A Different Approach to a Hybrid Acrylic Base with Metal Ceramics
Restoring life after mandibular reconstruction
By Jayme Hong; Eric Park, CDT, LVI; and Seong J. Kim, CDT
CAD/CAM milled hybrid restorations are no longer unusual in the dental industry. Many laboratories are capable of designing and milling the components in-house. From the design and production of a printed titanium jaw to milled bars, CAD/CAM technology has allowed laboratories to produce dental prostheses and appliances at a level that was unthinkable to some only five years ago.
Certain complex cases, however, still demand creative treatment planning. The authors’ laboratory encountered such a case recently, and the team soon realized it would need to develop an entirely different case plan than it normally would — one that would not allow a reliance solely on state-of-the-art technology. This case required careful consideration of all options, and ultimately the team elected to employ traditional techniques along with a twist utilizing today’s technology.
Case Presentation
The patient had suffered from oral cancer, and the removal of the tumor had involved the mandibular arch. The surgeon had rebuilt the mandibular arch using bone from the patient’s fibula, which is the smaller of the two bones in the lower leg. An artery, soft tissue, and veins also were removed with the bone. This process is called micro-vascularized fibula-free flap mandibular reconstruction. It involves three surgical teams: head and neck, plastic surgery, and dental. The combination of procedures, surgeries, and healing processes is challenging and delicate.
The patient had a history of malignant neoplasm of the tongue. Radiation therapy was performed with 60 Gy/30 fractions. The patient also underwent hyperbaric oxygen therapy (HBOT) with 40 HBOT dives. After the patient’s mandibular arch was reconstructed with the fibula-free flap, implant placement was performed on teeth Nos. 22, 25, 27, 28, and 30, with guided surgery being utilized to provide optimal support for the implant-supported fixed prosthesis.
When treatment planning for the fabrication of the prosthesis itself, precision and an immediately comfortable fit were key because the patient had already suffered through agonizing pain and spent many hours in treatment. The authors led the case, and office team members Heather Jung and Haesung Yang communicated with the dentist. A devotion to their craft would be crucial in dramatically changing the life of this patient.
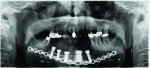
In order to restore the appearance and function that were negatively affected by the cancer and subsequent treatment, the initial case plan was to perform in-house fabrication of a CAD/CAM milled titanium hybrid prosthesis with ceramic teeth. However, the patient’s bone loss measured 19.2 mm (Figure 1). The severe depth and length were such that CAD/CAM processes could not produce a framework with suitable height for the abutments. In light of this, the technicians decided to utilize a handcrafted metal substructure.
Case Design
The most challenging factor was the location of the implant placement. At 19.2 mm, it was three to four times deeper than the typical range, requiring a more architectural approach. Adding appropriate support for the missing area was crucial. Using more metal was not viable as it would result in excessive weight. It was determined that fabricating the prosthesis solely with porcelain would result in poor esthetics, with a thick appearance that would be prone to fracture. Secondarily, an acrylic base and denture teeth would be less hygienic than porcelain. Thus, it was decided that an alternative material and frame design were necessary.
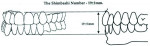
The Shimbashi Number (Figure 2) was used to measure ideal mandibular restoration. In studies of approximately 500 patients, Henry Shimbashi, DDS, of Edmonton, Alberta, Canada, determined that an ideal relationship exists between the maxilla and mandible, and that part of this relationship includes a measurement from the gingival margins of the maxillary central incisors to the gingival margins of the mandibular incisors; Shimbashi concluded that the ideal measurement is 19 mm, plus or minus 1 mm.1 When an optimal position exists for the lower jaw relative to the upper jaw, the muscles that are connected to them will also be at their optimal length and can function ideally.
Next, a spider web framework design was laid out to build a screw-retained acrylic base with ceramics. The benefits of utilizing a spider web frame design include minimizing metal usage, therefore reducing the weight of the prosthesis while maximizing its strength, as well as allowing easy bonding of the resin without the use of retention beads. It creates a natural undercut for smooth fitting and firm retention.
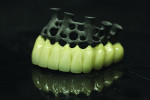
Additionally, the technicians wanted more support on the substructure, so they applied a technique from the masonry field: They utilized offset structural elements similar to a brick wall. The intentional design of an unevenly distributed connecting line provides more strength than a straight, even-lined substructure would (Figure 3). It also creates a natural undercut to better hold the resin and metal framework while preventing distortion of the metal substructure.
Gingival Characterization
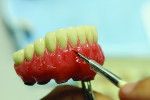
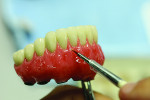
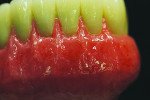
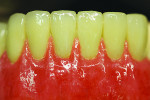
With the foundation of the spider web framework, a porcelain buildup and gingival characterization plan was followed. After the acrylic base was processed to the framework and festooned, a composite stain was artistically applied from the CEJ apically to imitate the natural texture of the gingiva.
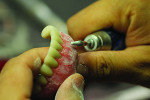
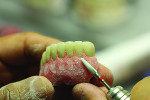
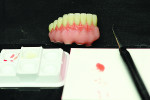
Figure 4 shows the preparation for the composite and stain. More space was provided by utilizing a grinding bur. The groundwork was then set for contouring and characterization, rendering the natural curves of the gingiva according to the shape of the roots (Figure 5). The technician mixed multiple shades of stain directly onto the composite to portray the patient’s natural tissue (Figure 6). This also created a unique, customized, and natural look.
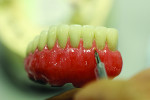
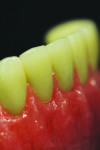
Figure 7 shows the start from embrasure to embrasure, and in Figure 8 a different angle was used to check throughout the basework. Figure 9 shows the completed composite.
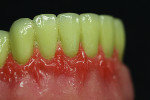
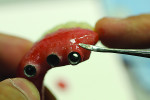
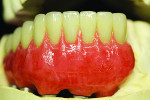
Figure 10 through Figure 12 show the stain being applied from the CEJ apically. A main focus was to portray blood vessels and reflection of the highlight. The extension of the opaque past the gum line was intentional to portray the look of root portion of the tooth under the acrylic.
Figure 13 shows the finishing and trimming, and Figure 14 shows the final curing.
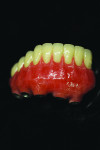
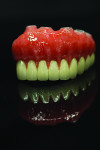
Using precise measurements, the technicians bulked up the acrylic base to fill the patient’s bone loss space and provide lip and chin support to the facial anatomy (Figure 17 and Figure 18).
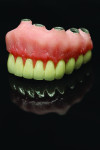
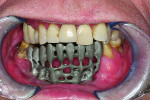
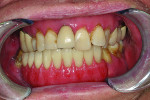
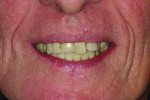
Ultimately, the plan of combining acrylic’s lightness with the esthetic beauty of ceramic was fulfilled (Figure 15 through Figure 20). After the framework try-in (Figure 21) and final delivery (Figure 22), the patient’s smile shows a well-supported lip and mandibular restoration (Figure 23).
Conclusion
The definitive prosthesis for the patient presented in this article needed to be completed within a short time period without sacrificing form, function, and esthetics. The entire team — dental office, patient, and dental technicians — were extremely pleased with the successful outcome. A crucial factor in this process was the technicians’ open mindset, which allowed them to blend techniques from the past as well as the present, and their artistic creativity allowed the laboratory team to help restore this patient’s life after the brutal effects of oral cancer and treatment.
Disclosure
The authors had no disclosures to report.
Reference
1. Long HA. A Predictable Approach to an All-Ceramic Full-Arch Restoration. Compend Contin Educ Dent. 2013;34(4):274-281.
About the Authors
Jayme Hong
CEO
IDOC Dental Lab, Inc.
Orange, California
Eric Park, CDT, LVI
Master Ceramist
IDOC Dental Lab, Inc.
Orange, California
Seong J. Kim, CDT
Master Metal Technician
IDOC Dental Lab, Inc.
Orange, California