Accident Case: Diagnosis and Prep Design Following the Treatment Plan Wax-Up
Utilizing a specialized digital concept to create natural color
Luke S. Kahng, CDT
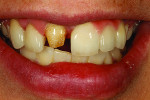
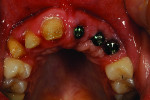
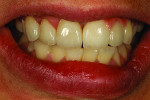
Technicians often face difficult cases and have to imagine themselves in the patient’s mindset to help understand the patient’s experiences and expectations. This case study will focus on a female in her mid-20s who had been in a car accident. Her case was, therefore, rehabilitative. By the time she came to see the author, she had received oral surgery in order to have 3 implants placed.
In this process, she had consulted with multiple dental professionals and had decided on a treatment plan and detailed guide for her final restorations. She was looking for predictability but also high esthetics.
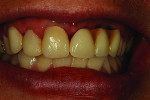
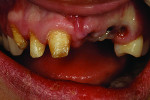
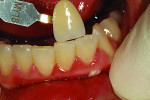
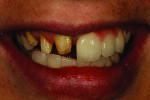
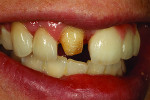
When she visited the author’s laboratory for her appointment, she was wearing a plastic flipper, which was easy to fit into her mouth and remove. But due to problems caused by the missing dentition, the adjacent teeth had shifted and created subtle occlusion contact. The mandibular teeth erupted, hence the need for placement of 3 implants, as noted above.
During the custom shade appointment, the author recorded that the patient’s midline had been offset and would need correction during the rehabilitation. Her flipper was strictly temporary, which she knew. The patient was eager to begin the rehabilitation of her smile.
Through the outlined treatment plan, preparation design, wax-up contour, and tooth shaping, the author was able to utilize the specialized digital concept to create natural color from an excellent foundation and create high esthetics for the patient.
Case Study
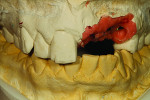
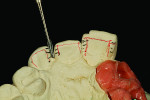
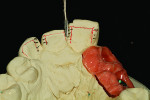
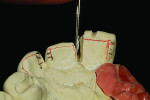
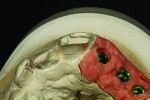
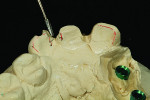
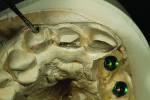
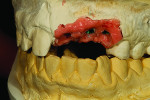
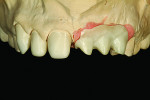
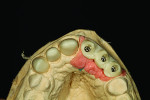
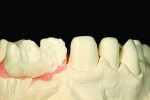
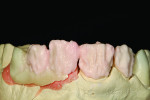
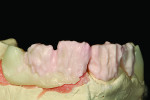
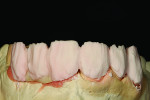
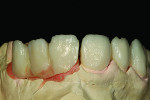
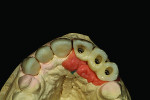
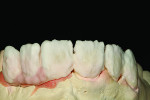
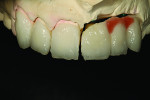
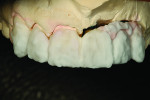
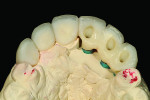
Figure 1 shows how the preoperative model had been poured up and mounted with the opposing. In this mounted alignment, the arches lined up. Next, with a pencil, the author drew black lines on the model to break the interproximal contact (Figure 2) from the canine to the central in order to “open up” the central teeth. Figure 3 provides an occlusal view for facial reduction and the incisal 1.5-mm reduction. Figure 4 shows a black line that the author had drawn to mark the tissue contour that he and the dentist discussed preparing. The clinician later performed a gingivectomy to help create that rounder appearance in the shaping of the gingiva line.
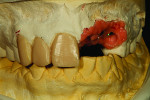
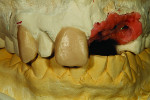
The author then moved forward with his preparation design for the canines. After completing the model preparation, he photographed the frontal and side views. The rough wax design was completed on the model for teeth Nos. 6 and 8 and then for tooth No. 7 as well (Figure 5).
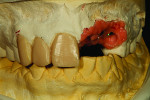
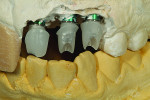
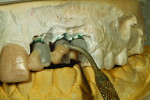
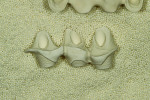
The author then placed a titanium base onto the model for the implants (Figure 6) and created dummy copings from his in-house milling machine. The implant cement-retained dummy copings were placed on the model (Figure 7). The author then completed the wax-up (Figure 8). He later recommended a screw-retained bridge because, in his opinion, the laboratory would not be able to duplicate the patient’s tissues with cement-retained restorations. He believed the gingival line area would need high contour for tissue and shape, and the dentist agreed.
The processing and milling of the restorations was handled in the laboratory with Ceramill Motion 2 milling machines (Amann Girrbach, amanngirrbach.com). The pre-shaded appearance is shown in Figure 9. After sintering, the margins and design were modified (Figure 10). In the author’s opinion, this stage is critical because the frame design must not be compromised. Next, the facial contour for the screw-retained bridge is shown on the model (Figure 11).
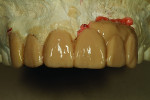
An interior color No. 44 was applied (Figure 12) before an A1 base dentin (Figure 13), and then was cut back. After firing at 810° C, the copings were then ready for their second buildup. On the model, the author performed a facial contour check for teeth Nos. 6 through 11 (Figure 14). Various shades of porcelain were used during his multilayering technique, illustrated in Figure 15 during his second buildup consisting of dentin, enamel, and pink porcelain for gingival enamel. After firing, the restorations were again placed on the model (Figure 16) before being baked a third time. In Figure 17, the restorations are in the bisque bake stage, and Figure 18 shows a mirrored image of the screw-retained, layered porcelain implant bridge.
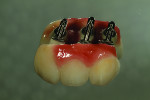
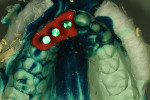
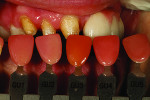
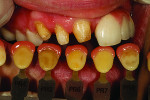
Preoperatively, the patient was wearing the aforementioned plastic removable flipper, and the dentist took an impression for the laboratory (Figure 19). Figure 20 is an image of his preparation design for teeth Nos. 6 through 8 and implants for site Nos. 9 through 11. A shade check was noted for the lower anterior teeth (Figure 21) before the pink tissue color was selected using the author-fabricated ceramic shade tabs (Figure 22). For a final preparation color check, the author again used his ceramic shade tabs.
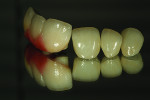
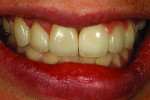
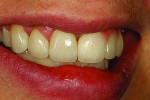
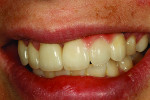
The screw-retained implant zirconia bridge was tried in for teeth Nos. 9 through 11 and then teeth Nos. 6 and 7 singles, after which tooth No. 8 was added for an immediate smile view (Figure 23). An occlusion view is shown in Figure 24, with healing caps in place and then a left view comparing the size of teeth Nos. 7 and 9 (Figure 25). Immediately after a full try-in, the author photographed the patient from multiple views. The final image of the patient illustrates the harmony and blending of color that the author was able to achieve due to the planning and care taken with the case during each step (Figure 26). A radiograph of the screw-retained bridge is the final image (Figure 27).
Conclusion
By having open and continual communication, the dentist, patient, and technician were able to reach the final goal established for this case. The patient was pleased with her final restorations, telling the author that they looked better than her natural teeth.
The treatment plan, material selection, color, and the size of the teeth had been discussed beforehand, leading to superior results. Everyone involved was happy with the outcome.
About the Author
Luke S. Kahng, CDT
Owner/Founder
LSK121 Oral Prosthetics
Naperville, IL