A Simplified Approach to Digital Dentures
Digital Dentures with the DGSHAPE DWX-51D and DWP-80S from Roland
Justin Marks, CDT
Digital denture design software has been commercially available now for a number of years. As with digital removable partial dentures (RPDs) previously, the challenge with digital denture fabrication has long been due to manufacturing limitations. Any digitally designed restoration may look great on a computer screen but has little benefit until it can be transformed into a physical object for delivery to patients.
In the coming years we will no doubt witness the introduction of viable materials and methods for entirely 3D-printed dentures. For the time being, however, currently available 3D-printed photopolymers do not rival the physical properties of a quality heat- and pressure-cured polymethyl methacrylate (PMMA) denture base.
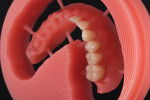
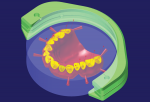
With this in mind, the author set out a number of years ago to develop a digital denture workflow that repurposes existing milling equipment and combines it with commercially available materials and design software (Figure 1). This process can be utilized in laboratories that have already integrated CAD/CAM or by those that plan to acquire the necessary equipment and gain full control over the digital denture workflow.
Two of the biggest challenges in digital denture fabrication are:
1. Addressing the fabrication of ancillary denture products including custom impression trays, base plates, and trial evaluation dentures.
2. Reducing the ridge lap portion of a pre-manufactured denture tooth for placement into a milled (or 3D-printed) denture base.
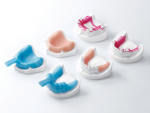
Fabricating custom trays, bite blocks, and try-ins is well-suited to additive manufacturing since the appliances are single-use only, and photopolymers work well for them. The DWP-80S 3D printer (Figure 2) from DGSHAPE by Roland is used to print these items (Figure 3). Custom trays are designed in less than 5 minutes and allow the laboratory to set specific parameters such as impression material spacing, tray thickness, and tissue stops.
Of particular interest is the use of DGSHAPE's base plate resin. The author's denture laboratory made it a goal to stop using wax and plaster by the end of 2018, and digitizing the denture setup is a critical part of realizing this vision. This same resin can be used to print stabilized base plates for occlusal rim fabrication or to print a monolithic denture design for trial evaluation.
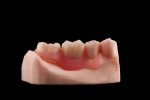
At present, the author prefers to use pre-manufactured denture teeth in full dentures, since they offer acceptable esthetics and eliminate the need for additional milling (as in the case of fully milled denture teeth). It should be noted that for partial dentures the author prefers to mill custom denture teeth with the DWX-51D for complete customization, improved function, and reduced inventory (Figure 4).
Full-denture design software is available from most developers including 3Shape (3shape.com), Dental Wings (dentalwings.com), and exocad (exocad.com). The author currently uses 3Shape and has compiled a number of denture tooth libraries that were either provided by the manufacturer or created internally by scanning denture teeth and virtually positioning them into occlusion. The process begins with scanning models of the maxillary and mandibular arches along with the maxillo-mandibular relationship positioned through the use of a wax occlusal rim. The occlusal and sagittal planes are identified virtually on the wax rim along with anatomical landmarks that will be used for a proposed denture-tooth setup using the library selected by the designer.
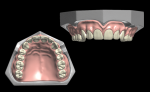
The proposed tooth arrangement is manipulated by the designer to customize the setup. The library used in this scenario is programmed so that the shape and size of the denture teeth cannot be altered, thus ensuring that they will match the physical dimensions of the pre-manufactured teeth. Alternate settings available in 3Shape allow for complete customization of the denture teeth and for the tooth design to be exported for milling or 3D printing. Once the tooth arrangement has been finalized, the borders of the denture are drawn virtually on the cast. Wax is added to a precise thickness and then morphed and sculpted to fill interproximal papillae and provide initial characterization to the denture (Figure 5).
The finalized design is output to three separate 3D models for manufacturing: a monolithic design for trial evaluation, a tooth reduction jig, and the final denture base with tooth sockets for milling (Figure 6). The monolithic version is sent to the clinician for trial evaluation. If a new bite registration is needed it can be obtained at the trial appointment and re-scanned upon return to the laboratory. Once verified, a putty matrix is recorded over the occlusal and buccofacial surfaces of the 3D-printed monolithic design. This matrix is dual purpose and will be used both as a placement guide to reduce the basal surfaces of denture teeth and to position the teeth into the milled final denture base.
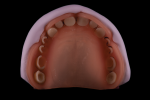
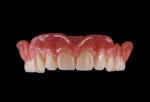
Multiple CAM platforms exist that can be used to mill dentures with the DGSHAPE DWX-51D. The author has successfully used both hyperDENT (FOLLOW-ME! Technology; follow-me-tech.com) and SUM3D (CIMsystem; cimsystem.com) for this workflow (Figure 7). The final denture base is milled in pink PMMA on the DWX-51D (Figure 8), and the teeth are prepared using the 3D-printed reduction jig and the putty matrix taken from the monolithic denture (Figure 9). The teeth and matrix are then transferred to the milled denture base and polymerized into position using standard pour acrylic in a pressure vessel. The denture can be finalized either through conventional polishing techniques or by applying light-cured extrinsic stains and glazes to the external surfaces of the denture for a more characterized appearance (Figure 10).
The digital denture workflow is best utilized by the laboratory as a means to streamline production and reduce the opportunities for error that can frequently occur when processing denture acrylics. Clinicians can continue to use the methods and materials they are comfortable with while laboratories can adopt digital technology to address the increased demand for dentures driven by a growing edentulous population.
Disclaimer: The statements and opinions contained in the preceding material are not of the editors, publisher, or the Editorial Board of Inside Dental Technology.
About the Author
Justin Marks, CDT, is the owner of Master-Touch Dental Lab in Brooklyn, New York.
Manufacturer Contact Information
Roland DGA
rolanddga.com
800-542-2307