Complete Denture Retention
Atmospheric pressure devices can play a major role in resisting dislodging forces.
By Martin Rigutto
Clinicians generally accept that denture retention is dependent on the control of the flow of saliva, its viscosity, and film thickness. Interfacial surface tension contributes to retention,1,2 but the most important are good base adaptation and border seal.3-5 This may be relevant to maxillary dentures. However, mandibular dentures will stand helpless in resisting dislodging forces due to their smaller support area, unfavorable distribution of occlusal forces, and an increased rate of bone resorption.6 The use of endosseous implants can certainly assist in the support and stabilization of complete maxillary dentures.7,8 However, there are situations when it is impossible to prescribe implant surgery to patients that are unable or unwilling to undergo implant surgery on medical grounds or financial constraints.9 In an effort to overcome many of the retention problems associated with maxillary dentures, what may be the role of atmospheric pressure devices as an effective, non-invasive procedure for enhancing denture retention was investigated.10
Atmospheric pressure has been claimed to be an important factor in complete denture retention.12,13 For atmospheric pressure to be fully effective, there must be a lower pressure beneath the dentures and vacuum must be present. If the dentures have an effective seal around their borders, atmospheric pressure can act to resist dislodging forces.14,15 This is called suction, because it is the resistance to removal in a direction opposite to that of insertion. But there is no suction or negative pressure, except when another force is applied.16
Under the assumption that vacuum could be generated by exerting a pull to increase the volume beneath the dentures, lower atmospheric pressure would have to be generated by external means and a seal must be created and maintained around their entire borders for the vacuum to be sustained.17 This can be achieved by taking full advantage of the mechanism principle of denture valves.
How Do They Work?
Two unidirectional valves are embedded into the denture plate, one on each side of the lingual flanges or on the palatal aspect of the denture. As the wearer bites firmly, the air trapped between the mucosa and the base of the denture is expelled through the valves via two tiny 1-mm air passages, creating a negative atmospheric pressure beneath the denture. The diaphragms seal off the one-way valves, preventing air reintroduction. The lower pressure obtained beneath the denture tends to exert a pull and helps to secure the denture against the ridge, resulting in a better fit to the tissue and improved resistance to dislodging forces.
Following are the step-by-step procedures for laboratory processing of the UltraSuction denture system:
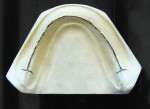
1. A Type III hard stone model is fabricated from the impression of the edentulous ridge (Figure 1).
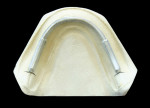
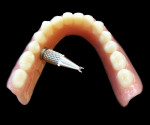
2. The location of the profiled bar is precisely placed in the middle of the ridge (Figure 2). It must stop 1 cm short of the end of the denture’s pad or notch, depending on whether it is an upper or lower denture. If necessary, the bar can be cut to the proper length.
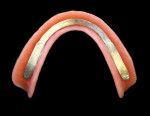
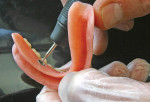
3. The profiled bar is stabilized on the model by using two to three small drops of cynoacrylate (Super Glue® type), making sure to block out the undercuts (Figure 3). The bar is burnished as closely as possible to the ridge form. The teeth are set for try-in. Note: The bar will remain on the model during acrylic processing. Alternate procedure: Bar may be placed after the boiling out procedure following the above process of burnishing and blocking undercuts.
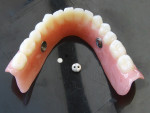
4. After polymerization, the profiled bar is carefully removed, paying particular attention not to damage the walls of the suction chamber (Figure 4). Note: Only a fine filing of the edges is permitted. The same process applies when used in conjunction with soft liners.
5. Two cavities are prepared at the chosen lingual site in which the valves will be placed (Figure 5).
6. The graded end of the key may be used for guidance at the top of the notched area for depth and diameter where the valve body assembly is placed (Figure 6).
7. A brass processing cap is placed in each valve to protect the core from being filled with acrylic (Figure 7). Process and place the valve body carefully with self-curing acrylic. After polishing, the processing cap is removed. Note: An analog will be made available that will eliminate the post curing of the valve body.
8. Using a 1-mm bur, a communication channel approximately 2 mm in depth is drilled in line with the center access hole of the valve body at the top of the air chamber (Figure 8). Drill the channel on an angle, guided by the transparency of the acrylic, to just above the air chamber 1 mm to 2 mm.
9. Carefully join the communication channel from valve body to the previously made channel from underneath the denture at the top of the air chamber using the same fissure 1-mm barrel bur drill (Figure 9). Always make sure the channel from the valve body is made in line above the high point of the air chamber, not the side. Do not scar the metal. Guided by the transparency of the acrylic to just above the air chamber, the two channels that make the denture stable are complete.
10. Rinse the denture and air-dry (Figure 10). A plastic diaphragm is placed in each valve and the perforated cover is closed using the key provided.
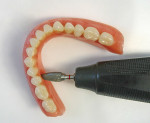
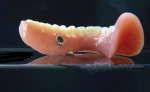
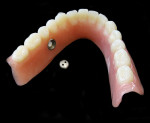
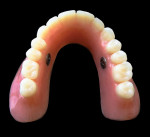
11. The finished upper and lower dentures with installed UltraSuction™ valves are completed (Figure 11 and Figure 12).
Conclusion
The UltraSuction system increases the retention of mandibular complete dentures. Their retentive capacity in comparison to conventional mandibular dentures has been positively demonstrated in clinical studies and retention tests.11
Martin Rigutto is the president of OnCore Dental Inc. OnCore Dental Inc. is the US distributor of UltraSuction™.
For more information, contact:
OnCore Dental Inc
Phone 360-841-8426
Web www.oncore-dental.com
E-mail martin@oncore.com
Disclaimer
The preceding material was provided by the manufacturer. The statements and opinions contained therein are solely those of the manufacturer and not of the editors, publisher, or the Editorial Board of Inside Dental Technology.
For more information on the UltraSuction System, please visit www.dentalaegis.com/go/idt18
References
1. Page HL. Mucostatics, a principle not a “technique.” Chicago, IL: Published by author; 1946:22-23.
2. Barco MT Jr, Dembert ML. Cast aluminium denture base. J Prosthet Dent. 1987;58(2):179-186.
3. Roessler DM. Complete denture success for patients and dentists. Int Dent J. 2003;53(5):340-345.
4. DeMagistris DP. Physicomechanical characterization and formulation of natural, modified natural, and synthetic polymers including polymer salt and ester derivatives as oral bioadhesive materials. Ann Arbor, MI: University Microfilms, Inc.; 1981:1-48.
5. Mazurat NM, Mazurat RD. Discuss before fabricating: communicating the realities of partial denture therapy. Part II: clinical outcomes. J Can Dent Assoc. 2003;69(2):96-100.
6. Zarb GA, Bolender CL, Carlsson G, eds. Boucher’s Prosthodontic Treatment for Edentulous Patients. 11th ed. St. Louis, MO: C.V. Mosby; 1997:460-468.
7. Ambard AJ, Fanchiang J, Mueninghoff L, Dasanayake A. Cleansability of and patients’ satisfaction with implant-retained overdentures: a retrospective comparison of two attachment methods. J Am Dent Assoc. 2002;133(9):1237-1242.
8. Misch CE. Dental Implant Prosthetics. St. Louis, MO: Mosby; 2005:211, 223.
9. Gahan MJ, Walmsley AD. The neutral zone impression revisited. Br Dent J. 2005;198(5):269-272.
10. Cox AM. A consideration of the fundamental physical principles involved in the retention of artificial dentures. Br Dent J. 1926;47:1059-1071.
11. Badra SH, Radi I, Aboulela A. The effect of ultra suction system on the retention of mandibular complete denture. Egypt Dent J. 2010;56(1):101-109.
12. Hoffman-Axthelm W. History of Dentistry. Philadelphia, PA: Quintessence; 1981.
13. Jacobson TE, Krol AJ. A contemporary review of the factors involved in complete denture retention, stability, and support. Part I: retention. J Prosthet Dent. 1983;49(1):5-15.
14. Hall RE. Retention of full dentures. Dent Items of Interest. 1919;41:292-305.
15. Kubali KN. The theoretic basis of the functional vacuum method for complete denture construction. J Prosthet Dent. 1960;10:673-681.
16. Shay K. The retention of complete dentures. In: Zarb GA, Bolender, CL, Carlsson GE, eds. Boucher’s Prosthodontic Treatment for Edentulous Patients. 11th ed. St. Louis: MO: Mosby; 1997:400-411.
17. Darwell BW, Clark RK. The physical mechanisms of complete denture retention. Br Dent J. 2005;189(5):248-252.