diamond paste. The tops and emergence areas of the custom telescopic abutments were hand polished and steam cleaned, then cleaned with 99% isopropyl alcohol.
The master model with soft tissue in place was sprayed with a silicone separator on the soft tissue. The abutments were placed (Figure 14) and screwed into the implant analogs and the screw access holes are blocked with wax. A silicone duplicate was made using this model, and the silicone duplicate was poured in a type-IV resin-reinforced die stone, a "processing duplicate" poured using GC Pattern Resin (GC America, gcamerica.com) in the telescope sites, and a screw placed into the resin for retention followed by pouring in a type-IV resin-reinforced die stone. The processing model was cross mounted to the opposing on the articulator for any post-processing occlusal adjustments needed after final polymerization. The abutments were removed and then prepared for the electroforming process by cleaning with Clean Fix (Gramm Technik, gramm-technik.de).
Electroforming
The electroforming process yields a uniform gold coping which fits the primary abutment between 4 to 5 microns. This intimate fit to the primary abutment across multiple abutments generates the excellent retentive quality that is the hallmark of telescopic restorations. In order to achieve this fit, it was best to electroform the gold directly to the primary abutment and not on a duplicate die.
Once the abutments were cleaned with Clean Fix (Gramm Technik), they were connected to the rods in the optiCLIC contacting system (Heimerle + Meule GmbH, heimerle-meule.com) using GC Pattern Resin on the optiCLIC holder. The access holes were blocked with a light-curing resin. The abutments were then airbrushed with a conductive silver lacquer (Gramm Technik). A lead was painted on with a small brush from the exposed metal to the surface of the telescopic abutment using the conductive silver lacquer (Figure 15).
After drying the abutments, the areas that still had silver conductive lacquer where it was not desired were blocked out with a light-curing resin. The electrical contacts were verified with the voltmeter. The abutments on the optiCLIC rods were then placed onto the plating head in their respective positions and retained by the magnetic retention of the optiCLIC plating head.
The desired gold content was calculated using the telescopic abutment guide and entered into the electroformer interface (Gramm Optimo 2, Gramm Tecknik). The required gold solution SG200 (Gramm Tecknik) and activator were calculated by the electroformer and the appropriate container and magnetic stirrer were shown on the screen. The SG200 and activator were added to the beaker, and the plating head was attached and placed into the electroformer, at which point the electroforming process began.
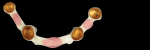
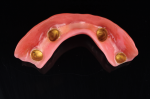
After electroforming, the gold copings were divested and placed into a beaker with a 40% nitric acid solution in an ultrasonic for approximately 15 to 20 minutes. They were carefully removed using protective gloves and eyewear, and the acid was neutralized with neutralizer. The copings were adjusted at the margins as necessary and air abraded on the outside with aluminum oxide at 2 bar pressure. The corresponding tooth numbers were etched into the buccal surface of the gold. The soft tissue was removed from the master cast. All abutments were placed on the master verified cast after cleaning out any remaining pattern resin from the access holes (Figure 16). The gold copings were placed onto the abutments and prepared for the next digital process used to create the tertiary structure.
Tertiary Structure Design
Tertiary structures for telescopic restorations continue to advance in terms of designs and materials; in some cases they can be as simple as a strengthening bar designed to be wrapped in acrylic. They can also be designed with thimble or other varieties of cutback designs for layering composite or for cementing pressed ceramics, milled ceramics, or even milled hybrid ceramic materials.
The model with abutments in place and galvano gold seated was sprayed with scan spray and a new prescription was opened in exocad. Then, the model with abutments and gold in place were scanned (Figure 17). The restoration type over each abutment site was selected as Offset Coping, and those were connected in the software with the Bar selection.
Each offset coping was outlined, and it was preferred to set the margin of the offset coping just slightly above the margin of the galvano gold coping. Once designed, the offset copings could be connected with the bar segments and the volumes and shapes of the bar could be manipulated. It was also best to load the antagonist and tissue scans from the preliminary scans when designing the primary telescopic abutments. These same scans could then be used to design the offset copings and bar segments to fit below the basal surfaces of all denture teeth and provide easy seating during the preparation for final processing. There was also a 1-mm spacer incorporated on the basal side of the bar between the bar and the tissue to allow for opaquing and acrylic.
It was even possible in advanced editing to control and manipulate the bar in a variety of ways, adding undercut angulations to its geometry in order to enhance acrylic retention to the tertiary structure. Once the tertiary structure was complete (Figure 18), it could be submitted for either milling in TriLor® material (Harvest Dental, harvestdental.com) or by selective laser melting (SLM). When the structure was fabricated, it was checked over the abutments and gold for passivity, and a minimum of three tissue stops were made using a light-curing pink composite at the planned height away from the tissue.
Cement vents were also sliced into the buccal surfaces of the tertiary structure to allow excess cement to vent out at the cementation step (Figure 19).
Passive Pick-Up
Probably the most important clinical step in this telescopic restoration was the passive pickup of the gold copings into the tertiary structure. This passive pickup step allowed the most accurate fit possible and eliminated any movement or micro-movement in the connection from the prosthesis to the implant.
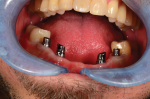
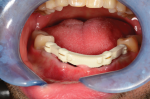
During this clinical appointment, the primary abutments were seated, x-ray verified, and torqued. The galvano gold copings were seated on the primary abutments with the respective tooth numbers facing to the buccal. The tertiary Trilor structure was seated over the abutment sites and checked for passivity (Figure 20 and Figure 21). If the tertiary structure was completely passive throughout seating until the tissue stops were seated on the tissue, then the next step, cementation, could be completed. If the tertiary structure did not seat completely and was binding on the galvano gold copings, then the tertiary structure would have needed to be adjusted until complete seating was realized.
It was critical that a dry field was maintained, particularly that the galvano gold copings were kept dry. The copings and inside of the offset copings of the tertiary structure were primed with a metal primer prior to cementation in the case of SLM structures. In the case of a Trilor structure, it was advisable to use Shofu Ceraresin Bond (CRB) (Shofu, shofu.com).
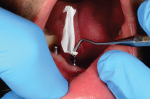
A small amount of adhesive resin cement was placed into the offset copings in the tertiary structure. The tertiary structure was carefully seated over the gold copings until the tissue stops were touching the tissue. The adhesive resin cement vented through the venting slots, and the cement was "tack" cured with a light-curing unit at the sites of venting (Figure 22). The structure was allowed to set completely for 8 minutes prior to removal. The tertiary structure was removed and, importantly, not tried back onto the model, but sent to the laboratory immediately (Figure 23).
The solid acrylic temporary was placed and adjusted as necessary over the telescopic abutments (Figure 24), and once seated, the abutment screw access holes were sealed. Teflon tape to protect the screw heads and flowable composite were recommended (Figure 25).
Final Processing
The entire Trilor tertiary structure was then primed with Shofu Cereresin Bond (Figure 26). A light-cured opaque was brushed on and light cured. The structure was placed onto the "processing" model fabricated earlier, and the matrix with tooth positions was used to reattach the denture teeth to the tertiary frame. The case was waxed up and invested on the processing model in a flask.
Once the flask had been opened and wax removed (Figure 27), the tertiary structure was removed, cleaned with steam, and dried. The teeth were cleaned and prepared for processing in the flask. A small amount of light body VPES Impression Material (GC America) was injected into the inside of all of the galvano gold copings (Figure 28) and immediately seated on the processing model, ensuring complete seating to the tissue stops. Any excess VPES was removed with a microbrush. The gingival characterization was added using acrylic polymers (Naturecryl, GC America) that had been sifted to remove fibers. In this case, only two shades were used, but they were blended in a such a way as to mimic a transitional third shade (Figure 29 and Figure 30).
Final processing could be carried out with either the traditional press packing method or, as in this case, with an injected acrylic system.
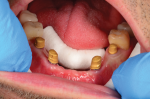
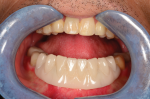
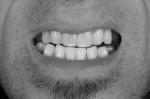
The benefits of using the processing model in concert with the VPES were apparent when divesting in that the inner surfaces of the gold copings were perfectly protected and the case divested very cleanly and easily. After divesting, the case was trimmed as needed and polished with a variety of carbide tools and polishers (Figure 31 and Figure 32). Final polishing was performed with pumice substitute and a single-row brush and buff wheel, followed by a high-speed buff wheel and Acryl Marvel (Dental Ventures, dentalventures.com). The case could then be delivered for seating and final delivery (Figure 33 and Figure 34).
Conclusion
Patient-specific implant solutions are continuing to evolve and redefine what can be expected in terms of implant prosthetics. As newer materials, techniques, and digital workflows flourish, we find that combining these with long-standing, well-proven traditional solutions becomes even more advantageous to dentistry and ultimately to dental patients with implants.
About the Author
Arian Deutsch, CDT
Owner
Deutsch Dental Arts
Surprise, AZ