Low-Risk Dentistry Using Additive-Only (“No-Prep”) Porcelain Veneers
Abstract
“No-prep” porcelain veneers have been effectively in use for more than two decades, and the bonding of porcelain to 100% enamel has enjoyed extraordinary success. Today’s refined techniques, new and improved materials, and better training in emulating nature have enabled additive-only veneers to rival, or in some cases even exceed, the results of traditionally prepared veneers. In this case presentation, the author uses conservative, additive-only dentistry to enhance a young woman’s smile by creating improved anterior esthetics.
Kois Center Case of the Month
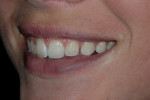
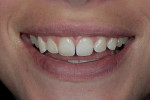
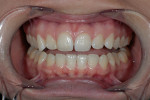
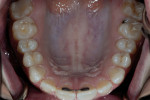
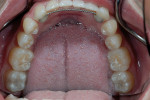
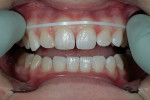
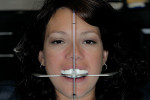
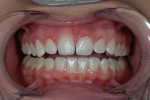
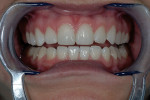
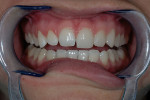
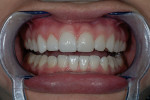
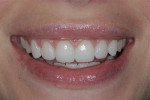
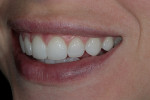
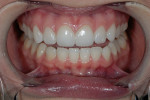
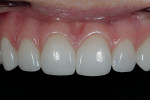
A 26-year-old woman reported to the author’s office with a desire to improve her smile. Her chief concerns included multiple diastemas present in the anterior, discolored composite bonding on tooth No. 7, and a generalized yellow hue (Figure 1, Figure 2, Figure 3 and Figure 4). She desired her teeth to have more “presence,” both in architecture and color. She stated that her orthodontist struggled to close all of the spaces while she was a teenager, and that she had fixed lingual retainers ever since.
Medical History
The patient reported to be in excellent health, and her health history was unremarkable.
Dental History
Other than the orthodontic treatment, there was very little dental history, with only a few small restorations on her permanent molars noted.
Diagnostic Findings
Temporomandibular Joints: A clinical exam revealed all facets within normal limits with no clicking or crepitus upon opening and closing. Maximum opening was within average range with no deviation upon opening and closing. Load testing produced no pain or discomfort.
Extraoral: Exam found everything within normal limits.
Intraoral: Exam found everything within normal limits. A cancer exam accompanied with a VELscope survey was negative. The patient had a Class 1 cuspid and molar relationship, with a midline shift to the right approximately 1 mm. In addition, a slight anterior cant was noted so that tooth No. 6 was slightly lower than No. 11 from a horizontal perspective.
Diagnosis
Periodontal: The patient was healthy periodontally, with little to no evidence of gingival inflammation. Bone levels were optimal.
Biomechanical: The patient appeared to have minimal risk, with only a few small restorations present and no existing decay.
Functional: The patient had highly acceptable function with no visible signs of wear or instability (Figure 5, Figure 6 and Figure 7). It is likely that at one time there was anterior constriction, which would account for the opening of spaces in the anterior post-orthodontics. The patient reported stability of the anterior teeth in recent years, and there was no detectable mobility.
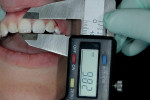
Dentofacial: The patient appeared to have a tooth/arch size discrepancy, with the dental arches having more space than the teeth could occupy. In addition, there was a slight cant from right to left, with the gingival architectures being lower on the right canine and lateral than on the left side. Another observation was the relatively large size of the lips and oral cavity (the frame) in relation to the size of the teeth, which typically makes these types of cases good candidates for additive-only or “no-prep” restorations. Figure 8 documents that the upper central incisors were less than 10 mm in length, which is further evidence that the teeth may be slightly smaller than ideal.
Risk Assessment
Periodontal: Low
Biomechanical: Low
Functional: Low
Dentofacial: Low
The author’s goal, as always, was to maintain low risk factors by choosing treatment modalities that are minimally invasive and involve minimal risk.
Treatment Goals
1. Close spaces and create ideal anterior esthetics.
2. Eliminate the slight horizontal cant.
3. Create nice, bright color.
4. Accomplish all treatment as conservatively as possible.
Treatment Plan
1. Remove old bonding from tooth No. 7.
2. Whiten upper and lower teeth.
3. Use diode laser to adjust tissue levels to ideal architecture.
4. Create eight custom composite prototypes for teeth Nos. 5 through 12 to design the smile and serve as a “test drive” for the case.
5. Fabricate “no-prep” porcelain veneers for teeth Nos. 5 through 12.
Restorative
First, the old composite veneer had to be removed from tooth No. 7 using a 7910 carbide bur (Patterson Dental, www.pattersondental.com) with magnification, being careful to minimize enamel removal. Afterwards, the bone was sounded to confirm gingival excess; then the tissue heights were raised slightly on teeth Nos. 6, 7, and 9 using a diode laser. In many cases it is helpful to stretch a piece of floss across the gingivae to provide a straight line to visualize the amount of tissue removal needed (Figure 9 and Figure 10). In this case the goal was to guide the incisal length off of tooth No. 6 and guide the gingival architecture off of tooth No. 11 in order to correct the horizontal cant.
Obviously, with additive-only dentistry there is no preparation with a high-speed handpiece needed. The only minor alteration necessary in some cases, as was done in this case, is to smooth the incisal edges with a course disc (Sof-Lex™, 3M ESPE, www.3MESPE.com) to remove sharp internal surfaces. All of the teeth were then cleaned with an Enhance® polishing cup (DENTSPLY Caulk, www.caulk.com) to ensure there was no plaque or debris on the teeth. Two master impressions were captured with Precision™ heavy- and light-body impression material (Discus Dental, www.discusdental.com), which is the author’s routine practice so as to avoid any requests from the laboratory to remove the prototypes and make a new master impression. A Kois Dento-Facial Analyzer was used for proper orientation in a Panadent articulator (www.panadent.com), and a maximal intercuspal position (MIP) bite was captured using Blu-Mousse® (Parkell, Inc., www.parkell.com) (Figure 11)). Shade photographs were taken of the existing color, and the focus then shifted to creating the prototypes. Figure 12 shows the teeth just prior to creating the prototypes with the old bonding removed on tooth No. 7 and tissue architecture idealized.
Custom composite prototypes were fabricated by hand using Tetric EvoCeram® (Ivoclar Vivadent, www.ivoclarvivadent.com) shade Bleach L, spot-etching approximately a 2-mm to 3-mm circle in the mid-facial area. This composite is well suited for this application as it is highly viscous and does not slump or stick to the composite instrument. The Bleach L color provides an ideal white hue (020 range) while maintaining enamel-like translucency. Both centrals were formed before curing to maintain symmetry, followed by both laterals, both cuspids, and then both bicuspids. In essence, two teeth were done at a time before curing and moving to the next two teeth.
This technique works well to maintain symmetry of the contralateral teeth and also aids in keeping the smile line level with the horizon. Final contouring was done with burs and sandpaper disks to create proper line angles and facial anatomy, followed by polishing with a #12 Robinson Bristle brush and Diashine polishing paste (Brasseler USA, www.brasselerusa.com). Once the prototypes were finished, the patient was dismissed and asked to “test drive” them for several days.
Laboratory Instructions
After the patient had time to evaluate the prototypes a follow-up visit was scheduled in preparation for handing the job off to the laboratory. The patient was pleased with the prototypes, and, therefore, the architecture of the case was clearly established along with proper phonetics and occlusion (Figure 13). Photographs of the prototypes, along with an accurate polyvinyl impression, were taken so that the laboratory could copy the restorations with a silicone matrix of the model. Communicating color and incisal effects is a much more difficult task, but the prototypes provide a great deal of information in the color arena as well. Through years of handling these cases, the author’s ceramist knows which porcelain powders to use to match the 020 composite. If the patient desires a brighter or darker shade than the prototypes, adjustments can be made in the powder selection to match the requested shade. Since the thickness of these restorations greatly affects the final shade, it is invaluable to have a reference in color using the same thickness as the final restorations.
For this case, the final instructions to the laboratory were to:
- produce eight feldspathic prepless veneers (teeth Nos. 5 through 12).
- copy the prototypes in shade, length, facial anatomy, etc.
- place the margins just slightly shy of the tissue line.
- make the shade a slightly brighter color than the prototypes, somewhere between 010 and 020.
- make incisal translucency and characteristics similar to the original teeth.
Insertion and Finishing
After receiving the restorations from the laboratory they were carefully inspected for overall integrity and then placed on the master model to compare visually to the prototype model. It is always wise to handle these delicate restorations over a foam pad to ensure they do not fall on a hard surface and break. Following the author’s normal protocol, the patient was anesthetized to ensure comfort during the insertion process, as the chemicals and post-cementation finishing can be quite uncomfortable despite the fact that the teeth have not been prepared. The prototypes on only the right side were removed to compare the length, facial contours, etc, of the prototypes to the final restorations (Figure 14 and Figure 15). This is an important step to ensure that the laboratory duplicated the prototypes the patient approved. In addition, the shade was checked using clear try-in gel to verify that the color and effects closely matched what was ordered. The laboratory matched the blueprint extremely well, so the remaining prototypes were then removed and all the veneers were placed on the teeth with clear try-in gel to verify overall esthetics, fit, and appropriate contacts.
A rubber dam was then placed and the veneers were prepared along with the teeth using the exact same protocol as traditional veneers. Clear Variolink® cement (Ivoclar Vivadent) was used as the luting cement; it works well for thin veneers because they need a low-viscosity resin that requires minimal pressure to seat. All of the veneers were seated at once and spot-tacked into place with a 2-mm light tip. After the initial cement clean-up, the resin was completely polymerized.
The margins were finished into an “infinity margin” using “mosquito” finishing diamonds (Axis Dental, www.axisdental.com). Once the margins were no longer detectable with an explorer, they were refinished using the OptraFine® intraoral porcelain polishing system (Ivoclar Vivadent) followed by a #12 Robinson bristle brush and Diashine polishing paste. Careful attention was given to not traumatize the tissue by using deflecting retraction instruments. In addition, continuous air was blown on the teeth while polishing to guard against overheating.
The occlusion was evaluated and adjusted in centric occlusion and in lateral and protrusive movements. The lingual margins were then smoothed with a diamond-impregnated pre-polisher wheel (Axis Dental), followed by final polish with a Robinson Bristle brush and Diashine polishing paste. The patient was dismissed and returned 1 week later for an engineering check and final photos (Figure 16, Figure 17, Figure 18, Figure 19, Figure 20 and Figure 21).
Summary
By minimizing risk factors, additive-only dentistry can be an intensely rewarding procedure for both the dentist and patient. In this case, the patient was most pleased with the outcome and grateful for the conservative approach taken.
Acknowledgment
The author would like to thank Mark Willes at Experience Dental Studio in Provo, Utah for the ceramic work in this case.
About the Author
Dennis Wells, DDS
Private Practice
Nashville, Tennessee