Team Diagnostics and Analyses Solve Difficult Cases
A look at six cases to restore chips and breaks in natural dentition
Nothing is more rewarding for a dental technician than helping clients solve a difficult case. That is especially true when patients present with a small defect on an anterior or posterior tooth. These types of cases are often not only difficult to repair adequately chairside, but they are also difficult for patients if conventional indirect treatment options are proposed. Patients may be upset when informed that their dentist will need to remove their remaining healthy tooth structure in order to repair such a small defect. In these circumstances, technicians have the opportunity to make their client dentists look like heroes by using indirect additive techniques that eliminate the need for gross tooth reduction, anesthesia, and sometimes drilling.
Most often dental technicians receive the case only after the teeth have been prepared. It is an unfortunate reality that most clinicians elect restorative options that require gross reduction of healthy tooth structure in order to restore slightly chipped or broken dentition. While no-preparation cases should be hand picked, tooth structure conservation should always be a priority when restoring damaged dentition. This article will feature case studies using indirect additive techniques that dentists and dental technicians can use to restore minor chips and breaks in natural dentition. These techniques are beneficial not only to the dentist clients, but most importantly to the patient.
Case 1
It is very common for patients to present with chipped teeth in the posterior region of the mouth. For the patient, a chipped tooth is often uncomfortable and needs to be restored due to pain, loss of esthetics, or partial loss of function. In many cases, gross preparation treatment protocols are not necessary. By using indirect additive techniques, small defects can be restored using either feldspathic ceramic or pressed techniques.
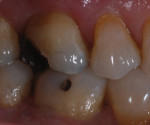
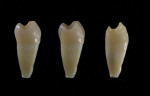
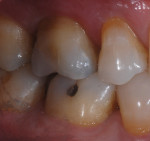
Posterior teeth chip for many reasons. The patient presented here cracked a tooth when chewing on a piece of ice (Figure 1). In order to restore the tooth back to its natural function and esthetics, dental technicians must always remember to study nature. When using refractory veneering techniques, the ceramic must always follow a natural build up. The dentin must be layered to the same contours observed in nature. Figure 2 illustrates how the dentinal cone was layered in the way nature intended. Dental professionals can understand this concept better by analyzing natural dentition that has been stripped of enamel using hydrochloric acid to show the underlying dentinal makeup.
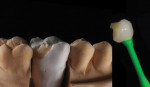
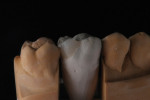
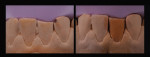
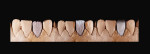
Once the dentin layer has been properly applied (Figure 3), the enamel layer can be overlaid to create the natural composition of the previous cusp tip that had chipped away (Figure 4). Figure 5 shows the final outcome of the additive chip.
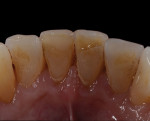
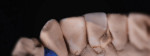
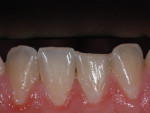
Additive veneering can also be used to help relieve a patient’s discomfort. The patient shown in Figure 6 presented with a rough lingual surface on his lower central incisor. The rough surface abraded his tongue as it pressed against the surface during meals or even when he spoke. Using refractory veneering techniques, an enamel shell was created (Figure 7) that fit his lingual surface precisely, covering the roughened area with smooth new enamel that was both comfortable and unobtrusive for the patient’s tongue (Figure 8).
Case 2
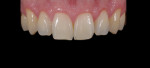
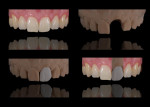
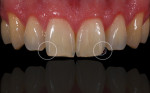
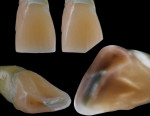
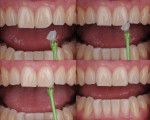
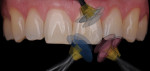
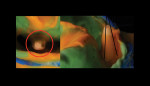
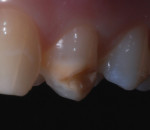
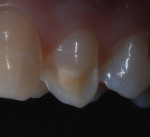
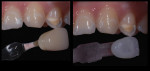
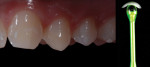
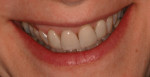
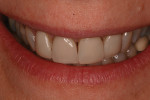
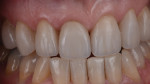
Anterior esthetics plays a significant role in restoring chipped or worn dentition. The patient shown in Figure 9 chipped the distal area of tooth No. 9 during a surfing accident. His goal was to restore the tooth to its natural shape and esthetics. Using additive techniques, the dental team eliminated the preparation stage and merely smoothed the tooth surface where the chip occurred to ensure there were no sharp angles. An impression was taken of the chip and an alveolar model was fabricated to restore the case using the refractory die technique (Figure 10). The refractory die was then burned out in a KDF burnout oven (KDF US, www.kdfus.com). This oven is preferred because it enables the technician to completely control the rise and stages of the degas cycle. Before the ceramic layering process begins, one must analyze the adjacent teeth to determine color selection (Figure 11). Although the chip was small, it was evident from studying similar situations on natural dentition that many different shades would be involved in restoring such a small space (Figure 12). Once the shading was analyzed and the ceramic colors and effects were determined, the ceramic layering was accomplished (Figure 13). The chip was finalized on the refractory die and then divested. Because of the fragile nature and size of the chip, the refractory material was cut with a disc in close proximity to the chip and then embedded in a silicone matrix (Figure 14). The silicone allows the restoration to divest without the chip blowing away. The restorative chip was then etched and finished with ceramic etching gel (Tri-Dynamics, Pearson Dental Supplies, www.pearson.com) and rinsed clean with hydrofluoric acid to ensure a strong bond (Figure 15). The chip was then affixed to a seating tool for easy handling, and wax was used to hold the chip steady for the try-in. Once in place on the tooth, the entire tooth and restoration are hydrated with water to determine if the chameleon effect had been achieved (Figure 16). The chip was then bonded to the remaining natural tooth structure and finished intraorally on the extended clear margins until a seamless effect was achieved (Figure 17). The final restoration exhibited the vitality of a natural
tooth (Figure 18).
Case 3
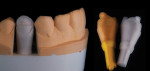
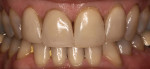
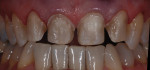
Lower anterior teeth are also very susceptible to trauma and chip quite often. The no- preparation chip technique is an appropriate restorative treatment for these situations as well. This patient presented with a chip to his lower central incisor (Figure 19). For this case, an alveolar model was created to follow the refractory die technique using G-Cera® ORBIT VEST (GC America, www.gcamerica.com) refractory die material (Figure 20). To create an alveolar model, the main objective is to use a bur that will not create any undercuts (Figure 21). The die was cut to mimic a root formation and embedded back into the impression to check for any undercuts that would not allow the die to be ejected from the master stone cast (Figure 22). Once the alveolar model had been poured and the die removed, it was imperative to check the removable die with a silicone index of the solid model to ensure accuracy (Figure 23). The die was then sealed with GC Initial™ clear ceramic and fired at 50 degrees higher than the final temperature (Figure 24). Ceramic layering, following the principles of nature, was then carried out. A thin layer of dentin was applied to help block out any chip line or junction, and then the enamels were overlaid over the dentin layer (GC Initial dentin A1, e58/clear, and eop3, eop2) (Figure 25). Once the ceramic application was finished on the die, it was ready for divesting. While still on the refractory die, the restorative chip was embedded in silicone and sandblasted at a very low pressure to ensure no holes were blown through it (Figure 26). Once divested, the fragile chip was handled with delicate care during try-in (Figure 27). The try-in confirmed color match and fit accuracy. The chip was finished intraorally (Figure 28) to blend harmoniously with surrounding dentition (Figure 29).
Case 4
Restoring a chip in a tooth can also conserve natural dentition when the tooth has to be prepared. In this case, the patient presented with both an esthetic and hygienic concern on her upper bicuspid (Figure 30). When diagnosing for the prepared design, the dentist can preserve very important aspects of the natural dentition to help aid the technician in achieving a natural result. For this case, the dentist was able to preserve the natural incisal edge (Figure 31). The treatment plan called for the fabrication of a facial inlay using feldspathic ceramic. A shade was taken for the natural dentin and a custom ceramic tab was created (Figure 32) to determine the enamel overlay (GC Initial MC e0p3/e58/cl). A fast efficient model system from UniPin (Schutz Dental Group, www.schuetz-dental.de) was used to fabricate the chip using the refractory layering technique (Figure 33). Once layered, the chip was divested and fit into the facial inlay preparation for seamless integration (Figure 34).
Case 5
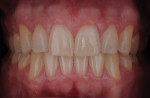
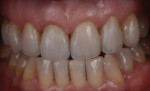
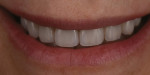
Additive feldspathic chips can also help complete a case and allow for a conservative approach. This patient presented with old veneers that she was very unhappy with (Figure 35 through Figure 37). The patient understood that the old veneers had to be removed, but she did not want to restore any other teeth due to her fear of destroying more of her natural dentition in order to achieve her desired final outcome. Analyzing the case, it was decided both goals could be achieved using no-preparation veneers on her canines and premolars since the dental team would be filling in her buccal corridor and broadening her arch. The patient accepted the treatment plan. The old veneers were removed and refinished leaving the remaining teeth to be restored untouched. In this case, facial veneers were created for the unprepared teeth. The facial veneers had a higher bond strength due to the fact that they were bonded to enamel (Figure 38). The finished case demonstrates the major improvement esthetically by incorporating six additional veneers into the treatment plan without preparing anything other than the old restorations (Figure 39 and Figure 40). The patient was extremely satisfied with her new smile and the conservative approach used to achieve the highly esthetic outcome (Figure 41).
Case 6
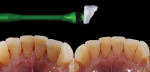
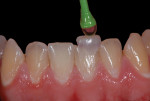
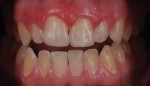
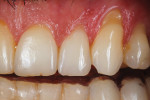
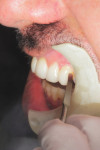
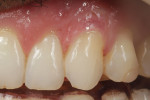
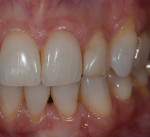
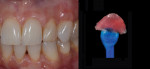
Adding restorative chips can also offer treatment options for dentists solving difficult cases. In the following case, the patient complained of a non-esthetic abfraction on his canine (Figure 42). The patient was given the option of periodontal surgery. He did not want to go through surgery due to the time investment, expense, and associated pain. With this in mind, the dental team solved the case by creating a pink composite chip to veneer the non-esthetic area. Either GRADIA® gum (GC America) or Anaxgum (anaxdent, www.anaxdent.com) pink composite can be used to fill and match the veneer intraorally (Figure 43). The color and form of the composite veneer chip was matched and the restoration was finished and glazed indirectly for a hygienic fit. Once finished, the composite chip was etched and treated before bonding to the abfraction (Figure 44). Placed in the mouth, the patient could see the difference immediately (Figure 45). If the patient ever does decide to undergo periodontal surgery, the composite veneer will act as a guide for the surgeon. A common complaint from patients exhibiting abfractions is tooth sensitivity (Figure 46). For this case, the pink veneer was created more to alleviate sensitivity for the patient than to optimize the esthetic outcome (Figure 47).
Conclusion
While the cases presented are unique and delicate, they cannot be achieved without the following criteria—an educated dentist and patient, good photographic documentation, accurate models, no sharp edges on dentition to be restored, a variety of ceramics to block out and mimic nature, and, most importantly, trust from your doctors. These cases will not yield the desired results if any one of these variables is missing from the equation. This article can serve as an educational tool to share with your clients on modern veneering techniques and how they can be applied in today’s dentistry.
Advancements in dental materials are providing dentists and technicians with an increased number of restorative options and solutions. Paramount to any case is properly diagnosing the problem and finding a solution and treatment option that meet the patient’s goals economically, esthetically, and as conservatively as possible. Conservative dentistry should always be the top priority when diagnosing cases. Once nature is destroyed, it has to be replaced. The best possible way to restore nature is to have nature on your side by preserving tooth structure.
Acknowledgment
The author would like to thank Dr. Barry Polansky, Dr. Joseph Cohen, Dr. Thomas, Backenstose, and Dr. Javier Vasquez for the dentistry in the article.
Find out why dental photography is so important in Joshua’s May 2012 article in Inside Dentistry, “A Picture is Worth a Thousand Words,” at dentalaegis.com/go/idt346
About the Author
Joshua Polansky, MDC, BA
Owner
Niche Dental Studio
Cherry Hill, New Jersey