A Systematic Method for Accurate Functional Diagnosis
Christopher Huff, DMD
Abstract
The “medical model” is a term coined for a set of procedures in which American physicians are trained. For dentistry, the sequentially ordered set of procedures includes: (1) immediate concerns; (2) medical/dental histories; (3) physical examination findings; (4) ancillary tests, if needed; (5) diagnosis; (6) risk assessment; (7) prognosis without treatment; (8) treatment-plan options/informed consent; (9) treatment; (10) post-treatment assessment and verification. This case report demonstrates a diagnostic system using the medical model via linear thinking—ie, step-by-step progression—to diagnose and conservatively treat a patient with a constricted chewing pattern.
Functional disease can lead to reduced tooth structure, pain, and tooth loss, as well as temporomandibular joint and neuromuscular dysfunction. Making an accurate determination of the cause of functional disease and providing the most conservative and effective treatment options can sometimes seem confusing and complex. The ultimate goal of treatment is to reduce the patient’s level of risk and improve the prognosis in the most conservative way. This requires rendering an accurate diagnosis. This article demonstrates a diagnostic system using the medical model via linear thinking to diagnose and conservatively treat a patient with a constricted chewing pattern.
Background
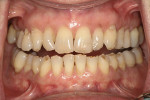
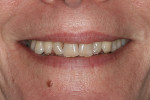
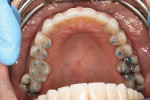
A 63-year-old female patient presented for her 6-month periodontal maintenance visit and expressed anxiety regarding increased wear and thinning of her front teeth (Figure 1). Several years earlier at the patient’s initial visit, concerns about the loss of tooth structure were discussed, but she was not troubled by it at the time. Now, however, the patient worried that her teeth might break or she might lose an anterior tooth. She wanted to prevent this from happening and correct the appearance of her front teeth.
Often, a functional diagnosis is reduced to attrition or abnormal wear, and an arbitrary diagnosis of bruxism is made rather than considering all contributing factors in an organized manner. Diagnosis is the determination of disease by the examination of disease indicators (signs/symptoms) and risk factors, and treatment is dependent on this process. Failure to diagnose or making a misdiagnosis may lead to a lack of treatment, wrong or inadequate treatment, or excess treatment.
The “medical model” is a term coined by psychiatrist R.D. Laing1 for a set of procedures in which American physicians are trained. For dentistry, that sequential order is as follows: (1) immediate concerns > (2) medical/dental histories > (3) physical examination findings (radiographs, photographs, models, and other data collection) > (4) ancillary tests, if needed (functional analysis, deprogrammer, salivary diagnostics, etc) > (5) diagnosis > (6) risk assessment > (7) prognosis without treatment > (8) treatment-plan options/informed consent > (9) treatment > (10) and post-treatment assessment and verification.
Linear thinking is a step-by-step progression in which a response to a step must be elicited before another step is taken. In such a system, each medical model step is considered—in order—without skipping any step, and a conclusion, the differential diagnosis, for each step is determined prior to moving to the next step until the definitive diagnosis is reached (Step 5).
If the sequential steps do not agree, the clinician must return to the initial step to find the error in reasoning or data collection. Without this linear process and consideration of all the risk factors and disease indicators (present and absent), diagnosis may be erroneously based on isolated signs, symptoms, or risk factors. The system’s inherent self-check mechanism allows the clinician to verify the definitive diagnosis and ensure the diagnostic protocol accuracy prior to treatment. For example, a new patient may present with a concern that his teeth are wearing short. A previous dentist may have diagnosed nocturnal bruxism and prescribed a nightguard. Despite being unaware of any grinding or clenching the patient still wore the appliance consistently and after 10 years was disappointed that the wear had continued. That diagnosis was based on one disease indicator, attrition, without consideration of all the disease indicators and risk factors. The result: ineffective therapy, further loss of tooth structure, the patient’s risk and prognosis never improving, and the cost of treatment now potentially much higher than necessary.
To implement the diagnostic system, several terms must be defined:
Disease: The cause of damage to the biologic system; that is, how and why the damage occurred (examples: caries, occlusal dysfunction).
Disease indicators (signs/symptoms): The damage caused by the disease, or how a disease expresses itself. These are the subjective/objective findings from the medical/dental histories and the physical examination (examples: cavity in a tooth, attrition, pain).
Risk factors: Variables that increase the probability of acquiring a disease. Example: Xerostomia is a risk factor for the disease caries.
Risk: The probability that further damage will occur to the biologic system due to the disease severity and risk factors that are present.
Prognosis: The prediction of what will happen to the biologic system based on the risk level, patient’s age, and patient’s expectations.
Functional Disease Differential Diagnosis (definitions courtesy of Dr. John Kois and the Kois Center)
Definitions regarding functional disease differential diagnosis include the following:
Acceptable function: Absence of a current functional disease.
Frictional chewing pattern (FCP): The patient’s maximum intercuspal position (MIP) is acceptable, but there are interfering teeth within the envelope of function.
Constricted chewing pattern (CCP): The orthopedic position of the mandible is the problem. The mandible is pushed back by the tooth position, constricting the envelope of function.
Occlusal dysfunction: Inefficient use of the masticatory muscles; posterior interferences into MIP create avoidance patterns, which may result from temporomandibular disorders.
Parafunction: Destructive use of the chewing system with no functional purpose, eg, nocturnal bruxism (4% to 8% of the population). Neurologic disorders: Conditions such as Parkinson’s disease and tardive dyskinesia; some medications can create this etiology.
Case Presentation
Step 1: Immediate Concern
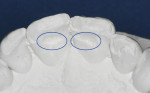
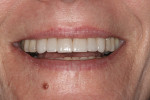
The patient’s concern was that her front teeth were wearing (Figure 2). Due to the progressive and noticeable loss of tooth structure to the patient, the diagnosis of acceptable function was eliminated from the differential diagnosis.
Step 2a: Medical History
The patient reported a history of hysterectomy and was treated with Evamist® for hormone replacement therapy. She also reported a herniated disk and used Mobic®, as needed. The patient denied any history of gastroesophageal reflux disease (GERD). Because there were no functional concerns related to her medical history, the diagnosis of neurologic disorders was eliminated from the differential diagnosis. Referring to the medical model flowchart (Table 1, Step 2a), note that this step complemented/corroborated the findings in Step 1.
This step requires a complete and accurate evaluation for any medical risk factors that may contribute to loss of tooth structure or occlusal disease. For example, diagnosis of GERD is strongly associated with sleep bruxism.2,3 A patient with sleep or breathing problems, such as obstructive sleep apnea, may exhibit altered mandibular posturing, which can result in occlusal and muscle dysfunction. Patients diagnosed with ADD/ADHD or who are taking antidepressant medications may present with movement disorders.
Step 2b: Dental History (Related to Functional Questions on Dental History Form)
Dental history questions related to bite and jaw joint function are listed in Figure 3. The patient reported occasional jaw discomfort and that she avoided chewing gum because of discomfort. She also described her mandible feeling as though it was pushed back when she closed her back teeth together. She felt the wear had increased over the past 3 years.
It is critical to discuss all the “yes/no” questions with the patient to clarify their meaning. The patient may not understand the meaning of a question or may not answer correctly. Failure to uncover the problem and understand the meaning of the answers may lead to critical errors in this step’s differential diagnosis. Referring to the medical model flowchart at this point (Table 1, Step 2b), the diagnosis of frictional chewing pattern was eliminated due to the fact that MIP was not acceptable because her mandible “felt pushed back.”
Step 3: Physical Examination/Data Collection
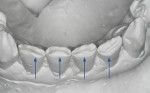
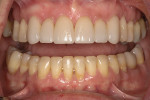
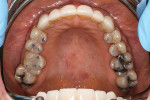
A thorough dental examination was completed, including diagnostic models, clinical photographs, a panoramic radiograph, and a cephalometric tracing. Moderate attrition was noted on the lingual of the maxillary incisors (Figure 4) and the facial of the mandibular incisors (Figure 5). No linear wear facets were noted, and there was a lack of posterior attrition. The patient was found to have several risk factors, including decreased overjet and slightly excessive overbite. A cephalometric tracing demonstrated the risk factors of the maxillary incisors being retroclined and the mandibular incisors being proclined.
Tooth structure loss that is not biofilm-mediated can be multifactoral. Occlusal problems and brain-mediated problems can result in abnormal attrition or bruxism. Environmental factors can lead to abrasion or erosion. The clinician must distinguish between these modes of tooth structure loss. Referring to the medical model flowchart at this step (Table 1, Step 3), occlusal dysfunction and parafunction were eliminated due to the pattern of attrition (ie, lack of linear wear facets and posterior attrition) and the risk factors that were noted. This left the remaining diagnosis of constricted chewing pattern.
Step 4: Ancillary Tests
This case did not require an ancillary test, such as a Kois deprogrammer, because a definitive diagnosis had been reached and each step of the model had complemented or corroborated the previous steps. By following the medical model via linear thinking, as in this case, the diagnosis can be reached prior to using a deprogrammer. Evaluation of all the disease indicators and risk factors may enable the other differential diagnoses to be effectively eliminated before using the deprogrammer.
If, after the physical examination, no definitive diagnosis had been reached, then a Kois deprogrammer may have been used to determine the position of the mandible in centric relation (CR) or adapted CR and help ascertain a definitive diagnosis based on whether the mandible came forward or went back. Had the patient stated she would not go through with orthodontics, then it would have been necessary to use the deprogrammer as a treatment device (not for diagnostics) to establish the reference position, CR, in order to increase the vertical dimension of occlusion (VDO) and correct the constricted chewing pattern.
Step 5: Diagnosis
The use of the medical model via linear thinking, as illustrated through the charts, ensured that all disease indicators and risk factors, whether present or absent, were considered, and that each step complemented or corroborated the previous step. This allowed the determination of the definitive functional diagnosis of a constricted chewing pattern (Table 1, Step 5).
Steps 6 and 7: Risk Assessment and Prognosis Without Treatment
Periodontal: Periodontal examination revealed probing depths of 1 mm to 4 mm and radiographic mild generalized interproximal horizontal bone loss and recession—less than 2 mm—that had been clinically stable.
Diagnosis: Mild chronic periodontitis, AAP type II
Risk: Low
Prognosis: Good
Biomechanical: Clinical examination revealed defective restorations for teeth Nos. 5 and 30 due to fracture and leaking margins. Questionable restorations were noted on teeth Nos. 2, 4, 6, 11 through 15, and 30. Structural compromises were noted on teeth Nos. 3 and 19. Occlusal erosion was noted on teeth Nos. 7 through 10 and 20 through 30, and cervical abrasion was noted on teeth Nos. 4 through 7, 10 through 13, 21, 28, and 30. The patient reported a history of drinking acidic beverages combined with aggressive brushing and denied any history of acid reflux.
Diagnosis: Listed above
Risk: Moderate
Prognosis: Poor, due to defective restorations
Functional: As discussed above, the clinical examination revealed anterior attrition involving the lingual of the maxillary incisors and the facial of the lower incisors. The patient reported her jaw felt pushed back and that the wear was increasing.
Diagnosis: Constricted chewing pattern (as discussed above)
Risk: Moderate
Prognosis: Fair
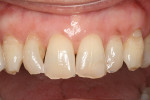
Dentofacial: The clinical examination revealed medium lip dynamics. The combination of thin periodontal phenotype, mild recession, and triangular-shaped teeth resulted in black triangles, which the patient disliked. She also was displeased with the thin, uneven incisal edges on her anterior teeth (Figure 6 and Figure 7).
Diagnosis: Moderate gingival display
Risk: Moderate
Prognosis: Poor, due to the patient’s displeasure with the appearance of her teeth
Treatment Goals
The primary goal of treatment was to create a healthy anterior functional relationship in the most conservative way while simultaneously addressing the patient’s esthetic concerns. This would require replacing the defective and questionable restorations and restoring the tooth structure lost to attrition, erosion, and abrasion.
Step 8: Treatment Plan Options/Informed Consent
After carefully considering the proposed treatment options (ie, increasing the VDO restoratively to remove the functional envelope interferences versus orthodontically repositioning the teeth) and providing informed consent, the patient agreed to correct the constricted chewing pattern with orthodontic treatment. This would reposition the anterior teeth so that chewing could occur without interferences in the functional envelope. Next, a diagnostic wax-up and intraoral mock-up would be completed and approved by the patient. Teeth Nos. 6 through 11 would then be prepared for adhesively retained porcelain veneers to replace lost tooth structure. Anterior tooth shape would be modified to remove the black triangles and improve the esthetics of her smile. Direct composites would be placed on teeth Nos. 22 through 27 to replace lost tooth structure and produce a level mandibular anterior occlusal plane. The direct composites would reduce cost for the patient while still addressing the esthetic concerns. Direct composites would also be placed on teeth Nos. 4, 5, 12, 13, 20, 21, 28, and 30 to restore areas of questionable and defective restorations and replace lost tooth structure due to erosion and abrasion. After delivery of the porcelain veneers, occlusion would be refined using an intraorally fabricated Kois deprogrammer. The patient would then wear retainers fabricated by the orthodontist.
A post-treatment assessment would be completed using the medical model and linear thinking to determine the post-treatment diagnosis, risk, and prognosis, in order to verify that the completed treatment had lowered the patient’s functional risk and improved her functional prognosis.
Step 9: Treatment (Phases)
Phase 1 (orthodontic therapy): The patient underwent orthodontic treatment to correct the constricted chewing pattern, the mild crowding, and the rotation of tooth No. 12. The orthodontist was unable to correct the cross-bite present at tooth No. 3. The patient maintained her 6-month periodontal maintenance visits throughout orthodontic treatment.
Phase 2 (restorative treatment): Postorthodontic models were made and mounted using the Kois dentofacial analyzer. A diagnostic wax-up was completed along with an intraoral mock-up, which the patient approved. Direct composites were placed on teeth Nos. 4, 5, 12, 13, 20 through 28, and 30 utilizing a putty matrix made from the wax-up to guide the placement for teeth Nos. 22 through 27. Teeth Nos. 6 through 11 were conservatively prepared for veneers, and provisionals were placed. E.max® (Ivoclar Vivadent, ivoclarvivadent.com) veneers were tried in at the next visit, and the patient approved of the esthetics. The veneers were cemented using Bis-Silane™ porcelain primer (Bisco, bisco.com), All-Bond Universal® adhesive (Bisco), and RelyX™ Veneer Cement translucent shade (3M ESPE, 3m.com) (Figure 8 and Figure 9). A chairside Kois deprogrammer was fabricated and used for refinement of the occlusion.4 The orthodontist then fabricated retainers for the patient.
Step 10: Treatment Assessment and Verification
Eight months after treatment, a post-treatment assessment was performed. The patient filled out new medical and dental history forms and a physical examination was completed. The occlusion was checked with 8-µm blue TrollFoil (Troll Dental, trolldental.com) articulating paper to ensure bilateral, simultaneous, equal-intensity posterior contacts (Figure 10). The functional envelope was checked for friction using 200-µm Bausch horseshoe articulating paper with the patient sitting upright and being asked to chew and the clinician checking for the absence of interference streaks on any teeth (Figure 11). The functional diagnosis of acceptable function was verified.
Periodontal: Risk: Low; Prognosis: Good
Biomechanical: Risk: Moderate; Prognosis: Fair, due to structural compromises and remaining questionable restorations
Functional: Risk: Low; Prognosis: Good
Dentofacial: Risk: Moderate; Prognosis: Good
Conclusion
Through the use of the medical model and linear thinking, conservative treatment was effectively implemented to reduce the patient’s functional risk and improve her biomechanical, functional, and dentofacial prognoses. Determining an accurate definitive diagnosis increased the predictability that the treatment would alleviate the occlusal disease that was present. The patient was extremely happy with her new smile (Figure 12) and even happier that her new occlusion felt comfortable and is expected to be stable for the long term.
Acknowledgement
The author would like to thank Howard Mizuta, DDS, Ric Shepherd, DDS, and Kim Larson, DDS, whose efforts and support made this article possible. He would also like to thank Leon Hermanides, CDT, and Protea Dental Studio for their exceptional laboratory support, and Stephen Searcy, DDS, for his excellent orthodontic treatment.
About The Author
Christopher Huff, DMD
Private Practice
Lafayette, Louisiana
References
1. Laing RD. The Politics of the Family and Other Essays. New York, NY: Routledge; 1971.
2. Mengatto CM, Dalberto Cda S, Scheeren B, Barros SG. Association between sleep bruxism and gastroesophageal reflux disease. J Prosthet Dent. 2013;110(5):349-355.
3. Ohmure H, Oikawa K, Kanematsu K, et al. Influence of experimental esophageal acidification on sleep bruxism: a randomized trial. J Dent Res. 2011;90(5):665-671.
4. Beshar MJ. Systematic treatment using a direct deprogrammer to resolve long-standing problems in a phobic patient. Compend Contin Educ Dent. 2015;36(6):418,421-425.