CAD/CAM Technology and Esthetic Dentistry: A Case Report
Abstract:
Advances in dental materials as well as in computer technology have made CAD/CAM-fabricated restorations not just possible in dentistry but plentiful. When using CAD/CAM systems, operators can fabricate restorations from several materials, including ceramics, metal alloys, and various composites. This case report describes the replacement of a porcelain-layered zirconia-based (coping) crown on a left lower cuspid that presented with a veneering ceramic chipping on a lithium-disilicate CAD/CAM-fabricated crown. It demonstrates how all-ceramic systems offer a promising alternative in the restoration of anterior teeth.
Over the past two decades, dentistry has seen the development of many new all-ceramic restorative systems. The drive for such materials and restorative techniques has been precipitated by patient expectations for excellent esthetic results and also by concerns about the biocompatibility of metals intraorally.1,2 The combination of advancements in dental materials as well as in computer technology has made computer-assisted design/computer-assisted manufacturing (CAD/CAM)-fabricated restorations possible—and plentiful—in dental clinics. As a result, all-ceramic restorations have become both a necessary alternative to metal–ceramic systems, as well as a preferred choice. These new all-ceramic systems can use a monolithic glass–ceramic material (eg, IPS e.max® CAD, Ivoclar Vivadent, www.ivoclarvivadent.com), whereas others utilize layered porcelain over the core.1
CAD/CAM technology was introduced to dentistry in the early 1980s, and since then, it has evolved in two directions. One is the intraoperatory (chairside) application for a one-appointment restoration fabrication and insertion using prefabricated ceramic monoblocks. The major impediment is its high initial cost, which can make it difficult for many dental offices to adopt the technology. The other direction is the development of systems for commercial production centers and dental laboratories.3 Regardless of the system (chairside or commercial laboratory), all CAD/CAM units have three functional components: data capture or scanning to capture and record data about the oral environment (eg, tooth preparation, adjacent teeth, and occluding tooth geometry); CAD to design the restoration to fit the preparation and to perform according to conventional dental requirements; and CAM to fabricate the restoration.4
CAD/CAM Systems
An example of a chairside system is the computer-assisted CERamic REConstruction system (CEREC®, Sirona Dental Systems, www.sirona.com), which was the first operational CAD/CAM system to be used in the dental office.5 The system has evolved through a series of software and hardware upgrades since its introduction to the dental marketplace.6 CEREC uses an intraoral digital 3-dimensional (3-D) scanning device (digitizer) that takes a 3-D image of the tooth preparation. It uses infrared waves, which are sent down to the preparation and back to the camera to measure heights of the tooth structure, adjacent teeth, and surrounding tissue. Nontoxic, titanium-dioxide powder is applied to the preparations and neighboring teeth to ensure the waves bounce back to the camera in a uniform manner. Since dentin, enamel, and gingiva absorb the infrared waves at different rates, an unpowdered field would reflect the waves inconsistently and result in a picture that the CEREC 3-D software cannot use.
Another example of a chairside system is the E4D (E4D Technologies LLC, www.e4d.com), which uses an intraoral digitizer laser—which requires no powder—to capture the teeth preparations.
Examples of CAD/CAM systems for commercial production centers and dental laboratories include NobelProcera™ (Nobel Biocare, www.nobelbiocare.com), which was first introduced in 1993,7 and Lava™ (3M ESPE, www.3MESPE.com), which launched in 2001.8
Materials Used for CAD/CAM Restorations
When using CAD/CAM systems, operators can fabricate restorations from ceramics, metal alloys, and various composites. Ceramic crowns can be fabricated using two types of systems9-11:
• A double-layer type of system, which has a high-strength core that is predominantly either zirconia or alumina (extremely strong but generally not as esthetic), which requires subsequent veneering using traditional hand-stacking methods to achieve acceptable esthetics.4
• A single-layer type (monolithic) without a separate core and overlying layered porcelain; this version is not subjected to the porcelain firing cycle.12
For the double-layer technique, zirconium-dioxide (zirconia ZrO2) ceramics, when compared to other all-ceramic systems, exhibit superior mechanical properties, high flexural strength (900 MPa to 1,200 MPa), and good fracture toughness (6 MPa to 10 MPa m1/2).13 Currently, two types of zirconia blocks are available for CAD/CAM systems. One is a completely sintered dense block for direct machining (DCS system, DCS Dental AG, www.dcs-dental.com), and the other requires post-machining sintering (eg, Lava, 3M ESPE, and Cerco©, DeguDent GmbH, www.degudent.com). The latter ones are namely blocks at the green stage (pre-sintered) form of zirconia.14 For these systems, the original copings/frameworks are enlarged precisely in order to compensate for the material shrinkage (20% to 25%) that occurs during the final stage of sintering.15,16
Completely sintered zirconia blocks are not subject to dimensional changes, but they are extremely difficult and time-consuming to machine. This can cause damage to the fabrication tools as well as chip formation during the manufacturing process. Milling of pre-sintered blocks is faster and causes less wear and tear on the fabrication hardware.
The addition of porcelain to the copings of the double-layer technique may cause a negative effect on the fit of the crowns.17,18 The differential contraction of the core and veneering ceramics upon cooling creates thermally induced stresses that change the resistance of the crown when subjected to mechanical loads.19 Although zirconia presents excellent mechanical properties, some clinical trials have reported the chipping of the veneer portion of the crowns.20 This chipping is attributable to the mechanical insufficiency of the veneering porcelain.
Many ceramic systems have been used for the single-layer techniques (monolithic) such as feldspathic ceramic (eg, Vitablocs® Mark II, Vita Zahnfabrik, www.vita-zahnfabrik.com) and leucite-reinforced glass-ceramics (eg, IPS Empress® CAD, Ivoclar Vivadent). A lithium-disilicate restorative material (IPS e.max CAD), which was initially designed for use in double-layer techniques as a coping material (more translucent than zirconia), then became available in a variety of shades and several translucencies for use in esthetic full-contour single-layer (monolithic) restorations.6 The blocks are produced by massive casting (transparent glass ingots) using a technology that prevents the formation of defects (pores, accumulation of pigments, etc) in the bulk of the ingot. Partial crystallization enables fast machining with CAD/CAM systems (blue, translucent state). Following the milling procedure, the restorations are tempered and thus reach the fully crystallized state. In the course of this process, lithium-disilicate crystals (Li2Si2O5) are formed, which impart the ceramic object with the desired high strength.21
In a 2010 laboratory study, investigators found monolithic lithium-disilicate ceramic crowns to have a ceramic fracture resistance better than that of porcelain-veneered zirconia (coping) crowns.22 A prospective study comparing 10-year outcome data of three-unit all-ceramic fixed dental prostheses (FDPs) fabricated from a monolithic lithium-disilicate ceramic (IPS e.max), with the outcome data regarding metal–ceramic FDPs as revealed by systematic reviews, reported the rate of ceramic chipping as 3% after 5 years and 6.1% after 10 years. These results were similar to those found with metal–ceramic FDPs (3% after 3 to 5 years), but were considerably smaller than has been reported for all-ceramic FDPs (10% after 3 years, and 13.6% to 16% after 5 years).23,24
The following case report describes the replacement of a porcelain-layered zirconia-based (coping) crown on a left lower cuspid that presented with a veneering ceramic chipping on a lithium-disilicate CAD/CAM-fabricated crown.
Case Report
Diagnosis and Treatment Planning
A 48-year-old man in excellent health was referred to replace an all-ceramic crown with unsatisfactory esthetics. During the examination, it was noted that the ceramic veneering material on the previously placed layered zirconia crown was chipped at the incisal edge. The patient was given the option of a porcelain-fused-to-metal (PFM) or an all-ceramic restoration using lithium disilicate. For esthetics reasons, the patient chose to have the crown replaced with the all-ceramic option.
Clinical Protocol
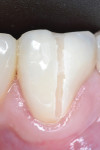
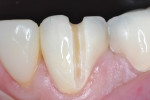
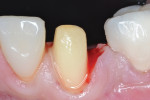
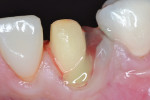
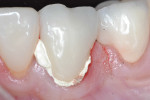
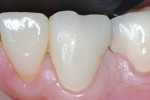
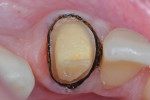
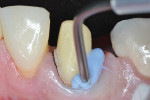
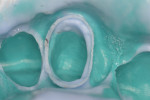
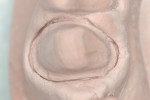
Preoperatively, occlusion was analyzed clinically, and then with the aid of mounted study models on a semi-adjustable articulator (Whip Mix 4640, Whip Mix Corp., www.whipmix.com). This was done to plan for proper tooth reduction. Another impression was made with a partial, disposable metal tray (TempTray™, Clinician’s Choice Dental Products, Inc., www.clinicianschoice.com) loaded with a vinyl polysiloxane (VPS) matrix material (Template®, Clinician’s Choice), prior to the crown removal in order to facilitate the fabrication of the provisional restoration. To remove the previously placed layered zirconia crown, a new diamond bur (Predator Zirconia®, Clinician’s Choice) designed especially for cutting zirconia copings and frameworks, was chosen in order to reduce the operatory time. Cuts were made through the ceramic layer (Figure 1), and then through the zirconia coping (Figure 2), using a long thin diamond bur. Next, the tooth was refined using modified shoulder diamond burs (medium and fine) (837KR 012 diamond, Brasseler USA, www.brasselerusa.com). During crown removal, the scattered ceramic caused some minor damage to the soft tissue (Figure 3) and a hemostatic agent (Tissue Goo™, Clinician’s Choice) was used to achieve hemostasis (Figure 4) prior to the fabrication of the temporary restoration.
The provisional restoration was fabricated using the Template matrix by applying a bis-acryl material (Temptation® Now, Clinician’s Choice) inside the impression. After polymerization, the provisional material was removed from the matrix. The margins were inspected, the occlusion was adjusted, and the provisional was coated with an unfilled light-cure resin (Glisten™ Provisional Resin Glaze, Clinician’s Choice) in order to provide a high-gloss shine finish. The temporary restoration was then cemented with a polycarboxylate resin-reinforced cement (Cling2®, Clinician’s Choice) (Figure 5) and the excess removed with an explorer.
At the following appointment (Figure 6), the provisional was removed and a small unimpregnated retraction cord was placed (Re-Cord™ No. 000, Clinician’s Choice) followed by a second cord (Re-Cord No. 00) (Figure 7). A small amount of bleeding occurred during this stage, and a hemostatic solution (Tissue Goo) was applied. The final full-arch impression was made with a combination of a heavy- and light-viscosity VPS (Affinity™ Putty and Affinity Light Body HF, Clinician’s Choice) (Figure 8 through Figure 10), and an impression of the opposing dentition was also made with multipurpose replication silicone (COUNTER-FIT™, Clinician’s Choice). An interocclusal record at the patient’s maximum intercuspation position and a facebow transfer were obtained. The shade was determined using a shade guide (Vitapan 3D Master, Vita, www.vident.com). The IPS e.max CAD crowns were then manufactured by the dental laboratory team.
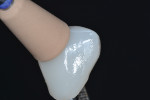
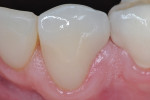
During the final appointment, the margins of the crown were inspected before cementation, and the occlusion was checked. An aluminum-oxide bur (Dura-Green®, Shofu Dental Corp., www.shofu.com) was used to adjust the occlusion, causing a rough surface at the buccal–incisal area (Figure 11). This area was repolished using a sequence of diamond impregnated polishers designed for hybrid composites and porcelain (D-Fine™ Double Diamond™, Clinician’s Choice) (Figure 12 and Figure 13), and the crown was cemented with a dual-cure resin cement (Variolink® II, Ivoclar Vivadent) (Figure 14).
Finally, the patient received postoperative care instructions, and recall appointments were scheduled.
Conclusions
All-ceramic systems offer a promising alternative for the restoration of anterior teeth. Clinical evaluations have demonstrated that high success rates can be achieved with this technique. It would seem that reports from in-vitro studies and some clinical trials show great promise for the use of lithium disilicate. This material provides high strength restorations with excellent esthetics and fit, and, being metal-free, the incidence of allergic reactions among patients is likely to be reduced.
ACKNOWLEDGMENT
The authors would like to acknowledge the educational grant and materials received from Clinician’s Choice used to support this article. They would also like to thank the Dental Design Centre (DDC) (London, Ontario, Canada) lab team for their excellent work.
DISCLOSURE
Dr. Gildo Santos is a paid consultant for research and development for Clinical Research Dental and Clinician’s Choice. Also, prior to retirement, Dr. Boksman was a paid part-time consultant to Clinical Research Dental and Clinician’s Choice with the title of Director of Clinical Affairs.
ABOUT THE AUTHORS
Gildo Coelho Santos Jr., DDS, MSc, PhD
Associate Professor and Chair, Division of Restorative Dentistry, Schulich School of Medicine and Dentistry, University of Western Ontario, London, Ontario, Canada
Leendert (Len) Boksman DDS, BSc
Former Associate Professor in Operative Dentistry, Schulich School of Medicine and Dentistry, University of Western Ontario, London, Ontario, Canada; Former Director of Clinical Affairs, Clinical Research Dental, London, Ontario, Canada, and Clinician’s Choice, New Milford, Connecticut; Dr. Boksman is now retired from private practice.
Maria Jacinta Moraes Coelho Santos, DDS, MSc, PhD
Assistant Professor, Schulich School of Medicine and Dentistry, University of Western Ontario, London, Ontario, Canada
REFERENCES
1. Barnfather KD, Brunton PA. Restoration of the upper dental arch using Lava all-ceramic crown and bridgework. Br Dent J. 2007;202(122):731-735.
2. Laeijendecker R, van Joost T. Oral manifestations of gold allergy. J Am Acad Dermatol. 1994;30(2 pt 1):205-209.
3. Walia S, Thomas PM, Sandhu H, Santos GC Jr. Restoring esthetics with metal-free ceramics: a case report. J Can Dent Assoc. 2009;75(5):353-355.
4. Strub JR, Rekow ED, Witkowski S. Computer-aided design and fabrication of dental restorations: current systems and future possibilities. J Am Dent Assoc. 2006;137(9):1289-1296.
5. Heymann HO, Bayne SC, Sturdevant JR, et al. The clinical performance of CAD-CAM-generated ceramic inlays: a four-year study. J Am Dent Assoc. 1996;127(8):1171-1181.
6. Fasbinder DJ. The CEREC system: 25 years of chairside CAD/CAM dentistry. J Am Dent Assoc. 2010;141(suppl 2):3S-4S.
7. Marks JG Jr, Belsito DV, DeLeo VA, et al. North American Contact Dermatitis Group patch-test results, 1996-1998. Arch Dermatol. 2000;136(2):272-273.
8. 3M ESPE Lava crowns and bridges: 7-year clinical performance. Dent Advisor. 2010;27(7):6-7.
9. McLaren EA, Terry DA. CAD/CAM systems, materials, and clinical guidelines for all-ceramic crowns and fixed partial dentures. Compend Contin Educ Dent. 2002;23(7):637-641, 644, 646.
10. Yara A, Ogura H, Shinya A, et al. Durability of diamond burs for the fabrication of ceramic crowns using dental CAD/CAM. Dent Mater J. 2005;24(1):134-139.
11. Tomita S, Shin-Ya A, Gomi H, et al. Machining accuracy of CAD/CAM ceramic crowns fabricated with repeated machining using the same diamond bur. Dent Mater J. 2005;24(1):123-133.
12. Lee KB, Park CW, Kim KH, Kwon TY. Marginal and internal fit of all-ceramic crowns fabricated with two different CAD/CAM systems. Dent Mater J. 2008;27(3):422-426.
13. Komine F, Blatz MB, Matsumura H. Current status of zirconia-based fixed restorations. J Oral Sci. 2010;52(4):531-539.
14. Kunii J, Hotta Y, Tamaki Y, et al. Effect of sintering on the marginal and internal fit of CAD/CAM-fabricated zirconia frameworks. Dent Mater J. 2007;26(6):820-826.
15. Filser F, Kocher P, Weibel F, et al. Reliability and strength of all-ceramic dental restorations fabricated by direct ceramic machining (DCM). Int J Comput Dent. 2001;4(2):89-106.
16. Suttor D, Bunke K, Hoescheler S, et al. LAVA—the system for all-ceramic ZrO2 crown and bridge frameworks. Int J Comput Dent. 2001;4(3):195-206.
17. Nothdurft FP, Pospiech PR. Clinical evaluation of pulpless teeth restored with conventionally cemented zirconia posts: a pilot study. J Prosthet Dent. 2006;95(4):311-314.
18. Luthardt RG, Holzhüter M, Sandkuhl O, et al. Reliability and properties of ground Y-TZP-zirconia ceramics. J Dent Res. 2002;81(7):487-491.
19. Griggs JA. Recent advances in materials for all-ceramic restorations. Dent Clin North Am. 2007;51(3):713-727, viii.
20. Luthardt RG, Sandkuhl O, Reitz B. Zirconia-TZP and alumina—advanced technologies for the manufacturing of single crowns. Eur J Prosthodont Restor Dent. 1999;7(4):113-119.
21. IPS e.max CAD. Ivoclar Vivadent AG. September 2005. Data on file.
22. Guess PC, Zavanelli RA, Silva NR, et al. Monolithic CAD/CAM lithium disilicate versus veneered Y-TZP crowns: comparison of failure modes and reliability after fatigue. Int J Prosthodont. 2010;23(5):434-442.
23. Sailer I, Pjetursson BE, Zwahlen M, Hämmerle CH. A systematic review of the survival and complication rates of all-ceramic and metal-ceramic reconstructions after an observation period of at least 3 years. Part II: Fixed dental prostheses. Clin Oral Implants Res. 2007;18(suppl 3):86-96.
24. Heintze SD, Rousson V. Survival of zirconia- and metal-supported fixed dental prostheses: a systematic review. Int J Prosthodont. 2010;23(6):493-502.