The Myths and Realities of Today's Zirconia Restorative Materials
More versatile than you think
By Nelson Rego, CDT, AAACD
Since their introduction, milled zirconia restorations have been increasingly requested by dentists as an alternative to porcelain-fused-to-metal (PFM) restorations based on their strength and more natural-looking esthetics than metal-based options.1 Unfortunately, the dense and opaque nature of the material has historically meant that restorations lacked many of the optical properties that would enable their use when esthetics was an equally important consideration; application of a veneering ceramic to enhance esthetics was required.
In recent years, however, manufacturers have begun to introduce zirconia options that can be milled to full-contour, demonstrate esthetics suitable for placement anywhere in the mouth, and exhibit requisite strength to withstand fracture. Despite the usability of zirconia for a variety of indications, confusion remains among dentists and laboratory technicians about what is possible with different types of zirconia dental materials.
This article reviews some of the myths and realities surrounding zirconia dental materials to help dentists and laboratory technicians understand the differences among the options available today. It will also help to clarify the relevance of the strength and mechanical property measurements used to describe and promote the benefits of the mechanical characteristics of zirconia restorative materials.
Myth: All zirconia materials are the same.
Reality: Based on a variety of factors that differentiate zirconia materials, not all zirconia materials are the same. These factors include composition, fracture resistance properties, optical properties, processing requirements, and others.
First, not all zirconia materials are manufactured in the same manner or contain the same formulation of components. Some dental zirconias contain greater or lesser amounts of stabilizers (eg, yttria), which influences the material's mechanical properties such as strength and fracture toughness as well as optical properties such as translucency.2,3 Essentially, the more yttria that is added to zirconia, the more translucent—but also the weaker and less fracture-resistant—it becomes.
Translucent monolithic dental zirconias behave differently, and their composition and microstructure influence their properties and clinical performance.4 Research has demonstrated that although a higher yttria content contributes to the most translucent and age-resistant Y-TZP ceramics, the materials' relative fracture toughness and strength are lowered considerably.5
Zirconias such as IPS e.max ZirCAD LT and MO, which are 3Y-TZP (ie, 3 molar percentage yttria-stabilized tetragonal zirconia polycrystal) materials, are high strength and demonstrate excellent mechanical properties and a low risk of temperature degradation.6 However they exhibit a lower level of translucency. This makes IPS e.max ZirCAD LT or MO the best zirconia choice for when strength and not esthetics is of the utmost importance. On the other hand, IPS e.max ZirCAD MT and MT Multi are 4Y-TZP zirconias that offer improved translucency for highly esthetic full-contour (ie, monolithic) restorations. MT and MT Multi offer the ideal level of strength, fracture toughness, and translucency, especially when compared to many of the HT zirconias on the market. These HT zirconias typically offer a lower fracture toughness that is comparable to lithium disilicate; although they do not offer the same esthetics as lithium disilicate. While MT and MT Multi offer high strength and esthetics in a zirconia material, their lowered fracture toughness in comparison to the 3Y-TZP zirconias (IPS e.max ZirCAD LT and MO) still limit their use in certain indications, wall thicknesses, and connector dimensions. A zirconia material's fracture toughness and strength can be attributed in part to the structural characteristics of its stabilization and polycrystalline composition.3 For example, the IPS e.max ZirCAD MT Multi zirconia demonstrates a fracture toughness of 3.6 MPa √m, which is higher than many other esthetic zirconia materials. This is ideal for three-unit cases with higher wall thicknesses, for which researchers have recommended the use of materials with a fracture toughness of no less than 3.
Myth: Flexural strength is the best predictor of clinical success with zirconia.
Reality: The flexural strength measurement, which is currently used to promote the strength of zirconia or any ceramic, is the absolutely incorrect measurement on which to assume fracture resistance and predict restoration longevity in the mouth. The amount of flexural strength (eg, 500 MPa, 750 MPa, 850 MPa) is not ideal when materials are compared for mechanical purposes. Fracture toughness, not flexural strength, is the ability of a material containing a crack to resist fracture, and is one of the most important properties of any material, especially zirconia.
To understand the difference in the two, consider the windshield of your car. When it is fracture tested, it is done so to determine how much of a tendency there is for a small crack to easily develop into a larger crack when it is hit by a rock. The ability of the windshield to resist fracturing is a product of toughness, not flexural strength. Flexural strength, the point when a material yields to bending, can be easily manipulated and does not always accurately represent the strength of a material. Also, it has been demonstrated that when 3Y-TZP zirconia has been sandblasted the measured strength increases but fracture toughness does not change.
Therefore, fracture toughness and/or fracture resistance is the more important measurement for predicting whether or not a zirconia restoration will resist fracturing or breaking in the mouth. Many of the high translucency zirconia materials have a fracture toughness of approximately 2.1, which is less than the fracture toughness of some other all-ceramic materials, such as lithium disilicate (eg, IPS e.max, 2.5 to 3). The applicability of fracture toughness measurements to the survival of dental restorations has been confirmed by scientists as the true predictor of long-lasting function of a restoration and its ability to resist a fracture.
Myth: All zirconia materials are unesthetic and, therefore, cannot be used for fabricating anterior restorations.
Reality: Traditionally, zirconia materials produced white, chalky, opaque, and unesthetic restorations that typically required laborious veneering, characterization, staining, and glazing procedures to impart lifelike esthetics. To combat these esthetic challenges, many manufacturers created HT or cubic zirconias (5Y-TZP) which increased the translucency, but can also “gray” when not in ideal lighting conditions. Today, however, zirconia materials are available that can be milled to full contour and demonstrate esthetics and translucency suitable for use in the anterior (eg, IPS e.max ZirCAD MT Multi).
IPS e.max ZirCAD MT Multi is designed with a special powder formulation and shading technology, so restorations demonstrate a natural progression of chroma and translucency from dentin to enamel, enabling efficient restoration production without requiring further characterization or staining.
Myth: If you want esthetic zirconia restorations, you have to sacrifice strength.
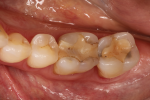
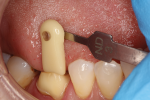
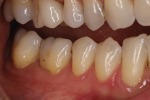
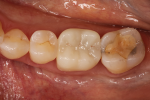
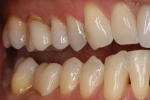
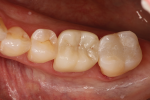
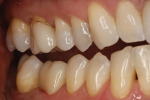
Reality: The more glass contained in a restorative material, the more attractive and esthetic it will be, but also the weaker it will be. Traditionally, as dentistry moved away from glass ceramics and selected zirconia, strong restorations were achieved that did not meet all of the necessary esthetic requirements. Until now we have been unable to control the light dynamics of zirconia and achieve the type of translucency and optical properties exhibited by more traditional glass ceramics (Figure 1 through Figure 5).
The unique IPS e.max ZirCAD MT and MT Multi formulations provide the perfect combination of zirconia strength, color, and translucency, making it the ideal zirconia choice for cases in which high mechanical stability, thin restoration walls, and natural esthetics are essential. The optimized raw material mixture increases the stress-bearing capacity, and as a result, there is no tradeoff between translucency and strength (Figure 6 and Figure 7). IPS e.max ZirCAD MT and MT Multi provide up to 50% higher fracture toughness than other common higher translucency zirconia materials.
Myth: Fabricating zirconia restorations that are both strong and esthetic requires laboratory ceramists to undertake labor-intensive procedures.
Reality: With IPS e.max ZirCAD, laboratory ceramists maintain individual freedom due to versatile processing options and can therefore fabricate zirconia restorations according to case requirements. In fact, once the IPS e.max ZirCAD discs are dry milled, the restorations can be sintered in the Ivoclar Vivadent Programat® S1 1600 furnace, which is capable of speed sintering zirconia restorations. After sintering, IPS e.max ZirCAD restorations can be glazed and/or characterized using IPS e.max CAD Crystall materials or new all-ceramic characterization systems such as IPS Ivocolor.
The sintering cycle after milling is significant to the combination of strength and esthetics. In particular, it contributes to such benefits as stronger, more esthetic restorations that will resist breaking in the mouth; doctor and patient confidence and satisfaction with treatment outcomes; and time and productivity savings overall from not having to remake restorations.
Myth: Esthetic zirconia restorations require dentists to follow a more complicated preparation and cementation protocol.
Reality: First, zirconia restorations are conventionally cementable using a self-adhesive resin cement, such as SpeedCEM® Plus. As a result, dentists typically don't need to anesthetize patients prior to seating the restoration, and there is less chance of postoperative sensitivity. Secondly, the preparation guidelines for esthetic zirconia restorations are the same as the preparation guidelines for adhesively cemented lithium disilicate restorations (eg, IPS e.max).
However, a benefit of IPS e.max ZirCAD restorations is their ability to remain strong and durable in monolithic form in cases for which there is considerably lower wall thickness. These include cases for posterior crowns with a minimum thickness of 0.6 mm or anterior crowns with a minimum of 0.4 mm for IPS e.max ZirCAD LT.
To view the references for this article, go to insidedentaltech.com/idt999
About the Author
Nelson Rego, CDT, AAACD, is co-owner of Smile Designs by Rego in Santa Fe Springs, California.
Manufacturer Contact Information
Ivoclar Vivadent
ivoclarvivadent.us
800-533-6825
Disclaimer: The statements and opinions contained in the preceding material are not of the editors, publisher, or the Editorial Board of Inside Dental Technology.
References
1. Schriwer C, Skjold A, Gjerdet NR, Øilo M. Monolithic zirconia dental crowns. Internal fit, margin quality, fracture mode and load at fracture. Dent Mater. 2017 Sep;33(9):1012-20.
2. Miyazaki T, Nakamura T, Matsumura H, Ban S, Kobayashi T. Current status of zirconia restoration. J Prosthodont Res. 2013 Oct;57(4):236-61.
3. Ramos CM, Cesar PF, Bonafante EA, et al. Fractographic principles applied to Y-TZP mechanical behavior analysis. J Mech Behav Biomed Mater. 2016 Apr;57:215-23.
4. Munoz EM, Longhini D, Antonio SG, Adabo GL. The effects of mechanical and hydrothermal aging on microstructure and biaxial flexural strength of an anterior and a posterior monolithic zirconia. J Dent. 2017 Aug;63:94-102.
5. Zhang F, Inokoshi M, Batuk M, et al. Strength, toughness and aging stability of highly-translucent Y-TZP ceramics for dental restorations. Dent Mater. 2016 Dec; 32(12):e327-e337.
6. Pinto PA, Colas G, Filleter T, DeSouza GM. Surface and mechanical characterization of dental yttria-stabilized tetragonal zirconia polycrystals (3Y-TZP) after different aging processes. Microsc Microanal. 2016 Dec;22(6):1179-88.