PREAT’s eFiber
A stronger and more esthetic option for reinforcing dental prosthetics
Prosthesis fracture is a common pitfall when providing a patient with an interim or provisional implant supported fixed resin prosthesis. The provisional restoration is important because it helps the dental team evaluate comfort, function, and esthetics in order to design the final restoration. Common steps to reduce fracture include shortening the arch, eliminating cantilevered teeth, taking the prosthesis out of occlusion, and reinforcing with metal, Kevlar, or cable fibers.
“Cable fiber reinforced dentures shatter in half every time,” says James Angelone, Clinical Dental Technician, owner of Ohio Professional Dental Lab, “I get called in to repair cable reinforced prosthetics every day.” Angelone has been reinforcing his dentures with the PREAT Corporation’s eFiber for the past year. He has found that since incorporating this material into his work, the dentures have become stronger and more durable.
PREAT’s eFiber is unique because it is impregnated with both PMMA (acrylic) and BIS-GMA (composite). This affords the dental team the choice of using either acrylic or composite resins with a reinforcement material that uniquely chemically bonds to both choices. In addition, because it fully bonds with resins, eFiber may be ground and polished, thus eliminating the annoying fraying fibers that can occur when other materials are adjusted.
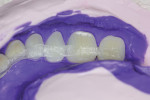
The placement of fiber is key to maximizing prosthesis strength. The area of the greatest tension is the incisal notch, and reinforcement placed perpendicular to these fracture forces at the optimal position—the juncture of denture tooth and acrylic—stops fractures before they begin. eFiber provides over 1400 MPa of flexural strength and over 100,000 biting cycles in fatigue testing.
eFiber may be used to easily and quickly reinforce traditional dentures, implant overdentures, and provisional and definitive fixed detachables. The goal when using eFiber in new cases is to stop a crack before it begins. Therefore, eFiber is placed at the prosthesis’ weakest position—the juncture of teeth and acrylic—and bonded directly to the denture teeth. A secondary benefit of this process is increased denture tooth retention and splinting.
Chris Norris, Removable and Implants Manager at Image Dental Laboratory, has experienced massive success using eFiber in his laboratory. He describes, “eFiber is definitely stronger than anything else, especially when placed in the cingulum of anterior teeth or ridgelap of posterior teeth.”
When placing eFiber, wax rope is used to measure the required length, and then the fiber is cut with scissors. Starting with the most posterior tooth, eFiber is pressed onto the tooth surface and the stepper tool is used to blockout the adjacent material while light curing the fiber, one tooth at a time, with a hand held light. The entire process should only take about 90 seconds.
After the eFiber has been bonded to the ridgelap of the denture teeth, normal denture processing techniques are utilized—inject, pack, or pour—for final processing. This is the ideal time during non-conversion cases to reinforce the intaglio surface by connecting the opaque temporary implant cylinders together with another strand of eFiber.
After wearing the fixed detachable provisional for eight weeks, the patient can provide helpful feedback regarding the esthetics, comfort, and function of the prosthesis. Any necessary adjustments to occlusion, lip support, incisal edge position, and speech are made at this time. Ultimately, a well-designed provisional will serve as a template for the laboratory technicians as they begin to fabricate the final prosthesis.
Reinforcing provisional implant prosthetics with eFiber has allowed Angelone to warranty his work. “They just don’t break, so I warranty them. My dentists love that there are no fractures or repairs.” For clinicians, eFiber eliminates non-revenue chairside time, provides peace of mind for the dental team, and provides the patient with the best restoration possible in only 10 minutes of bench time with no additional equipment necessary.
Disclaimer: The preceding material was provided by the manufacturer. The statements and opinions contained therein are solely those of the manufacturer and not of the editors, publisher, or the Editorial Board of Inside Dental Technology.
For more information, contact:
PREAT Corporation
P 800-232-7732
W www.preat.com