Redefining the Dental Laboratory Workflow with 3D Printing
Explore the technologies and capabilities of additive manufacturing
Chuck Stapleton, MBA, BS
Additive manufacturing-also known as 3D printing-has been a viable production technology in dentistry for more than a decade. Through additive manufacturing, patient-specific devices from highly detailed end-use dental prosthetic models and drill guides to frameworks for partial dentures, crowns, and bridges can be produced much more efficiently and at a lower cost. The desire to incorporate the technology into a laboratory's workflow is only the first step in the process. Understanding the various printers and materials is important to select the appropriate solution.
Technologies to Address a Variety of Applications
Plastic (resin) printing is divided into four core technologies: MultiJet Printing (MJP), Fused Deposition Molding (FDM), Stereolithography, and Selective Laser Sintering (SLS). Stereolithography can be further divided based on the light source into Selective Laser Apparatus (SLA), Masked Stereolithography (MSLA), and Digital Light Projector (DLP). 3D printing can also be used to create metal prostheses through Direct Metal Printing (DMP, also known as DMLP) or printing a resin pattern for casting. SLM is another name for SLS/DMP. This overview includes figures showing how each technology would print Figure 1.
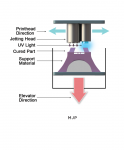
MJP
MultiJet Printing utilizes an inkjet head similar to that of a desktop paper printer. Material is jetted through the printhead in a thin layer. A UV light passes over the material and adheres it to the previous layer. One significant advantage of MJP is that the support material is typically wax- or water-soluble, and can be removed without support scarring. In addition, MJP is particularly effective for laboratories that do not run three shifts a day and thus need to produce large batches overnight (Figure 2). A similar technology is polyjet, utilized by Stratasys (stratasys.com).
Indications:
Full prosthodontic models
Quadrant prosthodontic models
Patterns for casting
Implant surgical guides
Strengths:
Highest accuracy
Separate support material
Overnight throughput
Weaknesses:
Cost of equipment
Speed for small batches
Maintenance difficulty
Material cost
FDM
Fused Deposition Molding uses an extruded plastic wire to create an object. This is the lowest-cost method to 3D print, but accuracy is sacrificed. The only FDM dental applications of interest have come from Arfona (arfona.com) for producing flexible partials; Arfona also recommends FDM for removable models (Figure 3).
Indications:
Flexible partials
Removable models
Strengths:
Low equipment cost
Low material cost
Weaknesses:
Accuracy of parts
Post-processing can be difficult
Material options
Stereolithography
Stereolithography is the oldest of the 3D printing technologies. However, unlike most technology, it has aged very well. In fact, many of the best printers on the market today utilize stereolithography in one fashion or another. Stereolithography uses a vat of light-curable resin sitting below or on top of a light source. The light source-which can be a laser as used in SLA, a projected light source as used in DLP, or a masked light source as used in MSLA-creates a pattern across the resin. The material is then settled and cured again by the light source, building up layer by layer.
Print speed with traditional SLA systems is on par with or faster than that of MJP, but slightly less accurate. Part of this is due to differential shrinking of parts when printing something like a full arch. After a system cures through a transparent plate, it peels the layer off the plate and waits for material to flow underneath it before curing the next layer. For a system with the light source on top, the material must be leveled before the next layer can be cured. This requires the system to slow down to avoid distorting the part.
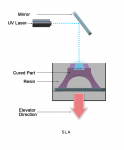
SLA
SLA utilizes a laser to draw the area of the material that needs to be cured. FormLabs' Form 2 (formlabs.com), perhaps the most disruptive product to date for dental, utilizes SLA technology and a laser that cures from below the platform. This product has been revolutionary for the value, offering an easy entry point into the 3D printing market.
There are also higher-capacity SLA machines like those provided by 3D Systems (3dsystems.com) that can print almost 200 full-arch models in a single run, but their size is quite large, and they are most often utilized for significant production applications. The vast majority of large orthodontic players use this equipment for their clear aligner production process (Figure 4).
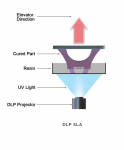
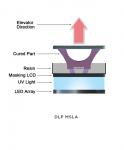
DLP
DLP uses a projected light source similar to what you would find in an office projection system, available in 1080 or 4k projections. The distance of the projector from the platform determines the size of the build area. Instead of drawing the cured area with a laser, the entire image is projected simultaneously onto the layer of material. EnvisionTEC (envisiontec.com) is well known for its line of DLP printers and is joined by solutions from 3D Systems, Asiga (Whip Mix, whipmix.com), Carbon (carbon3d.com), DGSHAPE by Roland (rolanddga.com), Kulzer (kulzer-us.com), and VOCO (vocoamerica.com), among others (Figure 5).
MSLA
MSLA is a variation on DLP in which a light source is constantly on, like an array of LEDs. That source is then masked by another layer, allowing light to pass through in certain areas. Structo (structo3d.com) currently offers a solution that utilizes MSLA technology. Both DLP and MSLA offer faster print speeds than SLA when comparing the same build area due to the ability to cure an entire layer at one time instead of drawing it with a laser. However, this is not a set rule, and there are exceptions depending on the application (Figure 6).
Indications:
Quadrant prosthodontic models
Orthodontic models
Surgical guides
Bite splints
Castable materials
Dentures
Composite crowns
Custom trays
Indirect bonding trays
Try-ins
Strengths:
Machine for every budget
Lower material cost than MJP technology
Wide range of materials
Weaknesses:
Not ideal for very high precision parts
Speed for certain SLA applications
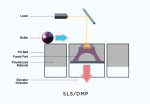
SLS and DMP
SLS (Selective Laser Sintering, also known as Selective Laser Melting) and DMP (Direct Metal Printing, also known as Direct Metal Laser Sintering) utilize two very similar technologies whose primary application is for end-use parts-particularly SLS with biocompatible nylon materials. Raw material in powder form is picked up by a roller and placed in a very thin layer. That layer is then hit with a laser, which causes it to melt and bond to the previous layer of material. The roller then places another thin layer on top of the previous one and the process continues.
DMP is the only option for direct metal printing, and some companies offer substructures manufactured with DMP technology. In addition, partial frameworks from companies like 3DRPD (3drpd.com) are also manufactured using DMP technology. This category of equipment bears a significant cost due to the laser technology utilized and the systems required to work with fine powders (Figure 7).
Indications:
Sleep apnea appliances (SLS)
Bite splints (SLS)
Metal substructures (DMP)
Partial frameworks/RPD (DMP)
Strengths:
End-use parts
Metal printing (DMP)
Nylon materials (SLS)
Weaknesses:
Cost of equipment
Speed of printing
Future developments
Future Considerations
The most significant developments occurring in 3D printing are in the areas of new materials, faster printing technologies, and equipment uptime/support.
No-Adhesion/Low-Adhesion Stereolithography
A recent breakthrough uses membranes that do not stick to the material, either with a liquid interface or an oxygen interface. With membranes, the light-cured material is literally floating on air or another liquid. When that layer is cured, it no longer needs to peel off the previous layer, but can be raised immediately, and the next layer can be cured. This leads to a significant decrease of print times. Prior to this, printing a platform of dental models in 30 minutes was unheard of. 3D Systems' Figure 4™ Technology, Carbon's Digital Light Synthesis™, and EnvisionTEC's Vida cDLM system all use this type of technology.
Materials
3D printing hardware is reaching a plateau in terms of innovation. Printers can produce clinically acceptable parts, and most recent improvements have related to speed. The next area for true innovation is materials-particularly those suitable for placement directly in the patient's mouth.
3D Systems recently released a new NextDent material that has regulatory clearance as a permanent crown. This, combined with their denture materials, enables printing of complete dentures. DENTCA also has a 3D-printed denture material that has FDA clearance and can be used on SLA systems. Other examples include companies launching bite splint materials, and Arfona has a 3D-printable flexible partial material.
Improved material strength and esthetics are two areas that should demonstrate significant improvement over the coming years. Companies like DWS (dwssystems.com) are already working on systems to produce end-use restorations in more than one shade.
Regulatory
Related to material development is the regulatory impact on 3D printing. The FDA is taking a stronger stance on newer CAD/CAM technologies. This means stricter controls and validation on what the combined systems (printer and material) are producing, which leads to better safety and long-term viability of the medical device. This also means that those capable of material development for 3D printing will need significant investments into building their validation processes.
Reliability and Support
As technologies converge and become commoditized, the two things that distinguish them are price and support. Price will be set by the market, but support level is something that is unique to each company. This is not just answering the phone but understanding what the laboratory is working on. Do they have a dedicated dental applications team for support? Equipment reliability is another distinguishing factor. How much uptime can be expected? Does it operate under the laboratory's conditions? What if a problem occurs? How long does it take to fix?
There are many ways to address these issues. Good engineering from the beginning is one, but the future is promising for remote fixes via software and cross-shipping equipment if something goes wrong. It will no longer be necessary to have an engineer come out and fix an issue. They will be able to diagnose a machine remotely through reported analytics, tell the user what is wrong, and provide a fix all within the same day. Through machine learning, companies can even predict when a machine will fail and address it proactively. A replacement printer could arrive at the laboratory because an algorithm predicted the current machine is due to have a failure.
Conclusion
3D printing is now more accessible than milling due to the cost of the equipment and ease-of-use. Due to this, dental laboratories and clinics should see a stronger adoption of the technology in the future.
About the Author
Chuck Stapleton, MBA, BS, is an Advanced Applications Engineer with 3D Systems, based in San Diego, California.